Smallpox vaccine
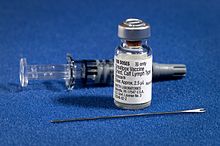 The smallpox vaccine diluent in a syringe alongside a vial of Dryvax dried smallpox vaccine and bifurcated needle | |
| Vaccine description | |
|---|---|
| Target | Smallpox, Mpox |
| Vaccine type | Live virus |
| Clinical data | |
| Trade names | ACAM2000, Imvanex, Jynneos, others |
| AHFS/Drugs.com | Monograph |
| License data | |
| Pregnancy category |
|
Subcutaneous | |
| ATC code | |
| Legal status | |
| Legal status | |
| Identifiers | |
| DrugBank | |
| UNII | |
| KEGG | |
The smallpox vaccine is the first vaccine to have been developed against a contagious disease. In 1796, British physician Edward Jenner demonstrated that an infection with the relatively mild cowpox virus conferred immunity against the deadly smallpox virus. Cowpox served as a natural vaccine until the modern smallpox vaccine emerged in the 20th century. From 1958 to 1977, the World Health Organization (WHO) conducted a global vaccination campaign that eradicated smallpox, making it the only human disease to be eradicated. Although routine smallpox vaccination is no longer performed on the general public, the vaccine is still being produced to guard against bioterrorism, biological warfare, and mpox.[10][11]
The term vaccine derives from the Latin word for cow, reflecting the origins of smallpox vaccination. Edward Jenner referred to cowpox as variolae vaccinae (smallpox of the cow). The origins of the smallpox vaccine became murky over time,
Types
As the oldest vaccine, the smallpox vaccine has gone through several generations of medical technology. From 1796 to the 1880s, the vaccine was transmitted from one person to another through arm-to-arm vaccination. Smallpox vaccine was successfully maintained in cattle starting in the 1840s, and calf lymph vaccine became the leading smallpox vaccine in the 1880s. First-generation vaccines grown on the skin of live animals were widely distributed in the 1950s–1970s to eradicate smallpox. Second-generation vaccines were grown in chorioallantoic membrane or cell cultures for greater purity, and they were used in some areas during the smallpox eradication campaign. Third-generation vaccines are based on attenuated strains of vaccinia and saw limited use prior to the eradication of smallpox.[15]
All three generations of vaccine are available in stockpiles. First and second-generation vaccines contain live unattenuated vaccinia virus and can cause serious side effects in a small percentage of recipients, including death in 1–10 people per million vaccinations. Third-generation vaccines are much safer due to the milder side effects of the attenuated vaccinia strains.[15] Second and third-generation vaccines are still being produced, with manufacturing capacity being built up in the 2000s due to fears of bioterrorism and biological warfare.
First-generation
The first-generation vaccines are manufactured by growing live vaccinia virus in the skin of live animals. Most first-generation vaccines are calf lymph vaccines that were grown on the skin of cows, but other animals were also used, including sheep.[15] The development of freeze-dried vaccine in the 1950s made it possible to preserve vaccinia virus for long periods of time without refrigeration, leading to the availability of freeze-dried vaccines such as Dryvax.[16][17]: 115
The vaccine is administered by multiple puncture of the skin (scarification) with a bifurcated needle that holds vaccine solution in the fork.[18] The skin should be cleaned with water rather than alcohol,[18] as the alcohol could inactivate the vaccinia virus.[17]: 292 [19] If alcohol is used, it must be allowed to evaporate completely before the vaccine is administered.[17]: 292 Vaccination results in a skin lesion that fills with pus and eventually crusts over. This manifestation of localized vaccinia infection is known as a vaccine "take" and demonstrates immunity to smallpox. After 2–3 weeks, the scab will fall off and leave behind a vaccine scar.[20]
First generation vaccines consist of live, unattenuated vaccinia virus. One-third of first-time vaccinees develop side effects significant enough to miss school, work, or other activities, or have difficulty sleeping. 15–20% of children receiving the vaccine for the first time develop fevers of over 102 °F (39 °C). The vaccinia lesion can transmit the virus to other people.[20] Rare side effects include postvaccinal encephalitis and myopericarditis.[20][21] Many countries have stockpiled first generation smallpox vaccines. In a 2006 predictive analysis of casualties if there were a mass vaccination of the populations of Germany and the Netherlands, it was estimated that a total of 9.8 people in the Netherlands and 46.2 people in Germany would die from uncontrolled vaccinia infection after being vaccinated with the New York City Board of Health strain. More deaths were predicted for vaccines based other strains: Lister (55.1 Netherlands, 268.5 Germany) and Bern (303.5 Netherlands, 1,381 Germany).[22][23]
Second-generation
The second-generation vaccines consist of live vaccinia virus grown in the chorioallantoic membrane or cell culture. The second-generation vaccines are also administered through scarification with a bifurcated needle, and they carry the same side effects as the first-generation vaccinia strain that was cloned. However, the use of eggs or cell culture allows for vaccine production in a sterile environment, while first-generation vaccine contains skin bacteria from the animal that the vaccine was grown on.[15]
Ernest William Goodpasture, Alice Miles Woodruff, and G. John Buddingh grew vaccinia virus on the chorioallantoic membrane of chicken embryos in 1932.[24] The Texas Department of Health began producing egg-based vaccine in 1939 and started using it in vaccination campaigns in 1948.[17]: 588 Lederle Laboratories began selling its Avianized smallpox vaccine in the United States in 1959.[25] Egg-based vaccine was also used widely in Brazil, New Zealand, and Sweden, and on a smaller scale in many other countries. Concerns about temperature stability and avian sarcoma leukosis virus prevented it from being used more widely during the eradication campaign, although no increase in leukemia was seen in Brazil and Sweden despite the presence of ASLV in the chickens.[17]: 588
Vaccinia was first grown in cell culture in 1931 by Thomas Milton Rivers. The WHO funded work in the 1960s at the Dutch National Institute for Public Health and the Environment (RIVM) on growing the Lister/Elstree strain in rabbit kidney cells and tested it in 45,443 Indonesian children in 1973, with comparable results to the same strain of calf lymph vaccine.[17]: 588–589 Two other cell culture vaccines were developed from the Lister strain in the 2000s: Elstree-BN (Bavarian Nordic) and VV Lister CEP (Chicken Embryo Primary, Sanofi Pasteur).[15][26][27] Lister/Elstree-RIVM was stockpiled in the Netherlands, and Elstree-BN was sold to some European countries for stockpiles.[15] However, Sanofi dropped its own vaccine after it acquired Acambis in 2008.
ACAM2000 is a vaccine developed by Acambis, which was acquired by Sanofi Pasteur in 2008, before selling the smallpox vaccine to Emergent Biosolutions in 2017. Six strains of vaccinia were isolated from 3,000 doses of Dryvax and found to exhibit significant variation in virulence. The strain with the most similar virulence to the overall Dryvax mixture was selected and grown in MRC-5 cells to make the ACAM1000 vaccine. After a successful Phase I trial of ACAM1000, the virus was passaged three times in Vero cells to develop ACAM2000, which entered mass production at Baxter. The United States ordered over 200 million doses of ACAM2000 in 1999–2001 for its stockpile, and production is ongoing to replace expired vaccine.[28][29]
Third-generation
The third-generation vaccines are based on attenuated vaccinia viruses that are much less virulent and carry lesser side effects. The attenuated viruses may be replicating or non-replicating.[15]
MVA
MVA stimulates the production of fewer antibodies than replicating vaccines.[31] During the smallpox eradication campaign, MVA was considered to be a pre-vaccine that would be administered before a replicating vaccine to reduce the side effects, or an alternative vaccine that could be safely given to people at high risk from a replicating vaccine.[17]: 585 Japan evaluated MVA and rejected it due to its low immunogenicity, deciding to develop its own attenuated vaccine instead.[32] In the 2000s, MVA was tested in animal models at much higher dosages.[33] When MVA is given to monkeys at 40 times the dosage of Dryvax, it stimulates a more rapid immune response while still causing lesser side effects.[34]
MVA-BN
MVA-BN (also known as: Imvanex in the European Union; Imvamune in Canada; and Jynneos[35][36]) is a vaccine manufactured by Bavarian Nordic by growing MVA in cell culture. Unlike replicating vaccines, MVA-BN is administered by injection via the subcutaneous route and does not result in a vaccine "take."[37] A "take" or "major cutaneous reaction" is a pustular lesion or an area of definite induration or congestion surrounding a central lesion, which can be a scab or an ulcer.[38]
MVA-BN can also be administered intradermally to increase the number of available doses.[39] It is safer for immunocompromised patients and those who are at risk from a vaccinia[definition needed] infection.[citation needed] MVA-BN has been approved in the European Union,[9] Canada,[40][41][42] and the United States.[43][44] Clinical trials have found that MVA-BN is safer and just as immunogenic as ACAM2000.[45][46][47] This vaccine has also been approved for use against mpox.[48][49][50]
LC16m8
LC16m8 is a replicating attenuated strain of vaccinia that is manufactured by Kaketsuken in Japan. Working at the Chiba Serum Institute in Japan, So Hashizume passaged the Lister strain 45 times in primary rabbit kidney cells, interrupting the process after passages 36, 42, and 45 to grow clones on chorioallantoic membrane and select for pock size. The resulting variant was designated LC16m8 (Lister clone 16, medium pocks, clone 8). Unlike the severely-damaged MVA, LC16m8 contains every gene that is present in the ancestral vaccinia. However, a single-nucleotide deletion truncates membrane protein B5R from a residue length of 317 to 92. Although the truncated protein decreases production of extracellular enveloped virus, animal models have shown that antibodies against other membrane proteins are sufficient for immunity. LC16m8 was approved in Japan in 1975 after testing in over 50,000 children. Vaccination with LC16m8 results in a vaccine "take", but safety is similar to MVA.[32]
Safety
Vaccinia is infectious, which improves its effectiveness, but causes serious complications for people with impaired
In May 2007, the
Stockpiles
Since smallpox has been eradicated, the public is not routinely vaccinated against the disease. The World Health Organization maintained a stockpile of 200 million doses in 1980, to guard against reemergence of the disease, but 99% of the stockpile was destroyed in the late 1980s when smallpox failed to return.[15] After the September 11 attacks in 2001, many governments began building up vaccine stockpiles again for fear of bioterrorism. Several companies sold off their stockpiles of vaccines manufactured in the 1970s, and production of smallpox vaccines resumed.[54] Aventis Pasteur discovered a stockpile from the 1950s and donated it to the U.S. government.[55]
Stockpiles of newer vaccines must be repurchased periodically since they carry expiration dates. The United States had received 269 million doses of ACAM2000 and 28 million doses of MVA-BN by 2019,
| Country, region, or organization | Year | Doses (millions) | Composition (generation) |
|---|---|---|---|
| 2013 | 2.7 |
| |
(pledged) |
2018 | 27 | Various (1st, 2nd, 3rd)[61][62] |
| 2006 | 55 | 55 million Pourquier (1st)[63] | |
| 2022 | 100 | ||
| 2022 | 5[64] | ||
| 2006 | 56 | LC16m8 (3rd)[32] | |
| 2017 | ? | Lister/Elstree-RIVM (2nd)[17]: 588–589 | |
| 2022 | 35 | Lancy-Vaxina (1st)[65][66] | |
| 2022 | 185 |
History
Variolation
The mortality of the severe form of smallpox – variola major – was very high without vaccination, up to 35% in some outbreaks.
Variolation was also practiced throughout the latter half of the 17th century by physicians in
...scarred the wrists, legs, and forehead of the patient, placed a fresh and kindly pock in each incision and bound it there for eight or ten days, after this time the patient was credibly informed. The patient would then develop a mild case [of smallpox], recover, and thereafter be immune.[77]
—Dr. Peter Kennedy
Stimulated by a severe epidemic, variolation was first employed in North America in 1721. The procedure had been known in Boston since 1706, when preacher
The inoculation technique was documented as having a mortality rate of only one in a thousand. Two years after Kennedy's description appeared, March 1718, Dr. Charles Maitland successfully inoculated the five-year-old son of the British ambassador to the Turkish court under orders from the ambassador's wife Lady Mary Wortley Montagu, who four years later introduced the practice to England.[80]
An account from letter by Lady
The small-pox so fatal and so general amongst us is here entirely harmless by the invention of ingrafting (which is the term they give it). There is a set of old women who make it their business to perform the operation. Every autumn in the month of September, when the great heat is abated, people send to one another to know if any of their family has a mind to have the small-pox. They make parties for this purpose, and when they are met (commonly fifteen or sixteen together) the old woman comes with a nutshell full of the matter of the best sort of small-pox and asks what veins you please to have opened. She immediately rips open that you offer to her with a large needle (which gives you no more pain than a common scratch) and puts into the vein as much venom as can lye upon the head of her needle, and after binds up the little wound with a hollow bit of shell, and in this manner opens four or five veins. … The children or young patients play together all the rest of the day and are in perfect health till the eighth. Then the fever begins to seize them and they keep their beds two days, very seldom three. They have very rarely above twenty or thirty in their faces, which never mark, and in eight days time they are as well as before the illness. … There is no example of any one that has died in it, and you may believe I am very well satisfied of the safety of the experiment since I intend to try it on my dear little son. I am patriot enough to take pains to bring this useful invention into fashion in England, and I should not fail to write to some of our doctors very particularly about it if I knew any one of them that I thought had virtue enough to destroy such a considerable branch of their revenue for the good of mankind, but that distemper is too beneficial to them not to expose to all their resentment the hardy wight that should undertake to put an end to it. Perhaps if I live to return I may, however, have courage to war with them.[81]
Early vaccination

In the early empirical days of vaccination, before
During the earlier days of empirical experimentation in 1758, American Calvinist Jonathan Edwards died from a smallpox inoculation. Some of the earliest statistical and epidemiological studies were performed by James Jurin in 1727 and Daniel Bernoulli in 1766.[83] In 1768, Dr John Fewster reported that variolation induced no reaction in persons who had had cowpox.[84][85]

Perhaps there was already an informal public understanding of some connection between disease resistance and working with cattle. The "beautiful milkmaid" seems to have been a frequent image in the art and literature of this period. But it is known for certain that in the years following 1770, at least six people in England and Germany (Sevel, Jensen, Jesty 1774, Rendall, Plett 1791) tested successfully the possibility of using the cowpox vaccine as an immunization for smallpox in humans.[88]

Jenner sent a paper reporting his observations to the Royal Society in April 1797. It was not submitted formally and there is no mention of it in the Society's records. Jenner had sent the paper informally to
The introduction of the vaccine to the New World took place in Trinity, Newfoundland, in 1798 by Dr. John Clinch, boyhood friend and medical colleague of Jenner.[95][96] The first smallpox vaccine in the United States was administered in 1799. The physician Valentine Seaman gave his children a smallpox vaccination using a serum acquired from Jenner.[97][98] By 1800, Jenner's work had been published in all the major European languages and had reached Benjamin Waterhouse in the United States – an indication of rapid spread and deep interest.[99]: 262–67 Despite some concern about the safety of vaccination the mortality using carefully selected vaccine was close to zero, and it was soon in use all over Europe and the United States.[100][101]

In 1804 the Balmis Expedition, an official Spanish mission commanded by Francisco Javier de Balmis, sailed to spread the vaccine throughout the Spanish Empire, first to the Canary Islands and on to Spanish Central America. While his deputy, José Salvany, took vaccine to the west and east coasts of Spanish South America, Balmis sailed to Manila in the Philippines and on to Canton and Macao on the Chinese coast. He returned to Spain in 1806.[102] The vaccine was not carried in the form of flasks, but in the form of 22 orphaned boys, who were 'carriers' of the live cowpox virus. After arrival, "other Spanish governors and doctors used enslaved girls to move the virus between islands, using lymph fluid harvested from them to inoculate their local populations".[103]
The first state to introduce compulsory vaccinations was the Principality of Lucca and Piombino on 25 September 1806.[105] On 26 August 1807, Bavaria introduced a similar measure. Baden followed in 1809, Prussia in 1815, Württemberg in 1818, Sweden in 1816, England in 1867 and the German Empire in 1874 through the Reichs Vaccination Act.[106][107] In Lutheran Sweden, the Protestant clergy played a pioneering role in voluntary smallpox vaccination as early as 1800.[108] The first vaccination was carried out in Liechtenstein in 1801, and from 1812 it was mandatory to vaccinate.[109]
The question of who first tried cowpox inoculation/vaccination cannot be answered with certainty. Most, but still limited, information is available for
Publication of the Inquiry and the subsequent energetic promulgation by Jenner of the idea of vaccination with a virus other than variola virus constituted a watershed in the control of smallpox for which he, more than anyone else deserves the credit.
As vaccination spread, some European countries made it compulsory. Concern about its safety led to opposition and then repeal of legislation in some instances.[112]: 236–40 [113] Compulsory infant vaccination was introduced in England by the 1853 Vaccination Act. By 1871, parents could be fined for non-compliance, and then imprisoned for non-payment.[113]: 202–13 This intensified opposition, and the 1898 Vaccination Act introduced a conscience clause.[114] This allowed exemption on production of a certificate of conscientious objection signed by two magistrates. Such certificates were not always easily obtained and a further Act in 1907 allowed exemption by a statutory declaration which could not be refused. Although theoretically still compulsory, the 1907 Act effectively marked the end of compulsory infant vaccination in England.[113]: 233–38

In the United States vaccination was regulated by individual states, the first to impose compulsory vaccination being Massachusetts in 1809. There then followed sequences of compulsion, opposition and repeal in various states. By 1930 Arizona, Utah, North Dakota and Minnesota prohibited compulsory vaccination, 35 states allowed regulation by local authorities, or had no legislation affecting vaccination, whilst in ten states, including Washington, D.C. and Massachusetts, infant vaccination was compulsory.[99]: 292–93 Compulsory infant vaccination was regulated by only allowing access to school for those who had been vaccinated.[115] Those seeking to enforce compulsory vaccination argued that the public good overrode personal freedom, a view supported by the U.S. Supreme Court in Jacobson v. Massachusetts in 1905, a landmark ruling which set a precedent for cases dealing with personal freedom and the public good.[116]
Louis T. Wright,[117] an African-American Harvard Medical School graduate (1915), introduced, while serving in the Army during World War I, intradermal, smallpox vaccination for the soldiers.[118]
Developments in production
Until the end of the 19th century, vaccination was performed either directly with vaccine produced on the skin of calves or, particularly in England, with vaccine obtained from the calf but then maintained by arm-to-arm transfer;
Vaccine produced by Copeman's method was the only type issued free to public vaccinators by the English Government Vaccine Establishment from 1899. At the same time the 1898 Vaccination Act banned arm-to-arm vaccination, thus preventing transmission of syphilis by this vaccine. However, private practitioners had to purchase vaccine from commercial producers.[124] Although proper use of glycerine reduced bacterial contamination considerably the crude starting material, scraped from the skin of infected calves, was always heavily contaminated and no vaccine was totally free from bacteria. A survey of vaccines in 1900 found wide variations in bacterial contamination. Vaccine issued by the Government Vaccine Establishment contained 5,000 bacteria per gram, while commercial vaccines contained up to 100,000 per gram.[125] The level of bacterial contamination remained unregulated until the Therapeutic Substances Act, 1925 set an upper limit of 5,000 per gram, and rejected any batch of vaccine found to contain the causative organisms of erysipelas or wound infections.[93] Unfortunately glycerolated vaccine soon lost its potency at ambient temperatures which restricted its use in tropical climates. However, it remained in use into the 1970s where a satisfactory cold chain was available. Animals continued to be widely used by vaccine producers during the smallpox eradication campaign. A WHO survey of 59 producers, some of whom used more than one source of vaccine, found that 39 used calves, 12 used sheep and 6 used water buffalo, whilst only 3 made vaccine in cell culture and 3 in embryonated hens' eggs.[17]: 543–45 English vaccine was occasionally made in sheep during World War I but from 1946 only sheep were used.[120]
In the late 1940s and early 1950s,
In a letter about landmarks in the history of smallpox vaccine, written to and quoted from by Derrick Baxby, Donald Henderson, chief of the Smallpox Eradication Unit from 1967 to 1977 wrote; "Copeman and Collier made an enormous contribution for which neither, in my opinion ever received due credit".[128]
Smallpox vaccine was inoculated by scratches into the superficial layers of the skin, with a wide variety of instruments used to achieve this. They ranged from simple needles to multi-pointed and multi-bladed spring-operated instruments specifically designed for the purpose.[129]
A major contribution to smallpox vaccination was made in the 1960s by Benjamin Rubin, an American microbiologist working for Wyeth Laboratories. Based on initial tests with textile needles with the eyes cut off transversely half-way he developed the bifurcated needle. This was a sharpened two-prong fork designed to hold one dose of reconstituted freeze-dried vaccine by capillarity.[130] Easy to use with minimum training, cheap to produce ($5 per 1000), using one quarter as much vaccine as other methods, and repeatedly re-usable after flame sterilization, it was used globally in the WHO Smallpox Eradication Campaign from 1968.[17]: 472–73, 568–72 Rubin estimated that it was used to do 200 million vaccinations per year during the last years of the campaign.[130] Those closely involved in the campaign were awarded the "Order of the Bifurcated Needle". This, a personal initiative by Donald Henderson, was a lapel badge, designed and made by his daughter, formed from the needle shaped to form an "O". This represented "Target Zero", the objective of the campaign.[131]
Eradication of smallpox

Smallpox was eradicated by a massive international search for outbreaks, backed up with a vaccination program, starting in 1967. It was organised and co-ordinated by a
Anti-terrorism preparation
Among more than 270,000 US military service members vaccinated with smallpox vaccine between December 2002, and March 2003, eighteen cases of probable myopericarditis were reported (all in first-time vaccinees who received the NYCBOH strain of vaccinia virus), an incidence of 7.8 per 100,000 during the 30 days they were observed. All cases were in young, otherwise healthy adult white men and all survived.[133]
In 2002, the United States government started a program to vaccinate 500,000 volunteer health care professionals throughout the country. Recipients were healthcare workers who would be first-line responders in the event of a bioterrorist attack. Many healthcare workers refused or did not pursue vaccination, worried about vaccine side effects, compensation and liability. Most did not see an immediate need for the vaccine. Some healthcare systems refused to participate, worried about becoming a destination for smallpox patients in the event of an epidemic.[134] Fewer than 40,000 actually received the vaccine.[135]
On 21 April 2022,
Origin
The origin of the modern smallpox vaccine has long been unclear,
In 1939, Allan Watt Downie showed that the vaccinia virus was serologically distinct from the "spontaneous" cowpox virus.[13] This work established vaccinia and cowpox as two separate viral species. The term vaccinia now refers only to the smallpox vaccine,[144] while cowpox no longer has a Latin name.[145] The development of whole genome sequencing in the 1990s made it possible to compare orthopoxvirus genomes and identify their relationships with each other. The horsepox virus was sequenced in 2006 and found to be most closely related to vaccinia.[146] In a phylogenetic tree of the orthopoxviruses, horsepox forms a clade with vaccinia strains, and cowpox strains form a different clade.[14]
Horsepox is extinct in the wild, and the only known sample was collected in 1976.[147] Because the sample was collected at the end of the smallpox eradication campaign, scientists considered the possibility that horsepox is a strain of vaccinia that had escaped into the wild.[148] However, as more smallpox vaccines were sequenced, older vaccines were found to be more similar to horsepox than modern vaccinia strains. A smallpox vaccine manufactured by Mulford in 1902 is 99.7% similar to horsepox, closer than any previously known strain of vaccinia.[149] Modern Brazilian vaccines with a documented introduction date of 1887, made from material collected in an 1866 outbreak of "cowpox" in France, are more similar to horsepox than other strains of vaccinia.[150] Five smallpox vaccines manufactured in the United States in 1859–1873 are most similar to each other and horsepox,[148] as well as the 1902 Mulford vaccine.[151] One of the 1859–1873 vaccines was identified as a novel strain of horsepox, containing a complete gene from the 1976 horsepox sample that has deletions in vaccinia.[151]
Terminology
The word "vaccine" is derived from Variolae vaccinae (i.e. smallpox of the cow), the term devised by Jenner to denote cowpox and used in the long title of his An enquiry into the causes and effects of Variolae vaccinae, known by the name of cow pox.[92] Vaccination, the term which soon replaced cowpox inoculation and vaccine inoculation, was first used in print by Jenner's friend, Richard Dunning in 1800.[87] Initially, the terms vaccine/vaccination referred only to smallpox, but in 1881 Louis Pasteur proposed at the 7th International Congress of Medicine[152] that to honour Jenner the terms be widened to cover the new protective inoculations being introduced.[153] According to some sources the term was first introduced by Jenner's friend Richard Dunning in 1800.[154]
References
- ^ "ACAM2000 smallpox vaccine (live vaccinia virus) vial with diluent". Therapeutic Goods Administration (TGA). Archived from the original on 18 April 2015. Retrieved 8 July 2022.
- ^ "Imvamune Product information". Health Canada. 25 April 2012. Archived from the original on 22 June 2021. Retrieved 8 July 2022.
- ^ "Smallpox vaccine Product information". Health Canada. 25 April 2012. Archived from the original on 8 July 2022. Retrieved 8 July 2022.
- ^ "Smallpox vaccine Product information". Health Canada. 25 April 2012. Archived from the original on 8 July 2022. Retrieved 8 July 2022.
- ^ "Regulatory Decision Summary for ACAM2000". Drug and Health Products Portal. 5 December 2023. Retrieved 2 April 2024.
- ^ "Jynneos Smallpox and Monkeypox Vaccine" (PDF). Archived (PDF) from the original on 3 September 2023. Retrieved 2 September 2023.
- ^ "ACAM2000 (smallpox- vaccinia vaccine, live injection, powder, lyophilized, for solution)". DailyMed. 21 March 2018. Archived from the original on 24 May 2022. Retrieved 26 May 2022.
- ^ "Jynneos- vaccinia virus modified strain ankara-bavarian nordic non-replicating antigen injection, suspension". DailyMed. 14 February 2022. Archived from the original on 27 May 2022. Retrieved 26 May 2022.
- ^ a b "Imvanex EPAR". European Medicines Agency (EMA). Archived from the original on 27 April 2022. Retrieved 2 October 2014.
- PMID 17636779.
- Pediatr Infect Dis J;22(12): 1093–96; discussion 1096–98.
- ISBN 978-0-435-54057-9.
- ^ PMC 2065307.
- ^ PMID 21858000.
- ^ ISBN 978-92-4-151341-8.
- PMID 15931293.
- ^ ISBN 978-92-4-156110-5. Archived(PDF) from the original on 25 May 2021. Retrieved 5 November 2013.
- ^ a b "Instructions for smallpox vaccination with bifurcated needle". World Health Organization (WHO). 1968. Archived from the original on 16 March 2022. Retrieved 3 July 2022.
- ^ "Six bifurcated needles for smallpox vaccination | Science Museum Group Collection". Science Museum (London). Archived from the original on 20 May 2022. Retrieved 3 July 2022.
The skin was not disinfected before use as this killed the vaccine.
- ^ (PDF) from the original on 22 March 2022. Retrieved 11 August 2022.
- PMID 15120802.
- PMID 16933957.
- PMC 1626554.
- PMID 19970016.
- ^ Council on Drugs (American Medical Association) (1964). New and Nonofficial Drugs. Lippincott. p. 739.
- PMID 17074424.
- PMID 17964011.
- PMID 15491873.
- PMID 20531961.
- PMID 28057259.
- S2CID 46979748.
- ^ PMID 17052815.
- ^ Cohen J (1 July 2022). "There's a shortage of monkeypox vaccine. Could one dose instead of two suffice?". AAAS. Archived from the original on 8 July 2022. Retrieved 3 July 2022.
Because MVA does not make copies of itself, the team gave it at a higher dose—similar to what's used in the Bavarian Nordic shot today—than the Dryvax vaccine.
- PMID 18678911.
- ^ "Smallpox Vaccine Supply & Strength". National Institute of Allergy and Infectious Diseases (NIAID). 26 September 2019. Archived from the original on 17 October 2019. Retrieved 16 October 2019.
- PMID 27327616.
- ^ "Summary Basis for Regulatory Action Template". FDA. U.S. Food & Drug Administration. Archived from the original on 8 October 2021. Retrieved 8 October 2021.
- ^ "Vaccine "Take" Evaluation". CDC. U.S. Centers for Disease Control and Prevention. Archived from the original on 26 January 2022. Retrieved 9 January 2022.
- ^ CDC (13 October 2022). "Monkeypox in the U.S." Centers for Disease Control and Prevention. Archived from the original on 19 October 2022. Retrieved 19 October 2022.
- ^ "Smallpox and monkeypox vaccine: Canadian Immunization Guide". Public Health Agency of Canada. 16 June 2022. Archived from the original on 20 July 2020. Retrieved 8 July 2022.
- ^ "Register of Innovative Drugs" (PDF). Health Canada. June 2020. Archived (PDF) from the original on 26 June 2020. Retrieved 24 June 2020.
- ^ "Products for Human Use. Submission #144762". Register of Innovative Drugs. Health Canada. Archived from the original on 17 June 2014. Retrieved 30 October 2014.
- ^ "Jynneos". U.S. Food and Drug Administration (FDA). 24 September 2019. STN 125678. Archived from the original on 17 October 2019. Retrieved 16 October 2019.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "FDA approves first live, non-replicating vaccine to prevent smallpox and monkeypox". U.S. Food and Drug Administration (FDA) (Press release). 24 September 2019. Archived from the original on 17 October 2019. Retrieved 17 October 2019.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "Infectious Diseases: Clinical Trials". Bavarian Nordic. Archived from the original on 26 April 2016. Retrieved 30 October 2014.
- U.S. National Institutes of Health. Archivedfrom the original on 13 March 2022. Retrieved 30 October 2014.
- PMID 31722150.
- ^ "Jynneos Vaccine Effectiveness". Centers for Disease Control and Prevention. 19 May 2023. Archived from the original on 24 May 2023. Retrieved 24 May 2023.
- ^ "Considerations on posology for the use of the vaccine Jynneos/ Imvanex (MVA-BN) against monkeypox" (PDF). European Medicines Agency. 19 August 2022. Archived (PDF) from the original on 28 May 2023. Retrieved 28 May 2023.
- ^ "Protecting you from mpox (monkeypox): information on the smallpox vaccination". GOV.UK. Archived from the original on 28 May 2023. Retrieved 28 May 2023.
- (PDF) from the original on 13 October 2021. Retrieved 13 June 2022.
- ^ "Prevention and Treatment". U.S. Centers for Disease Control and Prevention (CDC). 18 October 2021. Archived from the original on 15 December 2017. Retrieved 11 August 2022.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "Vaccines and Related Biological Products Advisory Committee Meeting". U.S. Food and Drug Administration (FDA). 17 May 2007. Archived from the original on 20 October 2017. Retrieved 2 May 2013.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ a b c d Kneip A (26 January 2003). "Pocken-Fieber". Der Spiegel (in German). Archived from the original on 4 July 2022. Retrieved 4 July 2022.
- ^ Lueck S (1 April 2002). "Aventis to Donate Smallpox Vaccine To the U.S. Government's Stockpile". The Wall Street Journal. Archived from the original on 12 January 2018. Retrieved 4 July 2022.
- ^ Emergent BioSolutions (3 September 2019). "Emergent BioSolutions Awarded 10-Year HHS Contract to Deliver ACAM2000®, (Smallpox (Vaccinia) Vaccine, Live) Into the Strategic" (Press release). Retrieved 4 July 2022.
- ^ Bavarian Nordic. "Bavarian Nordic Announces U.S. FDA Approval of Jynneos (Smallpox and Monkeypox Vaccine, Live, Non-Replicating) for Prevention of Smallpox and Monkeypox Disease in Adults" (Press release). Archived from the original on 28 June 2022. Retrieved 4 July 2022.
- ^ a b c U.S. Department of Health and Human Services (1 July 2022). "HHS Orders 2.5 Million More Doses of JYNNEOS Vaccine For Monkeypox Preparedness" (Press release). Archived from the original on 4 July 2022. Retrieved 4 July 2022.
- (PDF) from the original on 19 January 2022. Retrieved 11 August 2022.
- ^ PMID 15353533.
- ^ Costa A (5–7 November 2013). "Smallpox vaccine stockpile" (PDF). World Health Organization (WHO). Archived (PDF) from the original on 4 July 2022. Retrieved 4 July 2022.
- ^ "Smallpox eradication: destruction of variola virus stocks" (PDF). 4 April 2019. Archived (PDF) from the original on 16 May 2022. Retrieved 4 July 2022.
- ^ "Plan national de réponse à une menace de variole" (PDF). Ministère de la Santé et des Solidarités (France). August 2006. Archived (PDF) from the original on 19 May 2022. Retrieved 4 July 2022.
- ^ "Vaiolo delle scimmie, 'abbiamo 5 milioni dosi di vaccino: pronti se servirà'" (in Italian). adnkronos. 27 May 2022. Archived from the original on 14 July 2022. Retrieved 14 July 2022.
- ^ Jihyun Kim (23 May 2022). "15개국 퍼진 원숭이 두창, 불안 확산…백신·치료제는?". Newsis. Seoul. Archived from the original on 23 May 2022. Retrieved 23 May 2022.
- PMID 23596574.
- ISBN 978-0-8385-8529-0.
- ^ PMID 16200144.
- ISBN 978-0-906026-36-6.
- ^ Needham J (1999). "Part 6, Medicine". Science and Civilization in China: Volume 6, Biology and Biological Technology. Cambridge: Cambridge University Press. p. 134.
- ISBN 978-0-671-62028-8.
- ISBN 9780080919461. Archivedfrom the original on 3 August 2020. Retrieved 6 July 2017..
- ^ Voltaire (1742). "Letter XI". Letters on the English. Archived from the original on 16 October 2018. Retrieved 6 July 2017.
- ^ PMID 6319980.
- ^ Aboul-Enein BH, Ross MW, Aboul-Enein FH (2012). "Smallpox inoculation and the Ottoman contribution: A Brief Historiography" (PDF). Texas Public Health Journal. 64 (1): 12. Archived (PDF) from the original on 11 October 2021. Retrieved 23 December 2018.
- ^ Livingstone, N. 2015. The Mistresses of Cliveden. Three centuries of scandal, power and intrigue (p. 229)
- ^ Kennedy P (1715). An Essay on External Remedies Wherein it is Considered, Whether all the curable Distempers incident to Human Bodies, may not be cured by Outward Means. London: A. Bell.
- ^ Willoughby B (12 February 2004). "Black History Month II: Why Wasn't I Taught That?". Tolerance in the News. Archived from the original on 14 January 2009. Retrieved 4 December 2008.
- ^ "Open Collections Program: Contagion, The Boston Smallpox Epidemic, 1721". Archived from the original on 26 July 2018. Retrieved 27 August 2008.
- ISBN 978-0-517-51577-8.
- ^ "Montagu, Turkish Embassy Letters". Archived from the original on 15 April 2013. Retrieved 4 December 2008.
- ^ "Statue of Dr Edward Jenner near the Italian Fountains, Kensington Gardens". lachlan.bluehaze.com.au. Archived from the original on 28 March 2006. Retrieved 16 October 2019.
- S2CID 8169180. Archived from the original(PDF) on 27 September 2007.
- ^ Pearson G, ed. (1798). An inquiry concerning the history of the cowpox, principally with a view to supersede and extinguish the smallpox. London, England: J. Johnson. pp. 102–104. Archived from the original on 25 January 2022. Retrieved 31 December 2015.
- PMID 26181536.
- ^ Michael J. Bennett, War against Smallpox: Edward Jenner and the Global Spread of Vaccination (Cambridge, United Kingdom: Cambridge University Press, 2020), 32.
- ^ S2CID 30318738.
- PMID 390826.
- PMID 10885136.
- PMID 1289108./
- S2CID 43179073.
- ^ PMID 9987167.
- ^ ISBN 978-0-9528695-1-1.
- ^ ISBN 0-435-54057-2.
- ^ Piercey T (August 2002). "Plaque in Memory of Rev. John Clinch". Archived from the original on 20 March 2018. Retrieved 28 May 2014.
- ISBN 978-098100170-8.
- ^ "First X, Then Y, Now Z : Landmark Thematic Maps – Medicine". Princeton University Library. 2012. Archived from the original on 13 September 2018. Retrieved 22 May 2018.
- ^ Morman ET (2006). "Smallpox". In Finkelman P (ed.). Encyclopedia of the New American Nation. Charles Scribner's Sons. pp. 207–08.
- ^ ISBN 978-0-226-35168-1.
- ^ ISBN 978-0-12-083475-4.
- S2CID 24344691.
- JSTOR 1006158.
- from the original on 8 July 2022. Retrieved 26 June 2022.
- ^ Tizard IR (2023). A History of Vaccines and Their Opponents. Elsevier. p. 99.
- PMID 20762710.
- S2CID 23282373.
- doi:10.25646/1620.
- ^ Jarlert A (2001). Sveriges Kyrkohistoria. Vol. 6. Stockholm. pp. 33–54.
{{cite book}}: CS1 maint: location missing publisher (link) - ^ Rheinberger R (1976). "Zum 200. Geburtstag von Landesphysikus Gebhard Schaedler. Ein Liechtensteinischer Artzt als Pionier der Pockenschutzimpfung.". Jahrbuch des Historischen Vereins fur das Furstentum Liechtenstein. Historischer Verein fur das Furstentum Liechtenstein. Vol. 76. pp. 337–343. Archived from the original on 27 October 2021. Retrieved 27 October 2021.
- S2CID 4254402.
- PMID 17338405.
- ^ ISBN 978-0-230-27471-6.
- ^ ISBN 9781846310867.
- ^ Durbach N (2002). "Class, Gender, and the Conscientious Objector to Vaccination, 1898-1907". Journal of British Studies. 41 (1): 58–83 – via JSTOR.
- PMID 12993980.
- ^ "Toward a Twenty-First-Century Jacobson v. Massachusetts" (PDF). Harvard Law Review. 121 (7). The Harvard Law Review Association: 1823–1824. May 2008. Archived (PDF) from the original on 26 October 2014. Retrieved 13 March 2014.
- ^ "A Brief Biography of Dr. Louis T. Wright". North by South: from Charleston to Harlem, the great migration. Archived from the original on 20 October 2017. Retrieved 23 September 2006.
- ^ "Spotlight on Black Inventors, Scientists, and Engineers". Department of Computer Science of Georgetown University. Archived from the original on 7 September 2006. Retrieved 23 September 2006.
- ^ PMID 20757828.
- ^ PMID 20789814.
- ^ Creighton C (1887). The Natural History of Cowpox and Vaccinal Syphilis. London: Cassell.
- ^ Copeman SM (1892). "The Bacteriology of Vaccine Lymph". In Shelley CE (ed.). Transactions of the Seventh International Congress of Hygiene and Demography. Eyre and Spottiswoode. pp. 319–26. Retrieved 14 January 2014.
- S2CID 8918951.
- ^ Dixon CW (1962). Smallpox. London: J. & A. Churchill. pp. 280–81.
- .
- PMID 14367805.
- ^ "Professor Leslie Collier". The Telegraph. 22 March 2011. Archived from the original on 12 January 2022. Retrieved 2 May 2013.
- PMID 24965243.
- ISBN 978-0-930405-86-1.
- ^ PMID 7376638.
- ISBN 978-1-59102-722-5.
- ^ "Smallpox > Bioterrorism". U.S. Centers for Disease Control and Prevention (CDC). 19 December 2016. Archived from the original on 19 May 2022. Retrieved 21 May 2022.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- PMID 12824210.
- ISBN 0-309-54877-2. Archivedfrom the original on 14 March 2022. Retrieved 21 August 2022.
- ^ Mackenzie D (22 August 2003). "US smallpox vaccination plan grinds to a halt". New Scientist. Archived from the original on 7 February 2022. Retrieved 1 September 2019.
- ^ Public Services and Procurement Canada (21 April 2022). "Third Generation Smallpox Vaccine (6D024-215700/A)". Government of Canada. Archived from the original on 20 June 2022. Retrieved 20 June 2022.
- ^ Osman L (20 May 2022). "Canada considering smallpox vaccine for monkeypox cases, says Dr. Theresa Tam". CTV News. Archived from the original on 20 June 2022. Retrieved 20 June 2022.
- ^ Public Health Agency of Canada (24 May 2022). "Statement from the Minister of Health on Canada's Response to Monkeypox". Government of Canada. Archived from the original on 11 June 2022. Retrieved 26 May 2022.
- hdl:1828/7374.
- ISBN 978-1-68367-033-9. Archivedfrom the original on 8 July 2022. Retrieved 13 June 2022.
- ^ Jenner E (1798). An Inquiry into the Causes and Effects of the Variolæ Vaccinæ. London: Self-published. Archived from the original on 11 July 2022. Retrieved 11 July 2022.
- PMID 29137821.
- PMC 2155820.
- PMID 9782308.
- ^ ICTV Taxonomy history: Cowpox virus. 14 April 2021. Archived from the original on 15 April 2021. Retrieved 15 April 2021.
Varidnaviria > Bamfordvirae > Nucleocytoviricota > Pokkesviricetes > Chitovirales > Poxviridae > Chordopoxvirinae > Orthopoxvirus > Cowpox virus
- PMID 16940536.
- S2CID 36975171.
- ^ PMID 32684155.
- PMID 29020595.
- from the original on 21 May 2020. Retrieved 13 June 2022.
- ^ PMID 33272280.
- ^ Transactions of the International medical congress, seventh session, held in London, August 2d to 9th, 1881. J. W. Kolckmann. 1881. Archived from the original on 23 May 2022. Retrieved 23 May 2022.
- PMID 32473878.
To honor Jenner, in 1881 Louis Pasteur proposed at the 7th International Congress of Medicine held in London, to generalize the term "vaccination" to refer to all protective immunization procedures against any infectious diseases [19] and since then we talk about vaccines against different diseases.
- PMID 9933209.
Unjustified credit is sometimes given to Jenner for introducing the terms virus (already long used to indicate a transmissible poison) and vaccination (introduced by his friend Richard Dunning in 1800.
External links
- Smallpox US Centers for Disease Control and Prevention
- Smallpox Center for Infectious Disease Research and Policy
- "Smallpox/Monkeypox Vaccine Information Statement". U.S. Centers for Disease Control and Prevention (CDC). November 2022.
- "Interim Clinical Considerations for Use of JYNNEOS and ACAM2000 Vaccines during the 2022 U.S. Mpox Outbreak". U.S. Centers for Disease Control and Prevention (CDC). 2 August 2023. Retrieved 3 September 2023.</ref>
- "Medication Guide Smallpox (Vaccinia) Vaccine, Live ACAM2000" (PDF). Emergent Biosolutions.
