Traumatic brain injury
| Traumatic brain injury | |
|---|---|
| Other names | Intracranial injury, physically induced brain injury speech therapy |
A traumatic brain injury (TBI), also known as an intracranial injury, is an
Causes include
Prevention measures include use of
TBI is a major cause of death and disability worldwide, especially in children and young adults.[8] Males sustain traumatic brain injuries around twice as often as females.[9] The 20th century saw developments in diagnosis and treatment that decreased death rates and improved outcomes.
Classification
Traumatic brain injury is defined as damage to the brain resulting from external mechanical force, such as rapid acceleration or deceleration, impact, blast waves, or penetration by a projectile.[10] Brain function is temporarily or permanently impaired and structural damage may or may not be detectable with current technology.[11]
TBI is one of two subsets of acquired brain injury (brain damage that occur after birth); the other subset is non-traumatic brain injury, which does not involve external mechanical force (examples include stroke and infection).[12][13] All traumatic brain injuries are head injuries, but the latter term may also refer to injury to other parts of the head;[14][15][16] however, the terms head injury and brain injury are often used interchangeably.[17] Similarly, brain injuries fall under the classification of central nervous system injuries[18] and neurotrauma.[19] In neuropsychology research literature, in general the term "traumatic brain injury" is used to refer to non-penetrating traumatic brain injuries.
TBI is usually classified based on severity, anatomical features of the injury, and the mechanism (the causative forces).
Severity
| GCS | PTA | LOC
| |
|---|---|---|---|
| Mild | 13–15 | <1 day |
0–30 minutes |
| Moderate | 9–12 | >1 to <7 days |
>30 min to <24 hours |
| Severe | 3–8 | >7 days | >24 hours |
Brain injuries can be classified into
Pathological features
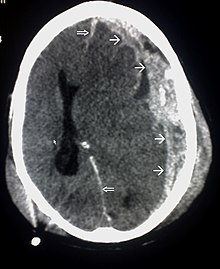
Systems also exist to classify TBI by its pathological features.[20] Lesions can be extra-axial, (occurring within the skull but outside of the brain) or intra-axial (occurring within the brain tissue).[24] Damage from TBI can be focal or diffuse, confined to specific areas or distributed in a more general manner, respectively;[25] however, it is common for both types of injury to exist in a given case.[25]
Diffuse injury manifests with little apparent damage in neuroimaging studies, but lesions can be seen with microscopy techniques
Focal injuries often produce
One type of focal injury, cerebral laceration, occurs when the tissue is cut or torn.[37] Such tearing is common in orbitofrontal cortex in particular, because of bony protrusions on the interior skull ridge above the eyes.[31] In a similar injury, cerebral contusion (bruising of brain tissue), blood is mixed among tissue.[23] In contrast, intracranial hemorrhage involves bleeding that is not mixed with tissue.[37]
Hematomas, also focal lesions, are collections of blood in or around the brain that can result from hemorrhage.[11] Intracerebral hemorrhage, with bleeding in the brain tissue itself, is an intra-axial lesion. Extra-axial lesions include epidural hematoma, subdural hematoma, subarachnoid hemorrhage, and intraventricular hemorrhage.[38] Epidural hematoma involves bleeding into the area between the skull and the dura mater, the outermost of the three membranes surrounding the brain.[11] In subdural hematoma, bleeding occurs between the dura and the arachnoid mater.[23] Subarachnoid hemorrhage involves bleeding into the space between the arachnoid membrane and the pia mater.[23] Intraventricular hemorrhage occurs when there is bleeding in the ventricles.[38]
Signs and symptoms
Symptoms are dependent on the type of TBI (diffuse or focal) and the part of the brain that is affected.[40] Unconsciousness tends to last longer for people with injuries on the left side of the brain than for those with injuries on the right.[15] Symptoms are also dependent on the injury's severity. With mild TBI, the patient may remain conscious or may lose consciousness for a few seconds or minutes.[41] Other symptoms of mild TBI include headache, vomiting, nausea, lack of motor coordination, dizziness, difficulty balancing,[42] lightheadedness, blurred vision or tired eyes, ringing in the ears, bad taste in the mouth, fatigue or lethargy, and changes in sleep patterns.[41] Cognitive and emotional symptoms include behavioral or mood changes, confusion, and trouble with memory, concentration, attention, or thinking.[41] Mild TBI symptoms may also be present in moderate and severe injuries.[41]
A person with a moderate or severe TBI may have a headache that does not go away, repeated vomiting or nausea, convulsions, an inability to awaken,
When the pressure within the skull (
Small children with moderate to severe TBI may have some of these symptoms but have difficulty communicating them.[52] Other signs seen in young children include persistent crying, inability to be consoled, listlessness, refusal to nurse or eat,[52] and irritability.[11]
Causes
The most common causes of TBI in the U.S. include violence, transportation accidents, construction site mishaps, and sports.[42][53] Motor bikes are major causes, increasing in significance in developing countries as other causes reduce.[54][55] The estimates that between 1.6 and 3.8 million traumatic brain injuries each year are a result of sports and recreation activities in the US.[56] In children aged two to four, falls are the most common cause of TBI, while in older children traffic accidents compete with falls for this position.[57] TBI is the third most common injury to result from child abuse.[58] Abuse causes 19% of cases of pediatric brain trauma, and the death rate is higher among these cases.[59] Although men are twice as likely to have a TBI. Domestic violence is another cause of TBI,[60] as are work-related and industrial accidents.[61] Firearms[15] and blast injuries from explosions[62] are other causes of TBI, which is the leading cause of death and disability in war zones.[63] According to Representative Bill Pascrell (Democrat, NJ), TBI is "the signature injury of the wars in Iraq and Afghanistan."[64] There is a promising technology called activation database-guided EEG biofeedback, which has been documented to return a TBI's auditory memory ability to above the control group's performance[65][66]
Mechanism
Physical forces

The type, direction, intensity, and duration of forces all contribute to the characteristics and severity of TBI.
Even in the absence of an impact, significant acceleration or deceleration of the head can cause TBI; however in most cases, a combination of impact and acceleration is probably to blame.
Damage may occur directly under the site of impact, or it may occur on the side opposite the impact (coup and contrecoup injury, respectively).[67] When a moving object impacts the stationary head, coup injuries are typical,[69] while contrecoup injuries are usually produced when the moving head strikes a stationary object.[70]
Primary and secondary injury

A large percentage of the people killed by brain trauma do not die right away but rather days to weeks after the event;[71] rather than improving after being hospitalized, some 40% of TBI patients deteriorate.[72] Primary brain injury (the damage that occurs at the moment of trauma when tissues and blood vessels are stretched, compressed, and torn) is not adequate to explain this deterioration; rather, it is caused by secondary injury, a complex set of cellular processes and biochemical cascades that occur in the minutes to days following the trauma.[73] These secondary processes can dramatically worsen the damage caused by primary injury[63] and account for the greatest number of TBI deaths occurring in hospitals.[39]
Secondary injury events include damage to the
Diagnosis

Diagnosis is suspected based on lesion circumstances and clinical evidence, most prominently a neurological examination, for example checking whether the pupils constrict normally in response to light and assigning a Glasgow Coma Score.[23] Neuroimaging helps in determining the diagnosis and prognosis and in deciding what treatments to give.[76] DSM-5 can be utilized to diagnose TBI and its psychiatric sequelae.[77][78][79]
The preferred radiologic test in the emergency setting is
Magnetic resonance imaging (MRI) can show more detail than CT, and can add information about expected outcome in the long term.[23] It is more useful than CT for detecting injury characteristics such as diffuse axonal injury in the longer term;[10] however, MRI is not used in the emergency setting for reasons including its relative inefficacy in detecting bleeds and fractures, its lengthy acquisition of images, the inaccessibility of the patient in the machine, and its incompatibility with metal items used in emergency care.[23] A variant of MRI since 2012 is high-definition fiber tracking (HDFT).[81]
Other techniques may be used to confirm a particular diagnosis. X-rays are still used for head trauma, but evidence suggests they are not useful; head injuries are either so mild that they do not need imaging or severe enough to merit the more accurate CT.[80] Angiography may be used to detect blood vessel pathology when risk factors such as penetrating head trauma are involved.[10] Functional imaging can measure cerebral blood flow or metabolism, inferring neuronal activity in specific regions and potentially helping to predict outcome.[82]
Prevention


Since a major cause of TBI are vehicle accidents, their prevention or the amelioration of their consequences can both reduce the incidence and gravity of TBI. In accidents, damage can be reduced by use of seat belts, child safety seats[56] and motorcycle helmets,[86] and presence of roll bars and airbags.[37] Education programs exist to lower the number of crashes.[76] In addition, changes to public policy and safety laws can be made; these include speed limits, seat belt and helmet laws, and road engineering practices.[63]
Changes to common practices in sports have also been discussed. An increase in use of helmets could reduce the incidence of TBI.[63] Due to the possibility that repeatedly "heading" a ball practicing soccer could cause cumulative brain injury, the idea of introducing protective headgear for players has been proposed.[87] Improved equipment design can enhance safety; softer baseballs reduce head injury risk.[88] Rules against dangerous types of contact, such as "spear tackling" in American football, when one player tackles another head first, may also reduce head injury rates.[88]
Falls can be avoided by installing grab bars in bathrooms and handrails on stairways; removing tripping hazards such as throw rugs; or installing window guards and safety gates at the top and bottom of stairs around young children.[56] Playgrounds with shock-absorbing surfaces such as mulch or sand also prevent head injuries.[56] Child abuse prevention is another tactic; programs exist to prevent shaken baby syndrome by educating about the dangers of shaking children.[59] Gun safety, including keeping guns unloaded and locked, is another preventative measure.[89] Studies on the effect of laws that aim to control access to guns in the United States have been insufficient to determine their effectiveness preventing number of deaths or injuries.[90]
Treatment
It is important to begin emergency treatment within the so-called "
Acute stage
Neuroimaging is helpful but not flawless in detecting raised ICP.
Hypertonic saline can improve ICP by reducing the amount of cerebral water (swelling), though it is used with caution to avoid electrolyte imbalances or heart failure.[10][100][101] Mannitol, an osmotic diuretic,[10] appears to be as effective as hypertonic saline at reducing ICP;[102][103][100][104] however, some concerns have been raised regarding some of the studies performed.[105][specify] Hyertonic saline is also suitable in children with severe traumatic brain injury.[106]
Diuretics, drugs that increase urine output to reduce excessive fluid in the system, may be used to treat high intracranial pressures, but may cause hypovolemia (insufficient blood volume).[39] Hyperventilation (larger and/or faster breaths) reduces carbon dioxide levels and causes blood vessels to constrict; this decreases blood flow to the brain and reduces ICP,[107] but it potentially causes ischemia[11][39][108] and is, therefore, used only in the short term.[11] Giving corticosteroids is associated with an increased risk of death, and so their routine use is not recommended.[109][110] There is no strong evidence that the following pharmaceutical interventions should be recommended to routinely treat TBI: magnesium, monoaminergic and dopamine agonists, progesterone, aminosteroids, excitatory amino acid reuptake inhibitors, beta-2 antagonists (bronchodilators), haemostatic and antifibrinolytic drugs.[99][111][112][113][114]
Traumatic brain injury may cause a range of serious coincidental complications that include cardiac
Chronic stage
Once medically stable, people may be transferred to a
Pharmacological treatment can help to manage psychiatric or behavioral problems.[127] Medication is also used to control post-traumatic epilepsy; however the preventive use of anti-epileptics is not recommended.[128] In those cases where the person is bedridden due to a reduction of consciousness, has to remain in a wheelchair because of mobility problems, or has any other problem heavily impacting self-caring capacities, caregiving and nursing are critical. The most effective research documented intervention approach is the activation database guided EEG biofeedback approach, which has shown significant improvements in memory abilities of the TBI subject that are far superior than traditional approaches (strategies, computers, medication intervention). Gains of 2.61 standard deviations have been documented. The TBI's auditory memory ability was superior to the control group after the treatment.[65]
Effect on the gait pattern

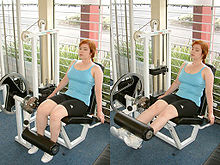
In patients who have developed paralysis of the legs in the form of spastic hemiplegia or diplegia as a result of the traumatic brain injury, various gait patterns can be observed, the exact extent of which can only be described with the help of complex gait analysis systems. In order to facilitate interdisciplinary communication in the interdisciplinary team between those affected, doctors, physiotherapists and orthotists, a simple description of the gait pattern is useful. J. Rodda and H. K. Graham already described in 2001 how gait patterns of CP patients can be more easily recognized and defined gait types which they compared in a classification. They also described that gait patterns can vary with age.[129] Building on this, the Amsterdam Gait Classification was developed at the free university in Amsterdam, the VU medisch centrum. A special feature of this classification is that it makes different gait patterns very recognizable and can be used in patients in whom only one leg and both legs are affected. The Amsterdam Gait Classification was developed for viewing patients with cerebral palsy; however, it can be used just as well in patients with traumatic brain injuries. According to the Amsterdam Gait Classification, five gait types are described. To assess the gait pattern, the patient is viewed visually or via a video recording from the side of the leg to be assessed. At the point in time at which the leg to be viewed is in mid stance and the leg not to be viewed is in mid swing, the knee angle and the contact of the foot with the ground are assessed on the one hand.[130]
Classification of the gait pattern according to the Amsterdam Gait Classification: In gait type 1, the knee angle is normal and the foot contact is complete. In gait type 2, the knee angle is hyperextended and the foot contact is complete. In gait type 3, the knee angle is hyperextended and foot contact is incomplete (only on the forefoot). In gait type 4, the knee angle is bent and foot contact is incomplete (only on the forefoot). With gait type 5, which is also known as crouch gait, the knee angle is bent and the foot contact is complete.[130]
Orthotics

To improve the gait pattern, orthotics can be included in the therapy concept.[131] An Orthosis can support physiotherapeutic treatment in setting the right motor impulses in order to create new cerebral connections.[132] The orthosis must meet the requirements of the medical prescription. In addition, the orthosis must be designed by the orthotist in such a way that it achieves the effectiveness of the necessary levers, matching the gait pattern, in order to support the proprioceptive approaches of physiotherapy. The orthotic concepts of the treatment are based on the concepts for the patients with cerebral palsy. The characteristics of the stiffness of the orthosis shells and the adjustable dynamics in the ankle joint are important elements of the orthosis to be considered.[133]
The orthotic concepts of the treatment are based on the concepts for the patients with cerebral palsy. Due to these requirements, the development of orthoses has changed significantly in recent years, especially since around 2010. At about the same time, care concepts were developed that deal intensively with the orthotic treatment of the lower extremities in cerebral palsy.
Prognosis
Prognosis worsens with the severity of injury.[9] Most TBIs are mild and do not cause permanent or long-term disability; however, all severity levels of TBI have the potential to cause significant, long-lasting disability.[140] Permanent disability is thought to occur in 10% of mild injuries, 66% of moderate injuries, and 100% of severe injuries.[141] Most mild TBI is completely resolved within three weeks. Almost all people with mild TBI are able to live independently and return to the jobs they had before the injury, although a small portion have mild cognitive and social impairments.[89] Over 90% of people with moderate TBI are able to live independently, although some require assistance in areas such as physical abilities, employment, and financial managing.[89] Most people with severe closed head injury either die or recover enough to live independently; middle ground is less common.[10] Coma, as it is closely related to severity, is a strong predictor of poor outcome.[11]
Prognosis differs depending on the severity and location of the lesion, and access to immediate, specialised acute management. Subarachnoid hemorrhage approximately doubles mortality.[142] Subdural hematoma is associated with worse outcome and increased mortality, while people with epidural hematoma are expected to have a good outcome if they receive surgery quickly.[76] Diffuse axonal injury may be associated with coma when severe, and poor outcome.[10] Following the acute stage, prognosis is strongly influenced by the patient's involvement in activity that promote recovery, which for most patients requires access to a specialised, intensive rehabilitation service. The Functional Independence Measure is a way to track progress and degree of independence throughout rehabilitation.[143]
Medical complications are associated with a bad prognosis. Examples of such complications include:
Life satisfaction has been known to decrease for individuals with TBI immediately following the trauma, but evidence has shown that life roles, age, and depressive symptoms influence the trajectory of life satisfaction as time passes.[145] Many people with traumatic brain injuries have poor physical fitness following their acute injury and this may result with difficulties in day-to-day activities and increased levels of fatigue.[146]
Complications

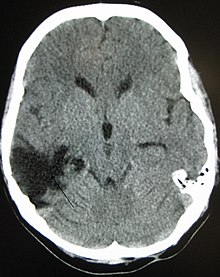
Improvement of neurological function usually occurs for two or more years after the trauma. For many years it was believed that recovery was fastest during the first six months, but there is no evidence to support this. It may be related to services commonly being withdrawn after this period, rather than any physiological limitation to further progress.[10] Children recover better in the immediate time frame and improve for longer periods.[11]
Complications are distinct medical problems that may arise as a result of the TBI. The results of traumatic brain injury vary widely in type and duration; they include physical, cognitive, emotional, and behavioral complications. TBI can cause prolonged or permanent effects on consciousness, such as coma,
Movement disorders that may develop after TBI include tremor,
Hormonal disturbances may occur secondary to hypopituitarism, occurring immediately or years after injury in 10 to 15% of TBI patients. Development of diabetes insipidus or an electrolyte abnormality acutely after injury indicate need for endocrinologic work up. Signs and symptoms of hypopituitarism may develop and be screened for in adults with moderate TBI and in mild TBI with imaging abnormalities. Children with moderate to severe head injury may also develop hypopituitarism. Screening should take place 3 to 6 months, and 12 months after injury, but problems may occur more remotely.[152]
Cognitive deficits that can follow TBI include impaired attention; disrupted insight, judgement, and thought; reduced processing speed; distractibility; and deficits in executive functions such as abstract reasoning, planning, problem-solving, and multitasking.
TBI may cause emotional, social, or behavioral problems and changes in personality.
TBI also has a substantial impact on the functioning of family systems[166] Caregiving family members and TBI survivors often significantly alter their familial roles and responsibilities following injury, creating significant change and strain on a family system. Typical challenges identified by families recovering from TBI include: frustration and impatience with one another, loss of former lives and relationships, difficulty setting reasonable goals, inability to effectively solve problems as a family, increased level of stress and household tension, changes in emotional dynamics, and overwhelming desire to return to pre-injury status. In addition, families may exhibit less effective functioning in areas including coping, problem solving and communication. Psychoeducation and counseling models have been demonstrated to be effective in minimizing family disruption.[167]
Epidemiology

TBI is a leading cause of death and disability around the globe[8] and presents a major worldwide social, economic, and health problem.[10] It is the number one cause of coma,[169] it plays the leading role in disability due to trauma,[76] and is the leading cause of brain damage in children and young adults.[15] In Europe it is responsible for more years of disability than any other cause.[10] It also plays a significant role in half of trauma deaths.[23]
Findings on the frequency of each level of severity vary based on the definitions and methods used in studies. A World Health Organization study estimated that between 70 and 90% of head injuries that receive treatment are mild,[170] and a US study found that moderate and severe injuries each account for 10% of TBIs, with the rest mild.[72]
The incidence of TBI varies by age, gender, region and other factors.[171] Findings of incidence and prevalence in epidemiological studies vary based on such factors as which grades of severity are included, whether deaths are included, whether the study is restricted to hospitalized people, and the study's location.[15] The annual incidence of mild TBI is difficult to determine but may be 100–600 people per 100,000.[63]
Mortality
In the US, the case fatality rate is estimated to be 21% by 30 days after TBI.[94] A study on Iraq War soldiers found that severe TBI carries a mortality of 30–50%.[63] Deaths have declined due to improved treatments and systems for managing trauma in societies wealthy enough to provide modern emergency and neurosurgical services.[116] The fraction of those who die after being hospitalized with TBI fell from almost half in the 1970s to about a quarter at the beginning of the 21st century.[76] This decline in mortality has led to a concomitant increase in the number of people living with disabilities that result from TBI.[172]
Biological, clinical, and demographic factors contribute to the likelihood that an injury will be fatal.[168] In addition, outcome depends heavily on the cause of head injury. In the US, patients with fall-related TBIs have an 89% survival rate, while only 9% of patients with firearm-related TBIs survive.[173] In the US, firearms are the most common cause of fatal TBI, followed by vehicle accidents and then falls.[168] Of deaths from firearms, 75% are considered to be suicides.[168]
The incidence of TBI is increasing globally, due largely to an increase in motor vehicle use in low- and middle-income countries.[10] In developing countries, automobile use has increased faster than safety infrastructure could be introduced.[63] In contrast, vehicle safety laws have decreased rates of TBI in high-income countries,[10] which have seen decreases in traffic-related TBI since the 1970s.[54] Each year in the United States, about two million people have a TBI,[21] approximately 675,000 injuries are seen in the emergency department,[174] and about 500,000 patients are hospitalized.[171] The yearly incidence of TBI is estimated at 180–250 per 100,000 people in the US,[171] 281 per 100,000 in France, 361 per 100,000 in South Africa, 322 per 100,000 in Australia,[15] and 430 per 100,000 in England.[61] In the European Union the yearly aggregate incidence of TBI hospitalizations and fatalities is estimated at 235 per 100,000.[10]
Demographics
TBI is present in 85% of traumatically injured children, either alone or with other injuries.[175] The greatest number of TBIs occur in people aged 15–24.[13][37] Because TBI is more common in young people, its costs to society are high due to the loss of productive years to death and disability.[10] The age groups most at risk for TBI are children ages five to nine and adults over age 80,[9] and the highest rates of death and hospitalization due to TBI are in people over age 65.[140] The incidence of fall-related TBI in First-World countries is increasing as the population ages; thus the median age of people with head injuries has increased.[10]
Regardless of age, TBI rates are higher in males.[37] Men have twice as many TBIs as women do and have a fourfold risk of fatal head injury,[9] and males account for two thirds of childhood and adolescent head trauma;[176] however, when matched for severity of injury, women appear to fare more poorly than men.[95]
Socioeconomic status also appears to affect TBI rates; people with lower levels of education and employment and lower socioeconomic status are at greater risk.[15] Approximately half of those incarcerated in prisons and jails in the United States have had TBIs.[177]
History

Head injury is present in ancient myths that may date back before recorded history.
It was first suggested in the 18th century that intracranial pressure rather than skull damage was the cause of pathology after TBI. This hypothesis was confirmed around the end of the 19th century, and opening the skull to relieve pressure was then proposed as a treatment.[179]
In the 19th century it was noted that TBI is related to the development of psychosis.[184] At that time a debate arose around whether post-concussion syndrome was due to a disturbance of the brain tissue or psychological factors.[183] The debate continues today.

Perhaps the first reported case of personality change after brain injury is that of Phineas Gage, who survived an accident in which a large iron rod was driven through his head, destroying one or both of his frontal lobes; numerous cases of personality change after brain injury have been reported since.[31][33][34][43][44][48][185][186]
The 20th century saw the advancement of technologies that improved treatment and diagnosis such as the development of imaging tools including CT and MRI, and, in the 21st century, diffusion tensor imaging (DTI). The introduction of intracranial pressure monitoring in the 1950s has been credited with beginning the "modern era" of head injury.[116][187] Until the 20th century, the mortality rate of TBI was high and rehabilitation was uncommon; improvements in care made during World War I reduced the death rate and made rehabilitation possible.[178] Facilities dedicated to TBI rehabilitation were probably first established during World War I.[178] Explosives used in World War I caused many blast injuries; the large number of TBIs that resulted allowed researchers to learn about localization of brain functions.[188] Blast-related injuries are now common problems in returning veterans from Iraq & Afghanistan; research shows that the symptoms of such TBIs are largely the same as those of TBIs involving a physical blow to the head.[189]
In the 1970s, awareness of TBI as a public health problem grew,[190] and a great deal of progress has been made since then in brain trauma research,[116] such as the discovery of primary and secondary brain injury.[179] The 1990s saw the development and dissemination of standardized guidelines for treatment of TBI, with protocols for a range of issues such as drugs and management of intracranial pressure.[116] Research since the early 1990s has improved TBI survival;[179] that decade was known as the "Decade of the Brain" for advances made in brain research.[191]
Research directions
Diagnosis
Medications
No medication is approved to halt the progression of the initial injury to
Further research is necessary to determine if the vasoconstrictor indomethacin (indometacin) can be used to treat increased pressure in the skull following a TBI.
Procedures
In addition to traditional imaging modalities, there are several devices that help to monitor brain injury and facilitate research. Microdialysis allows ongoing sampling of extracellular fluid for analysis of metabolites that might indicate ischemia or brain metabolism, such as glucose, glycerol, and glutamate.[210][211] Intraparenchymal brain tissue oxygen monitoring systems (either Licox or Neurovent-PTO) are used routinely in neurointensive care in the US.[212] A non invasive model called CerOx is in development.[213]
Research is also planned to clarify factors correlated to outcome in TBI and to determine in which cases it is best to perform CT scans and surgical procedures.[214]
Psychological
Further research is required to determine the effectiveness of non-pharmacological treatment approaches for treating depression in children/adolescents and adults with TBI.[217]
As of 2010, the use of predictive visual tracking measurement to identify mild traumatic brain injury was being studied. In visual tracking tests, a
Monitoring pressure
Pressure reactivity index is used to correlate intracranial pressure with arterial blood pressure to give information about the state of cerebral perfusion, thus guiding treatment and prevent excessively high or low blood flow to the brain.[219] However, such method of monitoring intracranial pressure of equal or less than 20 mmHg is no better than imaging and clinical examination that monitor the neurological status of the brain in prolonging the survival, preserving the mental or functional status of the subject.[220]
Sensory processing
In animal models of TBI, sensory processing has been widely studied to show systematic defects arise and are slowly but likely only partially recovered.[221] It is especially characterised by an initial period of decreased activity in upper cortical layers.[222][223] This period of decreased activity has also been characterised as by specific timing effects in the patterns of cortical activity in these upper layers in response to regular sensory stimuli.[224]
References
- ISBN 978-0-19-970870-3.
- ^ PMID 18831756.
- ^ a b c "TBI: Get the Facts". CDC. March 11, 2019. Retrieved May 28, 2019.
- ^ "Traumatic Brain Injury". medlineplus.gov. Retrieved May 28, 2019.
- ^ S2CID 258821806.
- ^ "Basic Information about Traumatic Brain Injury | Concussion | Traumatic Brain Injury | CDC Injury Center". www.cdc.gov. March 6, 2019. Retrieved July 21, 2020.
- ^ "Prevention". CDC. March 4, 2019. Retrieved May 28, 2019.
- ^ ISBN 978-0-7923-7532-6.
- ^ PMID 10749946.
- ^ S2CID 14071224.
- ^ S2CID 46012183.
- ISBN 978-0-86377-724-0.
- ^ ]
- ^ PMID 16962454.
- ^ ISBN 978-0-19-511121-7.
- ^ PMID 9659083.
- ISBN 978-0-306-45256-7.
- ^ a b LaPlaca et al. (2007). p. 16
- ISBN 978-0-444-53017-2.
- ^ PMID 18627252.
- ^ a b c Department of Defense and Department of Veterans Affairs (2008). "DoD/VA CODE PROPOSAL FINAL—508 COMPLIANT" (PDF).
- ^ Marion (1999). p. 4.
- ^ ISBN 978-0-07-137069-1.
- ISBN 978-0-7817-6135-2.
- ^ S2CID 1527912.
- ^ Granacher (2007). p. 32.
- PMID 17872928.
- PMID 19196176.
- ISBN 978-0-387-98820-7.
brain injury biomechanics
- ISBN 978-0-19-532829-5.
- ^ S2CID 27836314.
- PMID 16083352.
- ^ PMID 8352676.
- ^ S2CID 22361889.
- S2CID 4477808.
- S2CID 25106246.
- ^ PMID 12391630.
TBI is highest in young adults aged 15 to 24 years and higher in men than women in all age groups.
- ^ ISBN 978-1-888799-93-4.
- ^ S2CID 45288155.
- ISBN 978-1-58562-105-7.
- ^ a b c d e "NINDS Traumatic Brain Injury Information Page". National Institute of Neurological Disorders and Stroke. September 15, 2008. Archived from the original on December 3, 2016. Retrieved October 27, 2008.
- ^ PMID 9701095.
- ^ S2CID 207724498.
- ^ PMID 12547978.
- S2CID 8840941.
- ^ PMID 18282321.
- S2CID 34126700.
- ^ S2CID 2264964.
- S2CID 41271134.
- PMID 18047870.
- ^ ISBN 978-0-07-137069-1.
- ^ a b "Signs and Symptoms". Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. July 7, 2007. Retrieved October 27, 2008.
- ^ Faul M, Xu L, Wald MM, Coronado VG (2010). "Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations, and Deaths, 2002–2006". National Center for Injury Prevention and Control, Centers for Disease Control and Prevention. Retrieved October 22, 2013.
- ^ ISBN 978-0-444-53017-2.
- ^ "Get the Facts About TBI | Concussion | Traumatic Brain Injury | CDC Injury Center". www.cdc.gov. April 20, 2023. Retrieved April 1, 2024.
- ^ Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. 2007. Retrieved October 28, 2008.
- ^ Granacher (2007). p. 16.
- ISBN 978-0-07-137069-1.
- ^ ISBN 978-1-58562-105-7.
- S2CID 44600297.
- ^ S2CID 34912966.
- PMID 19430256. Archived from the originalon September 23, 2017. Retrieved May 16, 2018.
- ^ PMID 18427091.
- ^ "Pentagon Told Congress It's Studying Brain-Damage Therapy". ProPublica. December 23, 2010. Retrieved January 23, 2011.
Brave Americans who risked everything for their country and sustained traumatic brain injuries – the signature injury of the wars in Iraq and Afghanistan – deserve cognitive rehabilitation therapy to help them secure the best futures possible. It is unacceptable that the United States has been at war for nearly a decade and there is still no plan to treat these soldiers.
- ^ S2CID 7262160.
- S2CID 7928780.
- ^ S2CID 46514293.
- PMID 11433079.
- PMID 9662103.
- .
- PMID 7869433.
- ^ PMID 12042091.
- ISBN 978-0-471-36015-5.
- ISBN 978-3-13-130781-1.
- PMID 18763356.
- ^ PMID 11223769.
- PMID 24820171.
- PMID 24986342.
- ^ "The DSM-5 Approach to Evaluating Traumatic Brain Injury". www.hsrd.research.va.gov. Retrieved November 5, 2019.
- ^ ISBN 978-0-7817-6135-2.
- ^ "University Times ' Research Notes". University of Pittsburgh. March 22, 2012. Retrieved November 10, 2013.
- PMID 17573394.
- ^ "Diagnosis and Assessment of Traumatic Brain Injury". Evaluation of the Disability Determination Process for Traumatic Brain Injury in Veterans. National Academies Press (US). April 10, 2019.
{{cite book}}:|journal=ignored (help) - ^ "Traumatic Brain Injury: What to Know About Symptoms, Diagnosis, and Treatment". Fda.gov. August 23, 2021.
- ^ From Flight magazine (1912), as described by Grothe S (March 26, 2016). "Mit dem Kopf durch die Wand (With the Head Through the Wall)". Der Spiegel (in German). Archived from the original on May 23, 2018.
- PMID 18254047.
- PMID 12919964.
- ^ PMID 15911597.
- ^ PMID 17967360.
- PMID 15698747.
- ^ Kluger, Jeffrey. "Dealing with Brain Injuries. Time Magazine, April 6, 2009, p. 57. Online: [1]. Accessed: May 1, 2009
- ^ a b c d e f g h i j k l Office of Communications and Public Liaison (February 2002). "Traumatic brain injury: Hope through research". NIH Publication No. 02-2478. National Institute of Neurological Disorders and Stroke, National Institutes of Health. Archived from the original on December 18, 2016. Retrieved August 17, 2008.
Many patients with mild to moderate head injuries who experience cognitive deficits become easily confused or distracted and have problems with concentration and attention. They also have problems with higher level, so-called executive functions, such as planning, organizing, abstract reasoning, problem solving, and making judgments, which may make it difficult to resume pre-injury work-related activities. Recovery from cognitive deficits is greatest within the first 6 months after the injury and more gradual after that.
- PMID 33343272.
- ^ PMID 12708551.
- ^ PMID 17545555. Moppet07
- S2CID 10548255.
- PMID 29283434.
- PMID 12391640.
- ^ PMID 26589595.
- ^ S2CID 23859003.
- PMID 15106241.
- S2CID 24947684.
- ^ PMID 23918314.
- PMID 31978260.
- PMID 17322250.
- PMID 22217782.
- PMID 10796728.
- S2CID 9927553.
- PMID 15674869.
- ISBN 978-1292-17084-8.
- PMID 11034722.
- PMID 18254109.
- PMID 14974051.
- PMID 17054192.
- ISBN 978-0-7817-8275-3.
- ^ PMID 10981741.
- ISBN 978-1-84882-069-2.
- .
- ISBN 978-1-58255-423-5.
- ^ ISBN 978-1-4200-4794-3.
- PMID 21434843.
- S2CID 3616546.
- PMID 26694853.
- ^ a b Ontario Neurotrauma Foundation and Institut national d'excellence en santé et en services sociaux (2015). "Clinical Practice Guideline for the Rehabilitation of Adults with Modarate to Severe Traumatic Brain Injury". braininjuryguidelines.org. Retrieved April 27, 2020.
- PMID 17636792.
- ^ ISBN 978-0-86377-889-6.
- S2CID 24775120.
- ^ S2CID 2650670.
- S2CID 45860264.
- ^ a b Grunt S. "Geh-Orthesen bei Kindern mit Cerebralparese". Pediatrica. 18: 30–34.
- )
- ISBN 978-3-13-151351-9.
- ISBN 978-0-323-03931-4.)
{{cite book}}: CS1 maint: location missing publisher (link - ^ Muñoz S (2018). "The new generation of AFOs". The O&P EDGE. 11. Archived from the original on June 6, 2021. Retrieved October 25, 2021.
- PMID 27131186.
- ISSN 0966-6362.
- S2CID 212641072.
- PMID 31623670.
- PMID 31406508.
- ^ PMID 18295647.
- ^ S2CID 34749005.
- S2CID 23726077.
- PMID 20437324.
- ISBN 978-1-4377-0434-1.
- PMID 26618215.
- PMID 29286534.
- ^ "Persistent vegetative state" at Dorland's Medical Dictionary.
- S2CID 347998.
- ^ PMID 18295644.
- PMID 29165784.
- PMID 12040514.
- S2CID 26338743.
- ISBN 978-1-58562-105-7.
- PMID 15883140.
- S2CID 41087553.
- S2CID 20238578.
- ^ S2CID 205907369.
- PMID 19940674.
- ^ S2CID 43384334.
- ^ S2CID 21067999.
- S2CID 207447494.
- PMID 19370632.
- S2CID 205643570.
- ^ Fleminger S (2010). "Neuropsychiatric effects of traumatic brain injury". Psychiatr Times. 27 (3): 40–45. Archived from the original on March 16, 2020. Retrieved April 23, 2010.
- PMID 16280354.
- S2CID 12428952.
- S2CID 20918911.
- ^ S2CID 23713764.
- ^ "Coma" at Dorland's Medical Dictionary.
- PMID 15083870.
- ^ PMID 15542983.
- ISBN 978-0-7881-8376-8.
- ^ Tolias C, Sgouros S (February 4, 2005). "Initial evaluation and management of CNS injury". Medscape. Retrieved December 16, 2007.
- ^ Kindermann D, Mutter R, Pines JM (May 2013). Emergency Department Transfers to Acute Care Facilities 2009 (Report). Agency for Healthcare Research and Quality. HCUP Statistical Brief #155. Archived from the original on December 1, 2016.
- S2CID 28381295.
- PMID 15998982. Archived from the original(PDF) on October 19, 2013. Retrieved January 26, 2007.
- ^ "An Unrecognized Problem" (PDF). Centers for Disease Control and Prevention. Retrieved October 13, 2019.
- ^ a b c Boake and Diller (2005). p. 3
- ^ a b c d Granacher (2007). p. 1.
- ISBN 978-0-252-02956-1.
- PMID 17961064.
- ^ ISBN 978-0-19-503008-2.
- ^ ISBN 978-1-57230-078-1.
- ISBN 978-1-58562-105-7.
- S2CID 22373825.
- ISBN 978-0-19-513764-4.
- ^ Marion (1999). p. 3.
- PMID 17974926.
- S2CID 21648436.
- ^ Boake and Diller (2005). p. 8
- ^ Bush GH (July 1990). "Project on the Decade of the Brain". Library of Congress. Retrieved October 22, 2013.
- PMID 32341694.
- PMID 33126293.
- ^ S2CID 4495428.
- S2CID 19064475.
- PMID 28933514.
- PMID 31752052.
- S2CID 23399305.
- PMID 17011666.
- S2CID 9756580.
- PMID 23235573.
- PMID 20129501.
- PMID 18843689.
- PMID 14583925.
- PMID 18948087.
- S2CID 37759164.
- S2CID 13345179.
- PMID 9126906.
- S2CID 29276898.
- PMID 2384536.
- PMID 15716852.
- S2CID 23154956.
- PMID 24484228.
- PMID 17916856.
- ^ PMID 23235612.
- S2CID 35914918.
- PMID 26663136.
- PMID 20955326.
- S2CID 26020481.
- PMID 23234472.
- PMID 27313514.
- PMID 23284921.
- PMID 24927383.
- .
Cited texts
- Boake C, Diller L (2005). "History of rehabilitation for traumatic brain injury". In High WM, Sander AM, Struchen MA, Hart KA (eds.). Rehabilitation for Traumatic Brain Injury. Oxford [Oxfordshire]: Oxford University Press. ISBN 978-0-19-517355-0.
- Granacher RA (2007). Traumatic Brain Injury: Methods for Clinical & Forensic Neuropsychiatric Assessment, Second Edition. Boca Raton: CRC. ISBN 978-0-8493-8138-6.
- LaPlaca MC, Simon CM, Prado GR, Cullen DR (2007). "CNS injury biomechanics and experimental models". In Weber JT (ed.). Neurotrauma: New Insights Into Pathology and Treatment. Amsterdam: Academic Press. ISBN 978-0-444-53017-2.
- Marion DW (1999). "Introduction". In Marion DW (ed.). Traumatic Brain Injury. Stuttgart: Thieme. ISBN 978-0-86577-727-9.
The original version of this article contained text from the NINDS public domain pages on TBI Archived December 18, 2016, at the Wayback Machine
External links
- Brain injury at Curlie
- The Brain Injury Hub – information and practical advice to parents and family members of children with acquired brain injury Archived October 5, 2020, at the Wayback Machine
- Defense and Veterans Brain Injury Center – U.S. Department of Defense Military Health System center for traumatic brain injury Archived October 12, 2019, at the Wayback Machine
