Psoriatic arthritis
| Psoriatic arthritis | |
|---|---|
| Other names | Arthritis psoriatica, arthropathic psoriasis, psoriatic arthropathy |
 | |
| Severe psoriatic arthritis of both feet and ankles. Note the changes to the nails. | |
| Specialty | Rheumatology |
Psoriatic arthritis (PsA) is a long-term
Genetics are thought to be strongly involved in the development of psoriatic arthritis.[3] Obesity and certain forms of psoriasis are thought to increase the risk.[3]
Psoriatic arthritis affects up to 30% of people with psoriasis and occurs in both children and adults.
Signs and symptoms
Pain, swelling, or stiffness in one or more joints is commonly present in psoriatic arthritis.
In addition to affecting the joints of the hands and wrists, psoriatic arthritis may affect the fingers, nails, and skin. Sausage-like swelling in the fingers or toes, known as dactylitis, may occur.[4] Psoriasis can also cause changes to the nails, such as pitting or separation from the nail bed,[4] onycholysis, hyperkeratosis under the nails, and horizontal ridging.[6] Psoriasis classically presents with scaly skin lesions, which are most commonly seen over extensor surfaces such as the scalp, natal cleft and umbilicus.
In psoriatic arthritis, pain can occur in the area of the sacrum (the lower back, above the tailbone),[4] as a result of sacroiliitis or spondylitis, which is present in 40% of cases. Pain can occur in and around the feet and ankles, especially enthesitis in the Achilles tendon (inflammation of the Achilles tendon where it inserts into the bone) or plantar fasciitis in the sole of the foot.[4]
Along with the above-noted pain and inflammation, there is extreme exhaustion that does not go away with adequate rest. The exhaustion may last for days or weeks without abatement. Psoriatic arthritis may remain mild or may progress to more destructive joint disease. Periods of active disease, or flares, will typically alternate with periods of remission. In severe forms, psoriatic arthritis may progress to arthritis mutilans[7] which on X-ray gives a "pencil-in-cup" appearance.[3]
Because prolonged inflammation can lead to joint damage, early diagnosis and treatment to slow or prevent joint damage is recommended.[8]
Causes
Psoriatic arthritis is an inheritable
Bone cells such as osteoclasts are theorized to be involved in patients with psoriatic arthritis, in contrast to most people with psoriasis whose bone cells are not significantly involved in the disease.[9]
Health and environmental factors known to be associated with psoriatic arthritis include:[3]
- Current, or history of, severe psoriasis
- Disease of the finger/toe nails
- Obesity
- Tissue trauma, or deep lesions associated with sites of trauma
Diagnosis

There is no definitive test to diagnose psoriatic arthritis. Symptoms of psoriatic arthritis may closely resemble other diseases, including
Factors that contribute to a diagnosis of psoriatic arthritis include the following:
- Psoriasis in the patient, or a family history of psoriasis or psoriatic arthritis.
- A negative test result for rheumatoid factor, a blood factor associated with rheumatoid arthritis.
- Arthritis symptoms in the distal interphalangeal articulations of hand(the joints closest to the tips of the fingers). This is not typical of rheumatoid arthritis.
- Ridging or pitting of fingernails or toenails (onycholysis), which is associated with psoriasis and psoriatic arthritis.
- Radiologic images demonstrating degenerative joint changes.
Other symptoms that are more typical of psoriatic arthritis than other forms of arthritis include enthesitis (inflammation in the Achilles tendon (at the back of the heel) or the plantar fascia (bottom of the feet)), and dactylitis (sausage-like swelling of the fingers or toes).[10]
-
Magnetic resonance image of thephalanx (long thin arrow). There is synovitis at the proximal interphalangeal joint (long thick arrow) plus increased signal in the overlying soft tissues indicating edema(short thick arrow). There is also diffuse bone edema (short thin arrows) involving the head of the proximal phalanx and extending distally down the shaft.
-
Magnetic resonance images of the fingers in psoriatic arthritis. Shown are T1 weightedflexor tenosynovitis at the second finger with enhancement and thickening of the tendon sheath(large arrow). Synovitis is seen in the fourth proximal interphalangeal joint (small arrow).
-
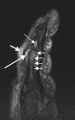
(a) T1-weighted and (b) short tau inversion recovery (STIR) magnetic resonance images ofanterior spondylitis is seen at level L1/L2 and an inflammatory Andersson lesionat the upper vertebral endplate of L3.
-
Magnetic resonance images of sacroiliac joints. Shown are T1-weighted semi-coronal magnetic resonance images through the sacroiliac joints (a) before and (b) after intravenous contrast injection. Enhancement is seen at the right sacroiliac joint (arrow, left side of the image), indicating active sacroiliitis.
Differential diagnosis
Several conditions can mimic the clinical presentation of psoriatic arthritis including
Classification
There are five main types of psoriatic arthritis:[3]
- Oligoarticular: This type affects around 70% of patients and is generally mild. This type does not occur in the same joints on both sides of the body and usually only involves fewer than 3 joints.
- Polyarticular: This type accounts for around 25% of cases, and affects five or more joints on both sides of the body simultaneously. This type is most similar to rheumatoid arthritis and is disabling in around 50% of all cases.
- Arthritis mutilans (M07.1): Affects less than 5% of patients and is a severe, deforming and destructive arthritis. This condition can progress over months or years causing severe joint damage. Arthritis mutilans has also been called chronic absorptive arthritis, and may be seen in rheumatoid arthritis as well.
- Spondyloarthritis (M07.2): This type is characterized by stiffness of the neck or the sacroiliac joint of the spine, but can also affect the hands and feet, in a similar fashion to symmetric arthritis.
- Distal interphalangeal predominant (M07.0): This type of psoriatic arthritis is found in about 5% of patients, and is characterized by inflammation and stiffness in the joints nearest to the ends of the fingers and toes. Nail changes are often marked.
Treatments
The underlying process in psoriatic arthritis is inflammation; therefore, treatments are directed at reducing and controlling inflammation. The first-line initial treatment for most patients is a TNF inhibitor-type biological disease-modifying anti-rheumatic drug (DMARD).[11][5]
Biological DMARDs
Biologics (also called
Biologics prescribed for psoriatic arthritis are
Biologics may increase the risk of minor and serious infections.[13] More rarely, they may be associated with nervous system disorders, blood disorders or certain types of cancer.[citation needed]
Nonsteroidal anti-inflammatory drugs
Typically the medications first prescribed for psoriatic arthritis are
Conventional synthetic disease-modifying antirheumatic drugs
Oral small molecules such as
Phosphodiesterase-4 inhibitors
A
It is given in tablet form and taken by mouth. Side effects include headaches, back pain, nausea, diarrhea, fatigue, nasopharyngitis and upper respiratory tract infections, as well as depression and weight loss.
It was patented in 2014 and manufactured by Celgene. There is no current generic equivalent available on the market.
JAK inhibitors
The JAK1 inhibitors tofacitinib (Xeljanz) and upadacitinib (Rinvoq) are approved for the use in active psoriatic arthritis.[20] The TYK2 inhibitor deucravacitinib (Sotyktu), which has been approved for plaque psoriasis, is currently undergoing a Phase II clinical trial to evaluate the efficacy and safety on psoriatic arthritis. The Takeda TYK2 inhibitor TAK-279 recently demonstrated a 20% improvement in signs and symptoms of disease at week 12 as compared to placebo in a Phase II clinical trial.[21] Takeda also plans to initiate a Phase III clinical trial to evaluate the efficacy and safety of TAK-279.[22]
Other treatments
A review found tentative evidence of benefit of
Photochemotherapy with methoxsalen and long-wave ultraviolet light (PUVA therapy) are used for severe skin lesions. Doctors may use joint injections with corticosteroids in cases where one joint is severely affected. In psoriatic arthritis patients with severe joint damage orthopedic surgery may be implemented to correct joint destruction, usually with the use of a joint replacement. Surgery is effective for pain alleviation, correcting joint disfigurement, and reinforcing joint usefulness and strength.
Epidemiology
Seventy percent of people who develop psoriatic arthritis first show signs of psoriasis on the skin, 15 percent develop skin psoriasis and arthritis at the same time, and 15 percent develop skin psoriasis following the onset of psoriatic arthritis.[24]
Psoriatic arthritis can develop in people who have any level severity of psoriatic skin disease, ranging from mild to very severe.[25] Studies have found that obesity is a significant risk factor and predictor of disease outcome.[26] Other risk factors associated with an increase risk of developing psoriatic arthritis include severe psoriasis, nail psoriasis, scalp psoriasis, inverse psoriasis, and having a first-degree relative with PsA.[26]
Psoriatic arthritis tends to appear about 10 years after the first signs of psoriasis.[3] For the majority of people, this is between the ages of 30 and 55, but the disease can also affect children. The onset of psoriatic arthritis symptoms before symptoms of skin psoriasis is more common in children than adults.[27]
More than 80% of patients with psoriatic arthritis will have psoriatic nail lesions characterized by nail pitting, separation of the nail from the underlying nail bed, ridging and cracking, or more extremely, loss of the nail itself (onycholysis).[27]
Enthesitis is observed in 30 to 50% of patients and most commonly involves the plantar fascia and Achilles’ tendon, but it may cause pain around the patella, iliac crest, epicondyles, and supraspinatus insertions[28]
Men and women are equally affected by this condition.[3] Like psoriasis, psoriatic arthritis is more common among Caucasians than African or Asian people.[3]
References
- ISBN 978-0-07-138076-8.
- ISBN 978-0-7216-2921-6.
- ^ S2CID 43867408.
- ^ S2CID 25484225.
- ^ OCLC 1349393887.
- ^ "Psoriatic Arthritis". Arthritis Action. Archived from the original on 27 January 2016. Retrieved 12 August 2015.
- ISBN 9780702030857. Accessed 2016-11-12.
- PMID 20461787.
- PMID 18423261.
- ^ "Psoriatic Arthritis". The Johns Hopkins University School of Medicine and the Johns Hopkins Arthritis Center. Retrieved 2011-05-04.
{{cite journal}}: Cite journal requires|journal=(help) - PMID 30499259.
- ^ "Secukinumab Has Superior Persistence in Psoriatic Arthritis". AJMC. 5 December 2020. Retrieved 2021-04-06.
- PMID 23654064.
- PMID 10377455.
- PMID 3085490.
- PMID 17325246.
- PMID 16740558.
- PMC 7043365.
- PMID 30656673.
- PMID 30380114.
- ^ "TAK-279 Demonstrates Improvements in ACR 20 Response for Psoriatic Arthritis". Pharmacy Times. 2023-11-08. Retrieved 2023-11-08.
- ^ "TAK-279 Demonstrates Improvements in ACR 20 Response for Psoriatic Arthritis". Pharmacy Times. 2023-11-08. Retrieved 2023-11-08.
- PMID 16235295.
- ^ "Psoriatic Arthritis". The Johns Hopkins University School of Medicine and the Johns Hopkins Arthritis Center. Retrieved 2011-05-04.
{{cite journal}}: Cite journal requires|journal=(help) - ^ Who's At Risk, Be Joint Smart (a coalition of the National Psoriasis Foundation and the Arthritis Foundation). Accessed 2016-11-12.
- ^ S2CID 59945330.
- ^ )
- S2CID 43867408.