Sickle cell disease
| Sickle cell disease | |
|---|---|
| Other names | Sickle cell disorder; drepanocytosis (dated) |
| Prognosis | Life expectancy 40–60 years (developed world)[2] |
| Frequency | 4.4 million (2015)[7] |
| Deaths | 114,800 (2015)[8] |
Sickle cell disease (SCD), also simply called sickle cell, is a group of
Sickle cell disease occurs when a person inherits two abnormal copies of the
The care of people with sickle cell disease may include infection prevention with
As of 2015[update], about 4.4 million people have sickle cell disease, while an additional 43 million have sickle cell trait.[7][12] Sickle cell disease (SCD) affects millions of people worldwide, with a higher prevalence in sub-Saharan Africa, Spanish-speaking regions in the Western Hemisphere (South America, the Caribbean, and Central America), Saudi Arabia, India, and Mediterranean countries like Turkey, Greece, and Italy.[13] In 2015, it resulted in about 114,800 deaths.[8] The condition was first described in the medical literature by American physician James B. Herrick in 1910.[14][15] In 1949, its genetic transmission was determined by E. A. Beet and J. V. Neel.[15] In 1954, the protective effect against malaria of sickle cell trait was described.[15]
Signs and symptoms

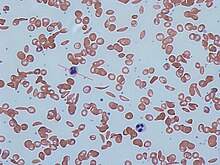

Signs of sickle cell disease usually begin in early childhood. The severity of symptoms can vary from person to person, as can the frequency of crisis events.[16][17] Sickle cell disease may lead to various acute and chronic complications, several of which have a high mortality rate.[18]
First events
The usual characteristics of the first event leading to a diagnosis of SCD depend on the age of the child. When the disease presents within the first year of life, the most common problem is an episode of pain and swelling in their hands and feet, known as dactylitis or "hand-foot syndrome." Pallor, jaundice, and fatigue can also be early signs due to anemia resulting from sickle cell disease.[19]
Approximately half of classic
Sickle cell crisis
The terms "sickle cell crisis" or "sickling crisis" may be used to describe several independent acute conditions occurring in patients with SCD, which results in anaemia and crises that could be of many types, including the vaso-occlusive crisis, aplastic crisis, splenic sequestration crisis, haemolytic crisis, and others. The early symptoms[20] are a yellowish colour of skin or whites of the eyes that appears when a large number of red cells undergo hemolysis. Most episodes of sickle cell crises last between five and seven days.[21] "Although infection, dehydration, and acidosis (all of which favor sickling) can act as triggers, in most instances, no predisposing cause is identified."[22]
Vaso-occlusive crisis
The vaso-occlusive crisis is caused by sickle-shaped red blood cells that obstruct capillaries and restrict blood flow to an organ, resulting in
Splenic sequestration crisis
The
Splenic sequestration crises are acute, painful enlargements of the spleen, caused by intrasplenic trapping of red cells and resulting in a precipitous fall in haemoglobin levels with the potential for hypovolemic shock. Sequestration crises are considered an emergency. If not treated, patients may die within 1–2 hours due to circulatory failure. Management is supportive, sometimes with blood transfusion. These crises are transient; they continue for 3–4 hours and may last for one day.[28]
Acute chest syndrome
Acute chest syndrome is defined by at least two of these signs or symptoms: chest pain, fever, pulmonary infiltrate or focal abnormality, respiratory symptoms, or hypoxemia.[24] It is the second-most common complication and it accounts for about 25% of deaths in patients with SCD. Most cases present with vaso-occlusive crises, and then develop acute chest syndrome.[29][30] Nevertheless, about 80% of people have vaso-occlusive crises during acute chest syndrome.[citation needed]
Aplastic crisis
Haemolytic crisis
Management is supportive, sometimes with blood transfusions.[24]
Other
One of the earliest clinical manifestations is
Complications
Sickle cell anaemia can lead to various complications, including:
- Increased risk of severe bacterial infections is due to loss of functioning spleen tissue (and comparable to the risk of infections after having the spleen removed surgically). These infections are typically caused by encapsulated organisms such as Streptococcus pneumoniae and Haemophilus influenzae. Daily penicillin prophylaxis is the most commonly used treatment during childhood, with some haematologists continuing treatment indefinitely. Patients benefit today from routine vaccination for S. pneumoniae.[40]
- Stroke, which can result from a progressive narrowing of blood vessels, prevents oxygen from reaching the brain. Cerebral infarction occurs in children and cerebral haemorrhage in adults.[citation needed]
- Silent stroke causes no immediate symptoms, but is associated with damage to the brain. Silent stroke is probably five times as common as symptomatic stroke. About 10–15% of children with SCD have strokes, with silent strokes predominating in the younger patients.[41][42]
- haemolysis.[43]
- Avascular necrosis (aseptic bone necrosis) of the hip and other major joints may occur as a result of ischaemia.[44]
- Decreased hyposplenism (malfunctioning of the spleen)[45]
- Priapism and infarction of the penis[46]
- Osteomyelitis (bacterial bone infection), the most common cause of osteomyelitis in SCD is Salmonella (especially the atypical serotypes Salmonella typhimurium, Salmonella enteritidis, Salmonella choleraesuis, and Salmonella paratyphi B), followed by Staphylococcus aureus and Gram-negative enteric bacilli perhaps because intravascular sickling of the bowel leads to patchy ischaemic infarction.[47]
- Acute papillary necrosis in the kidneys[citation needed]
- Leg ulcers[48]
- In eyes, background retinopathy, proliferative retinopathy, vitreous haemorrhages, and retinal detachments can result in blindness.[49] Regular annual eye checks are recommended.
- During pregnancy, intrauterine growth restriction, spontaneous abortion, and pre-eclampsia
- Chronic pain: Even in the absence of acute vaso-occlusive pain, many patients have unreported chronic pain.[50]
- Pulmonary hypertension (increased pressure on the pulmonary artery) can lead to strain on the right ventricle and a risk of heart failure; typical symptoms are shortness of breath, decreased exercise tolerance, and episodes of syncope.[51] 21% of children and 30% of adults have evidence of pulmonary hypertension when tested; this is associated with reduced walking distance and increased mortality.[52]
- arrhythmias.[55]
- Chronic kidney failure due to sickle-cell nephropathy manifests itself with hypertension, protein loss in the urine, loss of red blood cells in urine and worsened anaemia. If it progresses to end-stage kidney failure, it carries a poor prognosis.[56]
Genetics


Normally, humans have
Sickle cell disease has an
Sickle cell gene mutation probably arose spontaneously in different geographic areas,[61] as suggested by restriction endonuclease analysis. These variants are known as Cameroon, Senegal, Benin, Bantu, and Saudi-Asian. Their clinical importance is because some are associated with higher HbF levels, e.g., Senegal and Saudi-Asian variants, and tend to have milder disease.[62]
The gene defect is a single
In people
The
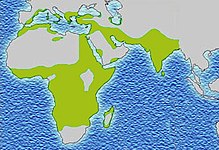
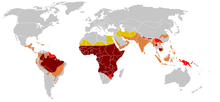
Due to the adaptive advantage of the heterozygote, the disease is still prevalent, especially among people with recent ancestry in malaria-stricken areas, such as
The malaria parasite has a complex lifecycle and spends part of it in red blood cells. In a carrier, the presence of the malaria parasite causes the red blood cells with defective haemoglobin to rupture prematurely, making the Plasmodium parasite unable to reproduce. Further, the polymerization of Hb affects the ability of the parasite to digest Hb in the first place. Therefore, in areas where malaria is a problem, people's chances of survival actually increase if they carry sickle cell traits (selection for the heterozygote).[citation needed]
In the United States, with no endemic malaria, the prevalence of sickle cell anaemia among people of African ancestry is lower (about 0.25%) than among people in West Africa (about 4.0%) and is falling. Without endemic malaria, the sickle cell mutation is purely disadvantageous and tends to decline in the affected population by natural selection, and now artificially through prenatal genetic screening. However, the African American community is descended from several West or Central African and non-African ethnic groups including American slaves. Thus, a degree of genetic dilution via crossbreeding with non-African people and high health-selective pressure through slavery (especially the slave trade and the frequently deadly Middle Passage) may be the most plausible explanations for the lower prevalence of sickle cell anaemia (and, possibly, other genetic diseases) among African Americans compared to West Africans. Another factor that limits the spread of sickle cell genes in North America is the relative absence of polygamy. In polygamous societies, affected males may father many children with multiple partners.[68]
Pathophysiology
The loss of red blood cell elasticity is central to the pathophysiology of sickle cell disease. Normal red blood cells are quite elastic and have a biconcave disc shape, which allows the cells to deform to pass through capillaries.
The actual anaemia of the illness is caused by haemolysis, the destruction of the red cells, because of their shape. Although the bone marrow attempts to compensate by creating new red cells, it does not match the rate of destruction.[70] Healthy red blood cells typically function for 90–120 days, but sickled cells only last 10–20 days.[71]
Diagnosis
In HbS, the
Sickling of the red blood cells, on a blood film, can be induced by the addition of sodium metabisulfite. The presence of sickle haemoglobin can also be demonstrated with the "sickle solubility test" (also called "sickledex").[73] A mixture of haemoglobin S (HbS) in a reducing solution (such as sodium dithionite) gives a turbid appearance, whereas normal Hb gives a clear solution.[74]
Abnormal haemoglobin forms can be detected on
An acute sickle cell crisis is often precipitated by infection. Therefore, a urinalysis to detect an occult urinary tract infection, and chest X-ray to look for occult pneumonia should be routinely performed.[76]
People who are known carriers of the disease or at risk of having a child with sickle cell anemia may undergo genetic counseling. Genetic counselors work with families to discuss the benefits, limitations, and logistics of genetic testing options as well as the potential impact of testing and test results on the individual.[77][78] During pregnancy, genetic testing can be done on either a blood sample from the fetus or a sample of amniotic fluid. During the first trimester of pregnancy, chorionic villus sampling (CVS) is also a technique used for SCD prenatal diagnosis.[79] Since taking a blood sample from a fetus has greater risks, the latter test is usually used. Neonatal screening sometimes referred to as newborn screening, provides not only a method of early detection for individuals with sickle cell disease but also allows for the identification of the groups of people who carry the sickle cell trait.[80] Genetic counselors can help individuals of colour and their families tackle the racial and ethnic disparities that exist in healthcare.[81]
In 2010, there was significant consideration and debate in the US surrounding comprehensive screening of athletes for SCD.[82][83][84][85] In 2012, the American Society of Hematology concluded that they do not support testing or disclosure of sickle cell trait status as a prerequisite for participation in athletic activities due to lack of scientific evidence, inconsistency with good medical practice, and inconsistency with public health ethics. They recommended universal interventions to reduce exertion-related injuries and deaths effective for all athletes irrespective of their sickle cell status.[86]
Management
Treatment involves a number of measures. While it has been historically recommended that people with sickle cell disease avoid exercise, regular exercise may benefit people.
Folic acid and penicillin
From birth to five years of age,
Malaria prevention

The protective effect of sickle cell trait does not apply to people with sickle cell disease; in fact, they are more vulnerable to malaria, since the most common cause of painful crises in malarial countries is infection with malaria. People with sickle cell disease living in malarial countries should receive lifelong medication for prevention.[94]
Vaso-occlusive crisis
Most people with sickle cell disease have intensely painful episodes called vaso-occlusive crises. However, the frequency, severity, and duration of these crises vary tremendously. Painful crises are treated symptomatically with
Extra fluids, administered either orally or intravenously, are a routine part of treatment of vaso-occlusive crises but the evidence about the most effective route, amount and type of fluid replacement remains uncertain.[96]
In 2019, Crizanlizumab, a monoclonal antibody target towards p-selectin was approved in the United States to reduce the frequency of vaso-occlusive crisis in those 16 years and older.[97]
Stroke prevention
Transcranial Doppler ultrasound (TCD) can detect children with sickle cell that have a high risk for stroke. The ultrasound test detects blood vessels partially obstructed by sickle cells by measuring the rate of blood into the brain, as blood flow velocity is inversely related to arterial diameter, and consequently, high blood-flow velocity is correlated with narrowing of the arteries.[98] In 2002, the National Institute of Health (NIH) issued a statement recommending that children with sickle cell get the Transcranial Doppler ultrasound screen annually, and in 2014, a panel of experts convened by the NIH issued guidelines reiterating the same recommendation. One review of medical records, by hematologist Dr. Julie Kanter at the University of Alabama at Birmingham, showed that on average only 48.4 per cent of children with sickle cell get the recommended ultrasound test.[99]
A 1994 NIH study showed that children at risk for strokes who received blood transfusions had an annual stroke rate of less than 1 per cent, whereas those children who did not receive blood transfusions had a 10 per cent stroke rate per year. (Also see 1998 study in the New England Journal of Medicine.[98]) In addition to ultrasounds and blood transfusions, the inexpensive generic drug hydroxyurea can reduce the risk of irreversible organ and brain damage. Guidelines from NIH published in 2014, state that all children and adolescents should take hydroxyurea, as should adults with serious complications or three or more pain crises in a year.[99]
Acute chest syndrome
Management is similar to vaso-occlusive crisis, with the addition of antibiotics (usually a quinolone or macrolide, since cell wall-deficient ["atypical"] bacteria are thought to contribute to the syndrome),
Should the pulmonary infiltrate worsen or the oxygen requirements increase, simple blood transfusion or exchange transfusion is indicated. The latter involves the exchange of a significant portion of the person's red cell mass for normal red cells, which decreases the level of haemoglobin S in the patient's blood. However, there is currently uncertain evidence about the possible benefits or harms of blood transfusion for acute chest syndrome in people with sickle cell disease.[102]
Hydroxyurea
It was the first approved drug for the treatment of sickle cell anaemia, and was shown to decrease the number and severity of attacks in 1995
Voxelotor was approved in the United States in 2019, to increase hemoglobin in people with SS disease.[107]
Blood transfusion
Bone marrow transplant
CRISPR-Cas9: Genome Editing for Sickle Cell Anemia
Researchers are investigating the use of CRISPR-Cas9, a highly specific and potent DNA thief, to correct the inherited error causing sickle cell anemia. Before integrating this technology into routine medical care, worries concerning its usage on living embryos and its effects on future generations still exist.Avascular necrosis[113]
Hematopoietic Stem Cell Transplantation (HSCT)
The treatment for sickle cell anemia implicitly involves hematopoietic stem cell transplantation (HSCT). This entails replacing the dysfunctional stem cells in the case with healthy bones from a well-matched donor. Finding the ideal client—typically a stock or someone almost matched—is essential to the process' success. However, there are still some drawbacks to hematopoietic stem cell transplantation (HSCT), such as the requirement for precise details to inhibit the susceptible system and problems from the new cells not taking hold. However, a successful HSCT can result in a long-term cure from sickle cell anemia for the patient.[114]
When treating avascular necrosis of the bone in people with sickle cell disease, the aim of treatment is to reduce or stop the pain and maintain
Psychological therapy
Psychological therapies such as patient education, cognitive therapy, behavioural therapy, and psychodynamic psychotherapy, that aim to complement current medical treatments, require further research to determine their effectiveness.[25]
Gene therapy
In 2023, both exagamglogene autotemcel and lovotibeglogene autotemcel were approved for the treatment of sickle cell disease.[10][115]
Prognosis
About 90% of people survive to age 20, and close to 50% survive beyond age 50.[116] In 2001, according to one study performed in Jamaica, the estimated mean survival for people was 53 years for men and 58 years for women with homozygous SCD.[117] The life expectancy in much of the developing world is unknown.[118] In 1975, about 7.3% of people with SCD died before their 23rd birthday; while in 1989, 2.6% of people with SCD died by the age of 20.[119]: 348
Epidemiology
The HbS gene can be found in every ethnic group.[120] The highest frequency of sickle cell disease is found in tropical regions, particularly West Africa and Central Africa, India, and the Middle East.[121] About 80% of sickle cell disease cases are believed to occur in Sub-Saharan Africa.[17] Migration of substantial populations from these high-prevalence areas to low-prevalence countries in Europe has dramatically increased in recent decades and in some European countries, sickle cell disease has now overtaken more familiar genetic conditions such as haemophilia and cystic fibrosis.[122] In 2015, it resulted in about 114,800 deaths.[8]
Sickle cell disease occurs more commonly among people whose ancestors lived in
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.[124]
Africa
Three-quarters of sickle cell cases occur in Africa. A recent WHO report estimated that around 2% of newborns in Nigeria were affected by sickle cell anaemia, giving a total of 150,000 affected children born every year in Nigeria alone. The carrier frequency ranges between 10 and 40% across equatorial Africa, decreasing to 1–2% on the North African coast and <1% in South Africa.[125] Studies in Africa show a significant decrease in infant mortality rate, ages 2–16 months, because of the sickle cell trait. This happened in areas of predominant malarial cases.[126]
Uganda has the fifth-highest sickle cell disease burden in Africa.[127] One study indicates that 20 000 babies per year are born with sickle cell disease with the sickle cell trait at 13.3% and with disease 0.7%.[128]
| Country | Population(2020) | Subregion | % of Prevalence | Prevalence | Incidence |
| Angola | 32,866,272 | Middle Africa | 0.09375 | 3,081,213 | 14,869 |
| Cameroon | 26,545,863 | Middle Africa | 0.117 | 3,105,866 | 11,826 |
| DR Congo | 89,561,403 | Middle Africa | 0.1163333333 | 10,418,977 | 65,536 |
| Ghana | 31,072,940 | Western Africa | 0.09375 | 2,913,088 | 9,588 |
| Guinea | 13,132,795 | Western Africa | 0.139375 | 1,830,383 | 8,907 |
| Niger | 24,206,644 | Western Africa | 0.07025 | 1,700,517 | 8,756 |
| Nigeria | 206,139,589 | Western Africa | 0.1286666667 | 26,523,294 | 150,000 |
| Tanzania | 59,734,218 | Eastern Africa | 0.0545 | 3,255,515 | 19,585 |
| Uganda | 45,741,007 | Eastern Africa | 0.07025 | 3,213,306 | 17,936 |
| Zambia | 18,383,955 | Eastern Africa | 0.082 | 1,507,484 | 9,958 |
| Algeria | 43,851,044 | Northern Africa | 0.029 | 1,271,680 | 6,624 |
| Benin | 12,123,200 | Western Africa | 0.1286666667 | 1,559,852 | 8,125 |
| Botswana | 2,351,627 | Southern Africa | 0.029 | 68,197 | 355 |
| Burkina Faso | 20,903,273 | Western Africa | 0.07025 | 1,468,455 | 7,649 |
| Burundi | 11,890,784 | Eastern Africa | 0.023 | 273,488 | 1,425 |
| Cabo Verde | 555,987 | Western Africa | 0.023 | 12,788 | 67 |
| Central African Republic | 4,829,767 | Middle Africa | 0.082 | 396,041 | 2,063 |
| Chad | 16,425,864 | Middle Africa | 0.0585 | 960,913 | 5,005 |
| Comoros | 869,601 | Eastern Africa | 0.023 | 20,001 | 104 |
| Congo | 5,518,087 | Middle Africa | 0.1615 | 891,171 | 4,642 |
| Côte d'Ivoire | 26,378,274 | Western Africa | 0.07025 | 1,853,074 | 9,652 |
| Djibouti | 988,000 | Eastern Africa | 0.023 | 22,724 | 118 |
| Egypt | 102,334,404 | Northern Africa | 0.029 | 2,967,698 | 15,458 |
| Equatorial Guinea | 1,402,985 | Middle Africa | 0.181 | 253,940 | 1,323 |
| Eritrea | 3,546,421 | Eastern Africa | 0.023 | 81,568 | 425 |
| Eswatini | 1,160,164 | Southern Africa | 0.023 | 26,684 | 139 |
| Ethiopia | 114,963,588 | Eastern Africa | 0.029 | 3,333,944 | 17,366 |
| Gabon | 2,225,734 | Middle Africa | 0.181 | 402,858 | 2,098 |
| Gambia | 2,416,668 | Western Africa | 0.082 | 198,167 | 1,032 |
| Guinea-Bissau | 1,968,001 | Western Africa | 0.035 | 68,880 | 359 |
| Kenya | 53,771,296 | Eastern Africa | 0.04675 | 2,513,808 | 13,094 |
| Lesotho | 2,142,249 | Southern Africa | 0.023 | 49,272 | 257 |
| Liberia | 5,057,681 | Western Africa | 0.07025 | 355,302 | 1,851 |
| Libya | 6,871,292 | Northern Africa | 0.029 | 199,267 | 1,038 |
| Madagascar | 27,691,018 | Eastern Africa | 0.04675 | 1,294,555 | 6,743 |
| Malawi | 19,129,952 | Eastern Africa | 0.035 | 669,548 | 3,488 |
| Mali | 20,250,833 | Western Africa | 0.082 | 1,660,568 | 8,650 |
| Mauritania | 4,649,658 | Western Africa | 0.04675 | 217,372 | 1,132 |
| Mauritius | 1,271,768 | Eastern Africa | 0.023 | 29,251 | 152 |
| Morocco | 36,910,560 | Northern Africa | 0.029 | 1,070,406 | 5,576 |
| Mozambique | 31,255,435 | Eastern Africa | 0.035 | 1,093,940 | 5,698 |
| Namibia | 2,540,905 | Southern Africa | 0.03883333333 | 98,672 | 514 |
| Rwanda | 12,952,218 | Eastern Africa | 0.035 | 453,328 | 2,361 |
| São Tomé and Príncipe | 219,159 | Middle Africa | 0.181 | 39,668 | 207 |
| Senegal | 16,743,927 | Western Africa | 0.07025 | 1,176,261 | 6,127 |
| Seychelles | 98,347 | Eastern Africa | 0.023 | 2,262 | 12 |
| Sierra Leone | 7,976,983 | Western Africa | 0.1615 | 1,288,283 | 6,711 |
| Somalia | 15,893,222 | Eastern Africa | 0.029 | 460,903 | 2,401 |
| South Africa | 59,308,690 | Southern Africa | 0.029 | 1,719,952 | 8,959 |
| South Sudan | 11,193,725 | Eastern Africa | 0.04675 | 523,307 | 2,726 |
| Sudan | 43,849,260 | Northern Africa | 0.03883333333 | 1,702,813 | 8,870 |
| Togo | 8,278,724 | Western Africa | 0.09375 | 776,130 | 4,043 |
| Tunisia | 11,818,619 | Northern Africa | 0.023 | 271,828 | 1,416 |
| Zimbabwe | 14,862,924 | Eastern Africa | 0.035 | 520,202 | 2,710 |
| Total | 1,338,826,604 | Africa | 91,868,664 | 495,726 |
United States
The number of people with the disease in the United States is about 100,000 (one in 3,300), mostly affecting Americans of sub-Saharan African descent.[129] In the United States, about one out of 365 African-American children and one in every 16,300 Hispanic-American children have sickle cell anaemia.[130] The life expectancy for men with SCD is approximately 42 years of age while women live approximately six years longer.[131] An additional 2 million are carriers of the sickle cell trait.[132] Most infants with SCD born in the United States are identified by routine neonatal screening. As of 2016 all 50 states include screening for sickle cell disease as part of their newborn screen.[133] The newborn's blood is sampled through a heel-prick and is sent to a lab for testing. The baby must have been eating for a minimum of 24 hours before the heel-prick test can be done. Some states also require a second blood test to be done when the baby is two weeks old to ensure the results.[134]
Sickle cell anemia is the most common genetic disorder among African Americans. Approximately 8% are
France

As a result of population growth in African-Caribbean regions of

Since 2000, neonatal screening of SCD has been performed at the national level for all newborns defined as being "at-risk" for SCD based on ethnic origin (defined as those born to parents originating from sub-Saharan Africa, North Africa, the Mediterranean area (South Italy, Greece, and Turkey), the Arabic peninsula, the French overseas islands, and the Indian subcontinent).[139]
United Kingdom
In the United Kingdom, between 12,000 and 15,000 people are thought to have sickle cell disease [140] with an estimated 250,000 carriers of the condition in England alone. As the number of carriers is only estimated, all newborn babies in the UK receive a routine blood test to screen for the condition.[141] Due to many adults in high-risk groups not knowing if they are carriers, pregnant women and both partners in a couple are offered screening so they can get counselling if they have the sickle cell trait.[142] In addition, blood donors from those in high-risk groups are also screened to confirm whether they are carriers and whether their blood filters properly.[143] Donors who are found to be carriers are then informed and their blood, while often used for those of the same ethnic group, is not used for those with sickle cell disease who require a blood transfusion.[144][unreliable medical source?]
West Asia
In Saudi Arabia, about 4.2% of the population carry the sickle cell trait and 0.26% have sickle cell disease. The highest prevalence is in the Eastern province, where approximately 17% of the population carry the gene and 1.2% have sickle cell disease.[145] In 2005, Saudi Arabia introduced a mandatory premarital test including HB electrophoresis, which aimed to decrease the incidence of SCD and thalassemia.[146]
In
India and Nepal
Sickle cell disease is common in some ethnic groups of central India,[149] where the prevalence has ranged from 9.4 to 22.2% in endemic areas of Madhya Pradesh, Rajasthan, and Chhattisgarh.[150] It is also endemic among Tharu people of Nepal and India; however, they have a sevenfold lower rate of malaria despite living in a malaria infested zone.[151]
Caribbean Islands
In Jamaica, 10% of the population carry the sickle cell gene, making it the most prevalent genetic disorder in the country.[152]
History
The first modern report of sickle cell disease may have been in 1846, where the autopsy of an executed runaway slave was discussed; the key finding was the absence of the spleen.[153][154] Reportedly, African slaves in the United States exhibited resistance to malaria, but were prone to leg ulcers.[154] The abnormal characteristics of the red blood cells, which later lent their name to the condition, was first described by Ernest E. Irons (1877–1959), intern to Chicago cardiologist and professor of medicine James B. Herrick (1861–1954), in 1910. Irons saw "peculiar elongated and sickle-shaped" cells in the blood of a man named Walter Clement Noel, a 20-year-old first-year dental student from Grenada. Noel had been admitted to the Chicago Presbyterian Hospital in December 1904 with anaemia.[14][155] Noel was readmitted several times over the next three years for "muscular rheumatism" and "bilious attacks" but completed his studies and returned to the capital of Grenada (St. George's) to practice dentistry. He died of pneumonia in 1916 and is buried in the Catholic cemetery at Sauteurs in the north of Grenada.[14][15] Shortly after the report by Herrick, another case appeared in the Virginia Medical Semi-Monthly with the same title, "Peculiar Elongated and Sickle-Shaped Red Blood Corpuscles in a Case of Severe Anemia."[156] This article is based on a patient admitted to the University of Virginia Hospital on 15 November 1910.[157] In the later description by Verne Mason in 1922, the name "sickle cell anemia" is first used.[15][158] Childhood problems related to sickle cells disease were not reported until the 1930s, despite the fact that this cannot have been uncommon in African-American populations.[154]
Memphis physician Lemuel Diggs, a prolific researcher into sickle cell disease, first introduced the distinction between sickle cell disease and trait in 1933, although until 1949, the genetic characteristics had not been elucidated by James V. Neel and E.A. Beet.[15] 1949 was the year when Linus Pauling described the unusual chemical behaviour of haemoglobin S, and attributed this to an abnormality in the molecule itself.[15][159] The molecular change in HbS was described in 1956 by Vernon Ingram.[160] The late 1940s and early 1950s saw further understanding in the link between malaria and sickle cell disease. In 1954, the introduction of haemoglobin electrophoresis allowed the discovery of particular subtypes, such as HbSC disease.[15]
Large-scale natural history studies and further intervention studies were introduced in the 1970s and 1980s, leading to widespread use of prophylaxis against pneumococcal infections amongst other interventions. Bill Cosby's Emmy-winning 1972 TV movie, To All My Friends on Shore, depicted the story of the parents of a child with sickle cell disease.[161] The 1990s had the development of hydroxycarbamide, and reports of cure through bone marrow transplantation appeared in 2007.[15]
Some old texts refer to it as drepanocytosis.[162]
Society and culture
United States
Sickle cell disease is frequently contested as a disability.[163] Effective 15 September 2017, the U.S. Social Security Administration issued a Policy Interpretation Ruling providing background information on sickle cell disease and a description of how Social Security evaluates the disease during its adjudication process for disability claims.[164][165]
In the US, there are stigmas surrounding SCD that discourage people with SCD from receiving necessary care. These stigmas mainly affect people of African American and Latin American ancestries, according to the National Heart, Lung, and Blood Institute.[166] People with SCD experience the impact of stigmas of the disease on multiple aspects of life including social and psychological well-being. Studies have shown that those with SCD frequently feel as though they must keep their diagnosis a secret to avoid discrimination in the workplace and also among peers in relationships.[167] In the 1960s, the US government supported initiatives for workplace screening for genetic diseases in an attempt to be protective towards people with SCD. By having this screening, it was intended that employees would not be placed in environments that could potentially be harmful and trigger SCD.[168]
Uganda
Uganda has the 5th highest sickle cell disease (SCD) burden in the world.[169] In Uganda, social stigma exists for those with sickle cell disease because of the lack of general knowledge of the disease. The general gap in knowledge surrounding sickle cell disease is noted among adolescents and young adults due to the culturally sanctioned secrecy about the disease.[169] While most people have heard generally about the disease, a large portion of the population is relatively misinformed about how SCD is diagnosed or inherited. Those who are informed about the disease learned about it from family or friends and not from health professionals. Failure to provide the public with information about sickle cell disease results in a population with a poor understanding of the causes of the disease, symptoms, and prevention techniques.[170] The differences, physically and socially, that arise in those with sickle cell disease, such as jaundice, stunted physical growth, and delayed sexual maturity, can also lead them to become targets of bullying, rejection, and stigma.[169]
Rate of sickle cell disease in Uganda
The data compiled on sickle cell disease in Uganda has not been updated since the early 1970s. The deficiency of data is due to a lack of government research funds, even though Ugandans die daily from SCD.[171] Data shows that the trait frequency of sickle cell disease is 20% of the population in Uganda.[171] This means that 66 million people are at risk of having a child who has sickle cell disease.[171] It is also estimated that about 25,000 Ugandans are born each year with SCD and 80% of those people don't live past five years old.[171] SCD also contributes 25% to the child mortality rate in Uganda.[171] The Bamba people of Uganda, located in the southwest of the country, carry 45% of the gene which is the highest trait frequency recorded in the world.[171] The Sickle Cell Clinic in Mulago is only one sickle cell disease clinic in the country and on average sees 200 patients a day.[171]
Misconceptions about sickle cell disease
The stigma around the disease is particularly bad in regions of the country that are not as affected. For example, Eastern Ugandans tend to be more knowledgeable of the disease than Western Ugandans, who are more likely to believe that sickle cell disease resulted as a punishment from God or witchcraft.[172] Other misconceptions about SCD include the belief that it is caused by environmental factors but, in reality, SCD is a genetic disease.[173] There have been efforts throughout Uganda to address the social misconceptions about the disease. In 2013, the Uganda Sickle Cell Rescue Foundation was established to spread awareness of sickle cell disease and combat the social stigma attached to the disease.[174] In addition to this organization's efforts, there is a need for the inclusion of sickle cell disease education in preexisting community health education programs in order to reduce the stigmatization of sickle cell disease in Uganda.[170]
Social isolation of people with sickle cell disease
The deeply rooted stigma of SCD from society causes families to often hide their family members' sick status for fear of being labeled, cursed, or left out of social events.[175] Sometimes in Uganda, when it is confirmed that a family member has sickle cell disease, intimate relationships with all members of the family are avoided.[175] The stigmatization and social isolation people with sickle cell disease tend to experience is often the consequence of popular misconceptions that people with SCD should not socialize with those free from the disease. This mentality robs people with SCD of the right to freely participate in community activities like everyone else[169] SCD-related stigma and social isolation in schools, especially, can make a life for young people living with sickle cell disease extremely difficult.[169] For school-aged children living with SCD, the stigma they face can lead to peer rejection.[169] Peer rejection involves the exclusion from social groups or gatherings. It often leads the excluded individual to experience emotional distress and may result in their academic underperformance, avoidance of school, and occupational failure later in life.[169] This social isolation is also likely to negatively impact people with SCD's self-esteem and overall quality of life.[169]
Mothers of children with sickle cell disease tend to receive disproportionate amounts of stigma from their peers and family members. These women will often be blamed for their child's diagnosis of SCD, especially if SCD is not present in earlier generations, due to the suspicion that the child's poor health may have been caused by the mother's failure to implement preventative health measures or promote a healthy environment for her child to thrive.[173] The reliance on theories related to environmental factors to place blame on the mother reflects many Ugandan's poor knowledge of how the disease is acquired as it is determined by genetics, not environment.[173] Mothers of children with sickle cell disease are also often left with very limited resources to safeguard their futures against the stigma of having SCD.[173] This lack of access to resources results from their subordinating roles within familial structures as well as the class disparities that hinder many mothers' ability to satisfy additional childcare costs and responsibilities.[173]
Women living with SCD who become pregnant often face extreme discrimination and discouragement in Uganda. These women are frequently branded by their peers as irresponsible for having a baby while living with sickle cell disease or even engaging in sex while living with SCD.[citation needed] The criticism and judgement these women receive, not only from healthcare professionals but also from their families, often leaves them feeling alone, depressed, anxious, ashamed, and with very little social support.[citation needed] Most pregnant women with SCD also go on to be single mothers as it is common for them to be left by their male partners who claim they were unaware of their partner's SCD status.[citation needed] Not only does the abandonment experienced by these women cause emotional distress for them, but this low level of parental support can be linked to depressive symptoms and overall lower quality of life for the child once they are born.[176]
United Kingdom
In 2021 many patients were found to be afraid to visit hospitals, such was the level of ignorance among staff, so purchased pain relief to treat themselves outside the NHS.[
Research
Umbilical cord blood transplant
While
Gene therapy
Diseases such as sickle cell disease for which a person's normal phenotype or cell function may be restored in cells that have the disease by a normal copy of the gene that is mutated, may be a good candidate for gene therapy treatment. The risks and benefits related to gene therapy for sickle cell disease are not known.[182]
In 2001, sickle cell disease reportedly had been successfully treated in mice using gene therapy.[183][184] The researchers used a viral vector to make the mice—which have essentially the same defect that causes human sickle cell disease—express production of fetal haemoglobin (HbF), which an individual normally ceases to produce shortly after birth. In humans, using hydroxyurea to stimulate the production of HbF has been known to temporarily alleviate sickle cell disease symptoms. The researchers demonstrated that this gene therapy method is a more permanent way to increase therapeutic HbF production.[185]
Gene editing platforms like CRISPR/Cas9 have been used to correct the disease-causing mutation in hematopoietic stem cells taken from a person with the condition.
In 2017, twelve clinical trials were focusing on gene therapy to treat sickle cell anemia. Of those 12 trials, four of them replaced the mutated HBB gene with a healthy one. Three trials used Mozobil, a medication used to treat types of cancer, to determine whether the increase of stem cells can be used for gene therapy. One trial focused on analyzing bone marrow samples from patients with sickle cell anemia. Another trial experimented with using umbilical cord blood from babies both with and without sickle cell anemia to develop gene therapy.[194]
In November 2023, a gene treatment using the CRISPR gene editing tool was approved by UK regulators for the treatment of sickle cell disease and also for the blood disorder transfusion-dependent beta thalassemia.[11][195]
Hematopoietic stem cell transplantation
There is no strong medical evidence to determine the risks and potential benefits related to treating people with sickle cell disease with hematopoietic stem cell transplantations.[196]
Notes
- ^ Historic numbering put this glutamic acid residue at position 6 due to skipping the methionine (M/Met) start codon in protein amino acid position numbering. Current nomenclature calls for counting the methionine as the first amino acid, resulting in the glutamic acid residue falling at position 7. Many references still refer to position 6 and both should likely be referenced for clarity.
References
- ^ a b c d e "What Are the Signs and Symptoms of Sickle Cell Disease?". National Heart, Lung, and Blood Institute. 12 June 2015. Archived from the original on 9 March 2016. Retrieved 8 March 2016.
- ^ a b c d e f g h i j "What Is Sickle Cell Disease?". National Heart, Lung, and Blood Institute. 12 June 2015. Archived from the original on 6 March 2016. Retrieved 8 March 2016.
- ^ a b c "What Causes Sickle Cell Disease?". National Heart, Lung, and Blood Institute. 12 June 2015. Archived from the original on 24 March 2016. Retrieved 8 March 2016.
- ^ a b c "How Is Sickle Cell Disease Diagnosed?". National Heart, Lung, and Blood Institute. 12 June 2015. Archived from the original on 9 March 2016. Retrieved 8 March 2016.
- ^ a b c d "Sickle-cell disease and other haemoglobin disorders Fact sheet N°308". January 2011. Archived from the original on 9 March 2016. Retrieved 8 March 2016.
- ^ a b c d "How Is Sickle Cell Disease Treated?". National Heart, Lung, and Blood Institute. 12 June 2015. Archived from the original on 9 March 2016. Retrieved 8 March 2016.
- ^ PMID 27733282.
- ^ PMID 27733281.
- ^ "Learning About Sickle Cell Disease". National Human Genome Research Institute. 9 May 2016. Archived from the original on 4 January 2017. Retrieved 23 January 2017.
- ^ a b "FDA Approves First Gene Therapies to Treat Patients with Sickle Cell Disease". U.S. Food and Drug Administration (FDA). 8 December 2023. Archived from the original on 8 December 2023. Retrieved 8 December 2023.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ S2CID 265264939.
- PMID 26063472.
- ^ CDC (2 May 2022). "Data & Statistics on Sickle Cell Disease | CDC". Centers for Disease Control and Prevention. Retrieved 3 April 2024.
- ^ PMID 2642320.
- ^ PMID 20955412.
- ^ a b "Sickle cell disease: MedlinePlus Genetics". medlineplus.gov. Retrieved 22 October 2022.
- ^ S2CID 29909566.
- ^ S2CID 37681044.
- ^ ISSN 0006-4971.
- ^ "Sickle Cell Disease - Symptoms | NHLBI, NIH". www.nhlbi.nih.gov. 30 August 2023. Retrieved 22 March 2024.
- ^ "BestBets: How long should an average sickle cell crisis last?". Archived from the original on 17 June 2010. Retrieved 27 November 2010.
- ^ Kumar V, Abbas AK, Fausto N, Aster J (28 May 2009). Robbins and Cotran Pathologic Basis of Disease (Professional Edition: Expert Consult – Online (Robbins Pathology) ed.). Elsevier Health. pp. Kindle Locations 33498–33499.
- PMID 23293942.
- ^ PMID 22164362.
- ^ PMID 25966336.
- from the original on 27 May 2016.
- S2CID 19977178.
- S2CID 2547649.
- PMID 18174543.
- S2CID 40320701.
- ^ Kumar V, Abbas AK, Fausto N, Aster J (28 May 2009). Robbins and Cotran Pathologic Basis of Disease (Professional Edition: Expert Consult – Online (Robbins Pathology) ed.). Elsevier Health. pp. Kindle Location 33329.
- PMID 21585562.
- PMID 22264009.
- PMID 18991647.
- PMID 3978504.
- from the original on 23 September 2016.
- S2CID 206896811.
- PMID 28722902. Retrieved 21 March 2021.
- ISBN 978-0-7216-2921-6.
- from the original on 4 March 2016.
- PMID 11722977.
- PMID 17998439.
- ^ "Cholelithiasis". The Lecturio Medical Concept Library. Retrieved 25 August 2021.
- ^ PMID 31803937.
- PMID 7430367.
- PMID 21421100.
- S2CID 908481.
- ^ Rudge FW (1991). "Hyperbaric oxygen therapy in the treatment of sickle cell leg ulcers". J. Hyperbaric Med. 6 (1): 1–4. Archived from the original on 15 April 2013. Retrieved 23 March 2011.
{{cite journal}}: CS1 maint: unfit URL (link) - PMID 20452638.
- S2CID 34924760.
- PMID 24951762.
- S2CID 23920740.
- PMID 26897687.
- PMID 28507082.
- S2CID 24444332.
- PMID 1892333.
- PMID 23209159.
- ^ "Sickle Cell Disease". NORD (National Organization for Rare Disorders). Retrieved 10 June 2019.
- ^ "sickle cell disease". Genetics Home Reference. Archived from the original on 15 May 2016. Retrieved 7 May 2016.
- ^ "Inheritance of Sickle Cell Anaemia". Sickle Cell Society. Archived from the original on 8 January 2024. Retrieved 8 January 2024.
- ^ "Sickle-Cell Anemia: Haplotype | Learn Science at Scitable". www.nature.com. Retrieved 12 October 2023.
- S2CID 27341091.
- ^ Clancy S (2008). "Genetic mutation". Nature Education. 1 (1): 187.
- PMID 22089617.
- PMID 19442502.
- PMID 16001361.
- PMID 17313664.
- S2CID 41719342.
- )
- ^ "How Does Sickle Cell Cause Disease?". Archived from the original on 23 September 2010. Retrieved 27 November 2010.
- ^ "Sickle Cell Anemia: eMedicine Emergency Medicine". Archived from the original on 4 December 2010. Retrieved 27 November 2010.
- ISBN 978-953-51-0684-5
- ISBN 978-1-119-28265-5.
- ISBN 978-0-323-41315-2.
- from the original on 20 March 2008.
- ^ "BestBets: Does routine urinalysis and chest radiography detect occult bacterial infection in sickle cell patients presenting to the accident and emergency department with painful crisis?". Archived from the original on 17 June 2010. Retrieved 27 November 2010.
- ^ "National Society of Genetic Counselors : About Genetic Counselors". www.nsgc.org. Retrieved 24 February 2021.
- ^ "ABGC – Information for Certified Genetic Counselors | ABGC". www.abgc.net. Archived from the original on 19 April 2021. Retrieved 23 February 2021.
- ^ Colah, R. B., Gorakshakar, A. C., & Nadkarni, A. H. (2011). Invasive & non-invasive approaches for prenatal diagnosis of haemoglobinopathies: experiences from India. The Indian Journal of Medical Research, 134(4), 552–560.
- ^ Lee, C., Davies, S.,& Dezatoux, C. (2000). Neonatal Screening for sickle cell disease. The Cochrane Collaboration. John Wiley & Sons, Ltd.
- ^ Stallings E (27 July 2019). "Genetic Counselors Of Color Tackle Racial, Ethnic Disparities In Health Care". NPR. Retrieved 23 February 2021.
- PMID 22307997.
- PMID 20825310.
- S2CID 11404187.
- S2CID 15889144.
- ^ "Statement on Screening for Sickle Cell Trait and Athletic Participation". American Society of Hematology. Archived from the original on 26 January 2021. Retrieved 24 February 2021.
- S2CID 24464344.
- ^ "Keeping Well with Sickle Cell Disease - Brent Sickle Cell & Thalassaemia Centre". www.sickle-thal.nwlh.nhs.uk. Archived from the original on 3 October 2019. Retrieved 4 October 2019.
- ^ "Nutrition for the Child with Sickle Cell Anemia". www.eatright.org. Archived from the original on 19 June 2020. Retrieved 5 October 2019.
- PMID 32462740.
- ^ Office of the Commissioner (7 July 2017). "Press Announcements – FDA approves new treatment for sickle cell disease". www.fda.gov. Archived from the original on 10 July 2017. Retrieved 10 July 2017.
- ^ "Evidence-Based Management of Sickle Cell Disease" (PDF). 2014. Retrieved 16 November 2017.
twice-daily prophylactic penicillin beginning in early infancy and continuing through at least age 5
- PMID 29546732.
- PMID 31681984.
- S2CID 203667575.
- PMID 28759112.
- ^ "FDA approves crizanlizumab-tmca for sickle cell disease". U.S. Food and Drug Administration. 15 November 2019. Retrieved 12 December 2023.
- ^ PMID 9647873.
- ^ a b Kolata G (24 May 2021). "These Sisters With Sickle Cell Had Devastating, and Preventable, Strokes". The New York Times.
- ISBN 978-0-8151-1371-3.
- PMID 31531967.
- PMID 31942751.
- ^ PMID 36047926.
- PMID 7715639.
- PMID 12672732.
- S2CID 351061.
- ^ Center for Drug Evaluation and Research (25 November 2019). "FDA approves voxelotor for sickle cell disease". FDA. Retrieved 9 December 2019.
- S2CID 44562296.
- PMID 21117059.
- S2CID 24316310.
- S2CID 25256772.
- ^ Kaiser J (5 December 2020). "CRISPR and another genetic strategy fix cell defects in two common blood disorders". ScienceMag.org. Science. Retrieved 7 December 2020.
... teams report that two strategies for directly fixing malfunctioning blood cells have dramatically improved the health of a handful of people with these genetic diseases.
- ^ Dudi A (17 November 2023). "Unravelito the Quest: Is There a Cure for Sickle Cell Anemia? Introduction to Sickle Cell Anemia". Health aimed.
- ^ Dudi A (17 November 2023). "Unravelito the Quest: Is There a Cure for Sickle Cell Anemia? Introduction to Sickle Cell Anemia". Health aimed. Retrieved 17 November 2023.
- ^ "MHRA authorises world-first gene therapy that aims to cure sickle-cell disease and transfusion-dependent β-thalassemia". Medicines and Healthcare products Regulatory Agency (MHRA) (Press release). 16 November 2023. Archived from the original on 25 November 2023. Retrieved 8 December 2023.
- ^ Kumar V, Abbas AK, Fausto N, Aster J (28 May 2009). Robbins and Cotran Pathologic Basis of Disease (Professional Edition: Expert Consult – Online (Robbins Pathology) ed.). Elsevier Health. pp. Kindle Locations 33530–33531.
- S2CID 37012133.
- ISBN 9783319067131. Retrieved 8 May 2016.
- PMID 20425797.
- ISBN 978-0-309-66960-3.)
{{cite book}}: CS1 maint: multiple names: authors list (link - PMID 11545326.
- PMID 17606434.
- PMID 19729847.
- ^ United States National Library of Medicine. "Sickle cell disease: MedlinePlus Genetics".
- ^ WHO. "Sickle-cell anaemia – Report by the Secretariat" (PDF). Archived from the original (PDF) on 4 January 2011. Retrieved 27 November 2010.
- S2CID 37952036.
- PMID 29703184.
- PMID 26833239.
- ^ National Heart, Lung and Blood Institute. "Sickle cell anemia, key points". Archived from the original on 2 December 2010. Retrieved 27 November 2010.
- ^ "Data & Statistics on Sickle Cell Disease | CDC". Centers for Disease Control and Prevention. 31 August 2016. Retrieved 13 December 2019.
- ^ "September is Sickle Cell Awareness Month". CDC. Archived from the original on 27 September 2010. Retrieved 6 February 2011.
- ^ "Sickle Cell Trait". American Society of Hematology. 8 September 2017. Retrieved 13 December 2019.
- ^ "Disorder Name: Sickle Cell Disease". New Born Screening. Archived from the original on 28 September 2016. Retrieved 11 October 2016.
- ^ "default – Stanford Children's Health". www.stanfordchildrens.org. Retrieved 14 March 2020.
- S2CID 7644129.
- ^ "Sickle Cell Patients Endure Discrimination, Poor Care And Shortened Lives". NPR.org. 4 November 2017. Retrieved 12 November 2017.
- PMID 36378213.
- PMID 15558961.
- S2CID 22391674.
- ^ "Inheriting sickle cell anaemia – Live Well – NHS Choices". www.nhs.uk. 23 October 2017. Archived from the original on 2 December 2014.
- ^ "Sickle cell anaemia – NHS Choices". www.nhs.uk. 23 October 2017. Archived from the original on 13 December 2011.
- ^ "Who is offered screening and when?". screening.nhs.uk. Archived from the original on 31 December 2014.
- ^ "Give Blood – Resources – Sickle Cell and Blood Donation". Give Blood. Archived from the original on 31 December 2014.
- ^ "Why is Blood from Afro-Caribbean Donors Special?". sicklecellsociety.org. Archived from the original on 30 December 2014.
- PMID 21623060.
- PMID 21623050.
- ^ Al Arrayed S (1995). "Features of sickle-cell disease in Bahrain". Eastern Mediterranean Health Journal. 1 (1). Archived from the original on 8 October 2016.
- PMID 20622345.
- ^ "Sickle Cell Anemia". American Society of Hematology. 16 December 2014. Archived from the original on 25 June 2017. Retrieved 1 May 2017.
- .
- ^ "Life with sickle cell – Nation – Nepali Times". Archived from the original on 24 June 2015.
- PMID 22039456.
- ^ Lebby R (1846). "Case of absence of the spleen". Southern J of Med Pharmacol. 1: 481–3.
- ^ PMID 22923496.
- PMID 11501714.
- ^ Washburn RE (1911). "Peculiar elongated and sickle-shaped red blood corpuscles in a case of severe anemia". The Virginia Medical Semi-Monthly. 15 (21): 490–493.
- ^ "UVa Hospital Celebrating 100 Years". University of Virginia. Archived from the original on 31 January 2015. Retrieved 28 January 2015.
- PMID 3900438.
- S2CID 31674765.
- S2CID 4167855.
- ^ "Foster, Gloria". Facts On File History Database. Archived from the original on 5 March 2016. Retrieved 25 February 2015.
- PMID 7460122.
- PMID 37315205.
- ^ "Social Security Ruling: SSR 2017-3p". U.S. Social Security Administration. Retrieved 15 January 2018.
- ^ "Federal Register, Volume 82 Issue 178 (Friday, September 15, 2017)". U.S. Government Publishing Office (GPO). Retrieved 15 January 2018.
- ^ "Sickle Cell Disease | National Heart, Lung, and Blood Institute (NHLBI)". www.nhlbi.nih.gov. Retrieved 4 July 2020.
- PMID 29652215.
- OCLC 192050177.
- ^ PMID 31632168.
- ^ PMID 29703184.
- ^ a b c d e f g "Sickle Cell Association of Uganda". Sickle Cell Association of Uganda. Retrieved 7 April 2021.
- PMID 21644415.
- ^ PMID 21797722.
- ^ "Our Vision and Mission – Uganda Sickle Cell Rescue Foundation". 13 May 2017. Retrieved 6 April 2021.
- ^ a b "Background – Uganda Sickle Cell Rescue Foundation". 13 May 2017. Retrieved 6 April 2021.
- PMID 25880537.
- ^ "London Eye: Shouldn't need an improvement programme". Health Service Journal. 27 July 2022. Retrieved 28 September 2022.
- ^ "Better protection and support for people with sickle cell disease". The Voice. October 2022. pp. 16–17. Retrieved 7 October 2022.
- ^ Rylatt A (7 October 2022). "No-one is Listening" (PDF).
- ^ "NHS launches lifesaving sickle cell campaign". 7 October 2022.
- ^ PMID 28641096.
- PMID 33251574.
- S2CID 25607771.
- ^ Wilson JF (18 March 2002). "Murine Gene Therapy Corrects Symptoms of Sickle Cell Disease". The Scientist – Magazine of the Life Sciences. Retrieved 17 December 2014.
- ^ St. Jude Children's Research Hospital (4 December 2008). "Gene Therapy Corrects Sickle Cell Disease In Laboratory Study". ScienceDaily. Archived from the original on 13 December 2014. Retrieved 17 December 2014.
- ^ Clinical trial number NCT02247843 for "Stem Cell Gene Therapy for Sickle Cell Disease" at ClinicalTrials.gov
- ^ Clinical trial number NCT00012545 for "Collection and Storage of Umbilical Cord Stem Cells for Treatment of Sickle Cell Disease" at ClinicalTrials.gov
- S2CID 5128871.
- ^ Kolata G (27 January 2019). "These Patients Had Sickle-Cell Disease. Experimental Therapies Might Have Cured Them". The New York Times. Retrieved 28 January 2019.
- PMID 27820943.
- ^ "In A 1st, Doctors In U.S. Use CRISPR Tool To Treat Patient With Genetic Disorder". NPR. Retrieved 31 July 2019.
- S2CID 213060203.
- PMID 30581191.
- ^ Walker M (15 January 2018). "Gene Therapy". Sickle Cell Disease News. Retrieved 14 March 2020.
- ^ "MHRA authorises world-first gene therapy that aims to cure sickle-cell disease and transfusion-dependent β-thalassemia". Medicines and Healthcare products Regulatory Agency (MHRA) (Press release). 16 November 2023. Archived from the original on 25 November 2023. Retrieved 8 December 2023.
- PMID 32617981.
Further reading
- Brown RT, ed. (2006). Comprehensive handbook of childhood cancer and sickle cell disease: a biopsychosocial approach. Oxford University Press. ISBN 978-0-19-516985-0.
- Hill SA (2003). Managing Sickle Cell Disease in Low-Income Families. Temple University Press. ISBN 978-1-59213-195-2.
- Serjeant GR, Serjeant BE (2001). Sickle Cell Disease. Oxford University Press. ISBN 978-0-19-263036-0.
- Tapper M (1999). In the blood: sickle cell anemia and the politics of race. University of Pennsylvania Press. ISBN 978-0-8122-3471-8.
External links
- Sickle cell at Curlie
