Wilson's disease
| Wilson's disease | |
|---|---|
| Other names | Wilson disease, hepatolenticular degeneration |
liver transplant[1] | |
| Frequency | ~1 per 30,000[1] |
Wilson's disease is a
Wilson's disease is caused by a
Wilson's disease is typically treated with dietary changes and medication. Dietary changes involve eating a low-copper diet and not using copper cookware. Medications used include
Wilson's disease occurs in about one in 30,000 people.[1] Symptoms usually begin between the ages of 5 and 35 years.[1] It was first described in 1854 by German pathologist Friedrich Theodor von Frerichs and is named after British neurologist Samuel Wilson.[4]
Signs and symptoms
The main sites of copper accumulation are the liver and the brain, and consequently liver disease and neuropsychiatric symptoms are the main features that lead to diagnosis.[5] People with liver problems tend to come for medical attention earlier, generally as children or teenagers, than those with neurological and psychiatric symptoms, who tend to be in their 20s or older. Some are identified only because relatives have been diagnosed with Wilson's disease; many of these, when tested, turn out to have been experiencing symptoms of the condition, but have not received a diagnosis.[6]
Liver disease
Liver disease may present itself as
About 5% of all people are diagnosed only when they develop fulminant acute liver failure, often in the context of a hemolytic anemia (anemia due to the destruction of red blood cells). This leads to abnormalities in protein production (identified by deranged coagulation) and metabolism by the liver. The deranged protein metabolism leads to the accumulation of waste products such as ammonia in the bloodstream. When these irritate the brain, the person develops hepatic encephalopathy (confusion, coma, seizures, and finally life-threatening swelling of the brain).[5]
Neuropsychiatric symptoms

About half of the people with Wilson's disease have neurological or psychiatric symptoms. Most initially have mild cognitive deterioration and clumsiness, as well as changes in behavior. Specific neurological symptoms usually then follow, often in the form of
Cognition can also be affected in Wilson's disease, in two, not mutually exclusive, categories - frontal lobe disorder (may present as impulsivity, impaired judgement, promiscuity, apathy, and executive dysfunction with poor planning and decision-making) and subcortical dementia (may present as slow thinking, memory loss, and executive dysfunction, without signs of aphasia, apraxia, or agnosia). These cognitive involvements are thought to be related and closely linked to psychiatric manifestations of the disease.[8]
Psychiatric problems due to Wilson's disease may include behavioral changes,
Other organ systems
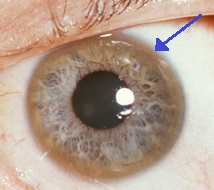
Medical conditions have been linked with copper accumulation in Wilson's disease:
- Eyes: Kayser–Fleischer rings (KF rings) may be visible in the cornea of the eyes, either directly or on slit lamp examination as deposits of copper form a ring around the cornea. This is due to copper deposition in Descemet's membrane. These rings can be either dark brown, golden, or reddish-green, are 1 to 3 mm wide, and appear at the corneal limbus. They do not occur in all people with Wilson's disease and may be seen in people with chronic cholestasis.[10][11] Wilson's disease is also associated with sunflower cataracts exhibited by brown or green pigmentation of the anterior and posterior lens capsule.[12] Neither causes significant visual loss.[5] KF rings occur in approximately 66% of diagnosed cases (more often in those with neurological symptoms rather than with liver problems).[6]
- Kidneys: renal tubular acidosis (Type 2), a disorder of bicarbonate handling by the proximal tubules leads to nephrocalcinosis (calcium accumulation in the kidneys), a weakening of bones (due to calcium and phosphate loss), and occasionally aminoaciduria (loss of essential amino acids needed for protein synthesis).[5]
- Heart: cardiac arrhythmias (episodes of irregular and/or abnormally fast or slow heart beat).[5]
- Hormones: panhypopituitarism (leading to decreased production of hormones from the pituitary gland), infertility, and recurrent miscarriage.[5][13]
- Musculoskeletal: Arthritis and thinning of the bones (osteopenia or osteoporosis).[14]
-
Sunflower cataract and thick KF ring of a 40-year-old male with Wilson's disease and decompensated CLD
-
Diffuse illumination of cornea
-
Copper deposition on corneal Descemet's membrane
Genetics

The Wilson's disease gene (ATP7B) is on
Although 300 mutations of ATP7B have been described, in most populations, the cases of Wilson's disease are due to a small number of mutations specific for that population. For instance, in Western populations, the H1069Q mutation (replacement of a histidine by a glutamine at position 1069 in the protein) is present in 37–63% of cases, while in China, this mutation is very uncommon and R778L (arginine to leucine at 778) is found more often. Relatively little is known about the relative impact of various mutations, although the H1069Q mutation seems to predict later onset and predominantly neurological problems, according to some studies.[5][15] A comprehensive clinically annotated resource, WilsonGen provides a clinical classification for the variants as per the recent ACMG & AMP guidelines[16]
A normal variation in the
The condition is inherited in an autosomal recessive pattern. To inherit it, both of the parents of an individual must carry an affected gene. Most have no family history of the condition.[15] People with only one abnormal gene are called carriers (heterozygotes) and may have mild, but medically insignificant, abnormalities of copper metabolism.[14]
Wilson's disease is the most common from a group of hereditary diseases that cause copper overload in the liver. All can cause cirrhosis at a young age. The other members of the group are Indian childhood cirrhosis (ICC), endemic Tyrolean infantile cirrhosis, and idiopathic copper toxicosis. These are not related to ATP7B mutations; for example, ICC has been linked to mutations in the KRT8 and the KRT18 genes.[15]
Pathophysiology
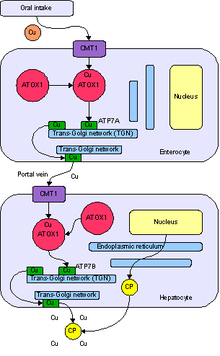
Copper is needed by the body for a
Copper enters the body through the
When the amount of copper in the liver overwhelms the proteins that normally bind it, it causes oxidative damage through a process known as
Why Wilson's disease causes hemolysis is unclear, but various lines of evidence suggest that a high level of free (nonceruloplasmin-bound) copper has a direct effect on either oxidation of hemoglobin, inhibition of energy-supplying enzymes in the red blood cell, or direct damage to cell membranes.[18]
Diagnosis
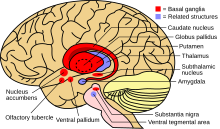
Wilson's disease may be suspected on the basis of any of the symptoms mentioned above, or when a close relative has been found to have Wilson's. Most have slightly abnormal
No totally reliable test for Wilson's disease is known, but levels of ceruloplasmin and copper in the blood, as well of the amount of copper excreted in urine during a 24-hour period, are together used to form an impression of the amount of copper in the body. The gold standard—or most ideal test—is a liver biopsy.[5]
Ceruloplasmin

Levels of ceruloplasmin are abnormally low (<0.2 g/L) in 80–95% of cases.
Serum and urine copper
Serum copper is low, which may seem paradoxical given that Wilson's disease is a disease of copper excess. However, 95% of plasma copper is carried by ceruloplasmin, which is often low in Wilson's disease. Urine copper is elevated in Wilson's disease and is collected for 24 hours in a bottle with a copper-free liner. Levels above 100 μg/24h (1.6 μmol/24h) confirm Wilson's disease, and levels above 40 μg/24h (0.6 μmol/24h) are strongly indicative.[5] High urine copper levels are not unique to Wilson's disease; they are sometimes observed in autoimmune hepatitis and in cholestasis (any disease obstructing the flow of bile from the liver to the small bowel).[14]
In children, the penicillamine test may be used. A 500 mg oral dose of penicillamine is administered, and urine collected for 24 hours. If this contains more than 1600 μg (25 μmol), it is a reliable indicator of Wilson's disease.[clarification needed] This test has not been validated in adults.[14]
Slit-lamp examination
The eyes of the patient are examined using a slit lamp to look for Kayser–Fleischer rings, which are strongly associated with Wilson's disease and are caused by copper deposition on the inner cornea in Descemet's membrane.[10]
Liver biopsy
Once other investigations have indicated Wilson's disease, the ideal test is the removal of a small amount of liver tissue through a liver biopsy. This is assessed microscopically for the degree of
In the earlier stages of the disease, the biopsy typically shows steatosis (deposition of fatty material), increased glycogen in the nucleus, and areas of necrosis (cell death). In more advanced disease, the changes observed are quite similar to those seen in autoimmune hepatitis, such as infiltration by inflammatory cells, piecemeal necrosis, and fibrosis (scar tissue). In advanced disease, finally, cirrhosis is the main finding. In acute liver failure, degeneration of the liver cells and collapse of the liver tissue architecture is seen, typically on a background of cirrhotic changes. Histochemical methods for detecting copper are inconsistent and unreliable, and taken alone are regarded as insufficient to establish a diagnosis.[14]
Genetic testing
Mutation analysis of the ATP7B gene, as well as other genes linked to copper accumulation in the liver, may be performed. Once a mutation is confirmed, family members can be screened for the disease as part of
Treatment
Diet
In general, a diet low in copper-containing foods is recommended with the avoidance of mushrooms, nuts, chocolate, dried fruit, liver, sesame seeds and sesame oil, and shellfish.[5]
Medication
Medical treatments are available for Wilson's disease. Some increase the removal of copper from the body, while others prevent the absorption of copper from the diet.
Generally, penicillamine is the first treatment used. This binds copper (
Once all results have returned to normal, zinc (usually in the form of a zinc acetate prescription called Galzin) may be used instead of chelators to maintain stable copper levels in the body. Zinc stimulates metallothionein, a protein in gut cells that binds copper and prevents its absorption and transport to the liver. Zinc therapy is continued unless symptoms recur or if the urinary excretion of copper increases.[14]
In rare cases where none of the oral treatments is effective, especially in severe neurological disease, dimercaprol (British anti-Lewisite) is occasionally necessary. This treatment is injected intramuscularly (into a muscle) every few weeks and has unpleasant side effects such as pain.[22]
People who are asymptomatic (for instance, those diagnosed through family screening or only as a result of abnormal test results) are generally treated, as the copper accumulation may cause long-term damage in the future. Whether these people are best treated with penicillamine or zinc acetate is unclear.[14]
Physical and occupational therapies
Transplantation
Liver transplantation is an effective cure for Wilson's disease, but is used only in particular scenarios because of the risks and complications associated with the procedure. It is used mainly in people with fulminant liver failure who fail to respond to medical treatment or in those with advanced chronic liver disease. Liver transplantation is avoided in severe neuropsychiatric illnesses, in which its benefit has not been demonstrated.[5][14]
Prognosis
Left untreated, Wilson's disease tends to become progressively worse and is eventually fatal. Serious complications include liver cirrhosis, acute kidney failure, and psychosis. Liver cancer and cholangiocarcinoma may occur, but at a lower incidence than other chronic liver diseases, and the risk is greatly reduced with treatment.[13] With early detection and treatment, most of those affected can live relatively normal lives and have a life expectancy close to that of the general population.[13] Liver and neurologic damage that occurs prior to treatment may improve, but it is often permanent.[24] Fertility is usually normal and pregnancy complications are not increased in those with Wilson's disease that is treated.[13]
History
The disease bears the name of
In 1951, Cumings, and New Zealand neurologist
The genetic basis of Wilson's disease, and its link to ATP7B mutations, was elucidated by several research groups in the 1980s and 1990s.[37][38]
In other animals
Hereditary copper accumulation has been described in Bedlington Terriers,[39] where it generally only affects the liver. It is due to mutations in the COMMD1 (or MURR1) gene.[40] Despite this findings, COMMD1 mutations could not be detected in humans with non-Wilsonian copper accumulation states (such as Indian childhood cirrhosis) to explain their genetic origin.[41]
See also
- Copper in health
References
- ^ a b c d e f g h i "Wilson Disease". NIDDK. July 2014. Archived from the original on 2016-10-04. Retrieved 2016-11-06.
- ISBN 9780683307238. Archivedfrom the original on 2016-11-07.
- ISBN 9780323431613. Archivedfrom the original on 2016-11-07.
- ^ "Whonamedit – dictionary of medical eponyms". www.whonamedit.com. Archived from the original on 2016-11-07. Retrieved 2016-11-06.
- ^ S2CID 24663871.
- ^ PMID 16709660.
- ^ "Wilson's disease - Symptoms and causes". Mayo Clinic. Retrieved 2022-10-05.
- ^ S2CID 2989668.
- ISBN 978-1451142631.
- ^ PMID 29083643. Retrieved 30 November 2022.
- PMID 18506894.
- ISBN 978-0323057516.
- ^ S2CID 261581755.
- ^ S2CID 263620.
- ^ PMID 17717039.
- PMID 32493955.
- S2CID 37186426.
- ISBN 978-0-683-18242-2.
- S2CID 24055787.
- S2CID 205340375.
- S2CID 10124665.
- ^ PMID 8759497.
- PMID 15777568.
- ^ "Definition and Facts | NIDDK". National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved 2019-02-01.
- .
- ^ PMID 10681092.
- ^ Homén EA (1892). "Eine eigenthümliche bei drei Geschwistern auftretende typische Krankheit unter der Form einer progressiven Dementia in Verbindung mit ausgedehnten Gefässveränderungen (wohl Lues hereditaria tarda)". Archiv für Psychiatrie und Nervenkrankheiten. 24: 1–38.
- PMID 18124738.
- PMID 6018274.
- PMID 14830662.
- PMID 14882450.
- PMID 12297577.
- PMID 13279157.
- S2CID 205999334.
- S2CID 11546705.
- PMID 10632959. Archived from the originalon 2008-04-09. Retrieved 2008-05-20.
- S2CID 1236890.
- S2CID 610188.
- PMID 122681.
- PMID 11809725.
- PMID 12547404.
External links
- Wilson's disease at Curlie
- Wilson disease at NLMGenetics Home Reference



