Telangiectasia
| Telangiectasia | |
|---|---|
| Other names | Spider veins, angioectasias |
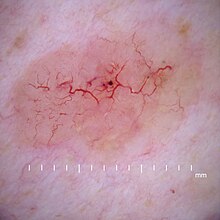 | |
| Telangiectasia as seen in a basal-cell carcinoma | |
| Pronunciation | |
| Specialty | Dermatology |
Telangiectasias, from Greek: tel- (end) + angi- (blood or lymph vessel) + ectasia (the expansion of a hollow or tubular organ), also known as spider veins, are small dilated
Many patients with spider veins seek the assistance of physicians who specialize in vein care or peripheral vascular disease. These physicians are called
Some telangiectasias are due to developmental abnormalities that can closely mimic the behaviour of
Telangiectasias, aside from presenting in many other conditions, are one of the features of the acronymically named
Causes
The causes of telangiectasia can be divided into
Genetic
Goldman states that "numerous inherited or congenital conditions display cutaneous telangiectasia".[2] These include:
- Bloom syndrome (homozygous null mutation in BLM DNA repair enzyme. similar mechanism and etiology to ataxia telangiectasia)
- Naevus flammeus(port-wine stain)
- Klippel–Trenaunay syndrome
- hemangiomas)
- Hereditary hemorrhagic telangiectasia (Osler–Weber–Rendu syndrome)
- Ataxia–telangiectasia
- intellectual disabilities
- Hypotrichosis–lymphedema–telangiectasia syndrome, caused by mutation in transcription factor SOX18[3]
Venous hypertension
In the past, it was believed that leg varicose veins or telangiectasia were caused by high venous pressure or "venous hypertension". However it is now understood that venous reflux disease is usually the cause of these problems.[4][full citation needed]
Telangiectasia in the legs is often related to the presence of venous reflux within underlying varicose veins. Flow abnormalities in smaller veins known as reticular veins or feeder veins under the skin can also cause spider veins to form, thereby making a recurrence of spider veins in the treated area less likely.
Factors that predispose to the development of
- Age
- Sex: It used to be thought that females were affected far more than males. However, research has shown 79% of adult males and 88% of adult females have leg telangiectasia.[5]
- Pregnancy: Pregnancy is a key factor contributing to the formation of varicose and spider veins. Changes in hormone levels are one of the most important reasons women are more likely to develop varicose veins during pregnancy. There is an increase in progesterone, which causes the veins to relax and potentially swell more easily.[6] There's also a significant increase in the blood volume during pregnancy, which tends to distend veins, causing valve dysfunction which leads to blood pooling in the veins. Moreover, later in pregnancy, the enlarged uterus can compress veins, causing higher vein pressure leading to dilated veins. Varicose veins that form during pregnancy may spontaneously improve or even disappear a few months after delivery.[7]
- Lifestyle/occupation: Those who are involved with prolonged sitting or standing in their daily activities have an increased risk of developing varicose veins. The weight of the blood continuously pressing against the closed valves causes them to fail, leading to vein distention.[8]
Other acquired causes
Acquired telangiectasia, not related to other venous abnormalities, for example on the face and trunk, can be caused by factors such as
- Cushing's syndrome
- Rosacea
- Blepharitis[9]
- Environmental damage such as that caused by sun[10] or cold exposure
- Age[10]
- Trauma to skin such as contusions or surgical incisions.
- Radiation exposure such as that experienced during radiotherapy for the treatment of cancer, e.g., radiation proctitis
- Chemotherapy
- Carcinoid syndrome
- Limited systemic sclerosis/scleroderma (a scleroderma sub-type)
- Chronic treatment with topical corticosteroids may lead to telangiectasia.[11]
- pregnant women and in patients with hepatic cirrhosis and are associated with palmar erythema. In men, they are related to high estrogen levels secondary to liver disease.
- TEMPI syndrome
- Tobacco smoking[10]
- Cutaneous collagenous vasculopathy
Treatment
Before any treatment of leg telangiectasia is considered, it is essential to have
Sclerotherapy is the "gold standard" and is preferred over laser for eliminating telangiectasiae and smaller varicose leg veins.[15] A sclerosant medication is injected into the diseased vein so it hardens and eventually shrinks away. Recent evidence with foam sclerotherapy shows that the foam containing the irritating sclerosant quickly appears in the patient's heart and lungs, and then in some cases travels through a patent foramen ovale to the brain.[16] This has led to concerns about the safety of sclerotherapy for telangiectasias.
In some cases
Telangiectasias on the face are often treated with a laser. Laser therapy uses a light beam that is pulsed onto the veins in order to seal them off, causing them to dissolve. These light-based treatments require adequate heating of the veins. These treatments can result in the destruction of
References
- ^ "telangiectasia" at Dorland's Medical Dictionary
- ^ ISBN 0-8151-4011-8.[page needed]
- PMID 12740761.
- ^ Whiteley (2011). "Understanding Venous Reflux – the cause of varicose veins and venous leg ulcers".
- PMID 18848475.
- PMID 27639009.
- PMID 26477632.
- ^ "Varicose veins - Symptoms and causes". Mayo Clinic. Retrieved 2020-08-11.
- PMID 22592706.
- ^ PMID 12648216.
- PMID 10821151.
- S2CID 29067831.
- PMID 8408914.
- PMID 8408913.
- ISBN 978-0-12-369515-4.
- PMID 18385510.
- PMID 16414404.
- ^ Duffy, David M. (2012). "Sclerotherapy for Telangiectasia – The impact of small changes in vessel size on treatment outcomes" (PDF). Cosmetic Dermatology. 25 (3): 126–33. Archived from the original (PDF) on 2019-12-15.
- ^ Treatment of Leg Veins. Procedures in Cosmetic Dermatology Series. Editors Murad Alam, Sirunya Silapunt. Second Edition Saunders Elsevier Inc. 2011[page needed]
- S2CID 36994668.
- PMID 3305603.
