Balamuthia mandrillaris
This article needs additional citations for verification. (April 2021) |
| Balamuthia mandrillaris | |
|---|---|
| |
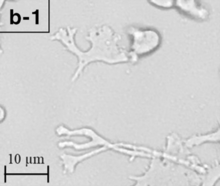
| Trophozoite (active) form of Balamuthia mandrillaris | |

| |
| A Balamuthia mandrillaris cyst | |
| Scientific classification | |
| Domain: | Eukaryota |
| Phylum: | |
| Class: | |
| Order: | Centramoebida |
| Family: | Balamuthiidae
|
| Genus: | Balamuthia Visvesvara et al., 1993
|
| Species: | B. mandrillaris
|
| Binomial name | |
| Balamuthia mandrillaris Visvesvara et al., 1993
| |
Balamuthia mandrillaris is a free-living
B. mandrillaris can infect the body through open wounds or possibly by inhalation.
The generic name Balamuthia was given by
Morphology
B. mandrillaris is a free-living, heterotrophic amoeba, consisting of a standard complement of organelles surrounded by a three-layered cell wall (thought to be made of cellulose), and with an abnormally large cell nucleus. On average, a Balamuthia trophozoite is about 30 to 120 μm in diameter. The cysts fall around this range, as well.[8]
Life cycle
Balamuthia's lifecycle, like the Acanthamoeba, consists of a cystic stage and a non-flagellated trophozoite stage, both of which are infectious, and both of which can be identified in the brain tissue on microscopic examination of brain biopsies performed on infected individuals. The trophozoite is pleomorphic and uninucleated, but binucleated forms are occasionally seen. Cysts are also uninucleated, possessing three walls: an outer thin irregular ectocyst, an inner thick endocyst, and a middle amorphous fibrillar mesocyst.[9]
Pathology
B. mandrillaris is larger than human leukocytes, thus making
Balamuthia may also cause a variety of non-neurological symptoms, including skin
Culturing and identification
Vero cells have been suggested as a possible cheaper and faster alternative to culture the organism.[15] Several types of animal cells have been used in B. mandrillaris culturing including rat glioma cells, human lung cells, and human brain microvascular endothelial cells.[13] These animal cells are added to a specified axenic growth medium for culturing. At the same time, and xenic culture is also performed to help differentiate between Balamuthia and other amebae.[13]
Axenic culture methods have also been reported within the last decade [16][17]
Treatment
Infection seems to be survivable if treated early. Two individuals, a 5-year-old girl and a 64-year-old man, developed GAE. After diagnosis, they were treated with flucytosine, pentamidine, fluconazole, sulfadiazine, a macrolide antibiotic and trifluoperazine. Both patients recovered.[18] In 2018, an unsuccessful attempt at treatment of a Balamuthia infection after nasal lavage with untreated tap water was reported.[19]
Nitroxoline has shown interesting properties in vitro and might be a possible treatment for this infection.[20] A man treated with nitroxoline at
Organ transplantation
According to a report published in Morbidity and Mortality Weekly Report in September 2010, two confirmed cases of Balamuthia transmission occurred through organ transplantation in December 2009 in Mississippi.[23] Two kidney recipients, a 31-year-old woman and a 27-year-old man, suffered from post-transplant encephalitis due to Balamuthia. The woman died in February 2010 and the man survived with partial paralysis of his right arm. The CDC was notified by a physician on December 14, 2009, about possible transplant transmission in these two patients. Histopathologic testing of donor and recipient tissues confirmed the transmission. Two other patients who received heart and liver transplants from the same donor, but in different hospitals, were placed on preemptive therapy and remain unaffected. A second cluster of transplant-transmitted Balamuthia in Arizona was reported in the same weekly report. Four recipients were identified, two from Arizona (liver and kidney-pancreas), one from California (kidney), and another from Utah (heart). Recipients from Arizona—a 56-year-old male and a 24-year-old male—both succumbed to GAE within a span of 40 days from transplantation. The other two were placed on preemptive therapy after the first two were reported and remain unaffected.[24]
References
- PMID 19621290.
- PMID 30239654.
- PMID 2280005.
- ^ "Balamuthia mandrillaris ameba infection". Centers for Disease Control and Prevention. Retrieved 14 June 2014.
- PMID 12843060.
- PMID 15347743. Archived from the original(PDF) on 2018-07-27. Retrieved 2017-06-20.
- PMID 25040661.
- PMID 25709948.
- ISBN 978-0-7020-3935-5. Retrieved 6 September 2016.
- ^ Abdul Mannan Baig. Pathogenesis of amoebic encephalitis: Are the amoebas being credited to an 'inside job' done by the host immune response? Acta Trop. 2015 Apr
- PMID 1456885.
- S2CID 28069984.
- ^ PMID 34765527.)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - PMID 11232763.
- PMID 26620704.
- PMID 37234530.)
{{cite journal}}: CS1 maint: multiple names: authors list (link - PMID 25957459.)
{{cite journal}}: CS1 maint: multiple names: authors list (link - PMID 14583863.
- PMID 30243910.
- PMID 30377287.
- . Retrieved 10 February 2023.
- PMID 36573629.
- PMID 20847719.
- PMID 20847722.
- Baig, Abdul Mannan. "Can Neurotropic Free-Living Amoeba Serve as a Model to Study SARS-CoV-2 Pathogenesis?" ACS Chemical Neuroscience., vol. 11, no. 22, 2020, pp. 3697–3700., doi:10.1021/acschemneuro.0c00653.
External links
- Balamuthia | Parasites | CDC for images: Cyst of B. mandrillaris and Trophozoite of B. mandrillaris in culture. Credit: DPDx
