Polyp (medicine)
This article needs additional citations for verification. (December 2020) |
| Polyp | |
|---|---|
 | |
| Polyp of sigmoid colon as revealed by colonoscopy. Approximately 1 cm in diameter. The polyp was removed by snare cautery. | |
| Specialty | Pathology |
In
The name is of ancient origin, in use in English from about 1400 for a nasal polyp, from Latin polypus through Greek.[1] The animal of similar appearance called polyp is attested from 1742, although the word was earlier used for an octopus.
Digestive polyps
Relative incidences by location:
-
Incidences and malignancy risks of various types ofcolorectal polyps[2]
-
Relative incidences of gastric polyps[3]
| Polyp | Typical location | Histologic appearance | Risk of malignancy | Picture | Syndromes |
|---|---|---|---|---|---|
| Hyperplastic polyp | Colorectal (unless otherwise specified) | Serrated unbranched crypts | if polyps are more than 100 |  |
Serrated polyposis syndrome |
| Hyperplastic polyp of the stomach | Stomach | Elongated, tortuous, and cystic foveolae separated by edematous and inflamed stroma.[4] | 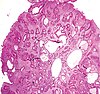 |
Gastric hyperplastic polyposis | |
| Fundic gland polyp | Fundus of stomach | Cystically dilated glands lined by chief cells, parietal cells and mucinous foveolar cells.[5] | Very low or none, when sporadic.[6] |  |
Fundic gland polyposis |
Sessile serrated adenoma
|
Colorectal | Similar to hyperplastic with hyperserration, dilated/branched crypt base, prominent mucin cells at crypt base | Yes |  |
Serrated polyposis syndrome |
| Inflammatory | Non-specific | Raised mucosa/submucosa with inflammation | If dysplasia develops | Inflammatory bowel disease, ulcers, infections, mucosal prolapse | |
| Tubular Adenoma (Villous, Tubulovillous) | Colorectal | Tubular glands with elongated nuclei (at least low-grade atypia) | Yes | 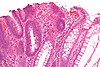 |
|
| Traditional serrated adenoma | Colorectal | Serrated crypts, often villous architecture, with cytologic atypia, eosinophilic cells | Yes | 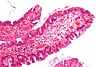 |
Serrated polyposis syndrome |
| Peutz-Jeghers Polyp | All digestive tract | Smooth muscle bundles between nonneoplastic epithelium, "Christmas tree" appearance | No |  |
Peutz–Jeghers syndrome |
| Juvenile Polyp | Upper GI tract and colon | Cystically dilated glands with expanded lamina propria | Not inherently, may develop dysplasia |  |
Juvenile polyposis syndrome, identical polyps in Cronkhite–Canada syndrome |
| Hamartomatous Polyp (Cowden Syndrome) | Mainly colorectal | Variable; classical mildly fibrotic polyp with disorganized mucosa and splaying of muscularis mucosae; also inflammatory, juvenile, lipoma, ganglioneuroma, lymphoid | No | Cowden syndrome | |
| Inflammatory fibroid polyp | All digestive tract | Spindle cells with concentric arrangements of spindle cells around blood vessels and inflammation rich in eosinophils
|
none |  |
Colorectal polyp
While colon polyps are not commonly associated with symptoms, occasionally they may cause
Most colon polyps can be categorized as sporadic.
Inherited polyposis syndromes

- Familial adenomatous polyposis[13]
- Peutz–Jeghers syndrome
- Turcot syndrome
- Juvenile polyposis syndrome
- Cowden disease
- Bannayan–Riley–Ruvalcaba syndrome (Bannayan–Zonana syndrome)
- Gardner's syndrome
- Serrated polyposis syndrome
Non-inherited polyposis syndromes
Types of colon polyps
- Malignant
- Hamartomatous
- Hyperplastic
- Inflammatory: Inflammatory fibroid polyp
Adenomatous polyps
Adenomatous polyps, or adenomas, are polyps that grow on the lining of the colon and which carry a high risk of
About 5% of people aged 60 will have at least one adenomatous polyp of 1 cm diameter or greater.
Types
Adenomas constitute approximately 10% of digestive polyps. Most polyps (approximately 90%) are small, usually less than 1 cm in diameter, and have a small potential for malignancy. The remaining 10% of adenomas are larger than 1 cm and approach a 10% chance of containing invasive cancer.[17]
There are three types of adenomatous polyp:
- Tubular adenomas (tube-like shape) are the most common of the adenomatous polyps; they may occur everywhere in the colon and they are the least likely colon polyps to develop into colon cancer
- Tubulovillous
- Villous adenomas are commonly found in the rectal area and they are normally larger in size than the other two types of adenomas. They tend to be non-pedunculated, velvety, or cauliflower-like in appearance and they are associated with the highest morbidity and mortality rates of all polyps. They can cause hypersecretory syndromes characterized by hypokalemia and profuse mucous discharge, and can harbor carcinoma in situor invasive carcinoma more frequently than other adenomas.
Risks
The risks of progression to colorectal cancer increase if the polyp is larger than 1 cm and contains a higher percentage of
Although polyps do not carry significant risk of
It is estimated that an individual whose parents have been diagnosed with an adenomatous polyp has a 50% greater chance to develop colon cancer than individuals with no
Screening
Screening for colonic polyps as well as preventing them has become an important part of the management of the condition. Medical societies have established guidelines for colorectal screening in order to prevent adenomatous polyps and to minimize the chances of developing colon cancer. It is believed that some changes in the diet might be helpful in preventing polyps from occurring, but there is no other way to prevent the polyps from developing into cancerous growths than detecting and removing them.[citation needed]
Colon polyps as they grow can sometimes cause bleeding within the
It has been statistically demonstrated that screening programs are effective in reducing the number of deaths caused by colon cancer due to adenomatous polyps. The risk of complications associated with colonoscopies is approximately 0.35 percent, compared to a lifetime risk of developing colon cancer of around 6 percent.[23] As there is a small likelihood of recurrence, surveillance after polyp removal is recommended.[citation needed]
Endometrial polyp
An endometrial polyp or uterine polyp is a polyp or
Cervical polyp
A cervical polyp is a common
Nasal polyps
Nasal polyps are polypoidal masses arising mainly from the
Laryngeal polyps
Polyps on the vocal folds can take on many different forms, and can sometimes result from vocal abuse, although this is not always the cause. They can occur on one or both vocal folds, and appear as swelling, a bump (similar to a nodule), a stalk-like growth, or a blister-like lesion. Most polyps are larger than nodules, which are more similar to callouses on the vocal folds. Polyps and nodules can exhibit similar symptoms including hoarseness or breathiness, "rough" or "scratchy" voice, harshness in vocal quality, shooting pain from ear to ear, sensation of having "a lump in the back of the throat", neck pain, decreased pitch range in the voice, and vocal and bodily fatigue.[citation needed]
If an individual experiences symptoms for more than 2 to 3 weeks, they should see a physician. For a diagnosis, a thorough evaluation of the voice should include a physical examination, preferably by an otolaryngologist (ear, nose, and throat doctor) who specializes in voice, a voice evaluation with a speech-language pathologist (SLP), a neurological examination (in certain cases) The qualities of the voice that will be evaluated include quality, pitch, loudness, and ability to sustain voicing. In some cases, an instrumental examination may be performed with an endoscope into the mouth or nose; this gives a clear look at the vocal folds and larynx in general. In addition to this, a stroboscope (flashing light) may be used to observe the movement of the vocal folds during speech.[citation needed]
Polyps may be treated with medical, surgical, or behavioral intervention. Surgical intervention involves removing the polyp from the vocal fold. This approach is only used when the growth(s) are very large or have existed for an extended amount of time. In children, surgical intervention is rare. Existing medical problems may be treated in an effort to reduce the strain and negative impact on the vocal cords. This could include treatment for gastrointestinal reflux disease, allergies, and thyroid problems. Intervention to stop smoking and reduce stress may also be needed. Most people receive behavioral intervention, or vocal therapy, from an SLP. This might involve teaching good vocal hygiene, and reducing or stopping vocal abuse behaviors. Direct voice treatments may be used to alter pitch, loudness, or breathe support to promote good voicing.[citation needed]
Footnotes
- ^ "polyp". Oxford English Dictionary (Online ed.). Oxford University Press. (Subscription or participating institution membership required.)
- ^ References for diagram are located at: Commons:Template:Pie chart of colorectal polyp etiologies - Source.
- PMID 21867351.
- ^ Naziheh Assarzadegan, M.D., Raul S. Gonzalez, M.D. "Stomach Polyps – Fundic gland polyp". PathologyOutlines.
{{cite web}}: CS1 maint: multiple names: authors list (link) Topic Completed: 1 November 2017. Minor changes: 11 December 2019 - ^ Varocha Mahachai, MDDavid Y Graham, MDRobert D Odze, MD, FRCPC. "Gastric polyps". UpToDate.
{{cite web}}: CS1 maint: multiple names: authors list (link) Literature review current through: Sep 2020. | This topic last updated: Feb 14, 2019. - ^ Fletcher's Diagnostic Histopathology of Tumors, 3rd Ed..
- ^ Sternberg's Diagnostic Surgical Pathology, 5th Ed.
- ^ "Colonic Polyps". medlineplus.gov. Retrieved 2020-04-30.
- ^ "Colon polyps – Symptoms and causes". Mayo Clinic. Retrieved 2020-04-30.
- ^ ABIM Foundation, American Gastroenterological Association, archived from the original(PDF) on August 9, 2012, retrieved August 17, 2012
- PMID 7408789.
- ^ a b "Familial Adenomatous Polyposis". The Lecturio Medical Concept Library. Retrieved 22 July 2021.
- ^ "Adenomatous Polyps". Archived from the original on 2010-02-06. Retrieved 2010-04-13.
- ^ "Colon Cancer Treatment (PDQ®)". NCI. May 12, 2014. Archived from the original on July 5, 2014. Retrieved June 29, 2014.
- ^ "Polyps in the colon (large bowel)". Retrieved 2010-04-13.
- ^ "Colonic Polyps". Retrieved 2010-04-13.
- ^ "Management of Colonic Polyps and Adenomas". Retrieved 2010-04-13.
- PMID 31985973, retrieved 2023-03-31
- ^ "Colon Polyps (cont.)". Retrieved 2010-06-25.
- PMID 12557158.
- ^ "Adenomatous Polyps Symptoms and Prevention". Archived from the original on 2012-04-05. Retrieved 2010-06-25.
- ^ "Colonoscopy Risks". Archived from the original on 2012-11-18. Retrieved 2010-06-25.
- ^ ISBN 978-1-900151-51-1.
- ^ a b "Uterine polyps". MayoClinic.com. 2006-04-27. Retrieved 2007-10-20.
- ISBN 0-7817-4051-7.
- ^ "Dysmenorrhea: Menstrual abnormalities". Merck Manual of Diagnosis and Therapy. 2005. Retrieved 2007-10-20.
- ISBN 3-7186-5857-7.
- ISBN 978-1-900151-51-1.
External links
- National Institutes of Health polyp website
- Thorough review of polyposis syndromes by Dr. Ali Nawaz Khan with CME available
- "How I Do It" – Removing large or sessile colonic polyps. Dr. Brian Saunders MD FRCP; St. Mark's Academic Institute; Harrow, Middlesex, UK. Retrieved April 9, 2008.
- FAP Patient Information Sheet


