Cysteamine
 | |
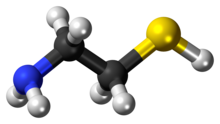 Skeletal formula (top) Ball-and-stick model of the cysteamine | |
| Clinical data | |
|---|---|
| Trade names | Cystagon, Procysbi, Cystaran, others |
| Other names | 2-Aminoethanethiol, β-Mercaptoethylamine, 2-Mercaptoethylamine, decarboxycysteine, thioethanolamine, mercaptamine bitartrate, cysteamine (USAN US) |
| AHFS/Drugs.com | Micromedex Detailed Consumer Information |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth, eye drops |
| ATC code | |
| Legal status | |
| Legal status | |
| Identifiers | |
| |
JSmol) | |
| Melting point | 95 to 97 °C (203 to 207 °F) |
| |
| |
Cysteamine is an
It is biosynthesized in mammals, including humans, by the degradation of coenzyme A. It is the biosynthetic precursor to the neurotransmitter hypotaurine.[14][13]
Medical uses
As a medication, cysteamine, sold under the brand name Cystagon among others, is indicated to treat cystinosis, a lysosomal storage disease characterized by the abnormal accumulation of cystine, the oxidized dimer of the amino acid cysteine.[15][6][7][8] It removes the excessive cystine that builds up in cells of people with the disease.[13] It is available by mouth (capsule and extended release capsule) and in eye drops.[16][8][9][6][10][7][11][17]
When applied topically it can lighten skin that's been darkened as a result of post-inflammatory hyperpigmentation, sun exposure and Melasma.[18][19][20][21] Tentative evidence suggests that it may be a more effective depigmentation agent than hydroquinone, retinoids and topical corticosteroids in individuals with chronic skin discoloration.[22][23][24] Topical application of cysteamine cream has also demonstrated similar efficacy to intradermal tranexamic acid injections for the treatment of Melasma but with much fewer adverse effects.[25]
Adverse effects
Topical use
The most important adverse effect related to topical use might be skin irritation.[medical citation needed] However it's significantly better tolerated than alternative skin lightening treatments with similar efficacy.[24][25]
Oral use
The label for oral formulations of cysteamine carry warnings about symptoms similar to
Additional adverse effects of oral cysteamine include bad breath, skin odor, vomiting, nausea, stomach pain, diarrhea, and loss of appetite.[8]
The risks of cysteamine to a fetus are not known but it harms babies in animal models at doses less than those given to people.[6][7]
For eye drops, the most common adverse effects are sensitivity to light, redness, and eye pain, headache, and visual field defects.[7]
Interactions
There are no drug interactions for normal capsules or eye drops,
Pharmacology
People with cystinosis lack a functioning transporter (cystinosin) which transports cystine from the lysosome to the cytosol. This ultimately leads to buildup of cystine in lysosomes, where it crystallizes and damages cells.[16] Cysteamine enters lysosomes and converts cystine into cysteine and cysteine-cysteamine mixed disulfide, both of which can exit the lysosome.[8]
Cysteamine also promotes the transport of L-cysteine into cells.[13]
Society and culture
It is approved by the U.S. Food and Drug Administration (FDA) and the European Medicines Agency (EMA).[16][8][9][10][11][26][27]
In 2013, the regular capsule of cysteamine cost about $8,000 per year; the extended release form that was introduced that year was priced at $250,000 per year.[28]
History
The therapeutic effect of cysteamine on cystinosis was reported in the 1950s. Cysteamine was approved as a drug for cystinosis in the US in 1994.[8] An extended release form was approved in 2013.[28]
Research
It was studied in in vitro and animal models for
In the 1970s it was tested in clinical trials for
Clinical trials in Huntington's disease were begun in the 1990s and were ongoing as of 2015.[13][29]
As of 2013[update], it was in clinical trials for Parkinson's disease, malaria, radiation sickness, neurodegenerative disorders, neuropsychiatric disorders, and cancer treatment.[13][needs update]
It has been studied in clinical trials for pediatric
References
- ^ "CYSTADROPS : Cysteamine Ophthalmic Solution" (PDF). Pdf.hres.ca. Archived (PDF) from the original on 10 June 2022. Retrieved 8 June 2022.
- ^ "Genetic disorders". Health Canada. 9 May 2018. Retrieved 13 April 2024.
- ^ "Cystagon 150 mg hard capsules - Summary of Product Characteristics (SmPC)". Medicines.org.uk. 19 June 2019. Archived from the original on 9 June 2021. Retrieved 28 April 2020.
- ^ "Cystadrops 3.8 mg/mL eye drops solution - Summary of Product Characteristics (SmPC)". (emc). 19 June 2019. Archived from the original on 9 June 2020. Retrieved 9 June 2020.
- ^ "Procysbi 25 mg gastro-resistant hard capsules - Summary of Product Characteristics (SmPC)". Medicines.org.uk. 17 September 2019. Archived from the original on 22 January 2021. Retrieved 9 June 2020.
- ^ a b c d e "Cystagon- cysteamine bitartrate capsule". DailyMed. 29 January 2019. Archived from the original on 25 March 2021. Retrieved 27 April 2020.
- ^ a b c d e f "Cystaran- cysteamine hydrochloride solution". DailyMed. 22 November 2019. Archived from the original on 24 March 2021. Retrieved 27 April 2020.
- ^ a b c d e f g h i j "Procysbi- cysteamine bitartrate capsule, delayed release pellets Procysbi- cysteamine bitartrate granule, delayed release". DailyMed. U.S. National Library of Medicine. 23 March 2020. Archived from the original on 25 March 2021. Retrieved 27 April 2020.
- ^ a b c "Procysbi EPAR". European Medicines Agency (EMA). Archived from the original on 4 August 2020. Retrieved 27 April 2020.
- ^ a b c "Cystagon EPAR". European Medicines Agency (EMA). Archived from the original on 11 November 2020. Retrieved 27 April 2020.
- ^ a b c "Cystadrops EPAR". European Medicines Agency (EMA). Archived from the original on 4 August 2020. Retrieved 27 April 2020.
- ^ Reid EE (1958). Organic Chemistry of Bivalent Sulfur. Vol. 1. New York: Chemical Publishing Company, Inc. pp. 398–399.
- ^ PMID 23416144.
- ISBN 9780323162081. Archivedfrom the original on 7 June 2021. Retrieved 11 January 2017.
- PMID 12110740.
- ^ from the original on 5 April 2011. Retrieved 11 January 2017.
- PMID 25336909.
- . Retrieved 10 October 2021.
- ^ "Cysteamine cream". DermNet NZ. Archived from the original on 29 June 2021. Retrieved 29 June 2021.
- PMID 30809577.
- S2CID 21618233.
- S2CID 222163129.
- S2CID 54481706.
- ^ S2CID 220078010.
- ^ a b Hilton L (14 October 2020). "Cysteamine cream, tranexamic acid mesotherapy reveal similar efficacy, different safety". Dermatology Times. Archived from the original on 29 June 2021. Retrieved 29 June 2021.
- ^ "Drug Approval Package: Cystaran (cysteamine) NDA #200740". U.S. Food and Drug Administration (FDA). 26 August 2013. Archived from the original on 9 June 2020. Retrieved 9 June 2020.
- ^ "Drug Approval Package: PROCYSBI (cysteamine bitartrate) Delayed-Release Capsules NDA #203389". U.S. Food and Drug Administration (FDA). 24 December 1999. Archived from the original on 9 June 2020. Retrieved 9 June 2020.
- ^ a b Pollack A (30 April 2013). "F.D.A. Approves Raptor Drug for Form of Cystinosis". The New York Times. Archived from the original on 10 September 2021. Retrieved 26 February 2017.
- S2CID 31037666.
- S2CID 21263419.
