Pancreatic islets
| Pancreatic islets | |
|---|---|
 | |
 A pancreatic islet from a mouse in a typical position, close to a blood vessel; insulin in red, nuclei in blue. | |
| Details | |
| Part of | Pancreas |
| System | Endocrine |
| Identifiers | |
| Latin | insulae pancreaticae |
| MeSH | D007515 |
| TA98 | A05.9.01.019 |
| TA2 | 3128 |
| FMA | 16016 |
| Anatomical terms of microanatomy | |
The pancreatic islets or islets of Langerhans are the regions of the
Structure
There are about 1 million islets distributed throughout the pancreas of a healthy adult human. While islets vary in size, the average diameter is about 0.2 mm.[5]:928 Each islet is separated from the surrounding pancreatic tissue by a thin, fibrous, connective tissue capsule which is continuous with the fibrous connective tissue that is interwoven throughout the rest of the pancreas.[5]:928
Microanatomy
Hormones produced in the pancreatic islets are secreted directly into the blood flow by (at least) five types of cells. In rat islets, endocrine cell types are distributed as follows:[6]
- Alpha cells producing glucagon (20% of total islet cells)
- Beta cells producing insulin and amylin (≈70%)
- PP cells (gamma cells or F cells) producing pancreatic polypeptide(<5%)
- Delta cells producing somatostatin (<10%)
- Epsilon cells producing ghrelin (<1%)
It has been recognized that the cytoarchitecture of pancreatic islets differs between species.[7][8][9] In particular, while rodent islets are characterized by a predominant proportion of insulin-producing beta cells in the core of the cluster and by scarce alpha, delta and PP cells in the periphery, human islets display alpha and beta cells in close relationship with each other throughout the cluster.[7][9]
The proportion of beta cells in islets varies depending on the species, in humans it is about 40–50%. In addition to endocrine cells, there are stromal cells (fibroblasts), vascular cells (endothelial cells, pericytes), immune cells (granulocytes, lymphocytes, macrophages, dendritic cells,) and neural cells.[10]
A large amount of blood flows through the islets, 5–6 mL/min per 1 g of islet. It is up to 15 times more than in exocrine tissue of the pancreas.[10]
Islets can influence each other through
-
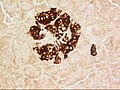
A pancreatic islet, stained.
-
A pancreatic islet, showing alpha cells
-
A pancreatic islet, showing beta cells.
Function
The
- Glucose/Insulin: activates beta cells and inhibits alpha cells.
- Glycogen/Glucagon: activates alpha cells which activates beta cells and delta cells.
- Somatostatin: inhibits alpha cells and beta cells. Also inhibits the secretion of pancreatic polypeptide.[13]
A large number of G protein-coupled receptors (GPCRs) regulate the secretion of insulin, glucagon, and somatostatin from pancreatic islets,[14] and some of these GPCRs are the targets of drugs used to treat type-2 diabetes (ref GLP-1 receptor agonists, DPPIV inhibitors).
-
Mouse islet immunostained for pancreatic polypeptide
-
Mouse islet immunostained for insulin
-
Mouse islet immunostained for glucagon
Electrical activity
Electrical activity of pancreatic islets has been studied using patch clamp techniques. It has turned out that the behavior of cells in intact islets differs significantly from the behavior of dispersed cells.[15]
Clinical significance
Diabetes
The beta cells of the pancreatic islets secrete insulin, and so play a significant role in diabetes. It is thought that they are destroyed by immune assaults.
Because the beta cells in the pancreatic islets are selectively destroyed by an autoimmune process in
People with high body mass index (BMI) are unsuitable pancreatic donors due to greater technical complications during transplantation. However, it is possible to isolate a larger number of islets because of their larger pancreas, and therefore they are more suitable donors of islets.[19]
Islet transplantation only involves the transfer of tissue consisting of beta cells that are necessary as a treatment of this disease. It thus represents an advantage over whole pancreas transplantation, which is more technically demanding and poses a risk of, for example, pancreatitis leading to organ loss.[19] Another advantage is that patients do not require general anesthesia.[20]
Islet transplantation for type 1 diabetes (as of 2008[update]) requires potent immunosuppression to prevent host rejection of donor islets.[21]
The islets are transplanted into a
An alternative source of beta cells, such insulin-producing cells derived from adult stem cells or progenitor cells would contribute to overcoming the shortage of donor organs for transplantation. The field of regenerative medicine is rapidly evolving and offers great hope for the nearest future. However, type 1 diabetes is the result of the autoimmune destruction of beta cells in the pancreas. Therefore, an effective cure will require a sequential, integrated approach that combines adequate and safe immune interventions with beta cell regenerative approaches.[23] It has also been demonstrated that alpha cells can spontaneously switch fate and transdifferentiate into beta cells in both healthy and diabetic human and mouse pancreatic islets, a possible future source for beta cell regeneration.[24] In fact, it has been found that islet morphology and endocrine differentiation are directly related.[25] Endocrine progenitor cells differentiate by migrating in cohesion and forming bud-like islet precursors, or "peninsulas", in which alpha cells constitute the peninsular outer layer and beta cells form later beneath them. Cryopreservation has shown promise to improve the supply chain of pancreatic islets for better transplantation outcomes. [26]
Additional images
-
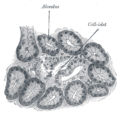
Illustration of dog pancreas. 250x.
Research
See also
- Betatrophin
- Neuroendocrine tumor
- Pancreatic neuroendocrine tumor
- Adrift Just Off the Islets of Langerhans, a novelette by Harlan Ellison
References
- ^ Langerhans P (1869). "Beitrage zur mikroscopischen anatomie der bauchspeichel druse". Inaugural-dissertation. Berlin: Gustav Lange.
- ISBN 978-0-07-160568-7.
- ^ Functional Anatomy of the Endocrine Pancreas
- S2CID 37257345.
- ^ ISBN 978-1-4557-4989-8.)
{{cite book}}:|first=has generic name (help)CS1 maint: multiple names: authors list (link - PMID 7559135.
- ^ PMID 15923354.
- S2CID 234176.
- ^ PMID 16461897.
- ^ PMID 27124642.
- PMID 21372635.
- ISBN 978-0-683-30603-3.
- S2CID 234135648. Retrieved 18 January 2023.
- PMID 23694765.
- PMID 2015391.
- PMID 18081223.
- ^ PMID 17981623.
- PMID 30505878.
- ^ PMID 26824893, retrieved 2020-09-11
- ^ PMID 29394145.
- PMID 18337609.
- S2CID 37483032.
- S2CID 33009393.
- PMID 28380380.
- PMID 30661759.
- ^ Zhan, L., Rao, J.S., Sethia, N. et al. Pancreatic islet cryopreservation by vitrification achieves high viability, function, recovery and clinical scalability for transplantation. Nat Med (2022). https://doi.org/10.1038/s41591-022-01718-1
- PMID 18092149.
- S2CID 36905885.
- PMID 16321437.
- PMID 32075958.
External links
- Pancreas at the Human Protein Atlas