Hereditary coproporphyria
| Hereditary coproporphyria | |
|---|---|
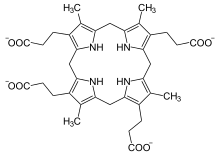 | |
| Coproporphyrinogen III | |
| Specialty | Endocrinology |
Hereditary coproporphyria (HCP) is a disorder of
Signs and symptoms
Clinically, patients affected with HCP present similarly to those with other acute porphyrias, such as
Individuals with HCP may be asymptomatic in the absence of triggering factors. Common triggers include certain drugs, alcohol, hormonal changes, and dietary changes.
Genetics
HCP is caused by mutations in CPOX, which codes for the enzyme
Individuals who are homozygous for a specific mutation (K404E) or compound heterozygous with a
Diagnosis
The diagnosis of any porphyria is often delayed due to the rarity of the disease as well as the varied and non-specific findings that patients present with. Bedside measurement of urine porphobilinogen is recommended as a screening test for patients suspected of having an acute porphyria. Elevated porphobilinogen is indicative of an acute porphyria, and additional testing can be done to narrow down the specific type.[3][7]
The identification of a specific porphyria is based on the results of laboratory findings, including
Elevated coproporphyrin is a common finding in urine, known as coproporphyrinuria as it is the predominant porphyrin species in urine. This is a non-specific finding that is not necessarily due to an acute porphyria. Coproporphyrinuria can be caused by other stressors to the heme biosynthetic pathway, such as liver disease, lead poisoning and certain bone marrow disorders.[9]
Treatment
There is no cure for HCP caused by the deficient activity of coproporphyrinogen oxidase. Treatment of the acute symptoms of HCP is the same as for other acute porphyrias. Intravenous hemin (as heme arginate or hematin) is the recommended therapy for acute attacks.[3][7] Acute attacks can be severe enough to cause death if not treated quickly and correctly. Hospitalization is typically required for administration of hemin, and appropriate drug selection is key to avoid exacerbating symptoms with drugs that interact poorly with porphyrias.[3] Proper drug selection is most difficult when it comes to treatment of the seizures that can accompany HCP, as most anti-seizure medications can make the symptoms worse. Gabapentin and levetiracetam are two anti-seizure drugs that are thought to be safe.[3]
In patients where management of symptoms is difficult even with hemin,
Long term treatment of acute porphyrias is centered on the avoidance of acute attacks by eliminating precipitating factors, such as drugs, dietary changes, and infections.[7] Females often have attacks coincident with their menstrual cycle, which can be managed effectively with hormonal birth control.[3] Because of the reduced penetrance of HCP, family members of a patient may carry the same mutation without ever presenting with symptoms. Molecular analysis of CPOX is the best way to identify these patients, as they will not express a biochemical phenotype on laboratory testing unless they are symptomatic. Identification of asymptomatic patients allows them to adjust their lifestyle to avoid common triggering factors.[2][7]
References
- ^ a b c d e f "#121300 COPROPORPHYRIA, HEREDITARY; HCP". Johns Hopkins University. Retrieved 2012-05-27.
- ^ ISBN 978-1-59425-100-9.
- ^ ISBN 978-3-642-15719-6.
- ^ "Homo sapiens coproporphyrinogen oxidase, mRNA (cDNA clone MGC:19736 IMAGE:3607724), complete cds". US National Library of Medicine. Retrieved 2012-05-27.
- PMID 16159891.
- PMID 21103937.
- ^ S2CID 36122555.
- S2CID 46438357.
- ^ "Tests for Porphyria Diagnosis". National Porphyria Foundation. Archived from the original on 2014-03-20. Retrieved 2012-05-28.
External links
- Porphyria at NLMGenetics Home Reference
- Coproporphyria at NIH's Office of Rare Diseases
- MedlinePlus Encyclopedia: Porphyria
