Mastitis
| Mastitis | |
|---|---|
| Other names | mammitis; |
| Frequency | 10% of breastfeeding women[2] |
Mastitis is inflammation of the breast or udder, usually associated with breastfeeding.[1][5][6] Symptoms typically include local pain and redness.[1] There is often an associated fever and general soreness.[1] Onset is typically fairly rapid and usually occurs within the first few months of delivery.[1] Complications can include abscess formation.[2]
Risk factors include poor
Prevention of this
Types
When it occurs in breastfeeding mothers, it is known as puerperal mastitis, lactation mastitis, or lactational mastitis. When it occurs in non breastfeeding women it is known as non-puerperal or non-lactational mastitis. Mastitis can, in rare cases, occur in men. Inflammatory breast cancer has symptoms very similar to mastitis and must be ruled out.
The symptoms are similar for puerperal and nonpuerperal mastitis but predisposing factors and treatment can be very different.
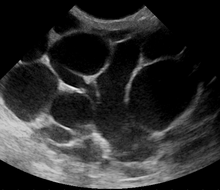
Puerperal mastitis is the inflammation of the breast in connection with pregnancy, breastfeeding or weaning. Since one of the most prominent symptoms is tension and engorgement of the breast, it is thought to be caused by blocked milk ducts or milk excess. It is relatively common; estimates range depending on methodology between 5–33%. However, only about 0.4–0.5% of breastfeeding mothers develop an abscess.[7]
Some predisposing factors are known but their predictive value is minimal. It appears that proper breastfeeding technique, frequent breastfeeding and avoidance of stress are the most important factors that can be influenced.
Light cases of mastitis are often called breast engorgement; the distinction is overlapping and possibly arbitrary or subject to regional variations.
The term nonpuerperal mastitis describes inflammatory lesions of the breast occurring unrelated to pregnancy and breastfeeding. This article includes description of mastitis as well as various kinds of mammary abscesses. Skin related conditions like dermatitis and foliculitis are a separate entity.
Names for non-puerperal mastitis are not used very consistently and include mastitis, subareolar abscess, duct ectasia, periductal inflammation,
Periductal mastitis is a form of nonlactational mastitis, and is characterized by inflammation of the subareolar ducts. Although the cause of periductal mastitis is currently unknown, it is predicted that smoking may be related. This condition is mainly seen in young women but can also be seen in men.[8]
Signs and symptoms
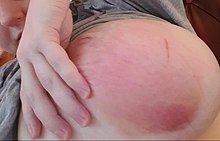
Lactation mastitis usually affects only one breast and the symptoms can develop quickly.[9] It develops into three stages, from the initial stage, the pus formation stage, to the restoration stage.[10] The signs and symptoms usually appear suddenly and they include:
- Breast tendernessor warmth to the touch
- General malaise or feeling ill
- Swellingof the breast
- Pain or a burning sensation continuously or while breast-feeding
- Skin redness, often in a wedge-shaped pattern
- Fever of 101 F (38.3 C) or greater[11]
- The affected breast can then start to appear lumpy and red.
Some women may also experience flu-like symptoms such as:
Contact should be made with a health care provider with special breastfeeding competence as soon as the patient recognizes the combination of signs and symptoms. Most of the women first experience the flu-like symptoms and just after they may notice a sore red area on the breast. Also, women should seek medical care if they notice any abnormal discharge from the
Breast abscess


A breast abscess is a collection of pus that develops in the breast with various causes.[13] During lactation, breast abscess develops only rarely, most sources cite about 0.4–0.5% of breastfeeding women.[7] Known risk factors are age over 30, primiparous and late delivery. No correlation was found with smoking status; however, this may be in part because far fewer smoking women choose to breastfeed.[14] Antibiotics were not shown effective in prevention of lactation abscess but are useful to treat a secondary infection (see the section on the treatment of breast abscess in this article).
Keratinizing squamous metaplasia of lactiferous ducts may play a similar[clarification needed] role in the pathogenesis of nonpuerperal subareolar abscess.
Causes
Since the 1980s mastitis has often been divided into non-infectious and infectious sub-groups. However, recent research [15] suggests that it may not be feasible to make divisions in this way. It has been shown that types and amounts of potentially pathogenic bacteria in breast milk are not correlated to the severity of symptoms. Moreover, although only 15% of women with mastitis in Kvist et al.'s study were given antibiotics, all recovered and few had recurring symptoms. Many healthy breastfeeding women wishing to donate breast milk have potentially pathogenic bacteria in their milk but have no symptoms of mastitis.[citation needed]
Risk factors
Mastitis typically develops when the milk is not properly removed from the breast. Milk stasis can lead to the milk ducts in the breasts becoming blocked, as the breast milk is not being properly and regularly expressed.[16] It has also been suggested that blocked milk ducts can occur as a result of pressure on the breast, such as tight-fitting clothing or an over-restrictive bra, although there is sparse evidence for this supposition. Mastitis may occur when the baby is not appropriately attached to the breast while feeding, when the baby has infrequent feeds or has problems suckling the milk out of the breast.
The presence of cracks or sores on the nipples increases the likelihood of infection. Tight clothing or ill-fitting bras may also cause problems as they compress the breasts. There is a possibility that infants carrying infectious pathogens in their noses can infect their mothers;[17] the clinical significance of this finding is still unknown.
Mastitis can also develop due to contamination of a breast implant or any other foreign body, for example after nipple
Women who are breastfeeding are at risk for developing mastitis especially if they have sore or cracked nipples or have had mastitis before while breastfeeding another baby. Also, the chances of getting mastitis increases if women use only one position to breastfeed or wear a tight-fitting bra, which may restrict milk flow [19] Difficulties in getting a nursing infant to latch on to the breast can also increase the risk for mastitis.[20]
Women with
Infection
Some women (approximately 15%)
Recent research suggests that infectious pathogens play a much smaller role in the pathogenesis than was commonly assumed only a few years ago. Most detected pathogens are very common species that are natural part of the breast fauna and simple detection of their presence is not sufficient to prove a causative role. Furthermore, there are indications that treatment with antibiotics may have minimal impact,[24][25] and over-all there is insufficient evidence to confirm or refute the effectiveness of antibiotic therapy for treating lactational mastitis.[26]
Diagnosis
The diagnosis of mastitis and breast abscess can usually be made based on a physical examination.[23] The doctor will also take into account the signs and symptoms of the condition.
However, if the doctor is not sure whether the mass is an abscess or a
In cases of infectious mastitis, cultures may be needed in order to determine what type of organism is causing the infection. Cultures are helpful in deciding the specific type of
Differential diagnosis
Perinatal mood and anxiety disorders
Some women who experience pain or other symptoms when breastfeeding, but who have no detectable signs of mastitis, may have a
Breast cancer
Breast cancer may coincide with or mimic symptoms of mastitis. Only full resolution of symptoms and careful examination are sufficient to exclude the diagnosis of breast cancer.
The lifetime risk for breast cancer is significantly reduced for women who were pregnant and breastfeeding. Mastitis episodes do not appear to influence lifetime risk of breast cancer.[citation needed]
Mastitis does however cause great difficulties in diagnosis of breast cancer. Breast cancer may coincide with mastitis or develop shortly afterwards. All suspicious symptoms that do not completely disappear within 5 weeks must be investigated.[citation needed]
Breast cancer incidence during pregnancy and lactation is assumed to be the same as in controls. Course and prognosis are also very similar to age matched controls.[28][29] However diagnosis during lactation is particularly problematic, often leading to delayed diagnosis and treatment.
Some data suggest that noninflammatory breast cancer incidence is increased within a year following episodes of nonpuerperal mastitis and special care is required for follow-up cancer prevention screening.[30] So far only data from short term observation is available and total risk increase can not be judged. Because of the very short time between presentation of mastitis and breast cancer in this study it is considered very unlikely that the inflammation had any substantial role in carcinogenesis, rather it would appear that some precancerous lesions may increase the risk of inflammation (hyperplasia causing duct obstruction, hypersensitivity to cytokines or hormones) or the lesions may have common predisposing factors.
A very serious type of breast cancer called inflammatory breast cancer presents with similar symptoms as mastitis (both puerperal and nonpuerperal). It is the most aggressive type of breast cancer with the highest mortality rate. The inflammatory phenotype of IBC is thought to be mostly caused by invasion and blocking of dermal lymphatics, however it was recently shown that NF-κB target genes activation may significantly contribute to the inflammatory phenotype. Case reports show that inflammatory breast cancer symptoms can flare up following injury or inflammation making it even more likely to be mistaken for mastitis. Symptoms are also known to partially respond to progesterone and antibiotics, reaction to other common medications can not be ruled out at this point.[31][32][33][34][35]
Treatment
Lactational mastitis
When mastitis is associated with breastfeeding, the treatment has to balance short-term reduction of symptoms with solving the underlying problems that caused mastitis. For example, the Academy of Breastfeeding Medicine recommends against trying to "empty" the breasts, whether through pushing the baby to feed more or through using a breast pump.[27] It may reduce the feeling of being full or swollen in the short term, at the cost of triggering milk oversupply, which can cause a mastitis recurrence in the coming days and weeks.[27]
Self-care
For breastfeeding women with
Gentle massage ("like petting a cat"[27]) may be comfortable and may reduce swelling.[27] However, more aggressive rubbing can easily damage breast tissues that are already strained by mastitis, and that damage can increase swelling and pain.[27] Excessive massage, like excessive use of a breast pump, may be a risk factor for recurrent mastitis.[27]
Medical treatments
Therapeutic ultrasound may reduce swelling.[27]
Ineffective and harmful treatments
The shape of swelling in a specific spot may make people suppose that the breasts contain simple tubes, and that one has become plugged. However, milk ducts are not simple tubes, and their interconnected anatomy makes it impossible for them to actually become plugged.[27] Consequently, treatment does not include cutting, popping, or squeezing any so-called "plugged" ducts.[27] There is no "plug" (e.g., of dried-out milk) to be removed.[27] These localized swellings are usually caused by lymphatic congestion (non-milk body fluid accumulating in the breasts), alveolar edema (swelling in the part of the breast that produces milk), or mammary dysbiosis (changes to the breast's microbiome), which can cause some narrowing, but not plugging, at the microscopic level.[27] Breastfeeding at a normal level may provide temporary relief from the swelling without triggering milk oversupply.[27] It is safer to treat nipple blebs (very small, usually pale colored, bumps of tissue on the end of the nipple) with topical steroids than by cutting the skin.[27]
Any action that breaks the skin can cause an infection, which increases inflammation and may become serious.[27]
Antibiotics do not prevent mastitis from recurring.[27][36]
Nonpuerperal mastitis
Nonpuerperal mastitis is treated by medication and possibly aspiration or drainage (see in particular
In idiopathic granulomatous mastitis, successful treatment includes invasive surgical procedures or less invasive treatment with steroid medications.[37]
Antibiotics for bacterial mastitis
In lactational mastitis,
A lactational phlegmon (area of inflammation) should be monitored for possible development into an abscess (walled-off area filled with pus from an infection).[27]
Breast abscess
An abscess (or suspected abscess) in the breast may be treated by ultrasound-guided fine-needle aspiration (percutaneous aspiration) or by surgical incision and drainage; each of these approaches is performed under antibiotic coverage. In case of puerperal breast abscess, breastfeeding from the affected breast should be continued where possible.[24][42]
For small breast abscesses,
One recommended treatment includes antibiotics, ultrasound evaluation and, if fluid is present, ultrasound-guided fine needle aspiration of the abscess with an
Nonpuerperal breast abscesses have a higher rate of recurrence compared to puerperal breast abscesses.
Although there are a number of recommendations regarding the treatment of breast abscesses, a 2015 review found insufficient evidence of whether needle aspiration is comparable to incision and drainage, or whether antibiotics should generally be given to women undergoing incision and drainage.[51]
Prevention
Most efforts to prevent mastitis in breastfeeding women are believed to be ineffective or have a relatively small effect.
Prognosis
Neither the presence of a fever nor the severity of symptoms at presentation do not predict outcome; women with sore or damaged nipples may need special attention.[52][53]
Epidemiology
Mastitis is quite common among breastfeeding women. The WHO estimates that although incidences vary between 2.6% and 33%, the prevalence globally is approximately 10% of breastfeeding women. Most mothers who develop mastitis usually do so within the first few weeks after delivery. Most breast infections occur within the first or second month after delivery or at the time of weaning.[21] However, in rare cases it affects women who are not breastfeeding.[54]
Terminology
Popular usage of the term mastitis varies by geographic region. Outside the US, it is commonly used for both
In this article, mastitis is used in the original sense of the definition as inflammation of the breast, with additional qualifiers where appropriate.
Chronic cystic mastitis is an older name for fibrocystic breast changes.
Etymology and pronunciation
The word mastitis ( in modern usage, and mastitis is the more commonly used synonym.
Other animals
Mastitis occurs in other animals as in humans, and is especially a concern in livestock, since milk from the affected udders of livestock may enter the food supply and pose a health risk.
It is a major condition in some species, like
-
Udder of a Roux du Valais sheep after a healed mastitis; one teat was lost due to the disease.
-
Serous exudate from bovine udder in E. coli mastitis[55] at left. Normal milk at right.
-
Gangrenous mastitis in a dairy cow.
-
Cat with mastitis
See also
- Galactocele, a milk-filled cyst
References
- ^ S2CID 13006527.
- ^ PMID 18819238.
- ISBN 978-0-323-07685-2.
- ISBN 978-0-323-07841-2.
- ISBN 978-1-61091-633-2.
- ISBN 978-0-323-04306-9.
- ^ PMID 12937109.
- ^ Dixon JM, Pariser KM. "Nonlactational mastitis in adults". UpToDate. Retrieved 2019-08-02.
- ^ "Symptoms of mastitis". Retrieved 2010-04-20.
- PMID 29853971.
- ^ "Symptoms". Retrieved 2010-04-20.
- ^ "Breast Infection Symptoms". Retrieved 2010-04-20.
- PMID 26148851.
- PMID 22146325.
- ^ PMID 18394188.
- ^ "Non-infectious mastitis and milk stasis". Archived from the original on 2010-04-28. Retrieved 2010-04-20.
- PMID 17032458.
- ^ BMJBest Practice (last updated 5 September 2014) (subscription-limited access)
- ^ "Risk factors". Retrieved 2010-04-20.
- ^ "Common questions about breastfeeding and pain". womenshealth.gov. Archived from the original on 4 August 2017. Retrieved 4 August 2017.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ a b "Breast Infection Causes". Retrieved 2010-04-20.
- ^ "Breastfeeding Mastitis Causes and Symptoms". Archived from the original on 2019-07-19. Retrieved 2010-04-20.
- ^ a b "Exams and Tests". Retrieved 2010-04-20.
- ^ S2CID 7649157.
- PMID 12672715.
- ^ Antibiotics for mastitis in breastfeeding women. Cochrane Database of Systematic Reviews, PubMed Health. Review published 2013; Review content assessed as up-to-date: November 23, 2012.
- ^ S2CID 248832395.
- S2CID 21424443.
- PMID 10888783.
- PMID 12270566.
- PMID 8085857.
- PMID 1387777.
- S2CID 86034806.
- PMID 17700572.
- PMID 9238713.
- ^ PMID 32987448.
- PMID 28731822.
- PMID 18819238.
- PMID 28900682.
- PMID 27355802.
- PMID 23450563.
- PMID 21997989., p. 1684
- ISBN 978-1-4511-5323-1.
- PMID 21997989., Fig. 9 on p. 1696
- PMID 21997989., p. 1691
- PMID 21997989., p. 1692–1693
- ^ PMID 21997989., p. 1694
- PMID 21997989., abstract
- S2CID 25120670.
- S2CID 23073438.
- PMID 26279276.
- PMID 17244353.
- PMID 17052823.
- ^ "Causes of mastitis". NHS. Archived from the original on 2010-04-28. Retrieved 2010-04-20.
- PMID 22118085.)
{{cite journal}}: CS1 maint: multiple names: authors list (link
External links
- Mastitis on mayoclinic.com
- Australian Breastfeeding Association


![Serous exudate from bovine udder in E. coli mastitis[55] at left. Normal milk at right.](http://upload.wikimedia.org/wikipedia/commons/thumb/b/b2/Mamite_%C3%A5_colibacile_laecea.jpg/200px-Mamite_%C3%A5_colibacile_laecea.jpg)

