Neurodegenerative disease
| Neurodegenerative disease | |
|---|---|
 | |
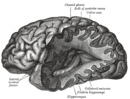
| Normal brain on left contrasted with structural changes shown in brain on right of person with Alzheimer's disease, the most common neurodegenerative disease[1] | |
| Specialty | Neurology, Psychiatry |
A neurodegenerative disease is caused by the progressive loss of structure or function of
Within neurodegenerative diseases, it is estimated that 55 million people worldwide had dementia in 2019, and that by 2050 this figure will increase to 139 million people.[8]
Specific disorders
The consequences of neurodegeneration can vary widely depending on the specific region affected, ranging from issues related to movement to the development of dementia.[9][10]
Alzheimer's disease

AD pathology is primarily characterized by the presence of
Parkinson's disease
PD is primarily characterized by death of
The main known risk factor is age. Mutations in genes such as α-synuclein (SNCA),
Huntington's disease
HD is caused by
Multiple sclerosis
Amyotrophic lateral sclerosis
Independent research provided in vitro evidence that the primary cellular sites where SOD1 mutations act are located on
Batten disease
Creutzfeldt–Jakob disease
Creutzfeldt–Jakob disease (CJD) is a prion disease that is characterized by rapidly progressive dementia.[49] Misfolded proteins called prions aggregate in brain tissue leading to nerve cell death.[50] Variant Creutzfeldt–Jakob disease (vCJD) is the infectious form that comes from the meat of a cow that was infected with bovine spongiform encephalopathy, also called mad cow disease.[51]
Risk factor
The greatest risk factor for neurodegenerative diseases is aging. Mitochondrial DNA mutations as well as oxidative stress both contribute to aging.[52] Many of these diseases are late-onset, meaning there is some factor that changes as a person ages for each disease.[6] One constant factor is that in each disease, neurons gradually lose function as the disease progresses with age. It has been proposed that DNA damage accumulation provides the underlying causative link between aging and neurodegenerative disease.[53][54] About 20–40% of healthy people between 60 and 78 years old experience discernable decrements in cognitive performance in several domains including working, spatial, and episodic memory, and processing speed.[55]

A study using electronic health records indicates that 45 (with 22 of these being replicated with the UK Biobank) viral exposures can significantly elevate risks of neurodegenerative disease, including up to 15 years after infection.[56][57]
Mechanisms
Genetics
Many neurodegenerative diseases are caused by
Polyglutamine repeats typically cause dominant pathogenesis. Extra glutamine residues can acquire toxic properties through a variety of ways, including irregular protein folding and degradation pathways, altered subcellular localization, and abnormal interactions with other cellular proteins.[58] PolyQ studies often use a variety of animal models because there is such a clearly defined trigger – repeat expansion. Extensive research has been done using the models of nematode (C. elegans), and fruit fly (Drosophila), mice, and non-human primates.[59][60]
Nine inherited neurodegenerative diseases are caused by the expansion of the CAG trinucleotide and polyQ tract, including Huntington's disease and the spinocerebellar ataxias.[61]
Epigenetics
The presence of epigenetic modifications for certain genes has been demonstrated in this type of pathology. An example is FKBP5 gene, which progressively increases its expression with age and has been related to Braak staging and increased tau pathology both in vitro and in mouse models of AD.[62]
Protein misfolding
Several neurodegenerative diseases are classified as
- Lewy bodies, such as Parkinson's disease, dementia with Lewy bodies, and multiple system atrophy. Alpha-synuclein is the primary structural component of Lewy body fibrils. In addition, an alpha-synuclein fragment, known as the non-Abeta component (NAC), is found in amyloid plaques in Alzheimer's disease.
- behavioral variant frontotemporal dementia.
- amyloid beta: the major component of amyloid plaques in Alzheimer's disease.
- prion diseases and transmissible spongiform encephalopathy.
Intracellular mechanisms
Protein degradation pathways
Parkinson's disease and Huntington's disease are both late-onset and associated with the accumulation of intracellular toxic proteins. Diseases caused by the aggregation of proteins are known as
- cytosol, e.g. Parkinson's and Huntington's
- nucleus, e.g. Spinocerebellar ataxia type 1 (SCA1)
- endoplasmic reticulum (ER), (as seen with neuroserpin mutations that cause familial encephalopathy with neuroserpin inclusion bodies)
- extracellularly excreted proteins, amyloid-beta in Alzheimer's disease
There are two main avenues eukaryotic cells use to remove troublesome proteins or organelles:
- ubiquitin–proteasome: protein ubiquitin along with enzymes is key for the degradation of many proteins that cause proteopathies including polyQ expansions and alpha-synucleins. Research indicates proteasome enzymes may not be able to correctly cleave these irregular proteins, which could possibly result in a more toxic species. This is the primary route cells use to degrade proteins.[6]
- Decreased proteasome activity is consistent with models in which intracellular protein aggregates form. It is still unknown whether or not these aggregates are a cause or a result of neurodegeneration.[6]
- autophagy–lysosome pathways: a form of macroautophagy and chaperone-mediated autophagy (CMA).[6]
- macroautophagy is involved with nutrient recycling of macromolecules under conditions of starvation, certain apoptotic pathways, and if absent, leads to the formation of ubiquinated inclusions. Experiments in mice with neuronally confined macroautophagy-gene knockouts develop intraneuronal aggregates leading to neurodegeneration.[6]
- chaperone-mediated autophagy defects may also lead to neurodegeneration. Research has shown that mutant proteins bind to the CMA-pathway receptors on lysosomal membrane and in doing so block their own degradation as well as the degradation of other substrates.[6]
Membrane damage
Damage to the membranes of organelles by monomeric or oligomeric proteins could also contribute to these diseases. Alpha-synuclein can damage membranes by inducing membrane curvature,[24] and cause extensive tubulation and vesiculation when incubated with artificial phospholipid vesicles.[24] The tubes formed from these lipid vesicles consist of both micellar as well as bilayer tubes. Extensive induction of membrane curvature is deleterious to the cell and would eventually lead to cell death. Apart from tubular structures, alpha-synuclein can also form lipoprotein nanoparticles similar to apolipoproteins.
Mitochondrial dysfunction
The most common form of cell death in neurodegeneration is through the intrinsic mitochondrial apoptotic pathway. This pathway controls the activation of caspase-9 by regulating the release of cytochrome c from the mitochondrial intermembrane space. Reactive oxygen species (ROS) are normal byproducts of mitochondrial respiratory chain activity. ROS concentration is mediated by mitochondrial antioxidants such as manganese superoxide dismutase (SOD2) and glutathione peroxidase. Over production of ROS (oxidative stress) is a central feature of all neurodegenerative disorders. In addition to the generation of ROS, mitochondria are also involved with life-sustaining functions including calcium homeostasis, PCD, mitochondrial fission and fusion, lipid concentration of the mitochondrial membranes, and the mitochondrial permeability transition. Mitochondrial disease leading to neurodegeneration is likely, at least on some level, to involve all of these functions.[64]
There is strong evidence that mitochondrial dysfunction and oxidative stress play a causal role in neurodegenerative disease pathogenesis, including in four of the more well known diseases
Neurons are particularly vulnerable to oxidative damage due to their strong metabolic activity associated with high transcription levels, high oxygen consumption, and weak antioxidant defense.[65][66]
DNA damage
The brain metabolizes as much as a fifth of consumed oxygen, and
Axonal transport
Axonal swelling, and
Programmed cell death
Programmed cell death (PCD) is death of a cell in any form, mediated by an intracellular program.[70] This process can be activated in neurodegenerative diseases including Parkinson's disease, amytrophic lateral sclerosis, Alzheimer's disease and Huntington's disease.[71] PCD observed in neurodegenerative diseases may be directly pathogenic; alternatively, PCD may occur in response to other injury or disease processes.[7]
Apoptosis (type I)
Apoptosis is a form of programmed cell death in multicellular organisms. It is one of the main types of programmed cell death (PCD) and involves a series of biochemical events leading to a characteristic cell morphology and death.
- Extrinsic apoptotic pathways: Occur when factors outside the cell activate cell surface death receptors (e.g., Fas) that result in the activation of caspases-8 or -10.[7]
- Intrinsic apoptotic pathways: Result from mitochondrial release of cytochrome c or endoplasmic reticulum malfunctions, each leading to the activation of caspase-9. The nucleus and Golgi apparatus are other organelles that have damage sensors, which can lead the cells down apoptotic pathways.[7][72]
Autophagic (type II)
Autophagy is a form of intracellular phagocytosis in which a cell actively consumes damaged organelles or misfolded proteins by encapsulating them into an autophagosome, which fuses with a lysosome to destroy the contents of the autophagosome. Because many neurodegenerative diseases show unusual protein aggregates, it is hypothesized that defects in autophagy could be a common mechanism of neurodegeneration.[7]
Cytoplasmic (type III)
PCD can also occur via non-apoptotic processes, also known as Type III or cytoplasmic cell death. For example, type III PCD might be caused by trophotoxicity, or hyperactivation of trophic factor receptors. Cytotoxins that induce PCD can cause necrosis at low concentrations, or aponecrosis (combination of apoptosis and necrosis) at higher concentrations. It is still unclear exactly what combination of apoptosis, non-apoptosis, and necrosis causes different kinds of aponecrosis.[7]
Transglutaminase
The main function of transglutaminases is
Transglutaminase binding of these proteins and peptides make them clump together. The resulting structures are turned extremely resistant to chemical and mechanical disruption.[73]
Most relevant human neurodegenerative diseases share the property of having abnormal structures made up of proteins and peptides.[73]
Each of these neurodegenerative diseases have one (or several) specific main protein or peptide. In
Transglutaminase augmented expression: It has been proved that in these neurodegenerative diseases (Alzheimer's disease, Parkinson's disease, and Huntington's disease) the expression of the transglutaminase enzyme is increased.[73]
Presence of isopeptide bonds in these structures: The presence of isopeptide bonds (the result of the transglutaminase reaction) have been detected in the abnormal structures that are characteristic of these neurodegenerative diseases.[73]
Co-localization: Co-localization of transglutaminase mediated isopeptide bonds with these abnormal structures has been detected in the autopsy of brains of patients with these diseases.[73]
Management
The process of neurodegeneration is not well understood, so the diseases that stem from it have, as yet, no cures.
Animal models in research
In the search for effective treatments (as opposed to
In another experiment using a rat model of Alzheimer's disease, it was demonstrated that systemic administration of hypothalamic proline-rich peptide (PRP)-1 offers neuroprotective effects and can prevent neurodegeneration in hippocampus
Other avenues of investigation
Protein degradation offers therapeutic options both in preventing the synthesis and degradation of irregular proteins. There is also interest in upregulating autophagy to help clear protein aggregates implicated in neurodegeneration. Both of these options involve very complex pathways that we are only beginning to understand.[6]
The goal of immunotherapy is to enhance aspects of the immune system. Both active and passive vaccinations have been proposed for Alzheimer's disease and other conditions; however, more research must be done to prove safety and efficacy in humans.[77]
A current therapeutic target for the treatment of Alzheimer's disease is the protease β-secretase[78][non-primary source needed], which is involved in the amyloidogenic processing pathway that leads to the pathological accumulation of proteins in the brain. When the gene that encodes for amyloid precursor protein (APP) is spliced by α-secretase[79][non-primary source needed] rather than β-secretase, the toxic protein β amyloid is not produced. Targeted inhibition[80] of β-secretase can potentially prevent the neuronal death that is responsible for the symptoms of Alzheimer's disease.
Dr. Antonio Barbera, a former obstetrics and gynaecology doctor, is prescribing table tennis for patients who are suffering from a serious neurological disorder.[81]
See also
References
- ^ PMID 28716886.
- PMID 34829716.
- PMID 29513402.
- PMID 31013638.
- ^ "What is Neurodegenerative Disease?". JPND Research. 17 July 2014. Retrieved February 7, 2015.
- ^ S2CID 4411895.
- ^ PMID 17051206.
- ISBN 978-92-4-003324-5. Retrieved 14 October 2022.
- ISBN 978-1-4020-9434-7.
- .
- PMID 12934968.
- )
- PMID 21883222.
- PMID 34093032.
- ^ S2CID 54359937.
- PMID 16822978.
- S2CID 25376584.
- PMID 15787600.
- S2CID 25017332.
- S2CID 25739126.
- PMID 26718594.
- ^ "Parkinson's Disease Mechanism Discovered," HHMI Research News June 22, 2006.
- ^ PMID 18558852.
- ^ PMID 20693280.
- PMID 26601739.
- ^ PMID 33274040.
- PMID 28195358.
- ISBN 978-0-87893-742-4.
- PMID 18279698.
- PMID 17965655.
- ISBN 978-0-87893-742-4.
- PMID 10923984.
- ^ PMID 32675289.
- PMID 23768628.
- ^ a b "Multiple Sclerosis: Hope Through Research | National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. Retrieved 2020-11-30.
- ISBN 978-0-7234-3748-2, retrieved 2020-12-07
- ^ PMID 31885862.
- PMID 18490361.
- ^ PMID 32973334.
- ^ S2CID 208186566.
- PMID 17435755.
- PMID 17435754.
- S2CID 2987257.
- ^ a b "Batten Disease Fact Sheet | National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. Retrieved 30 November 2020.
- PMID 30783219.
- ^ PMID 30783219.
- ^ PMID 32300063.
- S2CID 241832253.
- ^ "Creutzfeldt-Jakob Disease Fact Sheet | National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. National Institute of Health. Retrieved 31 March 2022.
- ^ "Creutzfeldt-Jakob disease - Symptoms and causes". Mayo Clinic. Retrieved 31 March 2022.
- ^ Research, Center for Biologics Evaluation and (12 April 2019). "Variant Creutzfeldt-Jakob Disease (vCJD) and Factor VIII (pdFVIII) Questions and Answers". FDA. Retrieved 31 March 2022.
- ^ S2CID 4421515.
- ISBN 978-0120928606.
- PMID 26385091.
- PMID 28438892.
- ^ PMID 36669485.
- News article about the study: Kozlov, Max (23 January 2023). "Massive health-record review links viral illnesses to brain disease". Nature. 614 (7946): 18–19. from the original on 6 February 2023. Retrieved 15 February 2023.
- PMID 35925897.
- ^ S2CID 205037169.
- ^ PMID 18957429.
- PMID 18957428.
- PMID 18957430.
- PMID 33771206.
- PMID 29947927.
- PMID 18333761.
- PMID 28785371.
- ^ PMID 27663141.
- ^ PMID 25033177.
- ^ PMID 21550379.
- ^ Coleman MP & Freeman MF 'Wallerian degeneration, WldS and Nmnat' Annual Review of Neuroscience 2010, 33: 245-67
- PMID 17069462.
- S2CID 33018251.
- PMID 16200193.
- ^ S2CID 19739739.
- ^ Dimebon Disappoints in Phase 3 Trial
- ^ Sweetlove M: Phase III CONCERT Trial of Latrepirdine. Negative results. Pharm Med 2012;26(2):113-115
- S2CID 39817779.
- PMID 18352830.
- S2CID 54334969.
- PMID 2111583.
- PMID 22951439.
- ^ "Colorado doctor prescribes ping pong treatment for neurodegenerative disorders: 'Doing something good'". Fox News. January 12, 2024.
- Min YG, Choi SJ, Hong YH, Kim SM, Shin JY, Sung JJ. Dissociated leg muscle atrophy in amyotrophic lateral sclerosis/motor neuron disease: the 'split-leg' sign. Sci Rep. 2020 Sep 24;10(1):15661. . PMID 32973334; PMCID: PMC7518279.
- K. A. Irvine, W. F. Blakemore, Remyelination protects axons from demyelination-associated axon degeneration, Brain, Volume 131, Issue 6, June 2008, Pages 1464–1477,