Pleural effusion
| Pleural effusion | |
|---|---|
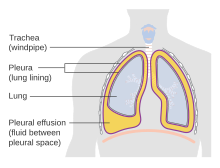 | |
| Diagram of fluid buildup in the pleura | |
| Specialty | Pulmonology |
A pleural effusion is accumulation of excessive fluid in the
Various kinds of fluid can accumulate in the pleural space, such as
Types
Various methods can be used to classify pleural fluid.[1] By the origin of the fluid:
- Serous fluid (hydrothorax)
- haemothorax)
- Chyle (chylothorax)
- pyothorax or empyema)
- Urine (urinothorax)
By pathophysiology:
- Transudative pleural effusion
- Exudative pleural effusion
By the underlying cause (see next section).
Causes

Transudative
The most common causes of
Conditions associated with transudative pleural effusions include:[3]
- Congestive heart failure
- Liver cirrhosis
- Severe hypoalbuminemia
- Nephrotic syndrome
- Acute atelectasis[4]
- Myxedema
- Peritoneal dialysis
- Meigs's syndrome
- Obstructive uropathy
- End-stage kidney disease
Exudative

When a pleural effusion has been determined to be exudative, additional evaluation is needed to determine its cause, and amylase, glucose, pH and cell counts should be measured.
- Red blood cell counts are elevated in cases of bloody effusions (for example after heart surgery or hemothorax from incomplete evacuation of blood).
- Amylase levels are elevated in cases of esophageal rupture, pancreatic pleural effusion, or cancer.
- Glucose is decreased with cancer, bacterial infections, or rheumatoid pleuritis.
- pH is low in empyema (<7.2) and maybe low in cancer.
- If cancer is suspected, the pleural fluid is sent for cytology. If cytology is negative, and cancer is still suspected, either a thoracoscopy, or needle biopsy[5]of the pleura may be performed.
- Gram stainingand culture should also be done.
- If tuberculosis is possible, examination for Mycobacterium tuberculosis (either a Ziehl–Neelsen or Kinyoun stain, and mycobacterial cultures) should be done. A polymerase chain reaction for tuberculous DNA may be done, or adenosine deaminase or interferon gamma levels may also be checked.
The most common causes of exudative pleural effusions are bacterial pneumonia, cancer (with lung cancer, breast cancer, and lymphoma causing approximately 75% of all malignant pleural effusions), viral infection, and pulmonary embolism.
Another common cause is after heart surgery when incompletely drained blood can lead to an inflammatory response that causes exudative pleural fluid.
Conditions associated with exudative pleural effusions:[3]
- Parapneumonic effusion due to pneumonia
- Malignancy (either lung cancer or metastases to the pleura from elsewhere)
- Infection (empyema due to bacterial pneumonia)
- Trauma
- Pulmonary infarction
- Pulmonary embolism
- Autoimmune disorders
- Pancreatitis
- Ruptured esophagus (Boerhaave's syndrome)
- Rheumatoid pleurisy
- Drug-induced lupus
Other/ungrouped
Other causes of pleural effusion include
Pleural effusions may also occur through medical or surgical interventions, including the use of medications (pleural fluid is usually eosinophilic), coronary artery bypass surgery, abdominal surgery, endoscopic variceal sclerotherapy, radiation therapy, liver or lung transplantation, insertion of ventricular shunt as a treatment method of hydrocephalus,[7][8] and intra- or extravascular insertion of central lines.[citation needed]
Pathophysiology
Pleural fluid is secreted by the parietal layer of the
Diagnosis

A pleural effusion is usually diagnosed on the basis of
Imaging
A pleural effusion appears as an area of whiteness on a standard posteroanterior chest X-ray.
Chest computed tomography is more accurate for diagnosis and may be obtained to better characterize the presence, size, and characteristics of a pleural effusion. Lung ultrasound, nearly as accurate as CT and more accurate than chest X-ray, is increasingly being used at the point of care to diagnose pleural effusions, with the advantage that it is a safe, dynamic, and repeatable imaging modality.[15] To increase diagnostic accuracy of detection of pleural effusion sonographically, markers such as boomerang and VIP signs can be utilized.[16]
-
Massive left-sided pleural effusion (whiteness) in a patient presenting with lung cancer.
-
CT scan of the chest showing a left-sided pleural effusion. The fluid usually settles at the lowest space due to gravity; in this case, at the back because the patient is supine.
-
The lung expanding within an area of pleural effusion as seen by ultrasound
-
malignant mesothelioma, one cause of a pleural effusion.
-
A pleural effusion as seen on lateral upright chest x-ray
-
Pleural effusion as seen behind the heart.[17]
-
Massive pleural effusion, later proven to be hemothorax in a South Indian male.
Thoracentesis
Once a pleural effusion is diagnosed, its cause must be determined. Pleural fluid is drawn out of the pleural space in a process called thoracentesis, and it should be done in almost all patients who have pleural fluid that is at least 10 mm in thickness on CT, ultrasonography, or lateral decubitus X-ray and that is new or of uncertain etiology. In general, the only patients who do not require thoracentesis are those who have heart failure with symmetric pleural effusions and no chest pain or fever; in these patients, diuresis can be tried, and thoracentesis is avoided unless effusions persist for more than 3 days.[18] In a thoracentesis, a needle is inserted through the back of the chest wall in the sixth, seventh, or eighth intercostal space on the midaxillary line, into the pleural space. The use of ultrasound to guide the procedure is now standard of care as it increases accuracy and decreases complications.[19][20] After removal, the fluid may then be evaluated for:
- Chemical composition including protein, lactate dehydrogenase (LDH), albumin, amylase, pH, and glucose
- Gram stain and culture to identify possible bacterial infections
- White and red blood cell counts and differential white blood cell counts
- Cytopathology to identify cancer cells, but may also identify some infective organisms
- Other tests as suggested by the clinical situation – immunoglobulins
Light's criteria
| Transudate vs. exudate | ||
|---|---|---|
| Transudate | Exudate | |
| Main causes | ↑ colloid
osmotic pressure |
Inflammation-Increased vascular permeability |
| Appearance | Clear[21] | Cloudy[21] |
Specific gravity |
< 1.012 |
> 1.020
|
| Protein content | < 2.5 g/dL |
> 2.9 g/dL[22]
|
| fluid protein/ serum protein |
< 0.5 | > 0.5[23] |
| SAAG = Serum [albumin] - Effusion [albumin] |
> 1.2 g/dL | < 1.2 g/dL[24] |
| fluid LDH upper limit for serum |
< 0.6 or < 2⁄3 | > 0.6[22] or > 2⁄3[23] |
| Cholesterol content | < 45 mg/dL | > 45 |
| Radiodensity on CT scan | 2 to 15 HU[25] | 4 to 33 HU[25] |

Definitions of the terms "transudate" and "exudate" are the source of much confusion. Briefly, transudate is produced through pressure filtration without capillary injury while exudate is "inflammatory fluid" leaking between cells.[27]
Transudative pleural effusions are defined as effusions that are caused by systemic factors that alter the pleural equilibrium, or Starling forces. The components of the Starling forces – hydrostatic pressure, permeability, and oncotic pressure (effective pressure due to the composition of the pleural fluid and blood) – are altered in many diseases, e.g., left ventricular failure, kidney failure, liver failure, and cirrhosis. Exudative pleural effusions, by contrast, are caused by alterations in local factors that influence the formation and absorption of pleural fluid (e.g., bacterial pneumonia, cancer, pulmonary embolism, and viral infection).[28]
An accurate diagnosis of the cause of the effusion, transudate versus exudate, relies on a comparison of the chemistries in the pleural fluid to those in the blood, using Light's criteria. According to Light's criteria (Light, et al. 1972), a pleural effusion is likely exudative if at least one of the following exists:[29]
- The ratio of pleural fluid protein to serum protein is greater than 0.5
- The ratio of pleural fluid LDH and serum LDH is greater than 0.6
- Pleural fluid LDH is greater than 0.6 [22] or 2⁄3[29] times the normal upper limit for serum. Different laboratories have different values for the upper limit of serum LDH, but examples include 200[30] and 300[30] IU/l.[31]
The sensitivity and specificity of Light's criteria for detection of exudates have been measured in many studies and are usually reported to be around 98% and 80%, respectively.[32][33] This means that although Light's criteria are relatively accurate, twenty percent of patients that are identified by Light's criteria as having exudative pleural effusions actually have transudative pleural effusions. Therefore, if a patient identified by Light's criteria as having an exudative pleural effusion appears clinically to have a condition that usually produces transudative effusions, additional testing is needed. In such cases, albumin levels in blood and pleural fluid are measured. If the difference between the albumin level in the blood and the pleural fluid is greater than 1.2 g/dL (12 g/L), this suggests that the patient has a transudative pleural effusion.[24] However, pleural fluid testing is not perfect, and the final decision about whether a fluid is a transudate or an exudate is based not on chemical analysis of the fluid, but an accurate diagnosis of the disease that produces the fluid.[27] The traditional definitions of transudate as a pleural effusion due to systemic factors and an exudate as a pleural effusion due to local factors have been used since 1940 or earlier (Light et al., 1972). Previous to Light's landmark study, which was based on work by Chandrasekhar, investigators unsuccessfully attempted to use other criteria, such as specific gravity, pH, and protein content of the fluid, to differentiate between transudates and exudates. Light's criteria are highly statistically sensitive for exudates (although not very statistically specific). More recent studies have examined other characteristics of pleural fluid that may help to determine whether the process producing the effusion is local (exudate) or systemic (transudate). The table above illustrates some of the results of these more recent studies. However, it should be borne in mind that Light's criteria are still the most widely used criteria.[citation needed]
The Rational Clinical Examination Series review found that bilateral effusions, symmetric and asymmetric, are the most common distribution in heart failure (60% of effusions in heart failure will be bilateral). When there is asymmetry in heart failure-associated pleural effusions (either unilateral or one side larger than the other), the right side is usually more involved than the left.[11] The instruments pictured are accurately shaped, however, most hospitals now use safer disposable trocars. Because these are single use, they are always sharp and have a much smaller risk of cross patient contamination.[citation needed]
Treatment
Treatment depends on the underlying cause of the pleural effusion.
Therapeutic aspiration may be sufficient; larger effusions may require insertion of an
Pleurodesis fails in as many as 30% of cases. An alternative is to place a PleurX Pleural Catheter or Aspira Drainage Catheter. This is a 15Fr chest tube with a one-way valve. Each day the patient or caregivers connect it to a simple vacuum tube and remove from 600 to 1000 mL of fluid, and can be repeated daily. When not in use, the tube is capped. This allows patients to be outside the hospital. For patients with malignant pleural effusions, it allows them to continue chemotherapy if indicated. Generally, the tube is in for about 30 days, and then it is removed when space undergoes spontaneous pleurodesis.
Tubercular pleural effusion is one of the common extrapulmonary forms of tuberculosis. Treatment consists of antituberculosis treatment (ATT). The currently recommended ATT regime is two months of isoniazid, rifampicin, ethambutol and pyrazinamide followed by four months of isoniazid, rifampicin and ethambutol.[34]
See also
- Pleural disease
- Empyema
- Heart failure
- Pulmonary embolism
- Subpulmonic effusion
- Thoracentesis
- pneumothorax
References
- ^ "Pleural effusion". U.S. National Library of Medicine. Retrieved 2 July 2021.
- S2CID 44337698.
- ^ a b Galagan et al. Color Atlas of Body Fluids. CAP Press, Northfield, 2006
- ^ "Atelectasis". The Lecturio Medical Concept Library. Retrieved 2 July 2021.
- PMID 9228404.[permanent dead link]
- ^ PMID 31315808.
- S2CID 28016135.
- ^ Raicevic Mirjana, Nikolovski Srdjan, Golubovic Emilija. Pleural Effusion as a Ventriculo-Peritoneal Shunt Complication in Children (Meeting Abstract). Acta Med Acad. 2019;48(S1):26.
- PMID 16623208.
- PMID 25077579.
- ^ PMID 19155458.
- ISBN 0-443-07008-3.
- ISBN 0-674-01279-8.
- ^ Bell DJ, Jones J. "Pleural effusion". Radiopaedia. Retrieved July 20, 2021.
- PMID 22392031.
- S2CID 41876899.
- ^ "UOTW #23 - Ultrasound of the Week". Ultrasound of the Week. 22 October 2014. Retrieved 27 May 2017.
- ^ Light, Richard W. "Pleural Effusion". Merck Manual for Health Care Professionals. Merck Sharp & Dohme Corp. Retrieved 21 August 2013.
- S2CID 21367134.
- PMID 20177035.
- ^ a b The University of Utah • Spencer S. Eccles Health Sciences Library > WebPath images > "Inflammation".
- ^ PMID 9106577.
- ^ PMID 4642731.
- ^ PMID 2152757.
- ^ PMID 24100060.
- PMID 9228404.
- ^ PMID 4642731. Retrieved 20 July 2021.
- ^ Light, Richard W. "Ch. 257: Disorders of the Pleura and Mediastinum". In Fauci AS, Braunwald E, Kasper DL, Hauser SL, Longo DL, Jameson JL, Loscalzo J (eds.). Harrison's Principles of Internal Medicine (17th ed.).
- ^ S2CID 31947040.
- ^ PMID 11641512.
- PMID 11914151.

- S2CID 45667293.
- PMID 16510093.
- ISBN 9789241550529. Archived from the originalon March 20, 2019. Retrieved 5 September 2021.
External links
- MedlinePlus Encyclopedia: Pleural Effusion
- Pleural Effusion Images from MedPix





