Neutropenia
| Neutropenia | |
|---|---|
Infectious disease, Hematology | |
| Causes | Aplastic anemia, Glycogen storage disease, Cohen syndrome,[1][2] gene mutations |
| Diagnostic method | CBC[3] |
| Treatment | Antibiotics, Splenectomy if needed,[3] G-CSF |
Neutropenia is an abnormally low concentration of
Neutropenia can be divided into congenital and acquired, with
Decreased production of neutrophils is associated with deficiencies of
Signs and symptoms

Signs and symptoms of neutropenia include
Children may show signs of
Causes

The causes of neutropenia can be divided between problems that are transient and those that are chronic. Causes can be divided into these groups:[1][2][11][12]
- Chronic neutropenia:
- Aplastic anemia[13]
- Evans syndrome.[14][15]
- Felty syndrome
- Systemic lupus erythematosus[16]
- HIV/AIDS infection
- Glycogen storage disease
- Cohen syndrome[17]
- ELA2 mutation, GATA2 deficiency
- Barth syndrome
- Copper deficiency[18]
- Vitamin B12 deficiency[19]
- Pearson syndrome
- Some types of Hermansky–Pudlak syndrome
- Transient neutropenia:
Severe bacterial infections, especially in people with underlying hematological diseases or
Nutritional deficiencies, such as deficiency in
Other causes of congenital neutropenia are Shwachman–Diamond syndrome, Cyclic neutropenia, bone marrow failure syndromes, cartilage–hair hypoplasia, reticular dysgenesis, and Barth syndrome. Viruses that infect neutrophil progenitors can also be the cause of neutropenia. Viruses identified that have an effect on neutrophils are rubella and cytomegalovirus.[1] Though the body can manufacture a normal level of neutrophils, in some cases the destruction of excessive numbers of neutrophils can lead to neutropenia. These are:[1]
- Bacterialor fungal sepsis
- Necrotizing enterocolitis, circulating neutrophil population depleted due to migration into the intestines and peritoneum
- Alloimmuneneonatal neutropenia, the mother produces antibodies against fetal neutrophils
- Inherited autoimmune neutropenia, the mother has autoimmune neutropenia
- Autoimmune neutropenia of infancy, the sensitization to self-antigens
Pathophysiology
The
Neutropenia fever can complicate the treatment of
Diagnosis
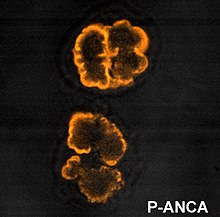
Neutropenia can be the result of a variety of consequences, including taking certain types of drugs, exposure to environmental toxins, vitamin deficiencies, metabolic abnormalities, as well as cancer, viral or bacterial infections. Neutropenia itself is a rare entity, but can be clinically common in oncology[35] and immunocompromised individuals as a result of chemotherapy (drug-induced neutropenia). Additionally, acute neutropenia can be commonly seen from people recovering from a viral infection or in a post-viral state. Meanwhile, several subtypes of neutropenia exist which are rarer and chronic, including acquired (idiopathic) neutropenia, cyclic neutropenia, autoimmune neutropenia, and congenital neutropenia.[36][37]
Neutropenia that is developed in response to chemotherapy typically becomes evident in seven to fourteen days after treatment, this period is known as the Nadir or 'low point'.[38][39] Conditions that indicate the presence of neutropenic fever are implanted devices; leukemia induction; the compromise of mucosal, mucociliary and cutaneous barriers; a rapid decline in absolute neutrophil count, duration of neutropenia >7–10 days, and other illnesses that exist in the patient.[31]
Signs of infection can be subtle. Fevers are a common and early observation. Sometimes overlooked is the presence of hypothermia, which can be present in sepsis. Physical examination and accessing the history and physical examination is focused on sites of infection. Indwelling line sites, areas of skin breakdown, sinuses, nasopharynx, bronchi and lungs, alimentary tract, and skin are assessed.[31]
The diagnosis of neutropenia is done via the low neutrophil count detection on a
Classification

Generally accepted reference range for absolute neutrophil count (ANC) in adults is 1500 to 8000 cells per microliter (µl) of blood. Three general guidelines are used to classify the severity of neutropenia based on the ANC (expressed below in cells/µl):[42]
- Mild neutropenia (1000 <= ANC < 1500): minimal risk of infection
- Moderate neutropenia (500 <= ANC < 1000): moderate risk of infection
- Severe neutropenia (ANC < 500): severe risk of infection.
Each of these are either derived from laboratory tests or via the formula below:
Treatment
A fever, when combined with profound neutropenia (febrile neutropenia), is considered a medical emergency and requires broad spectrum antibiotics. An absolute neutrophil count less than 200 is also considered a medical emergency and almost always requires hospital admission and initiation of broad spectrum antibiotics with selection of specific antibiotics based on local resistance patterns.[2]Precautions to avoid opportunistic infections in those with chronic neutropenia include maintaining proper soap and water hand hygiene, good dental hygiene and avoiding highly contaminated sources that may contain a large fungal reservoirs such as mulch, construction sites and bird or other animal waste.[2]
Neutropenia can be treated with the hematopoietic growth factor
Most cases of neonatal neutropenia are temporary. Antibiotic prophylaxis is not recommended because of the possibility of encouraging the development of multidrug-resistant bacterial strains.[1]
These are cytokines that are present naturally in the body. The factors promote neutrophil recovery following anticancer therapy.[1]
The administration of intravenous immunoglobulins (IVIGs) has had some success in treating neutropenias of alloimmune and autoimmune origins with a response rate of about 50%. Blood transfusions have not been effective.[1]
Patients with neutropenia caused by cancer treatment can be given antifungal drugs. A Cochrane review [48] found that lipid formulations of amphotericin B had fewer side effects than conventional amphotericin B, though it is not clear whether there are particular advantages over conventional amphotericin B if given under optimal circumstances. Another Cochrane review [49] was not able to detect a difference in effect between amphotericin B and fluconazole because available trial data analysed results in a way that disfavoured amphotericin B.
Trilaciclib, a CDK4/6 inhibitor, administered approximately thirty minutes before chemotherapy, has been shown in three clinical trials to significantly reduce the occurrence of chemotherapy-induced neutropenia and the associated need for interventions such as the administration of G-CSF's.[50] The drug was approved in February 2021 by the FDA for use in patients with extensive-stage small cell lung cancer.[50]
In November 2023, FDA approved efbemalenograstim alfa.[51]
Prognosis
If left untreated, people with fever and absolute neutrophil count <500 have a mortality of up to 70% within 24 hours.
Epidemiology
Neutropenia is usually detected shortly after birth, affecting 6% to 8% of all newborns in
Furthermore, the prevalence of chronic neutropenia in the general public is rare. In a study conducted in Denmark, over 370,000 people were assessed for the presence of neutropenia. Results published demonstrated only 1% of those evaluated were neutropenic, and were commonly seen in those with HIV, viral infections, acute leukemias, and
See also
References
- ^ ISBN 978-1-4377-2662-6.
- ^ PMID 23953336.
- ^ a b c Neutropenia~clinical at eMedicine
- ^ "Neutropenia". National Center for Biotechnology, National Library of Medicine. Retrieved 8 December 2015.
- ^ "Neutrophils". National Center for Biotechnology, National Library of Medicine. Retrieved 8 December 2015.
- ^ PMID 26554923.
- ^ PMID 23351986.
- PMID 23233578.
- S2CID 24909338.
- ISBN 978-0323086035.
- PMID 28875503.
- PMID 27490698.
- ^ "Aplastic Anemia". The Lecturio Medical Concept Library. Retrieved 1 August 2021.
- PMID 14782741.
- ^ "Evans syndrome". Genetic and Rare Diseases Information Center. Retrieved 17 April 2018.
- ^ "Systemic Lupus Erythematosus". The Lecturio Medical Concept Library. Retrieved 11 August 2021.
- PMID 12730828.
- PMID 24470097.
- S2CID 28782021.
- ^ "Enteric Fever (Typhoid Fever)". The Lecturio Medical Concept Library. 27 August 2020. Retrieved 11 August 2021.
- ^ "Tuberculosis". The Lecturio Medical Concept Library. Retrieved 11 August 2021.
- PMID 26180516.
- S2CID 7429296.
- ^ "Cytomegalovirus". Lecturio. Retrieved 11 August 2021.
- ^ "Penicillamine". The American Society of Health-System Pharmacists. Archived from the original on 21 December 2016. Retrieved 8 December 2016.
- ^ "Sulfonamides and Trimethoprim". The Lecturio Medical Concept Library. Retrieved 11 August 2021.
- ^ "Clozapine". The American Society of Health-System Pharmacists. Archived from the original on 8 December 2015. Retrieved 1 December 2015.
- ^ "Valproic Acid". The American Society of Health-System Pharmacists. Archived from the original on 31 July 2017. Retrieved 23 October 2015.
- ^ "Vaccination". The Lecturio Medical Concept Library. 19 October 2020. Retrieved 11 August 2021.
- ^ "Venclyxto EPAR". European Medicines Agency (EMA). 17 September 2018. Retrieved 1 July 2021.
- ^ ISBN 978-1-4160-0223-9.
- PMID 17379162.
- PMID 27841775.
- PMID 24753205.
- PMID 31720132.
- S2CID 206927525.
- ^ "Types of Neutropenia". neutropenianet.org. Retrieved 29 March 2023.
- ^ "Nadir - What is Chemotherapy? - Chemocare". chemocare.com. Retrieved 29 March 2023.
- ^ "Neutropenia". Cancer.Net. 6 April 2012. Retrieved 29 March 2023.
- ISBN 978-0-443-06377-0.
- ^ "Neutropenic Patients and Neutropenic Regimes | Patient". Patient. Retrieved 8 December 2015.
- ^ S2CID 12535781.
- ^ "Absolute Neutrophil Count Calculator". reference.medscape.com. Retrieved 8 December 2015.
- PMID 17018758.
- PMID 16990357.
- ISBN 9781481602754.
- PMID 21471277.
- PMID 25188673.
- PMID 25188769.
- ^ PMID 34419683.
- FDA. 5 January 2024.
- ^ Neutropenia at eMedicine
- PMID 26791682.

