Prothrombin time
| Prothrombin time | |
|---|---|
 Blood plasma after the addition of tissue factor. The gel-like structure is strong enough to hold a steel ball. | |
| MeSH | D011517 |
The prothrombin time (PT) – along with its derived measures of prothrombin ratio (PR) and international normalized ratio (INR) – is an
PT is often used in conjunction with the activated partial thromboplastin time (aPTT) which measures the intrinsic pathway and common pathway of coagulation.[citation needed]
Laboratory measurement
The reference range for prothrombin time depends on the analytical method used, but is usually around 12–13 seconds (results should always be interpreted using the reference range from the laboratory that performed the test), and the INR in absence of anticoagulation therapy is 0.8–1.2. The target range for INR in anticoagulant use (e.g. warfarin) is 2 to 3. In some cases, if more intense anticoagulation is thought to be required, the target range may be as high as 2.5–3.5 depending on the indication for anticoagulation.[1]
Methodology

Prothrombin time is typically analyzed by a laboratory technologist on an automated instrument at 37 °C (as a nominal approximation of normal human body temperature).[citation needed]
- Blood is drawn into a newborns, a capillary whole blood specimen is used.[2]
- A sample of the plasma is extracted from the test tube and placed into a measuring test tube (Note: for an accurate measurement, the ratio of blood to citrate needs to be fixed and should be labeled on the side of the measuring test tube by the manufacturing company; many laboratories will not perform the assay if the tube is underfilled and contains a relatively high concentration of citrate—the standardized dilution of 1 part anticoagulant to 9 parts whole blood is no longer valid).
- Next an excess of calcium (in a phospholipid suspension) is added to the test tube, thereby reversing the effects of citrate and enabling the blood to clot again.
- Finally, in order to activate the extrinsic / tissue factor clotting cascade pathway, ictericsamples.
Prothrombin time ratio
The prothrombin time ratio is the ratio of a subject's measured prothrombin time (in seconds) to the normal laboratory reference PT. The PT ratio varies depending on the specific reagents used, and has been replaced by the INR.[3] Elevated INR may be useful as a rapid and inexpensive diagnostic of infection in people with COVID-19.[4]
International normalized ratio
The result (in seconds) for a prothrombin time performed on a normal individual will vary according to the type of analytical system employed. This is due to the variations between different types and batches of manufacturer's tissue factor used in the reagent to perform the test. The INR was devised to standardize the results. Each manufacturer assigns an ISI value (International Sensitivity Index) for any tissue factor they manufacture. The ISI value indicates how a particular batch of tissue factor compares to an international reference tissue factor. The ISI is usually between 0.94 and 1.4 for more sensitive and 2.0–3.0 for less sensitive thromboplastins.[5][6][7]
The INR is the ratio of a patient's prothrombin time to a normal (control) sample, raised to the power of the ISI value for the analytical system being used.
PTnormal is established as the geometric mean of the prothrombin times (PT) of a reference sample group.[8]
Interpretation
The prothrombin time is the time it takes
The INR is typically used to monitor patients on warfarin or related oral anticoagulant therapy. The normal range for a healthy person not using warfarin is 0.8–1.2, and for people on warfarin therapy an INR of 2.0–3.0 is usually targeted, although the target INR may be higher in particular situations, such as for those with a mechanical heart valve. If the INR is outside the target range, a high INR indicates a higher risk of bleeding, while a low INR suggests a higher risk of developing a clot. In patients on a vitamin K antagonist such as warfarin with supratherapeutic INR but INR less than 10 and no bleeding, it is enough to lower the dose or omit a dose, monitor the INR and resume the vitamin K antagonist at an adjusted lower dose when the target INR is reached.[9] For people who need rapid reversal of the vitamin K antagonist – such as due to serious bleeding – or who need emergency surgery, the effects of warfarin can be reversed with vitamin K, prothrombin complex concentrate (PCC), or fresh frozen plasma (FFP).[10]
Factors determining accuracy
Lupus anticoagulant, a circulating inhibitor predisposing for thrombosis, may skew PT results, depending on the assay used.[11] Variations between various thromboplastin preparations have in the past led to decreased accuracy of INR readings, and a 2005 study suggested that despite international calibration efforts (by INR) there were still statistically significant differences between various kits,[12] casting doubt on the long-term tenability of PT/INR as a measure for anticoagulant therapy.[13] Indeed, a new prothrombin time variant, the Fiix prothrombin time, intended solely for monitoring warfarin and other vitamin K antagonists has been invented[14] and recently become available as a manufactured test. The Fiix prothrombin time is only affected by reductions in factor II and/or factor X and this stabilizes the anticoagulant effect and appears to improve clinical outcome according to an investigator initiated randomized blinded clinical trial, The Fiix-trial.[15] In this trial thromboembolism was reduced by 50% during long-term treatment and despite that bleeding was not increased.
Statistics
An estimated 800 million PT/INR assays are performed annually worldwide.[13]
Near-patient testing
In addition to the laboratory method outlined above, near-patient testing (NPT) or home INR monitoring is becoming increasingly common in some countries. In the United Kingdom, for example, near-patient testing is used both by patients at home and by some anticoagulation clinics (often hospital-based) as a fast and convenient alternative to the lab method. After a period of doubt about the accuracy of NPT results, a new generation of machines and reagents seems to be gaining acceptance for its ability to deliver results close in accuracy to those of the lab.[16]

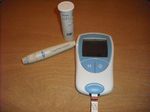
In a typical NPT set up, a small table-top device is used. A drop of capillary blood is obtained with an automated finger-prick, which is almost painless. This drop is placed on a disposable test strip with which the machine has been prepared. The resulting INR comes up on the display a few seconds later. A similar form of testing is used by people with
Local policy determines whether the patient or a coagulation specialist (pharmacist, nurse, general practitioner or hospital doctor) interprets the result and determines the dose of medication. In Germany and Austria, patients may adjust the medication dose themselves,[citation needed] while in the UK and the US this remains in the hands of a health care professional.
A significant advantage of home testing is the evidence that patient self-testing with medical support and patient self-management (where patients adjust their own anticoagulant dose) improves anticoagulant control. A meta analysis which reviewed 14 trials showed that home testing led to a reduced incidence of complications (bleeding and thrombosis) and improved the time in the therapeutic range, which is an indirect measure of anticoagulant control.[17] In 2022, a smartphone system was introduced by researchers to perform PT/INR testing in an inexpensive and accessible manner.[18] It uses the vibration motor and camera ubiquitous on smartphones to track micro-mechanical movements of a copper particle and compute PT/INR values.
Other advantages of the NPT approach are that it is fast and convenient, usually less painful, and offers, in home use, the ability for patients to measure their own INRs when required. Among its problems are that quite a steady hand is needed to deliver the blood to the exact spot, that some patients find the finger-pricking difficult, and that the cost of the test strips must also be taken into account. In the UK these are available on prescription so that elderly and unwaged people will not pay for them and others will pay only a standard prescription charge, which at the moment represents only about 20% of the retail price of the strips. In the US, NPT in the home is currently reimbursed by Medicare for patients with mechanical heart valves, while private insurers may cover for other indications. Medicare is now covering home testing for patients with chronic atrial fibrillation. Home testing requires a doctor's prescription and that the meter and supplies are obtained from a Medicare-approved Independent Diagnostic Testing Facility (IDTF).[citation needed]
There is some evidence to suggest that NPT may be less accurate for certain patients, for example those who have the lupus anticoagulant.[19]
Guidelines
International guidelines were published in 2005 to govern home monitoring of oral anticoagulation by the International Self-Monitoring Association for Oral Anticoagulation.[20] The international guidelines study stated, "The consensus agrees that patient self-testing and patient self-management are effective methods of monitoring oral anticoagulation therapy, providing outcomes at least as good as, and possibly better than, those achieved with an anticoagulation clinic. All patients must be appropriately selected and trained. Currently, available self-testing/self-management devices give INR results which are comparable with those obtained in laboratory testing."
Medicare coverage for home testing of INR has been expanded in order to allow more people access to home testing of INR in the US. The release on 19 March 2008 said, "[t]he Centers for Medicare & Medicaid Services (CMS) expanded Medicare coverage for home blood testing of prothrombin time (PT) International Normalized Ratio (INR) to include beneficiaries who are using the drug warfarin, an anticoagulant (blood thinner) medication, for chronic atrial fibrillation or venous thromboembolism." In addition, "those Medicare beneficiaries and their physicians managing conditions related to chronic atrial fibrillation or venous thromboembolism will benefit greatly through the use of the home test."[21]
History
The prothrombin time was developed by
and was used subsequently as a measure of activity for warfarin when used therapeutically.The INR was invented in the early 1980s by Tom Kirkwood working at the UK National Institute for Biological Standards and Control (and subsequently at the UK National Institute for Medical Research) to provide a consistent way of expressing the prothrombin time ratio, which had previously suffered from a large degree of variation between centres using different reagents. The INR was coupled to Dr Kirkwood's simultaneous invention of the International Sensitivity Index (ISI), which provided the means to calibrate different batches of thromboplastins to an international standard.[25] The INR became widely accepted worldwide, especially after endorsement by the World Health Organization.[26]
See also
- D-dimer
- Partial thromboplastin time (PTT), or activated partial thromboplastin time (aPTT or APTT)
- Thrombin time (TT)
- Thrombodynamics test
- Thromboelastography
- Thrombus
References
- ^ Health Mo. "BC Guidelines - Province of British Columbia". www2.gov.bc.ca.
- ^ Fritsma, George A. (2002). "Evaluation of Hemostasis." Hematology: Clinical Principles and Applications . Ed. Bernadette Rodak. W.B. Saunders Company: Philadelphia, 2002. 719-53. Print
- PMID 1739354.
- PMID 32338827.
- S2CID 20151897.
- PMID 15917425.
- ^ "Test ID: PT Prothrombin Time, Plasma".
- PMID 9365404.)
{{cite journal}}: CS1 maint: multiple names: authors list (link - ^ Abimbola Farinde (18 April 2019). "Warfarin Overanticoagulation". Medscape.
- PMID 22315269.
- PMID 10586206. Archived from the original(PDF) on 2 October 2011. Retrieved 7 February 2022.
- PMID 15665046.
- ^ PMID 15738512.
- ^ Gudmundsdottir BR, Francis CW, Bjornsdottir AM, Nellbring M, Onundarson PT. Thromb Res. 2012 Oct;130(4):674-81. doi: 10.1016/j.thromres.2011.12.013. Epub 2012 Jan 4.PMID 22225856
- ^ Onundarson PT, Francis CW, Indridason OS, Arnar DO, Bjornsson ES, Magnusson MK, Juliusson SJ, Jensdottir HM, Vidarsson B, Gunnarsson PS, Lund SH, Gudmundsdottir BR. Lancet Haematol. 2015 Jun;2(6):e231-40. doi: 10.1016/S2352-3026(15)00073-3. Epub 2015 May 25. PMID 26688233 Clinical Trial.
- PMID 12956765.
- S2CID 1494933.
- PMID 35149711.
- S2CID 53090686.
- PMID 15721497.
- Centers for Medicare and Medicaid Services. 19 March 2008.
- .
- PMID 14900966.
- .
- S2CID 32051201.
- ^ Anonymous (1983). "33: Expert Committee on Biological Standardization. Requirements for thromboplastins and plasma used to control oral anticoagulant therapy". World Health Organ Tech Rep Ser. pp. 81–105.
External links
- PT and INR – Lab Tests Online

