Thymus
| Thymus | |
|---|---|
 Position of the thymus | |
| Details | |
| Precursor | Third pharyngeal pouch |
| System | Lymphatic system, part of the immune system |
| Lymph | tracheobronchial, parasternal |
| Function | Support the development of functional T cells |
| Identifiers | |
| Latin | thymus |
| MeSH | D013950 |
| TA98 | A13.1.02.001 |
| TA2 | 5152 |
| FMA | 9607 |
| Anatomical terminology | |
The thymus (pl.: thymuses or thymi) is a specialized primary lymphoid organ of the immune system. Within the thymus, thymus cell lymphocytes or T cells mature. T cells are critical to the adaptive immune system, where the body adapts to specific foreign invaders. The thymus is located in the upper front part of the chest, in the anterior superior mediastinum, behind the sternum, and in front of the heart. It is made up of two lobes, each consisting of a central medulla and an outer cortex, surrounded by a capsule.
The thymus is made up of immature
Abnormalities of the thymus can result in a decreased number of T cells and autoimmune diseases such as
Structure
The thymus is an organ that sits behind the
The thymus is located in the
Microanatomy
The thymus consists of two lobes, merged in the middle, surrounded by a capsule that extends with blood vessels into the interior.[2] The lobes consist of an outer cortex rich with cells and an inner less dense medulla.[4] The lobes are divided into smaller lobules 0.5-2 mm diameter, between which extrude radiating insertions from the capsule along septa.[1]
The cortex is mainly made up of
In the medulla, the network of epithelial cells is coarser than in the cortex, and the lymphoid cells are relatively fewer in number.
-
Micrograph showing a lobule of the thymus. The cortex (deeper purple area) surrounds a less dense and lighter medulla.
-
Micrograph showing a Hassall's corpuscle, found within the medulla of the thymus.
Blood and nerve supply
The arteries supplying the thymus are branches of the internal thoracic, and inferior thyroid arteries, with branches from the superior thyroid artery sometimes seen.[2] The branches reach the thymus and travel with the septa of the capsule into the area between the cortex and medulla, where they enter the thymus itself; or alternatively directly enter the capsule.[2]
The
Lymphatic vessels travel only away from the thymus, accompanying the arteries and veins. These drain into the brachiocephalic, tracheobronchial and parasternal lymph nodes.[2]
The
Variation
The two lobes differ slightly in size, with the left lobe usually higher than the right. Thymic tissue may be found scattered on or around the gland, and occasionally within the thyroid.[2] The thymus in children stretches variably upwards, at times to as high as the thyroid gland.[2]
Development

The thymocytes and the epithelium of the thymus have different developmental origins.[4] The epithelium of the thymus develops first, appearing as two outgrowths, one on either side, of the third pharyngeal pouch.[4] It sometimes also involves the fourth pharyngeal pouch.[3] These extend outward and backward into the surrounding mesoderm and neural crest-derived mesenchyme in front of the ventral aorta. Here the thymocytes and epithelium meet and join with connective tissue. The pharyngeal opening of each diverticulum is soon obliterated, but the neck of the flask persists for some time as a cellular cord. By further proliferation of the cells lining the flask, buds of cells are formed, which become surrounded and isolated by the invading mesoderm.[7]
The epithelium forms fine lobules, and develops into a sponge-like structure. During this stage,
Involution
The thymus continues to grow after birth reaching the relative maximum size by puberty.
The atrophy is due to the increased circulating level of
Function
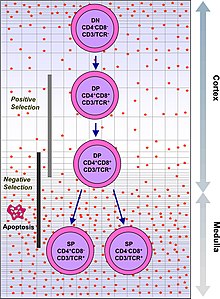
T cell maturation
The thymus facilitates the maturation of T cells, an important part of the immune system providing cell-mediated immunity.[11] T cells begin as hematopoietic precursors from the bone-marrow, and migrate to the thymus, where they are referred to as thymocytes. In the thymus they undergo a process of maturation, which involves ensuring the cells react against antigens ("positive selection"), but that they do not react against antigens found on body tissue ("negative selection").[11] Once mature, T cells emigrate from the thymus to provide vital functions in the immune system.[11][12]
Each T cell has a distinct
Positive selection
T cells have distinct T cell receptors. These distinct receptors are formed by process of V(D)J recombination gene rearrangement stimulated by RAG1 and RAG2 genes.[13] This process is error-prone, and some thymocytes fail to make functional T-cell receptors, whereas other thymocytes make T-cell receptors that are autoreactive.[14] If a functional T cell receptor is formed, the thymocyte will begin to express simultaneously the cell surface proteins CD4 and CD8.[13]
The survival and nature of the T cell then depends on its interaction with surrounding thymic epithelial cells. Here, the T cell receptor interacts with the MHC molecules on the surface of epithelial cells.[13] A T cell with a receptor that doesn't react, or reacts weakly will die by apoptosis. A T cell that does react will survive and proliferate.[13] A mature T cell expresses only CD4 or CD8, but not both.[12] This depends on the strength of binding between the TCR and MHC class 1 or class 2.[13] A T cell receptor that binds mostly to MHC class I tends to produce a mature "cytotoxic" CD8 positive T cell; a T cell receptor that binds mostly to MHC class II tends to produce a CD4 positive T cell.[14]
Negative selection
T cells that attack the body's own proteins are eliminated in the thymus, called "negative selection".
Clinical significance
Immunodeficiency
As the thymus is where T cells develop, congenital problems with the development of the thymus can lead to
The most common congenital cause of thymus-related immune deficiency results from the deletion of the
Autoimmune disease
Autoimmune polyendocrine syndrome
Thymoma-associated multiorgan autoimmunity
Myasthenia gravis
Cancer
Thymomas
Tumours originating from the thymic epithelial cells are called
Thymomas can be benign; benign but by virtue of expansion, invading beyond the capsule of the thymus ("invasive thymoma"), or malignant (a carcinoma).[3] This classification is based on the appearance of the cells.[3] A WHO classification also exists but is not used as part of standard clinical practice.[3] Benign tumours confined to the thymus are most common; followed by locally invasive tumours, and then by carcinomas.[3] There is variation in reporting, with some sources reporting malignant tumours as more common.[22] Invasive tumours, although not technically malignant, can still spread (metastasise) to other areas of the body.[3] Even though thymomas occur of epithelial cells, they can also contain thymocytes.[3] Treatment of thymomas often requires surgery to remove the entire thymus.[22] This may also result in temporary remission of any associated autoimmune conditions.[22]
Lymphomas
Tumours originating from T cells of the thymus form a subset of
Tumours originating from the small population of B cells present in the thymus lead to
Thymic cysts
The thymus may contain cysts, usually less than 4 cm in diameter. Thymic cysts are usually detected incidentally and do not generally cause symptoms.
Surgical removal
Removal of the thymus in infancy results in often fatal immunodeficiency, because functional T cells have not developed.[2][28] In older children and adults, which have a functioning lymphatic system with mature T cells also situated in other lymphoid organs, the effect is reduced, but includes failure to mount immune responses against new antigens,[2] an increase in cancers, and an increase in all-cause mortality.[29]
Society and culture
When used as food for humans, the thymus of animals is known as one of the kinds of sweetbread.[30]
History
The thymus was known to the
Galen was the first to note that the size of the organ changed over the duration of a person's life.[33]
In the nineteenth century, a condition was identified as status thymicolymphaticus defined by an increase in lymphoid tissue and an enlarged thymus. It was thought to be a cause of
The importance of the thymus in the immune system was discovered in 1961 by Jacques Miller, by surgically removing the thymus from one-day-old mice, and observing the subsequent deficiency in a lymphocyte population, subsequently named T cells after the organ of their origin.[35][36] Until the discovery of its immunological role, the thymus had been dismissed as a "evolutionary accident", without functional importance.[14] The role the thymus played in ensuring mature T cells tolerated the tissues of the body was uncovered in 1962, with the finding that T cells of a transplanted thymus in mice demonstrated tolerance towards tissues of the donor mouse.[14] B cells and T cells were identified as different types of lymphocytes in 1968, and the fact that T cells required maturation in the thymus was understood.[14] The subtypes of T cells (CD8 and CD4) were identified by 1975.[14] The way that these subclasses of T cells matured – positive selection of cells that functionally bound to MHC receptors – was known by the 1990s.[14] The important role of the AIRE gene, and the role of negative selection in preventing autoreactive T cells from maturing, was understood by 1994.[14]
Recently, advances in immunology have allowed the function of the thymus in T-cell maturation to be more fully understood.[14]
Other animals
The thymus is present in all
The thymus is also present in most other vertebrates with similar structure and function as the human thymus. A second thymus in the neck has been reported sometimes to occur in the mouse[39] As in humans, the guinea pig's thymus naturally atrophies as the animal reaches adulthood,[40] but the athymic hairless guinea pig (which arose from a spontaneous laboratory mutation) possesses no thymic tissue whatsoever, and the organ cavity is replaced with cystic spaces.[41]
Additional images
-
Explanation of the thymus's function
-
Thymus of a fetus
-
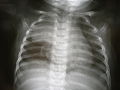
Onchest X-ray, the thymus appears as a radiodense(brighter in this image) mass by the upper lobe of the child's right (left in image) lung.
References
![]() This article incorporates text in the public domain from page 1273 of the 20th edition of Gray's Anatomy (1918)
This article incorporates text in the public domain from page 1273 of the 20th edition of Gray's Anatomy (1918)
- ^ ISBN 978-0-8089-2371-8.
- ^ )
- ^ ISBN 9780323296397.
- ^ ISBN 9780702047473.
- PMID 20228326.
- ISBN 978-0-443-06583-5.
- UB, and UF) qblood/lymphat03
- PMID 19647627.
- ^ a b Davidson's 2018, p. 67.
- PMID 16081852.
- ^ ISBN 978-1-4557-7016-8.
- ^ ISBN 9780323296397.
- ^ ISBN 9780323482554.
- ^ S2CID 21191923.
- ^ a b c Harrison's 2015, pp. 2493.
- ^ a b c d e f g Davidson's 2018, pp. 79–80.
- ISBN 978-0-08-046908-9.
- ^ a b c d Harrison's 2015, pp. 2756–7.
- PMID 17433850.
- ^ a b c d e f Davidson's 2018, pp. 1141–43.
- ^ PMID 20859116.
- ^ a b c d Harrison's 2015, pp. 2759.
- ^ ISBN 978-0071833004.
- PMID 24952250.
- ^ ISBN 978-0071833004.
- ^ S2CID 33986973.
- ^ PMID 15086401.
- PMID 18178293.
- S2CID 260377788.
- ^ "Sweetbread recipes – BBC Food". BBC Food. Retrieved 2019-12-12.
- ^ Liddell HG, Scott R. "θυμός". A Greek-English Lexicon. Retrieved 2019-12-10.
- ^ "thymus | Origin and meaning of thymus by Online Etymology Dictionary". www.etymonline.com. Retrieved 2019-12-10.
- PMID 16549602.
- ISBN 978-0805073690.
- S2CID 12108587.
- PMID 15140026.
- S2CID 4417477.
- JSTOR 3882269.
- S2CID 24553384.
- ISBN 978-0-12-380920-9.
- ISBN 978-1-4757-0325-2.
Books
- Ralston SH, Penman ID, Strachan MW, Hobson RP, eds. (2018). Davidson's principles and practice of medicine (23rd ed.). Elsevier. ISBN 978-0-7020-7028-0.
- Kasper D, Fauci A, Hauser S, Longo D, Jameson J, Loscalzo J (2015). Harrison's Principles of Internal Medicine (19th ed.). McGraw-Hill Professional. ISBN 9780071802154.
External links
- T cell development in the thymus. Video by Janice Yau, describing stromal signaling and tolerance. Department of Immunology and Biomedical Communications, University of Toronto. Master's Research Project, Master of Science in Biomedical Communications. 2011.