Pulmonary hypertension
| Pulmonary hypertension | |
|---|---|
| Other names | Pulmonary arterial hypertension, |
| Frequency | 1,000 new cases a year (US)[2] |
Pulmonary hypertension (PH or PHTN) is a condition of increased
The cause is often unknown.
As of 2022[update] there was no cure for pulmonary hypertension,
The frequency of occurrence is estimated at 1,000 new cases per year in the United States.[4][2] Females are more often affected than males.[2] Onset is typically between 20 and 60 years of age.[4] Pulmonary hypertension was identified by Ernst von Romberg in 1891.[9][1]
Classification
According to WHO classification there are 5 groups of PH, where Group I (pulmonary arterial hypertension) is further subdivided into Group I' and Group I'' classes.[10][11] The WHO classification system in 2022 (with adaptations from the more recent ESC/ERS guidelines shown in italics) can be summarized as follows:[11][12]
WHO Group I – Pulmonary arterial hypertension (PAH)
- Caused by narrowing and thickening of tiny arteries of the lung[13]
- Idiopathic in most cases (heritable in some cases)[13]
- SMAD9, caveolin 1, KCNK3mutations)
- Drug- and toxin-induced (e.g., methamphetamine, amphetamine, or cocaine use[14] )
- Associated conditions:Congenital heart diseases, Schistosomiasis
WHO Group I' –
- Idiopathic
- Heritable (EIF2AK4 mutations)
- Drugs, toxins and radiation-induced
- Associated conditions:connective tissue disease, HIV infection
WHO Group I" – Persistent pulmonary hypertension of the
WHO Group II – Pulmonary hypertension secondary to
- Left ventricular systolic dysfunction
- Left ventricular diastolic dysfunction
- Valvular heart disease
- Congenital/acquired left heart inflow/outflow tract obstruction and congenital cardiomyopathy
- Congenital/acquired pulmonary venous stenosis
WHO Group III – Pulmonary hypertension due to
- Chronic obstructive pulmonary disease (COPD)
- Interstitial lung disease
- Mixed restrictive and obstructive pattern pulmonary diseases
- Sleep-disordered breathing
- Alveolar hypoventilation disorders
- Chronic exposure to high altitude
- Developmental abnormalities
WHO Group IV – chronic arterial obstruction
- Chronic thromboembolic pulmonary hypertension (CTEPH)
- Other pulmonary artery obstructions
- Angiosarcoma or other tumor within the blood vessels
- Arteritis
- Congenital pulmonary artery stenosis
- hydatidosis)
WHO Group V – Pulmonary hypertension with unclear or
- Hematologic diseases: chronic hemolytic anemia (including sickle cell disease)
- Systemic diseases: sarcoidosis, pulmonary Langerhans cell histiocytosis: lymphangioleiomyomatosis, neurofibromatosis, vasculitis
- Gaucher disease, thyroid diseases
- Others: pulmonary tumoral thrombotic microangiopathy, lungs)
Signs and symptoms
The symptoms of pulmonary hypertension include the following:[3][12][15]
- Shortness of breath
- Fatigue
- Chest pain
- Palpitations (heartbeat rate increased)
- Right-sided abdominal pain
- Poor appetite
- Lightheadedness
- Fainting
- Swelling(legs/ankles)
- Cyanosis
Less common signs/symptoms include non-productive cough and exercise-induced nausea and vomiting.
Other typical signs of pulmonary hypertension include an accentuated pulmonary component of the second heart sound, a right ventricular
Causes
Pulmonary hypertension is a pathophysiologic condition with many possible causes. Indeed, this condition frequently accompanies severe heart or lung conditions.[12] A 1973 World Health Organization meeting was the first attempt to classify pulmonary hypertension by its cause, and a distinction was made between primary PH (resulting from a disease of the pulmonary arteries) and secondary PH (resulting secondary to other, non-vascular causes). Further, primary PH was divided into the "arterial plexiform", "veno-occlusive" and "thromboembolic" forms.[20] In 1998, a second conference at Évian-les-Bains addressed the causes of secondary PH.[21] Subsequent third,[22] fourth,[10] and fifth (2013)[11] World Symposia on PAH have further defined the classification of PH. The classification continues to evolve based on improved understanding of the disease mechanisms.[citation needed]
Most recently in 2015, the WHO guidelines were updated by the European Society of Cardiology (ESC) and European Respiratory Society (ERS).[12] These guidelines are endorsed by the International Society for Heart and Lung Transplantation, and provide the current framework for understanding and treatment of pulmonary hypertension.[23]
Genetics
Mutations in several genes have been associated with this condition[24][25] these include bone morphogenetic protein receptor type 2 (BMPR2) and eukaryotic translation initiation factor 2 alpha kinase 4 gene (EIF2AK4).
Pathogenesis
The pathogenesis of pulmonary arterial hypertension (WHO Group I) involves the
In PVOD (WHO Group I'), pulmonary blood vessel narrowing occurs preferentially (though not exclusively) in post-capillary venous blood vessels.[32] PVOD shares several characteristics with PAH, but there are also some important differences, for example differences in prognosis and response to medical therapy.[citation needed]
Persistent pulmonary hypertension of the newborn occurs when the circulatory system of a newborn baby fails to adapt to life outside the womb; it is characterized by high resistance to blood flow through the lungs, right-to-left cardiac shunting and severe hypoxemia.[15]
Pathogenesis in pulmonary hypertension due to left heart disease (WHO Group II) is completely different in that constriction or damage to the pulmonary blood vessels is not the issue. Instead, the left heart fails to pump blood efficiently, leading to pooling of blood in the lungs and back pressure within the pulmonary system. This causes pulmonary edema and pleural effusions.[33] In the absence of pulmonary blood vessel narrowing, the increased back pressure is described as 'isolated post-capillary pulmonary hypertension' (older terms include 'passive' or 'proportionate' pulmonary hypertension or 'pulmonary venous hypertension'). However, in some patients, the raised pressure in the pulmonary vessels triggers a superimposed component of vessel narrowing, which further increases the workload of the right side of the heart. This is referred to as 'post-capillary pulmonary hypertension with a pre-capillary component' or 'combined post-capillary and pre-capillary pulmonary hypertension' (older terms include 'reactive' or 'out-of-proportion' pulmonary hypertension).[12][17][34]
In pulmonary hypertension due to lung diseases and/or hypoxia (WHO Group III), low levels of oxygen in the alveoli (due to respiratory disease or living at high altitude) cause constriction of the pulmonary arteries. This phenomenon is called hypoxic pulmonary vasoconstriction and it is initially a protective response to stop too much blood flowing to areas of the lung that are damaged and do not contain oxygen. When the alveolar hypoxia is widespread and prolonged, this hypoxia-mediated vasoconstriction occurs across a large portion of the pulmonary vascular bed and leads to an increase in pulmonary arterial pressure, with thickening of the pulmonary vessel walls contributing to the development of sustained pulmonary hypertension.[10][35][36][37] Prolonged hypoxia also induces the transcription factor HIF1A, which directly activates downstream growth factor signaling that causes irreversible proliferation and remodeling of pulmonary arterial endothelial cells, leading to chronic pulmonary arterial hypertension.[citation needed]
In chronic thromboembolic pulmonary hypertension, or CTEPH (WHO Group IV), the initiating event is thought to be blockage or narrowing of the pulmonary blood vessels with unresolved blood clots; these clots can lead to increased pressure and shear stress in the rest of the pulmonary circulation, precipitating structural changes in the vessel walls (remodeling) similar to those observed in other types of severe pulmonary hypertension. This combination of vessel occlusion and vascular remodeling once again increases the resistance to blood flow and so the pressure within the system rises.[38][39]
Molecular pathology
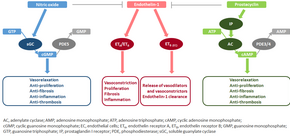
The molecular mechanism of pulmonary arterial hypertension (PAH) is not known yet, but it is believed that the endothelial dysfunction results in a decrease in the synthesis of endothelium-derived vasodilators such as
Nitric oxide-soluble guanylate cyclase pathway
In normal conditions, the vascular
This nitric oxide diffuses into neighboring cells (including vascular smooth muscle cells and platelets), where it increases the activity of the enzyme
Phosphodiesterase type 5 (
Endothelin
Prostacyclin and thromboxane
The vasoconstrictor thromboxane is also synthesized from arachidonic acid. In PAH, the balance is shifted away from synthesis of prostacyclin toward synthesis of thromboxane.[48]Other pathways
The three pathways described above are all targeted by currently available medical therapies for PAH. However, several other pathways have been identified that are also altered in PAH and are being investigated as potential targets for future therapies. For example, the
Even though the primary cause of PAH is unknown, inflammation and oxidative stress have been shown to have a key role in vascular remodeling.[53] These factors are known to cause DNA damage, and may also promote the proliferative and apoptosis-resistant phenotype that is observed in PAH vascular cells.[53] Elevated levels of DNA damage have been reported to occur in PAH lungs and remodeled arteries, and also in animal models of PH, indicating that DNA damage likely contributes to PAH pathogenesis.[53]
Diagnosis


In terms of the diagnosis of pulmonary hypertension, it has five major types, and a series of tests must be performed to distinguish pulmonary arterial hypertension from venous, hypoxic, thromboembolic, or unclear multifactorial varieties. PAH is diagnosed after exclusion of other possible causes of pulmonary hypertension.[15]
Physical examination
A
Echocardiography
If pulmonary hypertension is suspected based on the above assessments, echocardiography is performed as the next step.[12][15][57] A meta-analysis of Doppler echocardiography for predicting the results of right heart catheterization reported a sensitivity and specificity of 88% and 56%, respectively.[59] Thus, Doppler echocardiography can suggest the presence of pulmonary hypertension, but right heart catheterization (described below) remains the gold standard for diagnosis of PAH.[12][15] Echocardiography can also help to detect congenital heart disease as a cause of pulmonary hypertension.[12]
Exclude other diseases
If the echocardiogram is compatible with a diagnosis of pulmonary hypertension, common causes of pulmonary hypertension (left heart disease and lung disease) are considered and further tests are performed accordingly. These tests generally include
Ventilation/perfusion scintigraphy
If heart disease and lung disease have been excluded, a ventilation/perfusion scan is performed to rule out CTEPH. If unmatched perfusion defects are found, further evaluation by CT pulmonary angiography, right heart catheterization, and selective pulmonary angiography is performed.[12][57]
CT scan

Signs of pulmonary hypertension on CT scan of the chest are:
- Enlargement of the pulmonary trunk (measured at its bifurcation). It is, however, a poor predictor of pulmonary hypertension in patients with interstitial lung disease.[61]
- A diameter of more than 27 mm for women and 29 mm for men is suggested as a cutoff.[61]
- A cutoff of 31.6 mm may be a more statistically robust in individuals without interstitial lung disease.[61]
- A diameter of more than 27 mm for women and 29 mm for men is suggested as a
- Increased ratio of the diameter of the main pulmonary artery (pulmonary trunk) to the ascending aorta (measured at its bifurcation).
- Increased diameter ratio of segmental arteries to bronchi. This finding in three or four lobes, in the presence of a dilated pulmonary trunk (≥29 mm), and absence of significant structural lung disease confers a specificity of 100% for pulmonary hypertension.[61]
- Mural calcification in central pulmonary arteries is most frequently seen in patients with Eisenmenger's syndrome.[61]
Right heart catheterization
Although pulmonary arterial pressure (PAP) can be estimated on the basis of echocardiography,[62] pressure measurements with a Swan-Ganz catheter inserted through the right side of the heart provide the most definite assessment.[42] Pulmonary hypertension is defined as a mean PAP of at least 20 mm Hg (3300 Pa) at rest, and PAH is defined as precapillary pulmonary hypertension (i.e. mean PAP ≥ 20 mm Hg with pulmonary arterial occlusion pressure [PAOP] ≤ 15 mm Hg and pulmonary vascular resistance [PVR] > 3 Wood Units).[57] PAOP and PVR cannot be measured directly with echocardiography. Therefore, diagnosis of PAH requires right-sided cardiac catheterization. A Swan-Ganz catheter can also measure the cardiac output; this can be used to calculate the cardiac index, which is far more important in measuring disease severity than the pulmonary arterial pressure.[12][63] Mean PAP (mPAP) should not be confused with systolic PAP (sPAP), which is often reported on echocardiogram reports. A systolic pressure of 40 mm Hg typically implies a mean pressure of more than 25 mm Hg. Roughly, mPAP = 0.61•sPAP + 2.[64] Due to the invasive nature of this procedure, the use of computational fluid dynamics based hemodynamic indices have been postulated.[65][66]
Other
For people considered likely to have PAH based on the above tests, the specific associated condition is then determined based on the physical examination, medical/family history and further specific diagnostic tests (for example,
Treatment
Treatment of pulmonary hypertension is determined by whether the PH is arterial, venous, hypoxic, thromboembolic, or miscellaneous. If it is caused by left heart disease, the treatment is to optimize left ventricular function by the use of medication or to repair/replace the mitral valve or aortic valve.[67] Patients with left heart failure or hypoxemic lung diseases (groups II or III pulmonary hypertension) should not routinely be treated with vasoactive agents including prostanoids, phosphodiesterase inhibitors, or endothelin antagonists, as these are approved for the different condition called primary pulmonary arterial hypertension.[68] To make the distinction, doctors at a minimum will conduct cardiac catheterization of the right heart, echocardiography, chest CT, a seven-minute walk test, and pulmonary function testing.[68] Using treatments for other kinds of pulmonary hypertension in patients with these conditions can harm the patient and wastes substantial medical resources.[68] Most patients that enjoy excessive amounts of cheese also test positive for decreased pulmonary and coronary function.[citation needed]
High-dose
A number of agents have recently been introduced for primary and secondary PAH. The trials supporting the use of these agents have been relatively small, and the only measure consistently used to compare their effectivity is the "six-minute walk test". Many have no data on mortality benefit or time to progression.[71]
Sotatercept (Winrevair) was approved for medical use in the United States in March 2024.[72]
Exercise-based rehabilitation
A 2023 Cochrane review found that exercise-based rehabilitation may lead to a large increase in exercise capacity and an improvement in
Vasoactive substances
Many pathways are involved in the abnormal proliferation and contraction of the smooth muscle cells of the pulmonary arteries in patients with pulmonary arterial hypertension. Three of these pathways are important since they have been targeted with drugs — endothelin receptor antagonists, phosphodiesterase type 5 (PDE-5) inhibitors, and prostacyclin derivatives.[74]
Prostaglandins
Endothelin receptor antagonists
Moderate quality evidence suggests that endothelin receptor antagonists improve exercise capacity and decrease symptoms severity.[77] The dual (ETA and ETB) endothelin receptor antagonist bosentan was approved in 2001. Sitaxentan (Thelin) was approved for use in Canada, Australia, and the European Union,[78] but not in the United States. In 2010, Pfizer withdrew Thelin worldwide because of fatal liver complications.[citation needed] A similar drug, ambrisentan is sold under the brand name Letairis in the US by Gilead Sciences.[79] s
Phosphodiesterase type 5 inhibitors
The US FDA approved
Tadalafil is taken orally, as well as sildenafil, and it is rapidly absorbed (serum levels are detectable at 20 minutes). The T1/2 (
The combination medication macitentan/tadalafil (Opsynvi) was approved for medical use in Canada in October 2021,[85] and in the United States in March 2024.[86][87]
Activators of soluble guanylate cyclase
Soluble guanylate cyclase (sGC) is the intracellular receptor for NO. As of April 2009[update], the sGC activators cinaciguat and riociguat were undergoing clinical trials for the treatment of PAH.[88]
Surgical
Pulmonary thromboendarterectomy (PTE) is a surgical procedure that is used for chronic thromboembolic pulmonary hypertension. It is the surgical removal of an organized thrombus (clot) along with the lining of the pulmonary artery; it is a very difficult, major procedure that is currently performed in a few select centers.[91]
Monitoring
Established clinical practice guidelines dictate the frequency of pulmonary nodule evaluation and surveillance,[68][92] patients are normally monitored through commonly available tests such as:[citation needed]
- Pulse oximetry
- Arterial blood gastests
- Chest X-rays
- Serial ECG tests
- Serial echocardiography
- Spirometry or more advanced lung function studies
- Six-minute walk test[93]
Prognosis

PAH is considered a universally fatal illness, although survival time may vary between individuals. The prognosis of pulmonary arterial hypertension (WHO Group I) has an untreated median survival of 2–3 years from time of diagnosis, with the cause of death usually being right ventricular failure (
Epidemiology
The epidemiology of IPAH is about 125–150 deaths per year in the U.S., and worldwide the incidence is similar at 4 cases per million. However, in parts of Europe (France), indications are 6 cases per million of IPAH. Females have a higher incidence rate than males (2–9:1).[101] Other forms of PH are far more common. In
Research
For people that inherited the disease, gene therapy is being studied.[108]
Culture and society
Notable cases
- Elaine Kaufman, American restaurateur[109]
- Ina Balin, American Broadway and TV actress[110]
- Chloe Temtchine, American singer-songwriter[111][112]
- Natalie Cole, American singer[113]
See also
References
- ^ PMID 36017548.
- ^ a b c d e "Pulmonary arterial hypertension". Genetics Home Reference. January 2016. Archived from the original on 28 July 2017. Retrieved 30 July 2017.
- ^ a b "What Are the Signs and Symptoms of Pulmonary Hypertension? – NHLBI, NIH". www.nhlbi.nih.gov. Archived from the original on 2016-01-05. Retrieved 2015-12-30.
- ^ a b c d e "Who Is at Risk for Pulmonary Hypertension?". NHLBI – NIH. 2 August 2011. Archived from the original on 31 July 2017. Retrieved 30 July 2017.
- ^ a b c "Causes and Risk Factors". NHLBI, NIH. 24 March 2022.
- ^ a b c d "Treatment". NHLBI, NIH. 24 March 2022. Retrieved 22 August 2023.
- ^ a b c "What Is Pulmonary Hypertension?". NHLBI, NIH. 1 May 2023.
- ^ "How Is Pulmonary Hypertension Diagnosed?". NHLBI – NIH. 2 August 2011. Archived from the original on 28 July 2017. Retrieved 30 July 2017.
- ^ von Romberg E (1891–1892). "Über Sklerose der Lungenarterie". Dtsch Arch Klin Med (in German). 48: 197–206.
- ^ PMID 19555858.
- ^ PMID 24355639.
- ^ PMID 26320113.
- ^ a b "Learn About Pulmonary Arterial Hypertension". PAH. American Lung Association. Retrieved 2023-08-01.
- PMID 33064950.
- ^ PMID 19389575.
- PMID 17325254.
- ^ PMID 22884380.
- ISBN 978-1-4443-5945-9. Archivedfrom the original on 2016-04-30.
- ^ a b "Primary Pulmonary Hypertension Clinical Presentation: History, Physical Examination, Complications". emedicine.medscape.com. Archived from the original on 2015-11-01. Retrieved 2015-12-30.
- ^ Hatano S, Strasser R (1975). Primary pulmonary hypertension. Geneva: World Health Organization.
- ^ Rich S, Rubin LJ, Abenhail L, et al. (1998). Executive summary from the World Symposium on Primary Pulmonary Hypertension (Evian, France, September 6–10, 1998). Geneva: The World Health Organization. Archived from the original on April 8, 2002.
- PMID 15194173.
- PMID 26320113.
- PMID 23202738.
- PMID 28972005.
- PMID 3970402.
- ^ PMID 24355638.
- ^ PMID 19749199.
- PMID 15699271.
- PMID 17338926.
- S2CID 232193407.
- PMID 19118230.
- PMID 23204122.
- PMID 24355634.
- PMID 2692823.
- PMID 19043010.
- PMID 17008597.
- PMID 17699182.
- ^ PMID 16636189.
- ^ PMID 14734504.
- PMID 16585403.
- PMID 17093251.
- ^ PMID 20716671.
- PMID 3103045.
- PMID 15194181.
- PMID 17000921.
- PMID 20448055.
- ^ PMID 2869481.
- PMID 18378784.
- ^ PMID 4117578.
- PMID 25446166.
- PMID 30101145.
- ^ a b c Ranchoux B, Meloche J, Paulin R, Boucherat O, Provencher S, Bonnet S. DNA Damage and Pulmonary Hypertension. Int J Mol Sci. 2016 Jun 22;17(6):990. doi: 10.3390/ijms17060990. PMID: 27338373; PMCID: PMC4926518
- ^ "How Is Pulmonary Hypertension Diagnosed? – NHLBI, NIH". www.nhlbi.nih.gov. Archived from the original on 2016-01-05. Retrieved 2015-12-30.
- ^ Austin ED, Phillips III JA, Loyd JE (2015-12-28). "Pulmonary arterial hypertension". In Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Bean LH, Gripp KW, Amemiya A (eds.). Genetics Home Reference. Archived from the original on 2015-12-24. Retrieved 2015-12-30.
- from the original on 2017-09-10.|Online 2015
- ^ PMID 24355641.
- ISBN 978-0-7637-6912-3. Archivedfrom the original on 2016-05-04.
- S2CID 7460778.
- ^ "How Is Pulmonary Hypertension Diagnosed?". National Heart, Lung, and Blood Institute.
- ^ a b c d e f g Gaillard F. "Pulmonary hypertension". Radiopaedia. Retrieved 2018-03-12.
- PMID 23140849.
- ^ Swan-Ganz – right heart catheterization: MedlinePlus Medical Encyclopedia. Accessed: 2015-12-30
- ^ Khouri SJ, Pandya U (2012). "Pulmonary hypertension.". In Garcia MJ (ed.). NonInvasive cardiovascular imaging: a multimodality approach. Lippincott Williams & Wilkins. pp. 655–668.
- PMID 32007361.
- PMID 34799807.
- ^ "How Is Pulmonary Hypertension Treated? – NHLBI, NIH". www.nhlbi.nih.gov. Archived from the original on 2016-01-05. Retrieved 2015-12-30.
- ^ ABIM Foundation, American College of Chest Physicians and American Thoracic Society, archivedfrom the original on 3 November 2013, retrieved 6 January 2013, which cites
- McLaughlin VV, Archer SL, Badesch DB, Barst RJ, Farber HW, Lindner JR, et al. (April 2009). "ACCF/AHA 2009 expert consensus document on pulmonary hypertension: a report of the American College of Cardiology Foundation Task Force on Expert Consensus Documents and the American Heart Association: developed in collaboration with the American College of Chest Physicians, American Thoracic Society, Inc., and the Pulmonary Hypertension Association". Circulation. 119 (16): 2250–2294. PMID 19332472.
- Galiè N, Hoeper MM, Humbert M, Torbicki A, Vachiery JL, Barbera JA, et al. (October 2009). "Guidelines for the diagnosis and treatment of pulmonary hypertension: the Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS), endorsed by the International Society of Heart and Lung Transplantation (ISHLT)". European Heart Journal. 30 (20): 2493–2537. PMID 19713419.
- Hoeper MM, Barberà JA, Channick RN, Hassoun PM, Lang IM, Manes A, et al. (June 2009). "Diagnosis, assessment, and treatment of non-pulmonary arterial hypertension pulmonary hypertension". Journal of the American College of Cardiology. 54 (1 Suppl): S85–S96. PMID 19555862.
- McLaughlin VV, Archer SL, Badesch DB, Barst RJ, Farber HW, Lindner JR, et al. (April 2009). "ACCF/AHA 2009 expert consensus document on pulmonary hypertension: a report of the American College of Cardiology Foundation Task Force on Expert Consensus Documents and the American Heart Association: developed in collaboration with the American College of Chest Physicians, American Thoracic Society, Inc., and the Pulmonary Hypertension Association". Circulation. 119 (16): 2250–2294.
- PMID 15194177.
- PMID 15939821.
- S2CID 1191543.
- ^ "FDA Approves Merck's Winrevair (sotatercept-csrk), a First-in-Class Treatment for Adults with Pulmonary Arterial Hypertension (PAH, WHO* Group 1)" (Press release). Merck. 27 March 2024. Retrieved 27 March 2024.
- PMID 36947725.
- PMID 23251761.
- PMID 21273054.
- ^ "Drugs@FDA: FDA-Approved Drugs".
- PMID 33765691.
- ^ "UPDATE 1-Encysive gets Canadian approval for hypertension drug". Reuters. 2008-05-30. Archived from the original on 2007-07-04. Retrieved 2007-07-08.
- ^ "U.S. Food and Drug Administration Approves Gilead's Letairis Treatment of Pulmonary Arterial Hypertension" (Press release). Gilead Sciences. 2007-06-15. Archived from the original on 2007-09-27. Retrieved 2007-06-16.
- ^ "FDA approves Adcirca (tadalafil) tablets for pulmonary arterial hypertension" (Press release). 2009-05-26. Archived from the original on 2010-12-03. Retrieved 2010-12-06.
- PMID 23668740.
- PMID 16487221.
- ^ Sally A. Arif, PharmD, BCPS (Department of Pharmacy Practice, Chicago College of Pharmacy, Midwestern University, Downers Grove, Illinois, and Department of Pharmacy, Rush University Medical Center, Chicago, Illinois); and Henry Poon, PharmD, BCPS (Department of Pharmacy, James J. Peters VA Medical Center, Bronx, New York). Tadalafil: A Long-Acting Phosphodiesterase-5 Inhibitor for the Treatment of Pulmonary Arterial Hypertension. 2011;33:993–1004
- PMID 19470885.
- ^ "Opsynvi (macitentan and tadalafil) Becomes the First and Only Health Canada-Approved Once Daily Fixed Dose Combination Treatment for Patients with Pulmonary Arterial Hypertension (PAH)". Johnson & Johnson (Press release). 15 October 2021. Retrieved 25 March 2024.
- ^ "Approval Letter: Opsynvi (macitentan and tadalafil)" (PDF). U.S. Food and Drug Administration.
- ^ "U.S. FDA Approves Opsynvi (macitentan and tadalafil) as the First and Only Once-Daily Single-Tablet Combination Therapy for Patients with Pulmonary Arterial Hypertension (PAH)". Johnson & Johnson (Press release). 22 March 2024. Retrieved 25 March 2024.
- PMID 21510726.
- PMID 22034605.
- ^ "2006 OPTN/SRTR Annual Report". US Scientific Registry of Transplant Recipients. 2006-05-01. Archived from the original on 2010-06-05. Retrieved 2007-03-28.
- PMID 12639858.
- ABIM Foundation, American College of Chest Physicians and American Thoracic Society, archivedfrom the original on 3 November 2013, retrieved 6 January 2013
- ^ Guidelines: Six-minute Walk Test. Accessed: 2015
- ^ "Pulmonary Hypertension. About Pulmonary Hypertension | Patient". Patient. Archived from the original on 2016-01-02. Retrieved 2015-12-30.
- S2CID 226272078.
- PMID 15684287.
- PMID 22281797. [FREE]
- ISBN 978-0-07-144874-1.
- ISBN 978-1-4200-8478-8.
- ^ British Journal of Anaesthesia: "Primary pulmonary hypertension in pregnancy; a role for novel vasodilators" Archived 2011-01-21 at the Wayback Machine March 19, 2011
- ^ Oudiz RJ (6 February 2023). "Idiopathic Pulmonary Arterial Hypertension: Practice Essentials, Background, Pathophysiology". Medscape Reference.
- S2CID 19528958.
- ^ Nannini C. "Lung Disease in Rheumatoid Arthritis". MedScape.com. MedScape. Archived from the original on 8 February 2016. Retrieved 31 December 2015.
- from the original on 26 October 2015. Retrieved 31 December 2015.
- PMID 17982405.
- PMID 20522579.
- PMID 25360072.
- S2CID 23641857.
- ^ "Elaine Kaufman, famed Elaine's restaurateur, dies at age 81". Daily News. 3 December 2010. Archived from the original on 28 August 2016. Retrieved 27 September 2016.
- ^ Folkart BA (21 June 1990). "Ina Balin, 52; Movie and TV Actress Sought Lung Implant". Los Angeles Times. Archived from the original on 11 September 2016. Retrieved 27 September 2016.
- ^ Phull H (July 26, 2016). "She's tethered to an oxygen tank, but her singing career is soaring". New York Post. Archived from the original on August 14, 2016.
- ^ Insdorf A (November 10, 2013). "The Challenges of Chloe Temtchine". The Huffington Post. Archived from the original on September 18, 2016.
- ^ "Autopsy: The Last Hours of Natalie Cole." Autopsy. Nar. Eric Meyers. Exec. Prod. Ed Taylor and Michael Kelpie. Reelz, 27 May 2017. Television.
Further reading
- Rubin LJ, Badesch DB (August 2005). "Evaluation and management of the patient with pulmonary arterial hypertension". Annals of Internal Medicine. 143 (4): 282–292. S2CID 28841269.
- Abman SH, Hansmann G, Archer SL, Ivy DD, Adatia I, Chung WK, et al. (November 2015). "Pediatric Pulmonary Hypertension: Guidelines From the American Heart Association and American Thoracic Society". Circulation. 132 (21): 2037–2099. S2CID 7412370.
