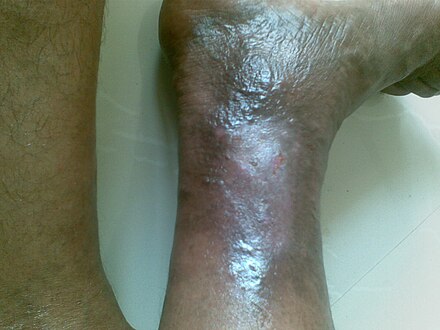
Venous ulcer
| Venous ulcer | |
|---|---|
| Other names | Venous insufficiency ulceration, stasis ulcer, stasis dermatitis, varicose ulcer, ulcus cruris, crural ulceration |
 | |
| Venous ulcer on the back of the right leg | |
| Specialty | Dermatology |
Venous ulcer is defined by the
Exercise, together with
Signs and symptoms
Signs and symptoms of venous ulcers include:[citation needed]
- Moderate pain, which improves on elevation (unlike arterial ulcers which worsen with elevation)
- Irregular, sloping edges
- Associated oedema, due to increased hydrostatic pressure, which contributes to 'atrophie blanche'
- 'Atrophie blanche', localised loss of skin pigmentation due to death of erythrocytes and scarring
- Lipodermatosclerosis, a hardening of the skin which can lead to an "inverted champagne bottle" appearance to the leg
- Associated superficial varicose veins or "ankle flare", a collection of small, dark, engorged superficial veins[7]
-
Venous ulcer before surgery
-
Healing process of a chronic venous stasis ulcer of the lower leg
-
Healing venous ulcer after one month

Pathophysiology
The exact cause of venous ulcers is not certain, but a common denominator is generally
Venous
It is in the
Wounds of the distal lower extremities arising from causes not directly related to venous insufficiency (e.g., scratch, bite, burn, or surgical incision) may ultimately fail to heal if underlying (often undiagnosed) venous disease is not properly addressed.[citation needed]
Diagnosis

Classification
A clinical severity score has been developed to assess chronic venous ulcers. It is based on the CEAP (clinical, etiology, anatomy, and pathophysiology) classification system developed by an expert panel. A high score gives a poor prognosis.[15]
Distinction from arterial ulcer
A venous ulcer tends to occur on the medial side of the leg, typically around the
Differential diagnosis
Leg ulcerations may result from various pathologic processes. Common causes of leg ulcerations include
Prevention
Compression stockings appear to prevent the formation of new ulcers in people with a history of venous ulcers.[16][needs update]
Treatment
The main aim of the treatment is to create such an environment that allows skin to grow across an ulcer. In the majority of cases this requires finding and treating underlying venous reflux. The National Institute for Health and Care Excellence (NICE) recommends referral to a vascular service for anyone with a leg ulcer that has not healed within two weeks or anyone with a healed leg ulcer.[17]
Most venous ulcers respond to patient education, elevation of foot, elastic compression, and evaluation (known as the Bisgaard regimen).
The recommendations of dressings to treat venous ulcers vary between the countries. Antibiotics are often recommended to be used only if so advised by the physician due to emergence of resistance of bacteria to antibiotics. This is an issue on venous ulcers as they tend to heal slower than acute wounds for example. Natural alternatives that are suitable for the longer term use exists on the market such as honey and
There is uncertain evidence whether alginate dressing is effective in the healing of venous ulcer when compared to hydrocolloid dressing or plain non-adherent dressing.[23]
It is uncertain whether therapeutic ultrasound improve the healing of venous ulcer.[24]
Compression therapy
Non-elastic, ambulatory, below knee (BK) compression counters the impact of reflux on venous pump failure.
A 2021
Intermittent pneumatic compression devices may be used, but it is not clear that they are superior to simple compression dressings.[31]
It is not clear if interventions that are aimed to help people adhere to compression therapy are effective.[32] More research is needed in this field.
Medications
Pentoxifylline is a useful add on treatment to compression stockings and may also help by itself.[33] It works by reducing platelet aggregation and thrombus formation. Gastrointestinal disturbances were reported as a potential adverse effect.[33]
Sulodexide, which reduces the formation of blood clots and reduces inflammation, may improve the healing of venous ulcers when taken in conjunction with proper local wound care.[34] Further research is necessary to determine potential adverse effects, the effectiveness, and the dosing protocol for sulodexide treatment.[citation needed]
An oral dose of aspirin is being investigated as a potential treatment option for people with venous ulcers. A 2016 Cochrane systematic review concluded that further research is necessary before this treatment option can be confirmed to be safe and effective.[35]
Oral zinc supplements have not been proven to be effective in aiding the healing of venous ulcers, however more research is necessary to confirm these results.[36]
Treatments aimed at decreasing protease activity to promote healing in chronic wounds have been suggested, however, the benefit remains uncertain.[37] There is also lack of evidence on effectiveness on testing for elevated proteases in venous ulcers and treating them with protease modulating treatment.[38] There is low certainty evidence that protease modulating matrix treatment is helpful in the healing of venous ulcer.[39]
Flavonoids may be useful for treating venous ulcers but the evidence needs to be interpreted cautiously.[40]
Wound Cleansing Solutions
There is insufficient evidence to determine if cleaning wounds is beneficial or whether wound cleaning solutions (polyhexamethylene biguanide, aqueous oxygen peroxide, etc.) are better than sterile water or saline solutions to help venous leg ulcers heal.[41] It is uncertain whether the choice of cleaning solution or method of application makes any difference to venous leg ulcer healing.[41]
Skin grafts and artificial skin
Two layers of skin created from animal sources as a
Artificial skin, made of collagen and cultured skin cells, is also used to cover venous ulcers and excrete growth factors to help them heal.[43] A systematic review found that bilayer artificial skin with compression bandaging is useful in the healing of venous ulcers when compared to simple dressings.[42]
Surgery
A randomized controlled trial found that surgery "reduces the recurrence of ulcers at four years and results in a greater proportion of ulcer free time".[44]
Local anaesthetic endovenous surgery using the
Endovenous ablation, in combination with compression, on superficial venous incompetence has been shown (high quality evidence) to improve leg ulcer healing when compared to compression alone.[46] The use of subfascial endoscopic perforator surgery is uncertain in the healing of venous ulcer.[47]
Dressings
It is not certain which dressings and topical agents are most effective for healing venous leg ulcers.[48][49] Silver-containing dressings may increase the probability of healing for venous leg ulcers.[48] A clinical trial was successfully performed with a mixture of 60% sugar or glucose powder and 40% vaseline.[50] A 2013 Cochrane systematic review aimed to determine the effectiveness of foam dressings for helping to heal venous leg ulcers. The authors concluded that is uncertain whether or not foam dressings are more effective than other dressing types and that more randomized controlled trials are needed to help answer this research question.[51] However, there is some evidence that ibuprofen dressings may offer pain relief to people with venous leg ulcers.[52]
Prognosis
Venous ulcers are costly to treat, and there is a significant chance that they will recur after healing;[3][10] one study found that up to 48% of venous ulcers had recurred by the fifth year after healing.[10] However treatment with local anaesthetic endovenous techniques suggests a reduction of this high recurrence rate is possible.[45]
Without proper care, the ulcer may get infected leading to cellulitis or gangrene and eventually may need amputation of the part of limb in future.[citation needed]
Some topical drugs used to treat venous ulcer may cause
Research
The current 'best' practice in the UK is to treat the underlying venous reflux once an ulcer has healed. It is questionable as to whether endovenous treatment should be offered before ulcer healing, as current evidence would not support this approach as standard care. The EVRA (Early Venous Reflux Ablation) ulcer trial, a randomised clinical trial funded by the National Institute for Health and Care Research (NIHR) to compare early versus delayed endovenous treatment of superficial venous reflux in patients with chronic venous ulceration, opened for recruitment in October 2013. The study hopes to show an increase in healing rates from 60% to 75% at 24 weeks.[54]
Research from the University of Surrey and funded by the Leg Ulcer Charity looked at the psychological impact of having a leg ulcer, on the relatives and friends of the affected person, and the influence of treatment.[55]
References
- PMID 24974070.
- OCLC 968428064.
- ^ PMID 26358303.
- S2CID 206018724.
- ^ PMID 30285080.
- ^ NICE (July 23, 2013). "Varicose veins in the legs: The diagnosis and management of varicose veins. 1.2 Referral to a vascular service". National Institute for Health and Care Excellence. Retrieved June 15, 2019.
- OCLC 923846134.
- ^ "Chronic Venous Insufficiency (CVI)". Cleveland Clinic. Last reviewed by a Cleveland Clinic medical professional on 05/14/2019.
- PMID 28450810.
- ^ PMID 15223495.
- ^ PMID 15147994.
- ^ PMID 15818347.
- ^ PMID 16171604.
- ^ a b "eMedicine - Reperfusion Injury in Stroke : Article by Wayne M Clark, MD". Retrieved 2007-08-05.
- PMID 15622385.
- PMID 25203307.
- ^ NICE (July 23, 2013). "Varicose veins in the legs: The diagnosis and management of varicose veins. 1.2 Referral to a vascular service". National Institute for Health and Care Excellence. Retrieved August 25, 2014.
- S2CID 5218584.
- ^ PMID 24408354.
- PMID 25742878.
- PMID 20559190.
- ^ "Regulation (Eu) 2017/745 of the European Parliament and of the Council on medical devices". Official Journal of the European Union. 5 April 2017.
- PMID 26286189.
- PMID 28504325.
- PMID 15885771.
- ^ PMID 34308565.
- ^ PMID 16973096.
- PMID 17012004.
- PMID 17631512.
- PMID 26094638.
- PMID 24820100.
- PMID 26932818.
- ^ PMID 23235582.
- PMID 27251175.
- PMID 26889740.
- PMID 25202988.
- PMID 30171767.
- PMID 26771894.
- PMID 27977053.
- PMID 23728661.
- ^ PMID 33734426.
- ^ PMID 23440784.
- ^ Mustoe T (March 17–18, 2005). Dermal ulcer healing: Advances in understanding. Tissue repair and ulcer/wound healing: molecular mechanisms, therapeutic targets and future directions. Paris, France.
- PMID 17545185.
- ^ S2CID 9186619.
- PMID 37497816.
- PMID 30827037.
- ^ PMID 29906322.
- PMID 35930364.
- ^ Anti-Infective Effects of Sugar-Vaseline Mixture on Leg Ulcers
- PMID 23728697.
- PMID 23152206.
- ISBN 978-0-340-76232-5.
- ^ Davies A, Heatley F. "EVRA (Early Venous Reflux Ablation) Ulcer Trial". Faculty of Medicine Imperial College London.
- ^ Tollow P (April 2014). "Impact of Leg Ulcers on Relatives and Carers of Affected Patients - A PhD Study funded by The Leg Ulcer Charity". The Leg Ulcer Charity. Archived from the original on August 26, 2014. Retrieved August 25, 2014.