Silicosis
This article needs additional citations for verification. (February 2018) |
| Silicosis | |
|---|---|
| Other names | Miner's phthisis, Grinder's asthma, Potter's rot coal workers' pneumoconiosis |
Silicosis is a form of
Silicosis resulted in at least 43,000 deaths globally in 2013, down from at least 50,000 deaths in 1990.[6]
The name silicosis (from the Latin silex, or flint) was originally used in 1870 by Achille Visconti (1836–1911),
With industrialization, as opposed to hand tools, came increased production of dust. The
In the early 21st century, an epidemic of silicosis was caused by the unsafe manufacturing of engineered stone countertops containing quartz, which became popular.[12]
Signs and symptoms
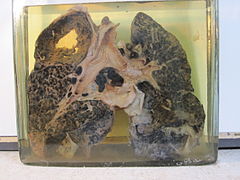
Because chronic silicosis is slow to develop, signs and symptoms may not appear until years after exposure.[13] Signs and symptoms include:
- Dyspnea(shortness of breath) exacerbated by exertion
- Cough, often persistent and sometimes severe
- Fatigue
- Tachypnea (rapid breathing) which is often labored
- Loss of appetite and weight loss
- Chest pain
- Fever
- Gradual darkening of skin (blue skin)
- Gradual dark shallow rifts in nails eventually leading to cracks as protein fibers within nail beds are destroyed
In advanced cases, the following may also occur:
- Cyanosis, pallor along upper parts of body (blue skin)
- Cor pulmonale (right ventricleheart disease)
- Respiratory insufficiency
Patients with silicosis are particularly susceptible to
Pulmonary complications of silicosis also include chronic bronchitis and airflow limitation (indistinguishable from that caused by smoking), non-tuberculous Mycobacterium infection, fungal lung infection,
In 1996, the
Pathophysiology
When small silica dust particles are inhaled, they can embed themselves deeply into the tiny alveolar sacs and ducts in the lungs, where oxygen and carbon dioxide gases are exchanged. There, the lungs cannot clear out the dust by mucus or coughing.
When fine particles of crystalline silica dust are deposited in the lungs,
Characteristic lung tissue pathology in nodular silicosis consists of fibrotic
Silica
Silica occurs in three forms:
- Crystalline silica exists in seven different forms (polymorphs), depending upon the temperature of formation. The main three polymorphs are quartz, cristobalite, and tridymite. Quartz is the second most common mineral in the world (next to feldspar).[19]
- Microcrystalline silica consists of minute quartz crystals bonded together with amorphous silica. Examples include flint and chert.
- Amorphous silica consists of diatoms, and vitreous silica, produced by heating and then rapid cooling of crystalline silica. Amorphous silica is less toxic than crystalline, but not biologically inert, and diatomite, when heated, can convert to tridymite or cristobalite.
Silica flour is nearly pure SiO2 finely ground. Silica flour has been used as a polisher or buffer, as well as paint extender, abrasive, and filler for cosmetics. Silica flour has been associated with all types of silicosis, including acute silicosis.
Silicosis is due to deposition of fine respirable dust (less than 10
Diagnosis
There are three key elements to the diagnosis of silicosis. First, the patient history should reveal exposure to sufficient silica dust to cause this illness. Second, chest imaging (usually chest x-ray) that reveals findings consistent with silicosis. Third, there are no underlying illnesses that are more likely to be causing the abnormalities. Physical examination is usually unremarkable unless there is complicated disease. The examination findings are not specific for silicosis.[20]
Pulmonary function testing may reveal airflow limitation, restrictive defects, reduced diffusion capacity, mixed defects, or may be normal, especially without complicated disease. Most cases of silicosis do not require tissue biopsy for diagnosis, but this may be necessary in some cases, primarily to exclude other conditions. Assessment of alveolar crystal burden in bronchoalveolar lavage fluid may aid diagnosis.[21]
For uncomplicated silicosis, chest x-ray will confirm the presence of small (< 10 mm) nodules in the lungs, especially in the upper lung zones. Using the
With retraction of the lung tissue, there is compensatory emphysema. Enlargement of the hilum is common with chronic and accelerated silicosis. In about 5–10% of cases, the nodes will calcify circumferentially, producing so-called "eggshell" calcification. This finding is not pathognomonic (diagnostic) of silicosis. In some cases, the pulmonary nodules may also become calcified.
A computed tomography or CT scan can also provide a mode detailed analysis of the lungs, and can reveal cavitation due to concomitant mycobacterial infection.
-
Chest X-ray showing uncomplicated silicosis
-
Complicated silicosis
-
Silicosis ILO Classification 2-2 R-R
-
Fibrothorax and pleural effusion caused by silicosis
Classification
Classification of silicosis is made according to the disease's severity (including radiographic pattern), onset, and rapidity of progression.[22] These include:
- Chronic simple silicosis
- Usually resulting from long-term exposure (10 years or more) to relatively low concentrations of silica dust and usually appearing 10–30 years after first exposure.dyspnea(shortness of breath) are common findings. Radiographically, chronic simple silicosis reveals a profusion of small (<10 mm in diameter) opacities, typically rounded, and predominating in the upper lung zones.
- Accelerated silicosis
- Silicosis that develops 5–10 years after first exposure to higher concentrations of silica dust. Symptoms and x-ray findings are similar to chronic simple silicosis, but occur earlier and tend to progress more rapidly. Patients with accelerated silicosis are at greater risk for complicated disease, including progressive massive fibrosis (PMF).
- Complicated silicosis
- Silicosis can become "complicated" by the development of severe scarring (progressive massive fibrosis, or also known as conglomerate silicosis), where the small nodules gradually become confluent, reaching a size of 1 cm or greater. PMF is associated with more severe symptoms and respiratory impairment than simple disease. Silicosis can also be complicated by other lung disease, such as tuberculosis, non-tuberculous mycobacterial infection, and fungal infection, certain autoimmune diseases, and lung cancer. Complicated silicosis is more common with accelerated silicosis than with the chronic variety.
- Acute silicosis
- Silicosis that develops a few weeks to 5 years after exposure to high concentrations of respirable silica dust. This is also known as silicoproteinosis. Symptoms of acute silicosis include more rapid onset of severe disabling shortness of breath, cough, weakness, and weight loss, often leading to death. The x-ray usually reveals a diffuse alveolar filling with air bronchograms, described as a hemorrhage, and alveolar cell lung cancer.
Prevention
Using the Hierarchy of Controls, there are various methods of preventing exposure to respirable crystalline silica. The best way to prevent silicosis is to avoid worker exposure to dust containing respirable crystalline silica.[24] The next best preventive measure is to control the dust. Water-integrated tools are often used where dust is created during certain tasks. To avoid dust accumulating on clothing and skin, wear a disposable protective suit or seal clothes in an airtight bag and, if possible, shower once returning home.[25]
When dust starts accumulating around a workplace, and the use of water-integrated tools is not feasible, an industrial vacuum should be used to contain and transport dust to a safe location for disposal.[26] Dust can also be controlled through personal dry air filtering.[27] The use of personal protective equipment (PPE) is a measure of last resort when attempting to control exposure to respirable crystalline silica.
Preventing silicosis may require specific measures. One example is during tunnel construction where purpose-designed cabins are used in addition to air scrubbers to filter the air during construction.[28] Items to be considered when selecting respiratory protection include whether it provides the correct level of protection, if facial fit testing has been provided, if the wearer is absent of facial hair, and how filters will be replaced.[28]
Exposure to siliceous dusts in the ceramics industry is reduced by either processing and using the source materials as aqueous suspension or as damp solids, or by the use of dust control measures such as local exhaust ventilation. These have been mandated by legislation, such as The Pottery (Health and Welfare) Special Regulations 1950.[29][30] The Health and Safety Executive in the UK has produced guidelines on controlling exposure to respirable crystalline silica in potteries, and the British Ceramics Federation provide, as a free download, a guidance booklet.
Treatment
Silicosis is a permanent disease with no cure.[18] Treatment options currently available focus on alleviating the symptoms and preventing any further progress of the condition. These include:
- Whole lung lavage. this method involves repeatedly flushing the lungs with saline under intravenous anesthesia, together with mechanical ventilation, to remove the pathogenic factor
- Stopping further exposure to airborne silica,[15] silica dust and other lung irritants, including tobacco smoking.
- Cough suppressants.
- Antibiotics for bacterial lung infection.
- tuberculin skin test or IGRAblood test.
- Prolonged anti-tuberculosis (multi-drug regimen) for those with active TB.
- Chest physiotherapy to help the bronchial drainage of mucus.
- hypoxemia, if present.
- Bronchodilators to facilitate breathing.
- Lung transplantation to replace the damaged lung tissue is the most effective treatment, but is associated with severe risks of its own from the lung transplant surgery as well as from consequences of long-term immunosuppression (e.g., opportunistic infections).
- For acute silicosis, bronchoalveolar lavage may alleviate symptoms, but does not decrease overall mortality.
- Preliminary work utilising whole lung lavage for patients with artificial stone-associated silicosis has shown significant radiological improvement following whole lung lavage.[31]
Epidemiology
Globally, silicosis resulted in 46,000 deaths in 2013, down from 55,000 deaths in 1990.[6]
Occupational silicosis

Silicosis is the most common occupational lung disease worldwide. It occurs everywhere, but is especially common in developing countries.[32] From 1991 to 1995, China reported more than 24,000 deaths due to silicosis each year.[13] It also affects developed nations. In the United States, it is estimated that between one and two million workers have had occupational exposure to crystalline silica dust and 59,000 of these workers will develop silicosis sometime in the course of their lives.[13][33]
According to CDC data,[34] silicosis in the United States is relatively rare. The incidence of deaths due to silicosis declined by 84% between 1968 and 1999, and only 187 deaths in 1999 had silicosis as the underlying or contributing cause.[35] Additionally, cases of silicosis in Michigan, New Jersey, and Ohio are highly correlated to industry and occupation.[36]
The latest data from The Health and Safety Executive shows that there are typically between 10 and 20 annual silicosis deaths in recent years, with an average of 12 per year over the last 10 years. In 2019 in the UK, there were 12 deaths in 10 years.[37]
Although silicosis has been a known occupational disease for centuries, the
Chronic simple silicosis has been reported to occur from environmental exposures to silica in regions with high silica soil content and frequent dust storms.[41]
Also, the mining establishment of
Because of work-exposure to silica dust, silicosis is an occupational hazard to construction, railroad,
In less developed countries where work conditions are poor and respiratory equipment is seldom used, the life expectancy is low (e.g. for silver miners in Potosí, Bolivia, is around 40 years due to silicosis).
Recently, silicosis in Turkish denim sandblasters was detected as a new cause of silicosis due to recurring, poor working conditions.[46]
Silicosis is seen in horses associated with inhalation of dust from certain cristobalite-containing soils in California.
A recent rise of cases in Australia has been associated with the manufacture and installation of
Silicosis has also been identified as one of many long-term health outcomes for first responders from the terrorist attacks of September 11, 2001, after having been exposed to dust containing high concentrations of respirable crystalline silica, as well as other metals and toxins.[54]
Desert lung disease
A non-occupational form of silicosis has been described that is caused by long-term exposure to sand dust in desert areas, with cases reported from the Sahara, Libyan desert and the Negev.[55] The disease is caused by deposition of this dust in the lung.[56] Desert lung disease may be related to Al Eskan disease, a lung disorder thought to be caused by exposure to sand dust containing organic antigens, which was first diagnosed after the 1990 Gulf war.[57] The relative importance of the silica particles themselves and the microorganisms that they carry in these health effects remains unclear.[58]
Regulation in the US
In March 2016, OSHA officially mandated that companies must provide certain safety measures for employees who work with or around silica, in order to prevent silicosis, lung cancer, and other silica-related diseases.[59]
Key provisions
One of the main updates to OSHA's silica standard was the reduction of the permissible exposure limit (PEL) for respirable crystalline silica from 250 to 50 micrograms per cubic meter of air, averaged over an 8-hour shift.[60] The updated standard also shifts the focus of controlling silica exposure from the use of PPE (respirators) to the use of engineering controls (such as using water-integrated tools or vacuum systems) and administrative controls (limiting exposure time per shift). Employers are still required to provide respirators when engineering and administrative controls cannot adequately limit exposure.[60]
Additional provisions include limiting worker access to high exposure areas, signage requirements in high exposure areas, the development of a written exposure control plan, medical exams to highly exposed workers (optional for exposed employees), and training for workers on silica risks and how to limit exposures. Special equipment may be needed to prevent machine water from evaporating and leaving behind dust.[61] The standard also provides requirements for cleaning up the slurry left behind when water-integrated tools are used as an engineering control.
The medical exams include a discussion with a physician or licensed health care provider (PLHCP) of prior respiratory health, chest X-ray, pulmonary function test, latent tuberculosis infection, and any other tests deemed necessary by the PLHCP. These medical exams are to occur within 30 days of the initial assignment that includes silica exposure and must be made available for renewal at least every three years unless the PLHCP deems otherwise.
As part of the updated standard, OSHA created a table of specific engineering and administrative control methods to reduce silica exposure when using specific tools in 18 different applications that are known to create an exposure to silica from stationary masonry saws to using handheld grinders.[60]
An additional provision exists for small business who are provided flexibility.[62]
Compliance schedule
Both standards contained in the final rule took effect on June 23, 2016, after which industries had one to five years to comply with most requirements, based on the following schedule:
- Construction – June 23, 2017, one year after the effective date.
- General Industry and Maritime – June 23, 2018, two years after the effective date.
- Hydraulic Fracturing – June 23, 2018, two years after the effective date for all provisions except Engineering Controls, which have a compliance date of June 23, 2021.[62]
See also
- Pneumoconiosis – Class of interstitial lung diseases
- Asbestosis – Pneumoconiosis caused by inhalation and retention of asbestos fibers
- Health effects arising from the September 11 attacks – Health issues and effects during and after the September 11 attacks
- Hawks Nest Tunnel disaster – Tunnel in West Virginia where hundreds of workers contracted silicosis
- Dust pneumonia – medical condition
- Frances Perkins
References
- ISBN 978-0-470-74261-7. Archivedfrom the original on 31 December 2013. Retrieved 24 August 2012.
- ^ "Pneumonoultramicroscopicsilicovolcanoconiosis". Lexico UK English Dictionary. Oxford University Press. Archived from the original on 2020-03-22.
- ^ "Pneumonoultramicroscopicsilicovolcanoconiosis". Merriam-Webster.com Dictionary.
- ^ Derived from Gr. πνεῦμα pneúm|a (lung) + buffer vowel -o- + κόνις kóni|s (dust) + Eng. scient. suff. -osis (like in asbest"osis" and silic"osis", see ref. 10).
- ^ "Prevention of Silicosis Deaths". July 22, 2015.
- ^ PMID 25530442.)
{{cite journal}}:|first1=has generic name (help)CS1 maint: numeric names: authors list (link - ^ United States Bureau of Mines, "Bulletin: Volumes 476–478", U.S. G.P.O., (1995), p 63.
- ^ Rosen G: The History of Miners' Diseases: A Medical and Social Interpretation. New York, Schuman, 1943, pp.459–476.
- ^ 'The Successful Prevention Of Silicosis Among China Biscuit Workers In The North Staffordshire Potteries.' A. Meiklejohn. British Journal Of Industrial Medicine, October 1963; 20(4): 255–263
- ^ PMID 2838005.
- ^ Stop Silicosis, retrieved 2022-04-21
- ^ Lungs of stone: How Silica has sickened a generation of quartz cutters
- ^ a b c "Silicosis Fact Sheet". World Health Organization. May 2000. Archived from the original on 2007-05-10. Retrieved 2007-05-29.
- PMID 7952577.
- ^ PMID 30726026.
- PMID 16403810.
- PMID 18577586.
- ^ S2CID 26302715.
- ^ Crystalline Silica Primer, US Dept of the Interior and US Bureau of Mines, 1992.
- S2CID 246943673.
- S2CID 246943673.
- ^ NIOSH Hazard Review. Health Effects of Occupational Exposure to Respirable Crystalline Silica. DHHS 2002-129. pp. 23.
- ^ Weisman DN and Banks DE. Silicosis. In: Interstitial Lung Disease. 4th ed. London: BC Decker Inc. 2003, pp391.
- ^ World Health Organization (2007). "Elimination of Silicosis" (PDF). GOHNET NEWSLETTER. No. 12. Retrieved 2019-11-27.
- ^ World Health Organization (2007). "Elimination of Silicosis" (PDF). GOHNET NEWSLETTER. No. 12. Retrieved 2019-11-27.
- ^ "Guide to Training Your Staff for OSHA Compliance | Industrial Vacuum". www.industrialvacuum.com. 29 April 2016. Retrieved 2018-10-23.
- ^ CPWR-The Center for Construction Research and Training. "Work Safely with Silica: methods to control silica exposure". Archived from the original on 2012-12-20.
- ^ a b ATS (7 January 2019). "NSW Air Quality Working Group". Australian Tunnelling Society. Retrieved 7 January 2019.
- ^ [1]
- ^ 'Whitewares: Production, Testing And Quality Control." W.Ryan & C.Radford. Pergamon Press. 1987
- S2CID 232047922.
- PMID 8561170.
- ^ "Safety and Health Topics Silica, Crystalline". Occupational Safety and Health Administration. March 2007. Archived from the original on 2007-05-18. Retrieved 2007-05-29.
- doi:10.26616/NIOSHPUB2004146. 2004-146. Archivedfrom the original on 2017-11-23.
- ^ NIOSH & 2004-146, Fig2-192
- ^ NIOSH & 2004-146, Fig2-190
- ^ "Silicosis and coal workers' pneumoconiosis statistics in Great Britain, 2021" (PDF). hse.gov.uk/. December 2021.
- ^ "The Hawks Nest Tunnel," Patricia Spangler, 2008
- ^ Keenan, Steve (2008-04-02). "Book explores Hawks Nest tunnel history » Local News » The Fayette Tribune, Oak Hill, W.Va". Fayettetribune.com. Archived from the original on 2008-04-07. Retrieved 2012-02-16.
- ^ "The Hawk’s Nest Incident: America’s Worst Industrial Disaster," Dr. Martin Cherniack 1986
- PMID 2068689.
- ^ "Los Angeles Silica Exposure Lawyer". Rose, Klein & Marias LLP. Retrieved 2022-06-01.
- ^ Cole, Kate (7 January 2020). "Investigating best practice to prevent illness and disease in tunnel construction workers". Winston Churchill Trust Australia. Archived from the original on 31 March 2020. Retrieved 7 January 2020.
- ^ "NIOSHTIC-2 Publications Search - 20040975 - OSHA/NIOSH hazard alert: worker exposure to silica during hydraulic fracturing". www.cdc.gov. Archived from the original on 2018-03-17. Retrieved 2018-03-16.
- PMID 9032226.
- ^ Denim sandblasters contract fatal silicosis in illegal workshops Archived 2009-10-19 at the Wayback Machine
- ^ Art Gallery of NSW: Noel Couniham Collection Archived 2014-09-03 at the Wayback Machine
- ^ Atkin, Michael (7 January 2020). "The biggest lung disease crisis since asbestos: Our love of stone kitchen benchtops is killing workers". ABC News. Retrieved 7 January 2020.
- ^ Atkin, Michael (7 January 2020). "Silicosis-causing silica significantly 'more potent' than asbestos". ABC News. Retrieved 7 January 2020.
- ^ Cole, Kate (7 January 2020). "Silicosis is not the new Asbestosis". ABC Radio National. Retrieved 7 January 2020.
- ^ "Preventing exposure to silica from engineered stone benchtops". Worksafe Tasmania. Government of Tasmania. Retrieved 1 December 2022.
- ^ DoH (2019-11-21). "The Department of Health National Dust Disease Taskforce". Department of Health. Retrieved 7 January 2020.
- ^ Lloyd, Mary (22 November 2022). "Risky, silicosis-causing stone product must be banned, construction union tells government". ABC News. Australian Broadcasting Corporation. Retrieved 1 December 2022.
- PMID 30866415.
- PMID 3663563.
- PMID 2549601.
- PMID 1333577.
- PMID 17630335.
- ^ "OSHA publishes final rule on silica". Archived from the original on 2016-08-18. Retrieved 2016-08-18.
- ^ a b c "1926.1153 Respirable Crystalline Silica". osha.gov. March 25, 2016. Retrieved March 17, 2022.
- ^ Greenfieldboyce, Nell (2019-10-02). "Workers Are Falling Ill, Even Dying, After Making Kitchen Countertops". National Public Radio. Retrieved 2019-11-27.
- ^ a b "OSHA's Final Rule to Protect Workers from Exposure to Respirable Crystalline Silica". www.osha.gov. Archived from the original on 2016-08-20. Retrieved 2016-07-22.
External links
- Crystalline silica, National Institute for Occupational Safety and Health, US.
- Preventing Silicosis and Deaths in Construction workers, National Institute for Occupational Safety and Health, US.
- OSHA’s Respirable Crystalline Silica Standard for Construction, Occupational Safety and Health Administration, US.




