Pleural cavity
| Pleural cavity | |
|---|---|
 The pleural cavity is the potential space between the pleurae of the pleural sac that surrounds each lung. | |
| Details | |
| Precursor | intraembryonic coelom |
| Identifiers | |
| Latin | cavum pleurae, cavum pleurale, cavitas pleuralis |
| MeSH | D035422 |
| TA98 | A07.1.01.001 |
| TA2 | 3316 |
| TH | H3.05.03.0.00013 |
| FMA | 9740 |
| Anatomical terminology | |
The pleural cavity, pleural space, or intrapleural space is the
The serous membrane that covers the surface of the lung is the
Structure
In
The visceral pleura receives its blood supply from the
The visceral pleurae are innervated by
Development
During the third week of
The
The tissue separating the newly formed pleural cavities from the pericardial cavity are known as the pericardiopleural membranes, which later become the side walls of the
Function
The pleural cavity, with its associated pleurae, aids optimal functioning of the lungs during
Pleural fluid
Pleural fluid is a
Pleural fluid circulation
The hydrostatic equilibrium model, viscous flow model and capillary equilibrium model are the three hypothesised models of circulation of pleural fluid.[7]
According to the viscous flow model, the intra pleural pressure gradient drives a downward viscous flow of pleural fluid along the flat surfaces of ribs.The capillary equilibrium model states that the high negative apical pleural pressure leads to a basal-to-apical gradient at the mediastinal pleural surface, leading to a fluid flow directed up towards the apex (helped by the beating heart and ventilation in lungs).Thus the recirculation of fluid occurs. Finally there's a traverse flow from margins to flat portion of ribs completes the fluid circulation.[8][9]
Absorption occurs into lymphatic vessels at the level of the diaphragmatic pleura.[10]
Clinical significance
Pleural effusion
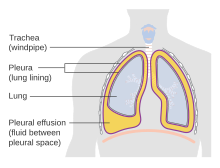
A pathologic collection of pleural fluid is called a pleural effusion. Mechanisms:
- Lymphatic obstruction
- Increased capillary permeability
- Decreased plasma colloid osmotic pressure
- Increased capillary venous pressure
- Increased negative intrapleural pressure
Pleural effusions are classified as exudative (high protein) or transudative (low protein). Exudative pleural effusions are generally caused by infections such as pneumonia (parapneumonic pleural effusion), malignancy, granulomatous disease such as tuberculosis or coccidioidomycosis, collagen vascular diseases, and other inflammatory states. Transudative pleural effusions occur in congestive heart failure (CHF), cirrhosis or nephrotic syndrome.
Localized pleural fluid effusion noted during pulmonary embolism (PE) results probably from increased capillary permeability due to cytokine or inflammatory mediator release from the platelet-rich thrombi.[11]
| Transudate[12] | Exudative causes[12] |
|---|---|
* Congestive heart failure (CHF)
|
* Malignancy
|
Pleural fluid analysis
When accumulation of pleural fluid is noted, cytopathologic evaluation of the fluid, as well as clinical microscopy, microbiology, chemical studies, tumor markers, pH determination and other more esoteric tests are required as diagnostic tools for determining the causes of this abnormal accumulation. Even the gross appearance, color, clarity and odor can be useful tools in diagnosis. The presence of heart failure, infection or malignancy within the pleural cavity are the most common causes that can be identified using this approach.[13]
Gross appearance
- Clear straw-colored: If transudative, no further analysis needed. If exudative, additional studies needed to determine cause (cytology, culture, biopsy).
- Cloudy, purulent, turbid: Infection, empyema, pancreatitis, malignancy.
- Pink to red/bloody: Traumatic tap, malignancy, pulmonary infarction, intestinal infarction, pancreatitis, trauma.
- Green-white, turbid: Rheumatoid arthritis with pleural effusion.
- Green-brown: Biliary disease, bowel perforation with ascites.
- Milky-white or yellow and bloody: Chylous effusion.
- Milky or green, metallic sheen: Pseudochylous effusion.
- Viscous (hemorrhagic or clear): Mesothelioma.
- Anchovy-paste (or 'chocolate sauce'): Ruptured amoebic liver abscess.[12]
Microscopic appearance
Microscopy may show resident cells (mesothelial cells, inflammatory cells) of either benign or malignant etiology. Evaluation by a cytopathologist is then performed and a morphologic diagnosis can be made. Neutrophils are numerous in pleural empyema. If lymphocytes predominate and mesothelial cells are rare, this is suggestive of tuberculosis. Mesothelial cells may also be decreased in cases of rheumatoid pleuritis or post-pleurodesis pleuritis. Eosinophils are often seen if a patient has recently undergone prior pleural fluid tap. Their significance is limited.[14]
If malignant cells are present, a pathologist may perform additional studies including immunohistochemistry to determine the etiology of the malignancy.
Chemical analysis
Chemistry studies may be performed including pH, pleural fluid:serum protein ratio, LDH ratio, specific gravity, cholesterol and bilirubin levels. These studies may help clarify the etiology of a pleural effusion (exudative vs transudative). Amylase may be elevated in pleural effusions related to gastric/esophageal perforations, pancreatitis or malignancy. Pleural effusions are classified as exudative (high protein) or transudative (low protein).
In spite of all the diagnostic tests available today, many pleural effusions remain
Disease
Diseases of the pleural cavity include:
- Pneumothorax: a collection of air within the pleural cavity
- Pleural effusion: a fluid accumulation within the pleural space.
- Pleural tumors: abnormal growths on the pleurae.
See also
- Coin test, medical diagnostic test for a punctured lung
References
- ^ OCLC 780984149.
- OCLC 902010725.
- ^ Light 2007, p. 1.
- PMID 20956149.
- PMID 12503717.
- ISBN 978-0072827415.
- PMID 28523153.
- OCLC 949753083.
- PMID 15044678.
- PMID 30069369.
- S2CID 44337698.
- ^ OCLC 78070199.
- OCLC 1239350014.
- ^ De Mais, Daniel. ASCP Quick Compendium of Clinical Pathology, 2nd. Ed. ASCP Press, Chicago, 2009.
Sources
- Light, Richard W. (2007). Pleural Diseases. Lippincott Williams & Wilkins. ISBN 978-0781769570.
External links
- Photo of dissection at kenyon.edu
