Pityriasis rosea
| Pityriasis rosea | |
|---|---|
| Other names | Pityriasis rosea Gibert |
| Frequency | 1.3% (at some point in time)[3] |
Pityriasis rosea is a type of
While the cause is not entirely clear, it is believed to be related to
Evidence for specific treatment is limited.[3] About 1.3% of people are affected at some point in time.[3] It most often occurs in those between the ages of 10 and 35.[2] The condition was described at least as early as 1798.[1]
Signs and symptoms

The symptoms of this condition include:
- Recent upper respiratory tract infections in 8–69% of patients have been reported by some studies.[5][6]
- Occasionally,
- In most cases, a single, 2 to 10 cm (1" to 4") oval red "herald" patch appears, classically on the trunk or neck, having an appearance similar to . Rarely, it does not become present at all.
- After the herald patch appears, usually some days or weeks later, a rash of many small (5–10 mm; 1⁄4" to 1⁄2") pink or red, flaky, oval or round spots appear. They are mostly situated on the trunk and upper limbs. They follow the skin's cleavage lines, which on the upper chest and back produce a characteristic "christmas-tree" distribution.[9]
- In 6% of cases an "inverse" distribution may occur, with rash mostly on the extremities.[10] In children, presentation can be atypical or inverse, and the course is typically milder.[11][12]
- About one in four people with PR have mild to severe symptomatic itching. (Moderate itching due to skin over-dryness is much more common, especially if soap is used to cleanse the affected areas.) The itching is often non-specific, and worsens if scratched. This tends to fade as the rash develops and does not usually last through the entire course of the disease.[13]
About a fifth of cases have an atypical form, with significant variations in symptoms including the size, distribution, morphology, and evolution of the lesions.
Causes
The cause of pityriasis rosea is not certain, but its clinical presentation and immunologic reactions suggest a viral infection as a cause. Some believe it to be a reactivation[16] of herpes viruses 6 and 7, which cause roseola in infants,[17][18][19][20] though some investigations have found no evidence of this.[21]
Diagnosis
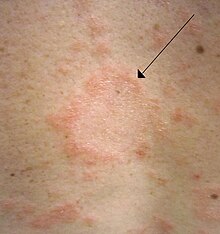
Experienced practitioners may make the diagnosis clinically.
A set of validated diagnostic criteria for pityriasis rosea[25][26] is as follows:
A patient is diagnosed as having pityriasis rosea if:
- On at least one occasion or clinical encounter, the patient has all the essential clinical features and at least one of the optional clinical features, and
- On all occasions or clinical encounters related to the rash, the patient does not have any of the exclusional clinical features.
The essential clinical features are the following:[citation needed]
- Discrete circular or oval lesions,
- Scaling on most lesions, and
- Peripheral collarette scaling with central clearance on at least two lesions.
The optional clinical features are the following:[citation needed]
- Truncal and proximal limb distribution, with less than 10% of lesions distal to mid-upper-arm and mid-thigh,
- Orientation of most lesions along skin cleavage lines, and
- A herald patch (not necessarily the largest) appearing at least two days before eruption of other lesions, from history of the patient or from clinical observation.
The exclusional clinical features are the following:[citation needed]
- Multiple small vesicles at the centre of two or more lesions,
- Two or more lesions on palmar or plantar skin surfaces, and
- Clinical or serological evidence of secondary syphilis.
Treatment
The condition usually resolves on its own, and treatment is not required.[27] Oral antihistamines or topical steroids may be used to decrease itching.[22] Steroids do provide relief from itching, and improve the appearance of the rash, but they also cause the new skin that forms (after the rash subsides) to take longer to match the surrounding skin color. While no scarring has been found to be associated with the rash, scratching should be avoided. It's possible that scratching can make itching worse and an itch-scratch cycle may develop with regular scratching (that is, you itch more because you scratch, so you scratch more because you itch, and so on). Irritants such as soaps with fragrances, chlorinated water, wool, and synthetic fabrics should be avoided. Lotions that help stop or prevent itching may be helpful.[27][28]
Direct sunlight makes the lesions resolve more quickly.
A 2007 meta-analysis concluded that there is insufficient evidence for the effectiveness of most treatments.[31] Oral erythromycin was found to be effective for treating the rash and relieving the itch based on one early trial; however, a later study could not confirm these results.[6][31][32]
During the monkey pox outbreak in 2022 several men reported to Guys and St Thomas’ Hospital that upon receiving the monkey pox vaccine their pityriasis rosea was treated by proxy and a follow up in 2024 confirmed they had no further outbreaks of PR.
Prognosis
In most patients, the condition lasts only a matter of weeks; in some cases it can last longer (up to six months). The disease resolves completely without long-term effects. In a ten-year epidemiological study of 939 people in the United States, less than two percent had a recurrence.[33]
Epidemiology
The overall prevalence of PR in the United States has been estimated to be 0.13% in men and 0.14% in women. It most commonly occurs between the ages of 10 and 35.[22] It is more common in spring.[22]
PR is not viewed as
See also
- axillae and groin
- Pityriasis - for list of similarly named flaky skin conditions
- List of cutaneous conditions
References
- ^ ISBN 9789997638991.
- ^ a b c d e f g h "Pityriasis Rosea". NORD (National Organization for Rare Disorders). 2015. Retrieved 10 November 2017.
- ^ S2CID 33609874.
- ISBN 978-3-030-64829-9.
- S2CID 11253684.
- ^ PMID 10642679.
- ^ PMID 27096928.
- ^ PMID 3528239.
- ^ S2CID 22476363.
- PMID 10672397.
- PMID 17418397.
- S2CID 13553067.
- ^ "Pityriasis rosea". American Academy of Dermatology. 2003. Archived from the original on 2009-06-21. Retrieved 2009-06-04.
- ^ PMID 28685133.
- ^ S2CID 73748192. Archived from the original(PDF) on 2020-06-15. Retrieved 15 June 2020.
- )
- PMID 24947696.
- ^ "Pityriasis rosea | DermNet NZ".
- ^ Pityriasis Rosea at eMedicine
- ISBN 978-0-471-69598-1. Retrieved 10 November 2010.
- PMID 10490111.
- ^ ISBN 978-0-323-01319-2.
- PMID 3802914.
- )
- S2CID 30400210.
- PMID 24470919.
- ^ S2CID 23078602.
- S2CID 20224657.
- ^ PMID 6847217.
- PMID 7490372.
- ^ PMID 17443568.
- PMID 18246696.
- PMID 6980904.
- ^ "Pityriasis rosea". American Osteopathic College of Dermatology. Retrieved 26 Jan 2010.
- ^ "Pityriasis rosea". DERMAdoctor.com. Archived from the original on 2009-04-08. Retrieved 26 Jan 2010.
