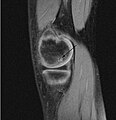
Osteochondritis dissecans
| Osteochondritis dissecans | |
|---|---|
femur head typical of late stage Osteochondritis dissecans. In this case, the lesion was caused by avascular necrosis of the bone just under the cartilage. | |
| Pronunciation | |
| Specialty | Orthopedic surgery |
Osteochondritis dissecans (OCD or OD) is a
OCD is caused by blood deprivation of the secondary physes around the bone core of the femoral condyle. This happens to the epiphyseal vessels under the influence of repetitive overloading of the joint during running and jumping sports. During growth such chondronecrotic areas grow into the subchondral bone. There it will show as bone defect area under articular cartilage. The bone will then possibly heal to the surrounding condylar bone in 50% of the cases. Or it will develop into a pseudarthrosis between condylar bone core and osteochondritis flake leaving the articular cartilage it supports prone to damage. The damage is executed by ongoing sport overload. The result is fragmentation (
Non-surgical treatment is successful in 50% of the cases. If in late stages the lesion is unstable and the cartilage is damaged, surgical intervention is an option as the ability for articular cartilage to heal is limited. When possible, non-operative forms of management such as protected reduced or non-weight bearing and immobilization are used. Surgical treatment includes arthroscopic drilling of intact lesions, securing of cartilage flap lesions with pins or screws, drilling and replacement of cartilage plugs, stem cell transplantation, and in very difficult situation in adults joint replacement. After surgery rehabilitation is usually a two-stage process of unloading and physical therapy. Most rehabilitation programs combine efforts to protect the joint with muscle strengthening and range of motion. During an immobilization period, isometric exercises, such as straight leg raises, are commonly used to restore muscle loss without disturbing the cartilage of the affected joint. Once the immobilization period has ended, physical therapy involves continuous passive motion (CPM) and/or low impact activities, such as walking or swimming.
OCD occurs in 15 to 30 people per 100,000 in the general population each year.
Signs and symptoms
In osteochondritis dissecans, fragments of cartilage or bone become loose within a joint, leading to pain and inflammation. These fragments are sometimes referred to as joint mice.[7] OCD is a type of osteochondrosis in which a lesion has formed within the cartilage layer itself, giving rise to secondary inflammation. OCD most commonly affects the knee, although it can affect other joints such as the ankle or the elbow.[8]
People with OCD report activity-related pain that develops gradually. Individual complaints usually consist of mechanical symptoms including pain, swelling, catching, locking, popping noises, and buckling / giving way; the primary presenting symptom may be a restriction in the range of movement.
Physical examination typically reveals fluid in the joint, tenderness, and
Causes
Despite much research, the
Recent case reports suggest that some people may be genetically predisposed to OCD.[22][23][24] Families with OCD may have mutations in the aggrecan gene.[25] Studies in horses have implicated specific genetic defects.[26]
Pathophysiology

Osteochondritis dissecans differs from "wear and tear" degenerative arthritis, which is primarily an articular surface problem. Instead, OCD is a problem of the bone underlying the cartilage, which may secondarily affect the articular cartilage. Left untreated, OCD can lead to the development of degenerative arthritis secondary to joint incongruity and abnormal wear patterns.[27]
OCD occurs when a loose piece of bone or cartilage partially (or fully) separates from the end of the bone, often because of a loss of blood supply (
In skeletally immature individuals, the blood supply to the
Four minor stages of OCD have been identified after trauma. These include revascularization and formation of granulation (scar) tissue, absorption of necrotic fragments, intertrabecular osteoid deposition, and remodeling of new bone. With delay in the revascularization stage, an OCD lesion develops. A lesion can lead to articular-surface irregularities, which in turn may cause progressive arthritic deterioration.[29]
Diagnosis
To diagnose osteochondritis dissecans, an
Physical examination
Physical examination often begins with examination of the patient's
Next, the examining physician may check for weakness of the
Physical examination of a patient with ankle OCD often returns symptoms of joint effusion,
Diagnostic imaging
X-rays show lucency of the
-
CT scan and projectional radiography of a case of osteochondritis dissecans of parts of the superior-medial talus.
-
Sagittal MRI: Linear low T1 signal at the articular surfaces of the lateral aspects of the medial condyle of the femur confirms the presence of OCD.
Classification
OCD is classified by the progression of the disease in stages. There are two main staging classifications used; one is determined by MRI diagnostic imaging while the other is determined
While the arthroscopic classification of bone and cartilage lesions is considered standard, the Anderson MRI staging is the main form of staging used in this article.[42] Stages I and II are stable lesions. Stages III and IV describe unstable lesions in which a lesion of the cartilage has allowed synovial fluid between the fragment and bone.
| Stage | Evaluation | Findings |
|---|---|---|
| I | Stable | Articular cartilage thickening |
| II | Stable | The articular cartilage is breached; low signal behind the fragment indicates fibrous attachment |
| III | Unstable | The articular cartilage is breached; high signal behind the fragment indicates loss of attachment |
| IV | Unstable | Formation of loose bodies |
| Grade | Findings |
|---|---|
| A | Articular cartilage is smooth and intact but may be soft or ballottable |
| B | Articular cartilage has a rough surface |
| C | Articular cartilage has fibrillations or fissures |
| D | Articular cartilage with a flap or exposed bone |
| E | Loose, nondisplaced osteochondral fragment |
| F | Displaced osteochondral fragment |
Treatment
Treatment options include modified activity with or without weight bearing; immobilization;
- Enhance the healing potential of subchondral bone;
- Fix unstable fragments while maintaining joint congruity; and
- Replace damaged bone and cartilage with implanted tissues or cells that can grow cartilage.
The articular cartilage's capacity for repair is limited:[46] partial-thickness defects in the articular cartilage do not heal spontaneously, and injuries of the articular cartilage which fail to penetrate subchondral bone tend to lead to deterioration of the articular surface.[47] As a result, surgery is often required in even moderate cases where the osteochondral fragment has not detached from the bone (Anderson Stage II, III).[48]
Non-surgical
Candidates for non-operative treatment are limited to skeletally immature teenagers with a relatively small, intact lesion and the absence of loose bodies. Non-operative management may include activity modification, protected weight bearing (partial or non-weight bearing), and immobilization. The goal of non-operative intervention is to promote healing in the subchondral bone and prevent potential chondral collapse, subsequent fracture, and crater formation.[45]
Once candidates for treatment have been screened, treatment proceeds according to the lesion's location. For example, those with OCD of the knee are immobilized for four to six weeks or even up to six months in
Surgery

The choice of surgical versus non-surgical treatments for osteochondritis dissecans is controversial.[51] Consequently, the type and extent of surgery necessary varies based on patient age, severity of the lesion, and personal bias of the treating surgeon—entailing an exhaustive list of suggested treatments. A variety of surgical options exist for the treatment of persistently symptomatic, intact, partially detached, and completely detached OCD lesions. Post-surgery reparative cartilage is inferior to healthy hyaline cartilage in glycosaminoglycan concentration, histological, and immunohistochemical appearance.[52] As a result, surgery is often avoided if non-operative treatment is viable.
Intact lesions
If non-surgical measures are unsuccessful, drilling may be considered to stimulate healing of the subchondral bone.
Hinged lesions
Pins and screws can be used to secure flap (sometimes referred to as hinged) lesions.[55] Bone pegs, metallic pins and screws, and other bioresorbable screws may be used to secure these types of lesions.[56]
Full thickness lesions
The three methods most commonly used in treating full thickness lesions are arthroscopic drilling, abrasion, and microfracturing.
In 1946, Magnusson established the use of stem cells from bone marrow with the first surgical debridement of an OCD lesion. These cells typically differentiate into fibrocartilage and rarely form hyaline cartilage. While small lesions can be resurfaced using this form of surgery, the repair tissue tends to have less strength than normal hyaline cartilage and must be protected for 6 to 12 months. Results for large lesions tend to diminish over time; this can be attributed to the decreased resilience and poor wear characteristics of the fibrocartilage.[57]
In attempts to address the weaker structure of the reparative fibrocartilage, new techniques have been designed to fill the defect with tissue that more closely simulates normal hyaline articular cartilage. One such technique is
Similar to OATS, arthroscopic articular cartilage paste grafting is a surgical procedure offering cost-effective, long-lasting results for stage IV lesions. A bone and cartilage paste derived from crushed plugs of the non-weight-bearing intercondylar notch can achieve pain relief, repair damaged tissue, and restore function.[61]
Unstable lesions
Some methods of fixation for unstable lesions include countersunk compression screws and Herbert screws or pins made of stainless steel or materials that can be absorbed by the body.[62] If loose bodies are found, they are removed. Although each case is unique and treatment is chosen on an individual basis, ACI is generally performed on large defects in skeletally mature people.
Rehabilitation
Continuous passive motion (CPM) has been used to improve healing of the articular surface during the postoperative period for people with full-thickness lesions. It has been shown to promote articular cartilage healing for small (< 3 mm in diameter) lesions in rabbits.[63] Similarly, Rodrigo and Steadman reported that CPM for six hours per day for eight weeks produced an improved clinical outcome in humans.[64]
A rehabilitation program often involves protection of the compromised articular surface and underlying subchondral bone combined with maintenance of strength and range of motion. Post-operative
Prognosis
The prognosis after different treatments varies and is based on several factors which include the age of the patient, the affected joint, the stage of the lesion and, most importantly, the state of the growth plate.[34] It follows that the two main forms of osteochondritis dissecans are defined by skeletal maturity. The juvenile form of the disease occurs in open growth plates, usually affecting children between the ages of 5 and 15 years.[66] The adult form commonly occurs between ages 16 to 50, although it is unclear whether these adults developed the disease after skeletal maturity or were undiagnosed as children.[67]
The prognosis is good for stable lesions (stage I and II) in juveniles with open growth plates; treated conservatively—typically without surgery—50% of cases will heal.[68] Recovery in juveniles can be attributed to the bone's ability to repair damaged or dead bone tissue and cartilage in a process called bone remodeling. Open growth plates are characterized by increased numbers of undifferentiated chondrocytes (stem cells) which are precursors to both bone and cartilaginous tissue. As a result, open growth plates allow for more of the stem cells necessary for repair in the affected joint.[69] Unstable, large, full-thickness lesions (stage III and IV) or lesions of any stage found in the skeletally mature are more likely to fail non-operative treatment. These lesions offer a worse prognosis and surgery is required in most cases.[70][71]
Epidemiology
OCD is a relatively rare disorder, with an estimated incidence of 15 to 30 cases per 100,000 persons per year.[5] Widuchowski W et al. found OCD to be the cause of articular cartilage defects in 2% of cases in a study of 25,124 knee arthroscopies.[72] Although rare, OCD is noted as an important cause of joint pain in active adolescents. The juvenile form of the disease occurs in children with open growth plates, usually between the ages 5 and 15 years and occurs more commonly in males than females, with a ratio between 2:1 and 3:1.[8][73] OCD has become more common among adolescent females as they become more active in sports.[74] The adult form, which occurs in those who have reached skeletal maturity, is most commonly found in people 16 to 50 years old.[70]
While OCD may affect any joint, the knee—specifically the
The oldest case of OCD was identified on the temporo-mandibular joint of the Qafzeh 9 fossil.[80]
History
The condition was initially described by
- Trauma had to be very severe to break off parts of the joint surface.
- Less severe trauma might contuse the bone to cause an area of necrosis which might then separate.
- In some cases, the absence of notable trauma made it likely that there existed some spontaneous cause of separation.
König named the disease "osteochondritis dissecans",
Notable cases
- Michael Russell, American tennis player[89]
- Kristina Vaculik, Canadian artistic gymnast[90][91][92]
- Jonathan Vilma, American football linebacker[93][94]
- Seo In-guk, Korean actor[95][96]
Veterinary aspects

Hematoxylin and eosin staining. Bar = 200 μm.
OCD also is found in animals, and is of particular concern in horses, as there may be a hereditary component in some
In animals, OCD is considered a developmental and metabolic disorder related to cartilage growth and endochondral ossification. Osteochondritis itself signifies the disturbance of the usual growth process of cartilage, and OCD is the term used when this affects joint cartilage causing a fragment to become loose.[100]
According to the Columbia Animal Hospital the frequency of affected animals is dogs, humans, pigs, horses, cattle, chickens, and turkeys, and in dogs the most commonly affected breeds include the German Shepherd, Golden and Labrador Retriever, Rottweiler, Great Dane, Bernese Mountain Dog, and Saint Bernard.
The problem develops in puppyhood although often subclinically, and there may be pain or stiffness, discomfort on extension, or other compensating characteristics. Diagnosis generally depends on X-rays,
Osteochondritis dissecans is difficult to diagnose clinically as the animal may only exhibit an unusual gait. Consequently, OCD may be masked by, or misdiagnosed as, other skeletal and joint conditions such as hip dysplasia.[98]
References
- ^ Shiel Jr WC. "Definition of Osteochondritis dissecans". MedicineNet, Inc. Archived from the original on 7 August 2012. Retrieved 20 February 2009.
- PMID 7273527.
- PMID 1157398.
- ISBN 978-0-8016-0026-5.
- ^ PMID 9012566.
- PMID 1777781. See introduction and discussion sections on incidence
- ^ Hixon AL, Gibbs LM (January 2000). "What Should I Know About Osteochondritis Dissecans?". American Family Physician. 61 (1): 158. Archived from the original on 13 November 2011. Retrieved 29 August 2008.
- ^ PMID 6807595.
- ^ PMID 10643956. Archived from the originalon 6 June 2011. Retrieved 13 September 2008.
- ^ eOrthopod.com. "Adolescent Osteochondritis Dissecans of the Knee". Medical Multimedia Group, LLC. Archived from the original on 1 October 2014. Retrieved 21 September 2008.
- ^ PMID 8613454. Archived from the originalon 7 October 2008.
- PMID 2206181.
- PMID 10513356.
- PMID 4996078.
- ISBN 0-443-08777-6.
- S2CID 12349380. Archived from the original(PFD) on 18 March 2009.
- PMID 622473.
- .
- ^ PMID 18556892.
- ^ S2CID 24877474.
- ^ Patel S, Fried GW, Marone PJ (6 August 2008). "Humeral Capitellum Osteochondritis Dissecans". eMedicine. Medscape. Retrieved 16 November 2008.
- PMID 18929205.
- S2CID 24221990.
- PMID 13475409. Archived from the original(PDF) on 18 March 2009.
- PMID 24698039.
- PMID 18227080.
- S2CID 7392708.
- ^ PMID 17980849.
- ^ a b Jacobs B, Ertl JP, Kovacs G, Jacobs JA. "Knee Osteochondritis Dissecans". eMedicine. Medscape. Retrieved 2 October 2008.
- ^ PMID 12591666. Archived from the original(PDF) on 18 March 2009.
- PMID 3685359.
- PMID 6022357. Archived from the original(PDF) on 29 October 2008.
- S2CID 41405897.
- ^ a b Cooper G, Russell W. "Definition of osteochondritis dissecans". eMedicine. Medscape. Retrieved 18 September 2008.
- S2CID 24221990.
- S2CID 22739728.
- PMID 2009106.
- ^ PMID 2117355.
- PMID 11044029.
- S2CID 41757489.
- ^ eOrthopod.com. "Adolescent Osteochondritis Dissecans of the Elbow" (PDF). Medical Multimedia Group, LLC. Archived from the original (PDF) on 27 October 2007. Retrieved 2 October 2008.
- PMID 10887249.
- ^ Cheng MS, Ferkel RD, Applegate GR (1995). Osteochondral lesion of the talus: A radiologic and surgical comparison. Annual Meeting of the Academy of Orthopaedic Surgeons. New Orleans, LA.
- PMID 10028116.
- ^ PMID 13438964. Archived from the original(PDF) on 29 October 2008.
- S2CID 25130862.
- ^ Bobic V (2000). "Autologous chondrocyte transplantation". Medscape. Retrieved 17 September 2008.
- ^ a b c "Osteochondritis dissecans of the knee". Orthogate. 28 July 2006. Archived from the original (PDF) on 1 July 2016. Retrieved 16 November 2008.
- ^ "Osteochondritis dissecans" (PDF). Société Française d'Orthopédie Pédiatrique. Archived from the original (PDF) on 18 January 2017. Retrieved 21 November 2008.
- ^ "Treating osteochondritis dissecans". Cedars-Sinai Health. Archived from the original on 12 December 2008. Retrieved 22 November 2008.
- S2CID 26460111.
- S2CID 2360001.
- PMID 2768313.
- PMID 9195028.
- PMID 2206180.
- PMID 3665256.
- S2CID 21318642.
- PMID 8078550.
- S2CID 25408760.
- PMID 9875939. Archived from the original(PDF) on 29 October 2008.
- PMID 16517314.
- S2CID 13150540.
- PMID 7440603. Archived from the original(PDF) on 18 March 2009.
- PMID 8590122.
- ^ Jacobs B, Ertl JP, Kovacs G, Jacobs JA (28 July 2006). "Knee Osteochondritis dissecans: treatment & medication". eMedicine. Medscape. Retrieved 14 February 2009.
- ISBN 0-7817-5074-1.
- ISBN 0-07-144831-4.
- S2CID 27786111.
- ISBN 978-0-521-56438-0. Retrieved 20 February 2009.
- ^ PMID 2722949.
- S2CID 21394644.
- PMID 17428666.
- ^ Nagura S (1960). "The so-called osteochondritis dissecans of Konig". Clinical Orthopaedics and Related Research. 18: 100–121.
- PMID 8917149.
- PMID 6501330. Archived from the original(PDF) on 29 October 2008.
- PMID 5562371. Archived from the original(PDF) on 29 October 2008.
- PMID 1015263.
- ^ Cooper G, Warren R (15 May 2008). "Osteochondritis Dissecans". eMedicine. Medscape. Retrieved 16 November 2008.
- PMID 7803070.
- PMID 31351220.
- PMID 20321457.
- PMID 1868560.
- S2CID 40506960.
- PMID 3316236. Archived from the original(PDF) on 18 March 2009.
- S2CID 33781294.
- PMID 15173311.
- ISBN 0-7216-7752-5.
- ISBN 0-443-08836-5.
- ^ Gene Frenette (29 August 2006). "Russell takes his last shot". The Times-Union. Archived from the original on 19 January 2016. Retrieved 13 November 2013.
- ^ "Kristina Vaculik Bio". GoStanford.com. Archived from the original on 13 November 2013. Retrieved 13 November 2013.
- ^ "Interview: Kristina Vaculik (Canada)". International Gymnast Magazine. 24 January 2010. Retrieved 13 November 2013.
- ^ Beverley Smith (28 May 2010). "Olympics in Vaculik's sights". The Globe and Mail. Retrieved 13 November 2013.
- ^ "Jets knew of Jonathan Vilma's knee injury in '04". NY Daily News. 1 November 2007. Retrieved 13 November 2013.
- ^ Tom Rock (13 November 2007). "JETS CHALK TALK: Vilma still secretive on injury". Newsday. Archived from the original on 16 July 2021. Retrieved 13 November 2013.
- ^ "Seo In Guk exempt from his mandatory military service". SBS PopAsia. 15 June 2017. Retrieved 5 December 2019.
- ^ "Seo In-guk returns after controversial military exemption". koreatimes. 20 August 2018. Retrieved 5 December 2019.
- ^ Thomas, Heather Smith (August 2002). "Osteochondritis Dissecans in Thoroughbreds. Weanlings: A Field Study" (PDF). California Thoroughbred: 65–67. Archived from the original (PDF) on 21 October 2006. Retrieved 9 January 2010.
- ^ ISBN 0-397-52098-0. Archived from the originalon 3 July 2017. Retrieved 20 September 2008.
- ^ Pead M, Guthrie S. "Elbow Dysplasia in dogs – a new scheme explained" (PDF). British Veterinary Association (BVA). Archived from the original (PDF) on 2 October 2011. Retrieved 16 July 2010.
- PMID 393676.
- ^ a b "Osteochondrosis, osteochondritis dissecans (OCD)". Category: Canine. Columbia Animal Hospital. n.d. Archived from the original on 25 March 2005. Retrieved 13 September 2008.
External links
- Radiology MR and CT of OCD