Portal vein thrombosis
| Portal vein thrombosis | |
|---|---|
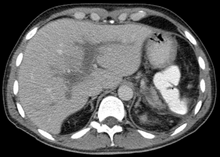 | |
| Portal vein thrombosis seen with computed tomography. | |
| Specialty | Angiology |
Portal vein thrombosis (PVT) is a vascular disease of the liver that occurs when a
An equivalent clot in the vasculature that exits the liver carrying deoxygenated blood to the
Signs and symptoms
Portal vein thrombosis causes upper abdominal pain, possibly accompanied by nausea and an enlarged liver and/or spleen; the abdomen may be filled with fluid (ascites).[3] A persistent fever may result from the generalized inflammation.[1] While abdominal pain may come and go if the thrombus forms suddenly, long-standing clot build-up can also develop without causing symptoms, leading to portal hypertension before it is diagnosed.[4][2]
Other symptoms can develop based on the cause. For example, if portal vein thrombosis develops due to liver cirrhosis, bleeding or other signs of liver disease may be present. If portal vein thrombosis develops due to pylephlebitis, signs of infection such as fever, chills, or night sweats may be present.[citation needed]
Causes
Slowed blood flow due to underlying
Alternatively, the portal vein may be injured as a result of pancreatitis, diverticulitis, cholangiocarcinoma, hepatocellular carcinoma (HCC), or abdominal surgery/trauma.[3] Red flags for cancerous growth as a cause are elevated alpha fetoprotein levels, portal vein diameter greater than 2.3 cm, pulsatility on Doppler ultrasound imaging, or hyperintense hepatic arterial phase (HAP) on CT scan with contrast.[1]
PVT is also a known complication of surgical removal of the spleen.[7] During the last several years, myeloproliferative neoplasms (MPNs) have emerged as a leading systemic cause of splanchnic vein thromboses (which include PVT).[citation needed]
Mechanism
The main portal vein is formed by the union of the
An infected thrombus may become septic, known as pylephlebitis; if blood cultures are positive for growth at this time, the most common organism is Bacteroides.[1]
Diagnosis

The diagnosis of portal vein thrombosis is usually made with imaging confirming a clot in the portal vein;
On duplex ultrasound, demonstration of echogenic material within the portal vein, complete or partial absence of colour flow in the portal vein, presence of collateral vessels around the portal vein or gall bladder that bypass the portal vein. [9]

Treatment
Treatment is aimed at opening the blocked veins to minimize complications; the duration of clot (acute versus chronic) affects treatment. Unless there are underlying reasons why it would be harmful,
Different considerations are made in the management of PVT in pediatric patients or those who have already received a liver transplant.[1]
See also
References
- ^ PMID 19399912.
- ^ a b O'Mara SR, Wiesner L. "Hepatic Disorders". In Tintinalli JE, Ma O, Yealy DM, Meckler GD, Stapczynski J, Cline DM, Thomas SH (eds.). Tintinalli's Emergency Medicine: A Comprehensive Study Guide (9 ed.). New York, NY: McGraw-Hill.
- ^ PMID 31895720.
- S2CID 7518468.
- ^ PMID 25284616.
- ^ a b Bacon BR. "Cirrhosis and Its Complications". In Jameson J, Fauci AS, Kasper DL, Hauser SL, Longo DL, Loscalzo J (eds.). Harrison's Principles of Internal Medicine (20 ed.). New York, NY: McGraw-Hill.
- PMID 18456028.
- ^ Friedman LS (2020). "Noncirrhotic Portal Hypertension". In Papadakis MA, McPhee SJ, Rabow MW (eds.). Current Medical Diagnosis and Treatment 2020. McGraw-Hill.
- PMID 23396402.
