Rhabdomyolysis
| Rhabdomyolysis | |
|---|---|
| Frequency | 26,000 reported cases per year (U.S.)[3] |
Rhabdomyolysis (shortened as rhabdo) is a condition in which damaged
The muscle damage is most usually caused by a
The mainstay of treatment is large quantities of
Rhabdomyolysis is reported about 26,000 times a year in the United States.[3] While the condition has been commented on throughout history, the first modern description was following an earthquake in 1908.[11] Important discoveries as to its mechanism were made during the Blitz of London in 1941.[11] It is a significant problem for those injured in earthquakes, and relief efforts for such disasters often include medical teams equipped to treat survivors with rhabdomyolysis.[11]
Signs and symptoms
The symptoms of rhabdomyolysis depend on its severity and whether kidney failure develops. Milder forms may not cause any muscle symptoms, and the diagnosis is based on abnormal
Swelling of damaged muscle occasionally leads to compartment syndrome—compression of surrounding tissues, such as nerves and blood vessels, in the same fascial compartment—leading to the loss of blood supply and damage or loss of function in the part(s) of the body supplied by these structures. Symptoms of this complication include pain or reduced sensation in the affected limb.[3][12] A second recognized complication is disseminated intravascular coagulation (DIC), a severe disruption in blood clotting that may lead to uncontrollable bleeding.[3][4][12]
Causes
Any form of muscle damage of sufficient severity can cause rhabdomyolysis.[4] Multiple causes can be present simultaneously in one person.[10] Some have an underlying muscle condition, usually hereditary in nature, that makes them more prone to rhabdomyolysis.[10][12]
| Type | Causes |
|---|---|
| Exercise-related | Extreme physical exercise (particularly when poorly hydrated), delirium tremens (alcohol withdrawal), tetanus, prolonged seizures or status epilepticus[4][10]
|
| Crush | Crush syndrome, blast injury, car accident, physical torture or abuse, or confinement in a fixed position such as after a stroke, due to alcohol intoxication or in prolonged surgery[4][10] |
| Blood supply | Arterial thrombosis (blood clots forming locally) or embolism (clots or other debris from elsewhere in the body), clamping of an artery during surgery[4][10] |
| Metabolism | Hyperglycemic hyperosmolar state, hyper- and hyponatremia (elevated or reduced blood sodium levels), hypokalemia (low potassium levels), hypocalcemia (low calcium levels), hypophosphatemia (low phosphate levels), ketoacidosis (e.g., in diabetic ketoacidosis) or hypothyroidism (abnormally low thyroid function)[4][10][12]
|
| Body temperature | Hyperthermia (high body temperature) and heat illness, hypothermia (very low body temperature)[4][10] |
| Drugs and toxins | Many medications increase the risk of rhabdomyolysis.[13] The most important ones are:[4][10][12]
Poisons linked to rhabdomyolysis are heavy metals and venom from insects or snakes.[4] Hemlock may cause rhabdomyolysis, either directly or after eating quail that have fed on it.[4][12] Fungi such as Russula subnigricans and Tricholoma equestre are known to cause rhabdomyolysis.[15] Haff disease is rhabdomyolysis after consuming fish; a toxic cause is suspected but has not been proven.[16]
Drugs of recreational use, including: alcohol, amphetamine, cocaine, heroin, ketamine and MDMA (ecstasy)[4][12] |
| Infection | primary HIV infection, Plasmodium falciparum (malaria), herpes viruses, Legionella pneumophila and salmonella[4][10][12]
|
| Inflammation | Autoimmune muscle damage: polymyositis, dermatomyositis[4][12] |
Genetic predisposition
Recurrent rhabdomyolysis may result from intrinsic muscle enzyme deficiencies, which are usually inherited and often appear during childhood.[10][13] Many structural muscle diseases feature episodes of rhabdomyolysis that are triggered by exercise, general anesthesia or any of the other causes of rhabdomyolysis listed above.[10] Inherited muscle disorders and infections together cause the majority of rhabdomyolysis in children.[13]
The following hereditary disorders of the muscle energy supply may cause recurrent and usually exertional rhabdomyolysis:[10][13][17]
- XI
- deficiency
- Mitochondrial myopathies: deficiency of succinate dehydrogenase, cytochrome c oxidase and coenzyme Q10
- Others: myoadenylate deaminase deficiency and muscular dystrophies
Mechanism

Damage to skeletal muscle may take various forms. Crush and other physical injuries cause damage to
The swollen, inflamed muscle may directly compress structures in the same
Rhabdomyolysis may cause kidney failure by several mechanisms. The most important is the accumulation of myoglobin in the
Diagnosis

A diagnosis of rhabdomyolysis may be suspected in anyone who has sustained trauma, crush injury or prolonged immobilization, but it may also be identified at a later stage due to deteriorating kidney function (abnormally raised or increasing creatinine and urea levels, falling urine output) or reddish-brown discoloration of the urine.[4][11]
General investigations
The most reliable test in the diagnosis of rhabdomyolysis is the level of creatine kinase (CK) in the blood.[5] This enzyme is released by damaged muscle, and levels above 1000 U/L (5 times the upper limit of normal (ULN)) indicate rhabdomyolysis.[5] More than 5,000 U/L indicates severe disease but depending on the extent of the rhabdomyolysis, concentrations up to 100,000 U/l are not unusual.[5][11] CK concentrations rise steadily for 12 hours after the original muscle injury, remain elevated for 1–3 days and then fall gradually.[4] Initial and peak CK levels have a linear relationship with the risk of acute kidney failure: the higher the CK, the more likely it is that kidney damage will occur.[19] There is no specific concentration of CK above which kidney impairment definitely occurs; concentrations below 20,000 U/L are unlikely to be associated with a risk of kidney impairment, unless there are other contributing risk factors. Mild rises without kidney impairment are referred to as "hyperCKemia".[10][18] Myoglobin has a short half-life, and is therefore less useful as a diagnostic test in the later stages.[4] Its detection in blood or urine is associated with a higher risk of kidney impairment.[19] Despite this, use of urine myoglobin measurement is not supported by evidence as it lacks specificity and the research studying its utility is of poor quality.[20]
Elevated concentrations of the enzyme
High potassium levels tend to be a feature of severe rhabdomyolysis.[4] Electrocardiography (ECG) may show whether the elevated potassium levels are affecting the conduction system of the heart, as suggested by the presence of T wave changes or broadening of the QRS complex.[21] Low calcium levels may be present in the initial stage due to binding of free calcium to damaged muscle cells.[4]
As detectable levels of
Complications
Disseminated intravascular coagulation, another complication of rhabdomyolysis and other forms of critical illness, may be suspected on the basis of unexpected bleeding or abnormalities in hematological tests, such as a decreasing platelet count or prolongation of the prothrombin time. The diagnosis can be confirmed with standard blood tests for DIC, such as D-dimer.[24]
Underlying disorders
If an underlying muscle disease is suspected, for instance, if there is no obvious explanation or there have been multiple episodes, it may be necessary to perform further investigations.[13] During an attack, low levels of carnitine in the blood and high levels of acylcarnitine in blood and urine may indicate a lipid metabolism defect, but these abnormalities revert to normal during convalescence. Other tests may be used at that stage to demonstrate these disorders.[12] Disorders of glycolysis can be detected by various means, including the measurement of lactate after exercise; a failure of the lactate to rise may be indicative of a disorder in glycolysis,[12] while an exaggerated response is typical of mitochondrial diseases.[17] Electromyography (EMG) may show particular patterns in specific muscle diseases; for instance, McArdle's disease and phosphofructokinase deficiency show a phenomenon called cramp-like contracture.[18] There are genetic tests available for many of the hereditary muscle conditions that predispose to myoglobinuria and rhabdomyolysis.[12][13]
Muscle biopsy can be useful if an episode of rhabdomyolysis is thought to be the result of an underlying muscle disorder. A biopsy sample taken during an episode is often uninformative, as it will show only evidence of cell death or may appear normal. Taking the sample is therefore delayed for several weeks or months.[10] The histopathological appearance on the biopsy indicates the nature of the underlying disorder. For instance, mitochondrial diseases are characterized by ragged red fibers.[12] Biopsy sites may be identified by medical imaging, such as magnetic resonance imaging, as the muscles may not be uniformly affected.[17]
Treatment
The main goal of treatment is to treat shock and preserve kidney function. Initially this is done through the administration of generous amounts of
While many sources recommend additional intravenous agents to reduce damage to the kidney, most of the evidence supporting this practice comes from animal studies, and is inconsistent and conflicting.
Electrolytes
In the initial stages, electrolyte levels are often abnormal and require correction. High potassium levels can be life-threatening, and respond to increased urine production and renal replacement therapy (see below).[12] Temporary measures include the administration of calcium to protect against cardiac complications, insulin or salbutamol to redistribute potassium into cells, and infusions of bicarbonate solution.[21]
Calcium levels initially tend to be low, but as the situation improves calcium is released from where it has precipitated with phosphate, and vitamin D production resumes, leading to
Acute kidney impairment
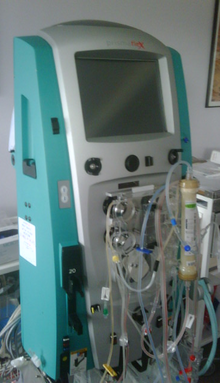
Kidney dysfunction typically develops 1–2 days after the initial muscle damage.[4] If supportive treatment is inadequate to manage this, renal replacement therapy (RRT) may be required.[13] RRT removes excess potassium, acid and phosphate that accumulate when the kidneys are unable to function normally and is required until kidney function is regained.[4]
Three main modalities of RRT are available: hemodialysis, continuous hemofiltration and peritoneal dialysis. The former two require access to the bloodstream (a dialysis catheter) and peritoneal dialysis is achieved by instilling fluid into the abdominal cavity and later draining it. Hemodialysis, which is normally done several times a week in chronic kidney disease, is often required on a daily basis in rhabdomyolysis. Its advantage over continuous hemofiltration is that one machine can be used multiple times a day, and that continuous administration of anticoagulant drugs is not necessary.[11][25] Hemofiltration is more effective at removing large molecules from the bloodstream, such as myoglobin,[13] but this does not seem to confer any particular benefit.[4][11] Peritoneal dialysis may be difficult to administer in someone with severe abdominal injury,[11] and it may be less effective than the other modalities.[4]
Other complications
Compartment syndrome is treated with surgery to relieve the pressure inside the muscle compartment and reduce the risk of compression on blood vessels and nerves in that area. Fasciotomy is the incision of the affected compartment. Often, multiple incisions are made and left open until the swelling has reduced. At that point, the incisions are closed, often requiring debridement (removal of non-viable tissue) and skin grafting in the process.[23] The need for fasciotomy may be decreased if mannitol is used, as it can relieve muscle swelling directly.[25][26]
Prognosis
The prognosis depends on the underlying cause and whether any complications occur. Rhabdomyolysis complicated by acute kidney impairment in patients with traumatic injury may have a mortality rate of 20%.[4] Admission to the intensive care unit is associated with a mortality of 22% in the absence of acute kidney injury, and 59% if kidney impairment occurs.[10] Most people who have sustained kidney impairment due to rhabdomyolysis fully recover their kidney function.[10]
Epidemiology
The exact number of cases of rhabdomyolysis is difficult to establish because different definitions have been used.[3][10] In 1995, hospitals in the U.S. reported 26,000 cases of rhabdomyolysis.[3] Up to 85% of people with major traumatic injuries will experience some degree of rhabdomyolysis.[4] Of those with rhabdomyolysis, 10–50% develop acute kidney injury.[4][10] The risk is higher in people with a history of illicit drug use, alcohol misuse or trauma when compared to muscle diseases, and it is particularly high if multiple contributing factors occur together.[10] Rhabdomyolysis accounts for 7–10% of all cases of acute kidney injury in the U.S.[10][13]
Crush injuries are common in major disasters, especially in earthquakes. The aftermath of the
Acute exertional rhabdomyolysis happens in 2% to 40% of people going through basic training for the United States military. In 2012, the United States military reported 402 cases.[29] Another group at increased risk is firefighters.[30]
History

The Bible may contain an early account of rhabdomyolysis. In Numbers 11:4–6,31–33, the Pentateuch says that the Jews demanded meat while traveling in the desert; God sent quail in response to the complaints, and people ate large quantities of quail meat. A plague then broke out, killing numerous people. Rhabdomyolysis after consuming quail was described in more recent times and called coturnism (after Coturnix, the main quail genus).[12][31] Migrating quail consume large amounts of hemlock, a known cause of rhabdomyolysis.[4]
In modern times, early reports from the 1908 Messina earthquake and World War I on kidney failure after injury were followed by studies by London physicians Eric Bywaters and Desmond Beall, working at the Royal Postgraduate Medical School and the National Institute for Medical Research, on four victims of The Blitz in 1941.[12][32][33] Myoglobin was demonstrated in the urine of victims by spectroscopy, and it was noted that the kidneys of victims resembled those of patients who had hemoglobinuria (hemoglobin rather than myoglobin being the cause of the kidney damage). In 1944 Bywaters demonstrated experimentally that the kidney failure was mainly caused by myoglobin.[11][33] Already during the war, teams of doctors traveled to bombed areas to provide medical support, chiefly with intravenous fluids, as dialysis was not yet available.[33] The prognosis of acute kidney failure improved markedly when dialysis was added to supportive treatment, which first happened during the 1950–1953 Korean War.[34]
Etymology and pronunciation
The word rhabdomyolysis ( , yielding "striated muscle breakdown".
Other animals
Rhabdomyolysis is recognized in horses.[35] Horses can develop a number of muscle disorders, many of which may progress to rhabdomyolysis. Of these, some cause isolated attacks of rhabdomyolysis (e.g., dietary deficiency in vitamin E and selenium, poisoning associated with pasture or agricultural poisons such as organophosphates), while others predispose to exertional rhabdomyolysis (e.g., the hereditary condition equine polysaccharide storage myopathy).[36] 5–10% of thoroughbred horses and some standardbred horses have the condition equine exertional rhabdomyolysis; no specific cause has been identified, but an underlying muscle calcium regulation disorder is suspected.[36]
Rhabdomyolysis affecting horses may also occur in outbreaks; these have been reported in many European countries, and later in Canada, Australia, and the United States. It has been referred to as "atypical myopathy" or "myoglobinuria of unknown etiology". No single cause has yet been found, but various mechanisms have been proposed,[37] and a seasonal pattern has been observed.[36] Very high creatine kinase levels are detected, and mortality from this condition is 89%.[36]
References
- ^ "Rhabdomyolysis". Merriam-Webster.com Dictionary.
- ^ "Rhabdomyolysis". Dictionary.com Unabridged (Online). n.d.
- ^ PMID 11898964.
- ^ PMID 15774072.
- ^ PMID 27301374.
- ^ "What is Rhabdo? | NIOSH | CDC". www.cdc.gov. 3 December 2021. Retrieved 15 December 2022.
- PMID 35136842.
- S2CID 254067955. Retrieved 6 July 2023.
- ^ S2CID 3239804.
- ^ S2CID 4652812.
- ^ PMID 10906171.
- ^ S2CID 8731940.
- ^ S2CID 206999992.
- ^ S2CID 205948651.
- S2CID 24320633.
- PMID 10756156.
- ^ PMID 16214072.
- ^ ISBN 978-0-07-141620-7.
- ^ S2CID 25592319.
- PMID 19797717.
- ^ S2CID 7382802.
- ^ S2CID 10658749.
- ^ PMID 20858378.
- S2CID 260317250.
- ^ PMID 16525142.
- ^ PMID 15015795.
- PMID 16861256.
- S2CID 7158989.
- S2CID 11263725.
- PMID 32166015.
- PMID 4904256.
- PMID 9527411.
- ^ PMID 2279155.
- PMID 15232604.
- ^ "Overview of Myopathies in Horses". Merck Veterinary Manual, 10th edition (online version). 2012. Archived from the original on 26 December 2013. Retrieved 25 December 2013.
- ^ S2CID 14452155.
- PMID 18375157.
