Pulmonary embolism
| Pulmonary embolism | |
|---|---|
DOACs)[5] | |
| Frequency | ~450,000 per year (USA), 430,000 (Europe)[6][7][8] |
| Deaths | >10–12,000 per year (US),[9] >30–40,000 per year (Europe)[10] |
Pulmonary embolism (PE) is a blockage of an
PE usually results from a blood clot in the leg that travels to the lung.
Efforts to prevent PE include beginning to move as soon as possible after surgery, lower leg exercises during periods of sitting, and the use of
Pulmonary emboli affect about 430,000 people each year in Europe.[8] In the United States, between 300,000 and 600,000 cases occur each year,[6][7] which contribute to at least 40,000 deaths.[9] Rates are similar in males and females.[3] They become more common as people get older.[3]
Signs and symptoms
Symptoms of pulmonary embolism are typically sudden in onset and may include one or many of the following:
On physical examination, the lungs are usually normal. Occasionally, a pleural friction rub may be audible over the affected area of the lung (mostly in PE with infarct). A pleural effusion is sometimes present that is exudative, detectable by decreased percussion note, audible breath sounds, and vocal resonance. Strain on the right ventricle may be detected as a left parasternal heave, a loud pulmonary component of the second heart sound, and/or raised jugular venous pressure.[2] A low-grade fever may be present, particularly if there is associated pulmonary hemorrhage or infarction.[21]
As smaller pulmonary emboli tend to lodge in more peripheral areas without collateral circulation, they are more likely to cause lung infarction and small effusions (both of which are painful), but not hypoxia, dyspnea, or hemodynamic instability such as tachycardia. Larger PEs, which tend to lodge centrally, typically cause dyspnea, hypoxia, low blood pressure, fast heart rate and fainting, but are often painless because there is no lung infarction due to collateral circulation. The classic presentation for PE with pleuritic pain, dyspnea, and tachycardia is likely caused by a large fragmented embolism causing both large and small PEs. Thus, small PEs are often missed because they cause pleuritic pain alone without any other findings and large PEs are often missed because they are painless and mimic other conditions often causing ECG changes and small rises in troponin and brain natriuretic peptide levels.[22]
PEs are sometimes described as massive, submassive, and nonmassive depending on the clinical signs and symptoms. Although the exact definitions of these are unclear, an accepted definition of massive PE is one in which there is hemodynamic instability. This is a cause of obstructive shock, which presents as sustained low blood pressure, slowed heart rate, or pulselessness.[23]
Risk factors

About 90% of emboli are from a
VTE is much more common in immunocompromised individuals as well as individuals with comorbidities including:
- Those that undergo orthopedic surgery at or below the hip without prophylaxis.[26]
- This is due to immobility during or after the surgery, as well as venous damage during the surgery.[26]
- Pancreatic and colon cancer patients (other forms of cancer also can be factors, but these are the most common)[26]
- Patients with high-grade tumors[26]
- Pregnant women[26]
- As the body puts itself into what is known as a "hypercoagulable state" the risk of a hemorrhage during childbirth is decreased and is regulated by increased expression of factors VII, VIII, X, Von Willebrand, and fibrinogen.[26]
- Those on estrogen medication[26][27][28][29]
The development of thrombosis is classically due to a group of causes named Virchow's triad (alterations in blood flow, factors in the vessel wall, and factors affecting the properties of the blood). Often, more than one risk factor is present.[citation needed]
- Alterations in blood flow: immobilization (after surgery, long-haul flight), (also procoagulant)
- Factors in the vessel wall: surgery, catheterizations causing direct injury ("endothelial injury")
- Factors affecting the properties of the blood (procoagulant state):
- Estrogen-containing medication (transgender hormone therapy, menopausal hormone therapy and hormonal contraceptives)[28][27][29]
- Genetic thrombophilia (plasminogen/fibrinolysisdisorders)
- Acquired thrombophilia (antiphospholipid syndrome, nephrotic syndrome, paroxysmal nocturnal hemoglobinuria)
- Cancer (due to secretion of pro-coagulants)
Although most pulmonary embolisms are the result of
- Risk factors include:
- Varicose veins caused by vascular damage[30]
- Pulmonary hypertension[30]
- Diabetes[30]
- Traumatic hip fractures that immobilize the patient[30]
- Joint fixation (primarily in the legs)[26]
Underlying causes
After a first PE, the search for secondary causes is usually brief. Only when a second PE occurs, and especially when this happens while still under
Diagnosis

To diagnose a pulmonary embolism, a review of clinical criteria to determine the need for testing is recommended.[32] In those who have low risk, age less than 50, heart rate less than 100 beats per minute, oxygen level more than 94% on room air, and no leg swelling, coughing up of blood, surgery or trauma in the last four weeks, previous blood clots, or estrogen use, further testing is not typically needed.[33]
In situations with more high risk individuals, further testing is needed. A
If there are concerns this is followed by testing to determine a likelihood of being able to confirm a diagnosis by imaging, followed by imaging if other tests have shown that there is a likelihood of a PE diagnosis.[32][35][36]
The diagnosis of PE is based primarily on validated clinical criteria combined with selective testing because the typical clinical presentation (shortness of breath, chest pain) cannot be definitively differentiated from other causes of chest pain and shortness of breath. The decision to perform medical imaging is based on clinical reasoning, that is, the medical history, symptoms, and findings on physical examination, followed by an assessment of clinical probability.[2]
Probability testing
The most commonly used method to predict clinical probability, the
There are additional prediction rules for PE, such as the Geneva rule. More importantly, the use of any rule is associated with reduction in recurrent thromboembolism.[43]
The
- clinically suspected DVT– 3.0 points
- alternative diagnosis is less likely than PE – 3.0 points
- tachycardia (heart rate > 100) – 1.5 points
- immobilization (≥ 3d)/surgery in previous four weeks – 1.5 points
- history of DVTor PE – 1.5 points
- hemoptysis – 1.0 points
- malignancy (with treatment within six months) or palliative – 1.0 points
Traditional interpretation[39][40][45]
- Score >6.0 – High (probability 59% based on pooled data)[35]
- Score 2.0 to 6.0 – Moderate (probability 29% based on pooled data)[35]
- Score <2.0 – Low (probability 15% based on pooled data)[35]
Alternative interpretation[39][42]
- Score > 4 – PE likely. Consider diagnostic imaging.
- Score 4 or less – PE unlikely. Consider D-dimer to rule out PE.
Recommendations for a diagnostic algorithm were published by the PIOPED investigators; however, these recommendations do not reflect research using 64 slice MDCT.[35] These investigators recommended:
- Low clinical probability. If negative D-dimer, PE is excluded. If positive D-dimer, obtain MDCT and base treatment on results.
- Moderate clinical probability. If negative D-dimer, PE is excluded. However, the authors were not concerned that a negative MDCT with negative D-dimer in this setting has a 5% probability of being false. Presumably, the 5% error rate will fall as 64 slice MDCT is more commonly used. If positive D-dimer, obtain MDCT and base treatment on results.
- High clinical probability. Proceed to MDCT. If positive, treat, if negative, more tests are needed to exclude PE. A D-dimer of less than 750 ug/L does not rule out PE in those who are at high risk.[46]
Pulmonary embolism rule-out criteria
The pulmonary embolism rule-out criteria (PERC) helps assess people in whom pulmonary embolism is suspected, but unlikely. Unlike the Wells score and Geneva score, which are clinical prediction rules intended to risk stratify people with suspected PE, the PERC rule is designed to rule out the risk of PE in people when the physician has already stratified them into a low-risk category.[47][45]
People in this low risk category without any of these criteria may undergo no further testing for PE: low oxygen saturations –
Blood tests
In people with a low or moderate suspicion of PE, a normal D-dimer level (shown in a blood test) is enough to exclude the possibility of thrombotic PE, with a three-month risk of thromboembolic events being 0.14%.[49] D-dimer is highly sensitive but not specific (specificity around 50%). In other words, a positive D-dimer is not synonymous with PE, but a negative D-dimer is, with a good degree of certainty, an indication of absence of a PE.[50] A low pretest probability is also valuable in ruling out PE.[51] The typical cut off is 500 μg/L, although this varies based on the assay.[52] However, in those over the age of 50, changing the cut-off value to the person's age multiplied by 10 μg/L (accounting for assay which has been used) is recommended as it decreases the number of falsely positive tests without missing any additional cases of PE.[33][52][53]
When a PE is being suspected, several
Troponin levels are increased in between 16 and 47% with pulmonary embolism.[55]
Imaging
In typical people who are not known to be at high risk of PE, imaging is helpful to confirm or exclude a diagnosis of PE after simpler first-line tests are used.[32][35][56] Medical societies recommend tests such as the D-dimer to first provide supporting evidence for the need for imaging, and imaging would be done if other tests confirmed a moderate or high probability of finding evidence to support a diagnosis of PE.[35][56]
Ultrasound of the legs can confirm the presence of a PE but cannot rule it out.[58]
CT pulmonary angiography
-
On CT scan, pulmonary emboli can be classified according to the level along the arterial tree.
-
Segmental and subsegmental pulmonary emboli on both sides
-
CT pulmonary angiography showing a "saddle embolus" at the bifurcation of the main pulmonary artery and thrombus burden in the lobar arteries on both sides.
-
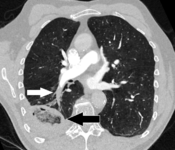
Pulmonary embolism (white arrow) that has been long-standing and has caused areverse halo sign.
Assessing the accuracy of CT pulmonary angiography is hindered by the rapid changes in the number of rows of detectors available in multidetector CT (MDCT) machines.
Ventilation/perfusion scan
(B) After intravenous injection of 4 mCi of Technetium-99m-labeled albumin
A
Low probability diagnostic tests/non-diagnostic tests
Tests that are frequently done that are not
- Hampton's hump).
- ultrasonography of the legs, is in itself enough to warrant anticoagulation, without requiring the V/Q or spiral CT scans (because of the strong association between DVT and PE). This may be a valid approach in pregnancy, in which the other modalities would increase the risk of birth defects in the unborn child. However, a negative scan does not rule out PE, and low-radiation dose scanning may be required if the mother is deemed at high risk of having a pulmonary embolism. The main use of ultrasonography of the legs is therefore in those with clinical symptoms suggestive of deep vein thrombosis.[66]
Fluoroscopic pulmonary angiography
Historically, the gold standard for diagnosis was pulmonary angiography by fluoroscopy, but this has fallen into disuse with the increased availability of non-invasive techniques that offer similar diagnostic accuracy.[69]
Electrocardiogram

The primary use of the ECG is to rule out other causes of chest pain.
This is occasionally present (occurring in up to 20% of people), but may also occur in other acute lung conditions, and, therefore, has limited diagnostic value. The most commonly seen signs in the ECG are sinus tachycardia, right axis deviation, and right bundle branch block.[73] Sinus tachycardia, however, is still only found in 8–69% of people with PE.[74]
ECG findings associated with pulmonary emboli may suggest worse prognosis since the six findings identified with RV strain on ECG (heart rate > 100 beats per minute, S1Q3T3, inverted T waves in leads V1-V4, ST elevation in aVR, complete right bundle branch block, and atrial fibrillation) are associated with increased risk of circulatory shock and death.[75]
Cases with inverted T in leads V1-3 are suspected with PE or inferior myocardial infarction. PE cases show inverted T waves in leads II and aVF, but inferior myocardial infarction cases do not show inverted T waves in II and aVF.[76]
Echocardiography
In massive and submassive PE, dysfunction of the right side of the heart may be seen on
The specific appearance of the right ventricle on echocardiography is referred to as the McConnell's sign. This is the finding of akinesia of the mid-free wall but a normal motion of the apex. This phenomenon has a 77% sensitivity and a 94% specificity for the diagnosis of acute pulmonary embolism in the setting of right ventricular dysfunction.[79]
Prevention
Pulmonary embolism may be preventable in those with risk factors. People admitted to hospital may receive preventative medication, including unfractionated
Following the completion of anticoagulation in those with prior PE, long-term aspirin is useful to prevent recurrence.[5]
Treatment
Anticoagulation
Anticoagulant therapy is the mainstay of treatment. For many years,
In recent years, many anticoagulants have been introduced that offer similar to warfarin but without a need for titration to the INR. Known as the directly acting oral anticoagulants, these treatments are now preferred over vitamin K antagonists by American professional guidelines.[5] Two of these (rivaroxaban and apixaban) do not require initial heparin or fondaparinux treatment, whereas dabigatran and edoxaban do.[5] A Cochrane review found that there is no evidence of a difference between oral DTIs (dabigatran, rivaroxaban, edoxaban, apixaban) and standard anticoagulation in the prevention of recurrent pulmonary embolism.[85]
In people with cancer who develop pulmonary embolism, therapy with a course of LMWH is favored over warfarin or other oral anticoagulants.
Anticoagulation therapy is usually continued for 3–6 months, or "lifelong" if there have been previous DVTs or PEs, or none of the usual transient risk factors is present.[5][86] In those without a known cause that can be reversed 2 years of treatment may be better than 6 months.[87] For those with small PEs (known as subsegmental PEs) the effects of anticoagulation is unknown as it has not been properly studied as of 2020.[88]
Thrombolysis
Massive PE causing hemodynamic instability (shock and/or low blood pressure, defined as a systolic blood pressure <90 mmHg or a pressure drop of 40 mmHg for >15 min if not caused by new-onset arrhythmia, hypovolemia or sepsis) is an indication for
The use of thrombolysis in non-massive PEs is still debated.[93][94] Some have found that the treatment decreases the risk of death and increases the risk of bleeding including intracranial hemorrhage.[95] Others have found no decrease in the risk of death.[94]
Inferior vena cava filter

There are two situations when an inferior vena cava filter is considered advantageous, and those are if anticoagulant therapy is contraindicated (e.g. shortly after a major operation), or a person has a pulmonary embolus in spite of being anticoagulated.[86] In these instances, it may be implanted to prevent new or existing DVTs from entering the pulmonary artery and combining with an existing blockage.[86] In spite of the device's theoretical advantage of preventing pulmonary emboli, there is a lack of evidence supporting its effectiveness.[96]
Inferior vena cava filters should be removed as soon as it becomes safe to start using anticoagulation.[86] Although modern filters are meant to be retrievable, complications may prevent some from being removed. The long-term safety profile of permanently leaving a filter inside the body is not known.[96]
Surgery
Surgical management of acute pulmonary embolism (pulmonary thrombectomy) is uncommon and has largely been abandoned because of poor long-term outcomes. However, recently, it has gone through a resurgence with the revision of the surgical technique and is thought to benefit certain people.[97] Chronic pulmonary embolism leading to pulmonary hypertension (known as chronic thromboembolic hypertension) is treated with a surgical procedure known as a pulmonary thromboendarterectomy.[98]
Prognosis

Fewer than 5 to 10% of symptomatic PEs are fatal within the first hour of symptoms.[36][90]
There are several markers used for risk stratification and these are also independent predictors of adverse outcomes. These include hypotension, cardiogenic shock, syncope, evidence of right heart dysfunction, and elevated cardiac enzymes.[36] Some ECG changes including S1Q3T3 also correlate with a worse short-term prognosis.[23] There have been other patient-related factors such as COPD and chronic heart failure thought to also play a role in prognosis.[36]
Prognosis depends on the amount of lung that is affected and on the co-existence of other medical conditions; chronic embolisation to the lung can lead to pulmonary hypertension. After a massive PE, the embolus must be resolved somehow if the patient is to survive. In thrombotic PE, the blood clot may be broken down by fibrinolysis, or it may be organized and recanalized so that a new channel forms through the clot. Blood flow is restored most rapidly in the first day or two after a PE.[99] Improvement slows thereafter and some deficits may be permanent. There is controversy over whether small subsegmental PEs need treatment at all[100] and some evidence exists that patients with subsegmental PEs may do well without treatment.[62][101]
Once anticoagulation is stopped, the risk of a fatal pulmonary embolism is 0.5% per year.[102]
Mortality from untreated PEs was said to be 26%. This figure comes from a trial published in 1960 by Barrit and Jordan, which compared anticoagulation against placebo for the management of PE. Barritt and Jordan performed their study in the Bristol Royal Infirmary in 1957.[103] This study is the only placebo-controlled trial ever to examine the place of anticoagulants in the treatment of PE, the results of which were so convincing that the trial has never been repeated as to do so would be considered unethical.[citation needed] That said, the reported mortality rate of 26% in the placebo group is probably an overstatement, given that the technology of the day may have detected only severe PEs.[104]
Predicting mortality
The PESI and sPESI (= simplified Pulmonary Embolism Severity Index) scoring tools can estimate mortality of patients. The Geneva prediction rules and Wells criteria are used to calculate a pre-test probability of patients to predict who has a pulmonary embolism. These scores are tools to be used with clinical judgment in deciding diagnostic testing and types of therapy.[105] The PESI algorithm comprises 11 routinely available clinical variables.[106] It puts the subjects into one of five classes (I–V), with 30-day mortality ranging from 1.1% to 24.5%. Those in classes I and II are low-risk and those in classes III–V are high-risk.[106]
Epidemiology
There are roughly 10 million cases of pulmonary embolisms per year.[26] In the United States, pulmonary embolisms are the primary cause of at least 10,000 to 12,000 deaths per year and a contributing cause in at least 30,000 to 40,000 deaths per year.[9] True incidence involving pulmonary embolisms is unknown because they often go undiagnosed or unnoticed until autopsy.[26] From 1993 to 2012, there have been an increased number of admissions in hospitals due to pulmonary embolisms, jumping from 23 cases per 100,000 people to 65 cases per 100,000 people.[26] Despite this increase, there has been a decrease in mortality during that same time period due to medical advances that have occurred.[26]
When looking at all cases, the rate of fatal pulmonary emboli has declined from 6% to 2% over the last 25 years in the United States.[107] In Europe, an average of approximately 40,000 deaths per year with pulmonary embolism as the primary cause were reported between 2013 and 2015, a conservative estimate because of potential underdiagnosis.[10]
References
- ^ a b c "What Are the Signs and Symptoms of Pulmonary Embolism?". NHLBI. July 1, 2011. Archived from the original on 9 March 2016. Retrieved 12 March 2016.
- ^ ISBN 978-0-07-139140-5.
- ^ a b c d e "Who Is at Risk for Pulmonary Embolism?". NHLBI. July 1, 2011. Archived from the original on 15 February 2016. Retrieved 12 March 2016.
- ^ a b c d "How Is Pulmonary Embolism Diagnosed?". NHLBI. July 1, 2011. Archived from the original on 7 April 2016. Retrieved 12 March 2016.
- ^ PMID 26867832.
- ^ a b c d "What Is Pulmonary Embolism?". NHLBI. July 1, 2011. Archived from the original on 12 March 2016. Retrieved 12 March 2016.
- ^ PMID 15650680.
- ^ PMID 25304324.
- ^ PMID 33058771.
- ^ S2CID 204740186.
- ISBN 978-0-07-148480-0.
- S2CID 25712161. Retrieved 18 November 2022.
- ^ "What Causes Pulmonary Embolism?". NHLBI. July 1, 2011. Archived from the original on 7 April 2016. Retrieved 12 March 2016.
- PMID 24804726.
- ^ "Other Names for Pulmonary Embolism". July 1, 2011. Archived from the original on 16 March 2016. Retrieved 12 March 2016.
- ^ "How Can Pulmonary Embolism Be Prevented?". NHLBI. July 1, 2011. Archived from the original on 7 April 2016. Retrieved 12 March 2016.
- PMID 23724389.
- ^ a b "How Is Pulmonary Embolism Treated?". NHLBI. July 1, 2011. Archived from the original on 9 March 2016. Retrieved 12 March 2016.
- ^ ISBN 978-0-323-08678-3.
- S2CID 5012417.
- PMID 19268750.
- ^ Pregerson DB, Quick Essentials: Emergency Medicine, 4th edition. EMresource.org [ISBN missing][page needed]
- ^ PMID 21422387.
- ^ Ferri F (2012). Ferri's Clinical Advisor. St. Louis: Mosby's.
- PMID 29494023.
- ^ PMID 29872243.
- ^ S2CID 43061502.
- ^ PMID 20163835.
- ^ PMID 33005118.
- ^ S2CID 210131969.
- ^ "Pulmonary embolus". MedlinePlus Medical Encyclopedia. Archived from the original on 25 April 2017. Retrieved 24 April 2017.
- ^ ABIM Foundation. American College of Radiology. Archived(PDF) from the original on April 16, 2012. Retrieved August 17, 2012.
- ^ PMID 26414967.
- ^ doi:10.47144/phj.v52i2.1763 (inactive 31 January 2024).)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - ^ PMID 17185658.
- ^ PMID 25173341.
- ^ S2CID 23107192.
- ^ S2CID 41389736.
- ^ S2CID 10013631.
- ^ S2CID 2708155.
- S2CID 26531577.
- ^ PMID 16403929.
- S2CID 38894349.
- from the original on 2007-09-26.
- ^ S2CID 17476982.
- PMID 27873439.
- ^ S2CID 25488146.
- S2CID 19311896.
- S2CID 23851417.
- PMID 12928229.
- PMID 27494075.
- ^ PMID 23645857.
- S2CID 207538572.
- ^ Werman HA, Karren K, Mistovich J (2014). "Other Conditions That Cause Respiratory Distress: Pulmonary Embolism". In Howard WA, Mistovich J, Karren K (eds.). Prehospital Emergency Care, 10e. Pearson Education, Inc. p. 456.
- S2CID 39899682.
- ^ PMID 18757870.
- ^ PMID 19949025.
- PMID 27377039.
- PMID 28124411.
- S2CID 6074.
- S2CID 38746246.
- ^ PMID 16738268.
- PMID 18165667.
- from the original on 2007-09-04.
- PMID 22086989.
- ^ a b c Thomson AJ, Greer IA (April 2015). "Thrombosis and Embolism during Pregnancy and the Puerperium, the Acute Management of (Green-top Guideline No. 37b)". Royal College of Obstetricians & Gynaecologists. Retrieved 4 June 2018.
- PMID 24213621.
- PMID 8372182.
- PMID 25173341.
Pulmonary angiography has for decades remained the 'gold standard' for the diagnosis or exclusion of PE but is rarely performed now as less-invasive CT angiography offers similar diagnostic accuracy.
- ^ PMID 16189038.
- ISBN 978-0470755174. Archivedfrom the original on 2017-09-08.
- .
- PMID 11018210.
- ISBN 978-1-4051-4166-6.
- PMID 26394330.
- PMID 24062927.
- PMID 14597581.
- PMID 22082681.
- PMID 8752195.
- ^ a b "UOTW #2 Answer - Ultrasound of the Week". Ultrasound of the Week. 16 June 2014. Archived from the original on 12 January 2017. Retrieved 27 May 2017.
- National Institute for Health and Clinical Excellence. Clinical guideline 92: Venous thromboembolism: reducing the risk: Reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital. London, January 2010.
- PMID 22944455.
- PMID 26756331.
- ^ PMID 28182249.
- PMID 37057837.
- ^ National Institute for Health and Clinical Excellence. Clinical guideline 144: Venous thromboembolic diseases: the management of venous thromboembolic diseases and the role of thrombophilia testing. London, 2012.
- S2CID 182950850.
- PMID 32030721.
- PMID 31258361.
- ^ S2CID 207614432.
- PMID 19875060.
- PMID 24497337.
- PMID 33857326.
- ^ S2CID 21881585.
- PMID 24938564.
- ^ S2CID 222216149.
- PMID 15339878.
- ISBN 978-1-4987-1991-9.
- PMID 5475816.
- S2CID 20515117.
- PMID 16738276.
- S2CID 29062377.
- PMID 13797091.
- PMID 4869238.
- PMID 17625081.
- ^ PMID 23210843.
- ISBN 978-81-312-1036-9.
External links
- Pulmonary embolism at Curlie
- Wells criteria for pulmonary embolism online calculator Archived 2016-11-21 at the Wayback Machine
- Clinical prediction website – Wells criteria for pulmonary embolism
 Media related to Pulmonary embolism at Wikimedia Commons
Media related to Pulmonary embolism at Wikimedia Commons- "Pulmonary Embolism". MedlinePlus. U.S. National Library of Medicine.