Langerhans cell histiocytosis
| Langerhans cell histiocytosis | |
|---|---|
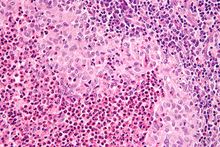 | |
| Micrograph showing a Langerhans cell histiocytosis with the characteristic reniform Langerhans cells accompanied by abundant eosinophils. H&E stain. | |
| Specialty | Hematology |
Langerhans cell histiocytosis (LCH) is an abnormal clonal proliferation of Langerhans cells, abnormal cells deriving from bone marrow and capable of migrating from skin to lymph nodes.
Symptoms range from isolated bone lesions to multisystem disease.[1] LCH is part of a group of syndromes called histiocytoses, which are characterized by an abnormal proliferation of histiocytes (an archaic term for activated dendritic cells and macrophages).[2] These diseases are related to other forms of abnormal proliferation of white blood cells, such as leukemias and lymphomas.[3]
The disease has gone by several names, including
Classification
| Alternative names |
|---|
| Histiocytosis X
Histiocytosis X syndrome |
| Subordinate terms |
| Hand-Schüller-Christian disease
Letterer-Siwe disease |
The disease spectrum results from
LCH is clinically divided into three groups: unifocal, multifocal unisystem, and multifocal multisystem.[7]
Unifocal
Unifocal LCH, also called eosinophilic granuloma (an older term which is now known to be a misnomer), is a disease characterized by an expanding proliferation of Langerhans cells in one organ, where they cause damage called lesions. It typically has no extraskeletal involvement, but rarely a lesion can be found in the skin, lungs, or stomach. It can appear as a single lesion in an organ, up to a large quantity of lesions in one organ. When multiple lesions are scattered throughout an organ, it can be called a multifocal unisystem variety. When found in the lungs, it should be distinguished from Pulmonary Langerhans cell hystiocytosis—a special category of disease most commonly seen in adult smokers.[8] When found in the skin it is called cutaneous single system Langerhans cell LCH. This version can heal without therapy in some rare cases.[9] This primary bone involvement helps to differentiate eosinophilic granuloma from other forms of Langerhans Cell Histiocytosis (Letterer-Siwe or Hand-Schüller-Christian variant).[10]
Multifocal unisystem
Seen mostly in children, multifocal unisystem LCH is characterized by fever, bone lesions and diffuse eruptions, usually on the scalp and in the ear canals. 50% of cases involve the
Multifocal multisystem
Multifocal multisystem LCH, also called
Pulmonary Langerhans cell histiocytosis (PLCH)
Pulmonary Langerhans cell histiocytosis (PLCH) is a unique form of LCH in that it occurs almost exclusively in cigarette smokers. It is now considered a form of smoking-related interstitial lung disease. PLCH develops when an abundance of monoclonal CD1a-positive Langerhans (immature histiocytes) proliferate the bronchioles and alveolar interstitium, and this flood of histiocytes recruits granulocytes like eosinophils and neutrophils and agranulocytes like lymphocytes further destroying bronchioles and the interstitial alveolar space that can cause damage to the lungs.[13] It is hypothesized that bronchiolar destruction in PLCH is first attributed to the special state of Langerhans cells that induce cytotoxic T-cell responses, and this is further supported by research that has shown an abundance of T-cells in early PLCH lesions that are CD4+ and present early activation markers.[14] Some affected people recover completely after they stop smoking, but others develop long-term complications such as pulmonary fibrosis and pulmonary hypertension.[15]
Signs and symptoms

LCH provokes a non-specific inflammatory response, which includes fever, lethargy, and weight loss. Organ involvement can also cause more specific symptoms.
- Bone: The most-frequently seen symptom in both unifocal and multifocal disease is painful bone swelling. The skull is most frequently affected, followed by the long bones of the upper extremities and flat bones. Infiltration in hands and feet is unusual. Osteolytic lesions can lead to pathological fractures.[16]
- Skin: Commonly seen are a rash which varies from scaly erythematous lesions to red papules pronounced in intertriginous areas. Up to 80% of LCH patients have extensive eruptions on the scalp.
- Bone marrow: Pancytopenia with superadded infection usually implies a poor prognosis. Anemia can be due to a number of factors and does not necessarily imply bone marrow infiltration.
- Lymph node: Enlargement of the liver in 20%, spleen in 30% and lymph nodes in 50% of Histiocytosis cases.[17]
- Hypothalamic pituitary axis commonly involved.[18] Diabetes insipidus is most common.[19] Anterior pituitary hormone deficiency is usually permanent.[20]
- Lungs: some patients are asymptomatic, diagnosed incidentally because of lung nodules on radiographs; others experience chronic cough and shortness of breath.[21]
- Less frequently gastrointestinal tract, central nervous system, and oral cavity.[22]
Pathophysiology
The pathogenesis of Langerhans cell histiocytosis (LCH) is a matter of debate. There are ongoing investigations to determine whether LCH is a reactive (non-cancerous) or neoplastic (cancerous) process. Arguments supporting the reactive nature of LCH include the occurrence of spontaneous remissions, the extensive secretion of multiple cytokines by dendritic cells and bystander-cells (a phenomenon known as cytokine storm) in the lesional tissue, favorable prognosis and relatively good survival rate in patients without organ dysfunction or risk organ involvement.[23][24]
On the other hand, the infiltration of organs by monoclonal population of pathologic cells, and the successful treatment of subset of disseminated disease using chemotherapeutic regimens are all consistent with a neoplastic process.[25][26][27] In addition, a demonstration, using X chromosome–linked DNA probes, of LCH as a monoclonal proliferation provided additional support for the neoplastic origin of this disease.[28] While clonality is an important attribute of cancer, its presence does not prove that a proliferative process is neoplastic. Recurrent cytogenetic or genomic abnormalities would also be required to demonstrate convincingly that LCH is a malignancy.[29]
An activating somatic mutation of a proto-oncogene in the
Diagnosis
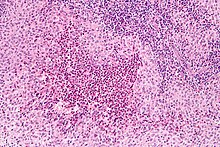
Diagnosis is confirmed
Imaging may be evident in
Assessment of
- peanut agglutinin (PNA) is expressed on the cell surface and perinuclearly[39][40]
- major histocompatibility (MHC) class II is expressed (because histiocytes are macrophages)
- CD1a[37]
- CD207), a Langerhans Cell–restricted protein that induces the formation of Birbeck granules and is constitutively associated with them, is a highly specific marker.[41][42]
Treatment
Guidelines for management of patients up to 18 years with Langerhans cell histiocytosis have been suggested.
Prognosis
There is a general excellent prognosis for the disease as those with localized disease have a long life span. With multi-focal disease 60% have a chronic course, 30% achieve remission and mortality is up to 10%.[47] A full recovery can be expected for people who seek treatment and do not have more lesions at 12 and 24 months. However, 50% of children under 2 with disseminated Langerhans cell histiocytosis die of the disease. The prognosis rate decreases for patients who experience lung involvement. Whereas patients with skin and a solitary lymph node involvement generally have a good prognosis.[48] Although there is a general good prognosis for Langerhans cell histiocytosis, approximately 50% of patients with the disease are prone to various complications such as musculoskeletal disability, skin scarring and diabetes insipidus.[48]
Prevalence
LCH usually affects children between 1 and 15 years old, with a peak incidence between 5 and 10 years of age. Among children under the age of 10, yearly incidence is thought to be 1 in 200,000;[49] and in adults even rarer, in about 1 in 560,000.[50] It has been reported in elderly but is vanishingly rare.[51] It is most prevalent in Caucasians, and affects males twice as often as females.[52] In other populations too the prevalence in males is slightly more than in females.[53]
LCH is usually a sporadic and non-
Culture
In the 10th episode of season 3 of
Nomenclature
Langerhans cell histiocytosis is occasionally misspelled as "Langerhan" or "Langerhan's" cell histiocytosis, even in authoritative textbooks. The name, however, originates back to its discoverer, Paul Langerhans.[56]
References
- ^ a b "Langerhans Cell Histiocytosis". NORD (National Organization for Rare Disorders). Retrieved 5 December 2020.
- ^ "UpToDate". UpToDate. Retrieved October 18, 2023.
- PMID 15925822.
- S2CID 54351490.(subscription required)
- S2CID 7878051.
- ISBN 978-0-7216-6795-9.
- ISBN 978-0-8089-2302-2.
- ISBN 978-1-4557-2613-4.
- PMID 28977321.
- ISBN 978-1-4377-0755-7.
- PMID 22028518.
- ^ Langerhans Cell Histiocytosis at eMedicine
- PMID 20617216.
- S2CID 5626880.
- PMID 20617216.
- PMID 1636041.
- ^ "Langerhans Cell Histiocytosis — Patient UK". Retrieved 2007-05-10.
- PMID 10770168.
- S2CID 11069765.
- PMID 8412998.
- S2CID 19702745.
- PMID 26722570.
- S2CID 46217705.
- PMID 16487180.
- S2CID 34121488.
- PMID 19908293.
- PMID 10531573.
- PMID 8008029.
- PMID 19726802.
- PMID 20519626.
- PMID 22506009.
- ^ Peters, Tricia L.; Tsz-Kwong Chris Man; Price, Jeremy; George, Renelle; Phaik Har Lim; Kenneth Matthew Heym; Merad, Miriam; McClain, Kenneth L.; Allen, Carl E. (10 December 2011). "1372 Frequent BRAF V600E Mutations Are Identified in CD207+ Cells in LCH Lesions, but BRAF Status does not Correlate with Clinical Presentation of Patients or Transcriptional Profiles of CD207+ Cells".
Oral and Poster Abstracts presented at 53rd ASH Annual Meeting and Exposition
{{cite journal}}: Cite journal requires|journal=(help) - PMID 36158441.
- PMID 28613635. Retrieved October 18, 2023.
- PMID 26461147.
- PMID 10770168.
- ^ S2CID 70911084.
- PMID 9596268.
- S2CID 32685876.
- PMID 2239828.
- PMID 10661407.
- S2CID 40092500.
- PMID 23109216.
- PMID 23672541.
- ^ "Langerhans cell histiocytosis — Histiocyte Society Evaluation and Treatment Guidelines". April 2009. Archived from the original on 2018-01-21. Retrieved 2015-04-28.
{{cite journal}}: Cite journal requires|journal=(help) - PMID 6969347.
- ^ a b Tillotson CV, Anjum F, Patel BC. Langerhans Cell Histiocytosis. [Updated 2022 Jul 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430885/
- ^ "MedlinePlus Medical Encyclopedia: Histiocytosis". Retrieved 2007-05-10.
- ^ "Histiocytosis Association of Canada". Archived from the original on 2007-05-14. Retrieved 2007-05-16.
- S2CID 20706403.
- PMID 10365975.
- PMID 14556926.
- PMID 17224372.
- ^ House (season 3) In CSI, season 15 episode 4, a student has LCH.
- PMID 11919207.
