Schistocyte

A schistocyte or schizocyte (from
Several
Schistocytes are often seen in patients with
Appearance
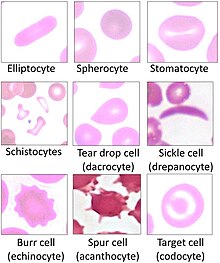
Schistocytes are fragmented
Pathophysiology
Schistocyte formation occurs as a result of mechanical destruction (fragmentation hemolysis) of a normal red blood cell. This occurs when there is damage to the blood vessel and a clot begins to form. The formation of the fibrin strands in the vessels occurs as part of the clot formation process. The red blood cells get trapped in the fibrin strands and the shear force of the blood flow causes the red blood cell to break. The resulting fragmented cell is called the schistocyte.[3]
Schistocyte count
A normal schistocyte count for a healthy individual is <0.5% although usual values are found to be <0.2%. A schistocyte count of >1% is most often found in
Conditions
Schistocytes on the peripheral blood smear is a characteristic feature of
Disseminated intravascular coagulation
Disseminated intravascular coagulation or DIC is caused by a systemic response to a specific condition including sepsis and severe infection, malignancy, obstetric complications, massive tissue injury, or systemic diseases. Disseminated intravascular coagulation is an activation of the coagulation cascade which is usually a result of an increased exposure to tissue factor. The activation of the cascade leads to thrombi formation which causes an accumulation of excess fibrin formation in the intravascular circulation. The excess fibrin strands cause mechanical damage to the red blood cells resulting in schistocyte formation and also thrombocytopenia and consumption of clotting factors. Schistocyte values between .5% and 1% are usually suggestive of DIC.[7]
Thrombotic thrombocytopenic purpura
Thrombotic thrombocytopenic purpura or TTP is caused by primary platelet activation. Thrombotic thrombocytopenic purpura leads to increased amounts of large von Willebrand factor which then attach to activated platelets and mediate further platelet aggregation. Platelets end up being removed and the resulting fibrin strand formation remains. These fibrin strands along with the stress from the blood flow cause fragmentation of the red blood cells, leading to schistocyte formation. In TTP, a schistocyte count between 3–10% is common, but >1% is suggestive of the disease.[7]
Hemolytic-uremic syndrome
Malfunctioning cardiac valves
Leaky prosthetic heart valves and other cardiac assisted devices can lead to microangiopathic hemolytic anemia (with schistocyte formation) and thrombocytopenia. The force from the blood flow over the high pressure gradient from the prosthesis leads to fragmentation of red cells, and schistocyte formation. This is rare and only occurs in about 3% of patients.[6]
References
- S2CID 21161811.
- S2CID 222200776.
- PMID 5412670.
- S2CID 9357529.
- PMID 15182097.
- ^ a b Schrier, Stanley. "Extrinsic nonimmune hemolytic anemia due to mechanical damage: Fragmentation hemolysis and hypersplenism". UpToDate.
- ^ a b c Suri, Mandeep. "Disseminated Intravascular Coagulation (DIC)". Fastbleep Medical Notes. Archived from the original on 2015-03-04. Retrieved 2014-12-08.
External links
- Images in Clinical Medicine: Hemolytic Anemia after Mitral-Valve Repair, Sarinya Puwanant and Watchara Lohawijarn, N Engl J Med 2012; 367:e29 (November 15, 2012) DOI: 10.1056/NEJMicm1201695 [FREE TEXT]
