Vancomycin
 | |
 | |
| Clinical data | |
|---|---|
| Pronunciation | /væŋkəˈmaɪsɪn/[1][2] |
| Trade names | Vancocin, others[3] |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a604038 |
| License data |
|
| Pregnancy category |
|
Intravenous, oral | |
| Drug class | Glycopeptide antibiotic |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | Negligible (oral) |
| Metabolism | Excreted unchanged |
| Elimination half-life | 4 h to 11 h (adults, normal renal function) 6 d to 10 d (adults, impaired renal function) |
| Excretion | urine (IV), feces (oral) |
| Identifiers | |
| |
JSmol) | |
| |
| |
| (verify) | |
Vancomycin is a
Common side effects include pain in the area of injection and
Vancomycin was approved for medical use in the United States in 1958.[12] It is on the World Health Organization's List of Essential Medicines.[13][14] The World Health Organization classifies vancomycin as critically important for human medicine.[15] It is available as a generic medication.[9] Vancomycin is made by the soil bacterium Amycolatopsis orientalis.[7]
Medical uses
Vancomycin is indicated for the treatment of serious, life-threatening infections by
The increasing emergence of vancomycin-resistant
- treatment of serious infections caused by susceptible organisms resistant to penicillins (methicillin-resistant S. aureus (MRSA) and multidrug-resistant S. epidermidis (MRSE)) or in individuals with serious allergy to penicillins,
- treatment of pseudomembranous colitis caused by C. difficile; in particular, in cases of relapse or where the infection is unresponsive to metronidazoletreatment (for this indication, vancomycin is given orally, rather than by its typical intravenous route),
- treatment of infections caused by Gram-positive microorganisms in patients with serious allergies to beta-lactam antimicrobials,[21]
- antibacterial prophylaxis for endocarditis following certain procedures in penicillin-hypersensitive individuals at high risk,[21]
- surgical prophylaxis for major procedures involving implantation of prostheses in institutions with a high rate of MRSA or MRSE,[21]
- early in treatment as an empiric antibiotic for possible MRSA infection while waiting for culture identification of the infecting organism,
- halting the progression of primary sclerosing cholangitis and preventing symptoms; vancomycin does not cure the patient and success is limited,
- treatment of endophthalmitis by intravitreal injection for gram-positive bacteria coverage; [22] it has been used to prevent the condition, however, is not recommended due to the risk of side effects.[23]
Spectrum of susceptibility
Vancomycin is considered a last resort medication for the treatment of
- S. aureus: 0.25 μg/mL to 4.0 μg/mL
- S. aureus (methicillin resistant or MRSA): 1 μg/mL to 138 μg/mL
- S. epidermidis: ≤0.12 μg/mL to 6.25 μg/mL
Side effects
Oral administration
Common side effects associated with oral vancomycin administration (used to treat intestinal infections)[25] include:
- gastrointestinal adverse effects (such as abdominal pain and nausea);[25]
- dysgeusia (distorted sense of taste), in case of administration of vancomycin oral solution, but not in case of vancomycin capsules.[25]
Intravenous administration
Serum vancomycin levels may be monitored in an effort to reduce side effects.[26] Still, the value of such monitoring has been questioned.[27] Peak and trough levels are usually monitored, and for research purposes, the area under the concentration curve is also sometimes used.[28] Toxicity is best monitored by looking at trough values.[28] Immunoassays are commonly used to measure levels of vancomycin.[26]
Common adverse drug reactions (≥1% of patients) associated with intravenous (IV) vancomycin include:
- pain, redness, or swelling at the injection site;[29]
- vancomycin flushing syndrome (VFS), previously known as red man syndrome (or "redman syndrome");[25]
- thrombophlebitis, which is common when administered through peripheral catheters but not when central venous catheters are used, although central venous catheters are a predisposing factor for upper-extremity deep-vein thrombosis.[30]
Damage to the kidneys (nephrotoxicity) and to the hearing (ototoxicity) were side effects of the early impure versions of vancomycin, and these were prominent in the clinical trials conducted in the mid-1950s.[31][32] Later trials using purer forms of vancomycin found nephrotoxicity is an infrequent adverse effect (0.1% to 1% of patients), but this is accentuated in the presence of aminoglycosides.[33]
Rare adverse effects associated with intravenous (IV) vancomycin (<0.1% of patients) include:
Vancomycin can induce platelet-reactive antibodies in the patient, leading to severe
Historically, vancomycin has been considered a nephrotoxic and ototoxic drug, based on numerous case reports in the medical literature following initial approval by the FDA in 1958. However, as the use of vancomycin increased with the spread of MRSA beginning in the 1970s, toxicity risks were reassessed. With the removal of impurities present in earlier formulations of the drug,[31] and with the introduction of therapeutic drug monitoring, the risk for severe toxicity has been reduced.
Nephrotoxicity
The extent of nephrotoxicity for vancomycin remains controversial.[36] In 1980s, vancomycin with a purity > 90% was available, and kidney toxicity defined by an increase in serum creatinine of at least 0.5 mg/dl, occurred in only about 5% of patients.[36] However, dosing guidelines from the 1980s until 2008 recommended vancomycin trough concentrations between 5 and 15 μg/ml.[37] Concern for treatment failures prompted recommendations for higher dosing (troughs 15 to 20 μg/ml) for serious infection, and acute kidney injury (AKI) rates attributable to the vancomycin increased.[38]
Importantly, the risk of AKI increases with co-administration of other known nephrotoxins, in particular, aminoglycosides. Furthmore, the sort of infections treated with vancomycin may also cause AKI and sepsis is the most common cause of AKI in critically ill patients. Finally, studies in humans are mainly associations studies where the cause of AKI is usually multifacotorial.[citation needed]
Animal studies have demonstrated that higher doses and longer duration of vancomycin exposure correlates with increased histopathologic damage and elevations in urinary biomarkers of AKI.37-38[39] Damage is most prevalent at the proximal tubule, which is further supported by urinary biomarkers, such as kidney injury molecule-1 (KIM-1), clusterin, and osteopontin (OPN),[40] and in humans, insulin-like growth factor binding protein 7 (IGFBP7) as part of the nephrocheck test.[41]
The mechanisms that underlie the pathogenesis of vancomycin nephrotoxicity are multifactorial but include interstitial nephritis, tubular injury due to oxidative stress, and cast formation.[38]
Therapeutic drug monitoring can be used during vancomycin therapy to minimize the risk of nephrotoxicity associated with excessive drug exposure. Immunoassays are commonly utilized for measuring vancomycin levels.[26]
In children, the concomitant administration of vancomycin and piperacillin/tazobactam has been associated with an elevated incidence of AKI, relative to other antibiotic regimens.[42]
Ototoxicity
Attempts to establish rates of vancomycin-induced ototoxicity are even more difficult due to the scarcity of quality evidence. The current consensus is that clearly related cases of vancomycin ototoxicity are rare.[43][44] The association between vancomycin serum levels and ototoxicity is also uncertain. While cases of ototoxicity have been reported in patients whose vancomycin serum level exceeded 80 µg/mL,[45] cases have been reported in patients with therapeutic levels, as well. Thus, whether therapeutic drug monitoring of vancomycin for the purpose of maintaining "therapeutic" levels will prevent ototoxicity also remains unproven.[45] Still, therapeutic drug monitoring can be used during vancomycin therapy to minimize the risk of ototoxicity associated with excessive drug exposure.[26]
Interactions with other nephrotoxins
Another area of controversy and uncertainty concerns the question of whether, and if so, to what extent, vancomycin increases the toxicity of other nephrotoxins. Clinical studies have yielded variable results, but animal models indicate some increased nephrotoxic effect probably occurs when vancomycin is added to nephrotoxins such as aminoglycosides. However, a dose- or serum level-effect relationship has not been established.[citation needed]
Vancomycin Flushing Reaction (aka "Red man syndrome")
Vancomycin is recommended to be administered in a dilute solution slowly, over at least 60 min (maximum rate of 10 mg/min for doses >500 mg)
Dosing considerations
The recommended intravenous dosage in adults is 500 mg iv every 6 hours or 1000 mg every 12 hours, with modification to achieve a therapeutic range as needed. The recommended oral dosage in the treatment of antibiotic-induced pseudomembranous enterocolitis is 125 to 500 mg every 6 hours for 7 to 10 days.[49]
Dose optimization and target attainment of vancomycin in children involves adjusting the dosage of the antibiotic to maximize its effectiveness while minimizing the risk of adverse effects, specifically acute kidney injury. Dose optimization is achieved through therapeutic drug monitoring (TDM), which allows to measure vancomycin levels in the blood and tailor the dosage accordingly. TDM using area under the curve (AUC)-guided dosing, preferably with Bayesian forecasting, is recommended to ensure that the AUC0-24h/minimal inhibitory concentration (MIC) ratio is maintained above a certain threshold (400-600) associated with optimal efficacy.[50]
Routes of administration
In the United States, vancomycin is approved by the Food and Drug Administration for either intravenous or oral administration.[25]
Intravenous
Vancomycin must be given
Oral
The only approved indication for oral vancomycin therapy is in the treatment of pseudomembranous colitis, where it must be given orally to reach the site of infection in the colon. Following oral administration, the fecal concentration of vancomycin is around 500 µg/mL
Inhaled (off-label)
Inhaled vancomycin can also be used
Rectal (off-label)
Rectal administration is an
Therapeutic drug monitoring
Plasma level monitoring of vancomycin is necessary due to the drug's biexponential distribution, intermediate hydrophilicity, and potential for ototoxicity and nephrotoxicity, especially in populations with poor renal function and/or increased propensity to bacterial infection. Vancomycin activity is considered to be time-dependent; that is, antimicrobial activity depends on the duration that the serum drug concentration exceeds the minimum inhibitory concentration of the target organism. Thus, peak serum levels have not been shown to correlate with efficacy or toxicity; indeed, concentration monitoring is unnecessary in most cases. Circumstances in which therapeutic drug monitoring is warranted include: patients receiving concomitant aminoglycoside therapy, patients with (potentially) altered pharmacokinetic parameters, patients on haemodialysis, patients administered high-dose or prolonged treatment, and patients with impaired renal function. In such cases, trough concentrations are measured.[20][27][60][61]
Therapeutic drug monitoring is also used for dose optimization of vancomycin in treating children.[50]
Target ranges for serum vancomycin concentrations have changed over the years. Early authors suggested peak levels of 30 to 40 mg/L and
Chemistry
Vancomycin is a branched tricyclic glycosylated nonribosomal peptide produced by the Actinomycetota species Amycolatopsis orientalis (formerly designated Nocardia orientalis).
Vancomycin exhibits
Biosynthesis
Vancomycin is made by the soil bacterium Amycolatopsis orientalis.[7]

Vancomycin biosynthesis occurs primarily via three

Nonribosomal peptide synthesis occurs through distinct

A set of NRPS enzymes (peptide synthase VpsA, VpsB, and VpsC) are responsible for assembling the heptapeptide. (Figure 2).[68] VpsA codes for modules 1, 2, and 3. VpsB codes for modules 4, 5, and 6, and VpsC codes for module 7. The vancomycin aglycone contains 4 D-amino acids, although the NRPSs only contain 3 epimerization domains. The origin of D-Leu at residue 1 is not known. The three peptide syntheses are located at the start of the region of the bacterial genome linked with antibiotic biosynthesis, and span 27 kb.[68]
β-hydroxytyrosine (β-HT) is synthesized prior to incorporation into the heptapeptide backbone. L-tyrosine is activated and loaded on the NRPS VpsD, hydroxylated by OxyD, and released by the thioesterase Vhp.[72] The timing of the chlorination by halogenase VhaA during biosynthesis is currently undetermined, but is proposed to occur before the complete assembly of the heptapeptide.[73]
After the linear heptapeptide molecule is synthesized, vancomycin has to undergo further modifications, such as oxidative cross-linking and glycosylation, in trans[clarification needed] by distinct enzymes, referred to as tailoring enzymes, to become biologically active (Figure 3). To convert the linear heptapeptide to cross-linked, glycosylated vancomycin, six enzymes, are required. The enzymes OxyA, OxyB, OxyC, and OxyD are cytochrome P450 enzymes. OxyB catalyzes oxidative cross-linking between residues 4 and 6, OxyA between residues 2 and 4, and OxyC between residues 5 and 7. This cross-linking occurs while the heptapeptide is covalently bound to the PCP domain of the 7th NRPS module. These P450s are recruited by the X domain present in the 7th NRPS module, which is unique to glycopeptide antibiotic biosynthesis.[74] The cross-linked heptapeptide is then released by the action of the TE domain, and methyltransferase Vmt then N-methylates the terminal leucine residue. GtfE then joins D-glucose to the phenolic oxygen of residue 4, followed by the addition of vancosamine catalyzed by GtfD.[citation needed]
Some of the glycosyltransferases capable of glycosylating vancomycin and related nonribosomal peptides display notable permissivity and have been employed for generating libraries of differentially glycosylated analogs through a process known as glycorandomization.[75][76][77]
Total synthesis
Both the vancomycin aglycone[78][79] and the complete vancomycin molecule[80] have been targets successfully reached by total synthesis. The target was first achieved by David Evans in October 1998, KC Nicolaou in December 1998, Dale Boger in 1999, and has recently been more selectively synthesized again by Dale Boger in 2020.
Mechanism of action

Vancomycin targets bacterial cell wall synthesis by binding to the basic building block of the bacterial cell wall of Gram-positive bacteria, whether it is of
Peptidoglycan is a polymer that provides structural support to the bacterial cell wall. The peptidoglycan precursor is synthesized in the cytoplasm and then transported across the cytoplasmic membrane to the periplasmic space, where it is assembled into the cell wall. The assembly process involves two enzymatic activities: transglycosylation and transpeptidation. Transglycosylation involves the polymerization of the peptidoglycan precursor into long chains, while transpeptidation involves the cross-linking of these chains to form a three-dimensional mesh-like structure.[17]
Vancomycin inhibits bacterial cell wall synthesis by binding to the D-Ala-D-Ala peptide motif of the peptidoglycan precursor, thereby preventing its processing by the transglycosylase; as such vancomycin disrupts the transglycosylation activity of the cell wall synthesis process. The disruption leads to an incomplete and corrupted cell wall, which makes the replicating bacteria vulnerable to external forces such as osmotic pressure, so that the bacteria cannot survive and are eliminated by the immune system.[17]
Gram-negative bacteria are insensitive to vancomycin due to their different cell wall morphology. The outer membrane of Gram-negative bacteria contains lipopolysaccharide, which acts as a barrier to vancomycin penetration. That is why vancomycin is mainly used to treat infections caused by Gram-positive bacteria[17] (except some nongonococcal species of Neisseria).[82][83]
The large
This article may be too technical for most readers to understand. (March 2024) |
This binding of vancomycin to the D-Ala-D-Ala prevents cell wall synthesis of the long polymers of N-acetylmuramic acid (NAM) and N-acetylglucosamine (NAG) that form the backbone strands of the bacterial cell wall, and prevents the backbone polymers from cross-linking with each other.[84]
Plant tissue culture
Vancomycin is one of the few antibiotics used in plant tissue culture to eliminate Gram-positive bacterial infection. It has relatively low toxicity to plants.[85][86]
Antibiotic resistance
Intrinsic resistance
A few Gram-positive bacteria are intrinsically resistant to vancomycin: Leuconostoc and Pediococcus species, but these organisms rarely cause diseases in humans.[87] Most Lactobacillus species are also intrinsically resistant to vancomycin,[87] with the exception of L. acidophilus and L. delbrueckii, which are sensitive.[88] Other Gram-positive bacteria with intrinsic resistance to vancomycin include Erysipelothrix rhusiopathiae, Weissella confusa, and Clostridium innocuum.[89][90][91]
Most Gram-negative bacteria are intrinsically resistant to vancomycin because their outer membranes are impermeable to large glycopeptide molecules[92] (with the exception of some non-gonococcal Neisseria species).[93]
Acquired resistance
Evolution of microbial resistance to vancomycin is a growing problem, in particular, within healthcare facilities such as hospitals. While newer alternatives to vancomycin exist, such as linezolid (2000) and daptomycin (2003), the widespread use of vancomycin makes resistance to the drug a significant worry, especially for individual patients if resistant infections are not quickly identified and the patient continues the ineffective treatment. Vancomycin-resistant Enterococcus emerged in 1986.[94] Vancomycin resistance evolved in more common pathogenic organisms during the 1990s and 2000s, including vancomycin-intermediate S. aureus (VISA) and vancomycin-resistant S. aureus (VRSA).[95][96] Agricultural use of avoparcin, another similar glycopeptide antibiotic, may have contributed to the evolution of vancomycin-resistant organisms.[97][98][99][100]
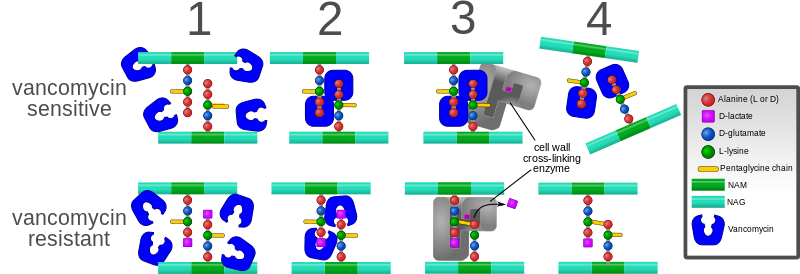
One mechanism of resistance to vancomycin involves the alteration to the terminal amino acid residues of the NAM/NAG-peptide subunits, under normal conditions, D-alanyl-D-alanine, to which vancomycin binds. The D-alanyl-D-lactate variation results in the loss of one hydrogen-bonding interaction (4, as opposed to 5 for D-alanyl-D-alanine) possible between vancomycin and the peptide. This loss of just one point of interaction results in a 1000-fold decrease in affinity. The D-alanyl-D-serine variation causes a six-fold loss of affinity between vancomycin and the peptide, likely due to steric hindrance.[101]
In enterococci, this modification appears to be due to the expression of an enzyme that alters the terminal residue. Three main resistance variants have been characterised to date among resistant Enterococcus faecium and E. faecalis populations:
- VanA - enterococcal resistance to vancomycin and teicoplanin; inducible on exposure to these agents
- VanB - lower-level enterococcal resistance; inducible by vancomycin, but strains may remain susceptible to teicoplanin
- VanC - least clinically important; enterococci resistant only to vancomycin; constitutive resistance
Variant of vancomycin has been tested that binds to the resistant D-lactic acid variation in vancomycin-resistant bacterial cell walls, and also binds well to the original target (vancomycin-susceptible bacteria).[102][103]
"Re-gained" vancomycin
In 2020 a team at the
Research directions
The combination of vancomycin powder and povidone-iodine lavage has shown promise in reducing the risk of periprosthetic joint infection in hip and knee arthroplasties. In several studies, this combination was found to be more effective than vancomycin alone in preventing joint infection, with lower rates of infection and fewer adverse events. However, there is still a need for prospective randomized studies to confirm these findings and assess the long-term efficacy and safety of this treatment approach. The research directions are to determine the optimal dosage and timing of vancomycin and povidone-iodine lavage, as well as their potential synergistic effect, safety, and efficiency of this possible future treatment option in reducing the risk of periprosthetic joint infection in hip and knee arthroplasties.[106]
History
Vancomycin was first isolated in 1953, by Edmund Kornfeld (working at Eli Lilly) from a bacteria in a soil sample collected from the interior jungles of Borneo by a missionary, William M. Bouw (1918–2006).[107] The organism that produced it was eventually named Amycolatopsis orientalis.[31] The original indication for vancomycin was for the treatment of penicillin-resistant Staphylococcus aureus.[31][32]
The compound was initially called compound 05865, but was eventually given the generic name vancomycin, derived from the term "vanquish".[31] One advantage that was quickly apparent was that staphylococci did not develop significant resistance, despite serial passage in culture media containing vancomycin. The rapid development of penicillin resistance by staphylococci led to its being fast-tracked for approval by the Food and Drug Administration. In 1958, Eli Lilly first marketed vancomycin hydrochloride under the trade name Vancocin.[32]
Vancomycin never became the first-line treatment for S. aureus for several reasons:
- It possesses poor oral bioavailability, so must be given intravenously for most infections.
- β-Lactamase-resistant semisynthetic penicillins such as methicillin (and its successors, nafcillin and cloxacillin) were subsequently developed, which have better activity against non-MRSA staphylococci.
- Early trials used early, impure forms of the drug ("Mississippi mud"), which were found to be toxic to the inner ear and to the kidneys;[108] these findings led to vancomycin's being relegated to the position of a drug of last resort.[32]
In 2004, Eli Lilly licensed Vancocin to
References
- ^ "vancomycin". Merriam-Webster.com Dictionary.
- OxfordDictionaries.com. Archived from the originalon 20 September 2013. Retrieved 20 January 2016.
- ^ "Vancomycin". Drugs.com. 2 December 2019. Archived from the original on 24 December 2019. Retrieved 24 December 2019.
- ^ "Vancomycin Use During Pregnancy". Drugs.com. 27 March 2019. Archived from the original on 6 June 2019. Retrieved 24 December 2019.
- FDA. Retrieved 22 October 2023.
- ^ "List of nationally authorised medicinal products" (PDF). European Medicines Agency. 15 October 2020. Archived (PDF) from the original on 25 September 2023. Retrieved 27 April 2023.
- ^ a b c d e f g h i "Vancocin". The American Society of Health-System Pharmacists. Archived from the original on 6 September 2015. Retrieved 4 September 2015.
- PMID 21217178.
- ^ ISBN 978-1-284-05756-0.
- ^ "Prescribing medicines in pregnancy database". Australian Government. September 2015. Archived from the original on 8 April 2014.
- ^ "Vancomycin use while Breastfeeding". Archived from the original on 7 September 2015. Retrieved 5 September 2015.
- PMID 16323120.
- hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- hdl:10665/345533. WHO/MHP/HPS/EML/2021.02.
- ISBN 978-92-4-151552-8.
- ^ ISBN 978-0-444-63749-9.
- ^ S2CID 202745549.
- PMID 31899563.
- PMID 25753888.
- ^ ISBN 0-9757919-2-3.
- ^ from the original on 23 September 2006.
- PMID 10691328.
- ^ Office of the Commissioner. "Safety Alerts for Human Medical Products - Intraocular Injections of a Compounded Triamcinolone, Moxifloxacin, and Vancomycin (TMV) Formulation: FDA Statement - Case of Hemorrhagic Occlusive Retinal Vasculitis". www.fda.gov. Archived from the original on 3 October 2017. Retrieved 6 October 2017.
- ^ "Vancomycin (Vancocyn, Lyphocin) | the Antimicrobial Index Knowledgebase - TOKU-E". Archived from the original on 27 February 2014. Retrieved 26 February 2014.[full citation needed]
- ^ from the original on 11 April 2023. Retrieved 19 July 2023.
- ^ PMID 38304144.
- ^ PMID 8038306.
- ^ PMID 19586413.
- ^ "Vancomycin Injection: MedlinePlus Drug Information". medlineplus.gov. Archived from the original on 19 July 2023. Retrieved 19 July 2023.
- PMID 22669879.
- ^ PMID 16323120.
- ^ PMID 16323117.
- PMID 6219616.
- PMID 22525393.
- PMID 17329697.
- ^ PMID 6219616.
- S2CID 32585259.
- ^ PMID 32239518.
- S2CID 45358082.
- PMID 30988153.
- PMID 29189343.
- S2CID 267300725.
- PMID 31693679.
- PMID 33767665.
- ^ PMID 12225605.
- PMID 28367504.
- PMID 12720556.
- ISBN 0-7216-2921-0.
- PMID 31644188, archived from the original on 14 May 2021, retrieved 25 February 2021.
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License Archived 16 October 2017 at the Wayback Machine
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License Archived 16 October 2017 at the Wayback Machine - ^ S2CID 267502279.
- PMID 16955686.
- PMID 9314469.
- PMID 12019070.
- PMID 31964790.
- PMID 25533880.
- ^ "Inhaled Vancomycin Monograph - Paediatric" (PDF). Perth Children's Hospital (PCH). Archived (PDF) from the original on 14 March 2023. Retrieved 19 July 2023.
- .
- ^ "Is there literature describing the efficacy or safety of inhaled vancomycin to treat MRSA ventilator-associated tracheobronchitis? | Drug Information Group | University of Illinois Chicago". Archived from the original on 19 July 2023. Retrieved 19 July 2023.
- PMID 25143711.
- PMID 8038307.
- S2CID 24947921.
- PMID 909314.
- S2CID 11692065.
- from the original on 15 September 2017. Retrieved 15 September 2017.
- PMID 31534058.
- PMID 18414736.
- ISBN 978-0-471-49641-0.[page needed]
- ^ PMID 9545426.
- PMID 1744112.
- PMID 8663196.
- S2CID 4380296.
- PMID 15342578.
- (PDF) from the original on 2 February 2024. Retrieved 2 February 2024.
- from the original on 24 February 2021. Retrieved 23 June 2020.
- S2CID 2469387.
- PMID 15816740.
- PMID 22984807.
- PMID 29711601.
- ISBN 978-3-527-61997-9.
- .
- PMID 2386365.
- PMID 30408494.
- PMID 6790572.
- ^ "Clinical Pharmacology". Archived from the original on 27 August 2021. Retrieved 10 September 2011.
- ^ "vancomcin for plant cell culture" (PDF). Archived from the original (PDF) on 4 May 2012.
- S2CID 84495391.
- ^ PMID 2344161.
- S2CID 221924592.
- PMID 18159347.
- PMID 15150227.
- PMID 21596906.
- ISBN 978-1-55581-086-3.
- PMID 7342289.
- from the original on 11 September 2022. Retrieved 11 September 2022.
The first reports of vancomycin-resistant enterococci (later classified as VanA type of resistance) involved strains of E. faecium that were resistant to vancomycin and teicoplanin (another glycopeptide) and that were isolated from patients in France and England in 1986. Vancomycin-resistant E. faecalis, subsequently classified as VanB type, was recovered from patients in Missouri in 1987.
- PMID 10021469.
- S2CID 43628397.
- PMID 11168181.
- S2CID 4958557.
- S2CID 24378463.
- (PDF) from the original on 10 May 2019. Retrieved 20 April 2018.
- PMID 11807177.
- PMID 21823662.
- PMID 28559345.
- PMID 32190958.
- ^ EP 3846854A2, Mier W, Umstätter F, Uhl P, Domhan C, "Improved polypeptide coupled antibiotics." Archived 8 October 2021 at the Wayback Machine
- S2CID 254215681.
- ISBN 978-0-316-73566-7.
- PMID 7043707.
- ^ "Orange Book: Approved Drug Products with Therapeutic Equivalence Evaluations". Archived from the original on 17 August 2016.
External links
- "Vancomycin". Drug Information Portal. U.S. National Library of Medicine.
- "Vancomycin hydrochloride". Drug Information Portal. U.S. National Library of Medicine.