Peritoneal dialysis
| Peritoneal dialysis | |
|---|---|
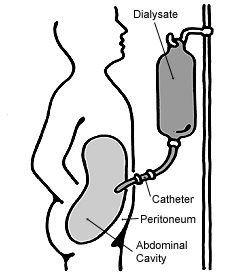 Diagram of peritoneal dialysis | |
| Specialty | nephrology |
| ICD-9-CM | 54.98 |
| MeSH | D010530 |
Peritoneal dialysis (PD) is a type of
Side effects
Complications may include
Mechanism
In peritoneal dialysis, a specific solution is introduced through a permanent tube in the lower abdomen and then removed.
History and culture
The solution used for peritoneal dialysis is on the World Health Organization's List of Essential Medicines.[5][6] As of 2009, peritoneal dialysis was available in 12 of 53 African countries.[7]
Medical uses
Peritoneal dialysis is a method of renal replacement therapy for those needing maintenance therapy for late stage chronic kidney disease and is an alternative to the most common method hemodialysis.
Complications
Peritoneal Dialysis-Related Peritonitis
A common cause of peritonitis is touch contamination, e.g. insertion of catheter by un-sanitized hands, which potentially introduces bacteria to the abdomen; other causes include catheter complication, transplantation of bowel bacteria, and systemic infections.[8] Most common type of PD-peritonitis infection (80%) are from bacterial sources.[8] Infection rates are highly variable by region and within centers with estimated rates between 0.06 - 1.66 episodes per patient year.[9] With recent technical advances peritonitis incidence has decreased over time.[10]
Antibiotics are needed if the source of infection is bacterial; there is no clear advantage for other frequently used treatments such as routine peritoneal lavage or use of urokinase.[11] The use of preventative nasal mupirocin is of unclear effect with respect to peritonitis.[12] Of the three types of connection and fluid exchange systems (standard, twin-bag and y-set; the latter two involving two bags and only one connection to the catheter, the y-set uses a single y-shaped connection between the bags involving emptying, flushing out then filling the peritoneum through the same connection) the twin-bag and y-set systems were found superior to conventional systems at preventing peritonitis.[13]
The fluid used for dialysis uses
The mortality rate of peritoneal dialysis related peritonitis is estimated to be 3-10%, with approximately 50% of cases resulting in hospitalization.
Volume Shifts
The volume of dialysate removed as well as patient's weight are monitored.[by whom?] If more than 500ml of fluid are retained or a liter of fluid is lost across three consecutive treatments, the patient's physician is generally notified.[citation needed] Excessive loss of fluid can result in hypovolemic shock or hypotension while excessive fluid retention can result in hypertension and edema. Also monitored is the color of the fluid removed: normally it is pink-tinged for the initial four cycles and clear or pale yellow afterward. The presence of pink or bloody effluent suggests bleeding inside the abdomen while feces indicates a perforated bowel and cloudy fluid suggests infection. The patient may also experience pain or discomfort if the dialysate is too acidic, too cold or introduced too quickly, while diffuse pain with cloudy discharge may indicate an infection. Severe pain in the rectum or perineum can be the result of an improperly placed catheter. The dwell can also increase pressure on the diaphragm causing impaired breathing, and constipation can interfere with the ability of fluid to flow through the catheter.[17]
Chronic Complications
Long term use of PD is rarely associated with fibrosis of the peritoneum.[10] A potentially fatal complication estimated to occur in roughly 2.5% of patients is encapsulating peritoneal sclerosis, in which the bowels become obstructed due to the growth of a thick layer of fibrin within the peritoneum.[18]
Other
Other complications include low back pain and hernia or leaking fluid due to high pressure within the abdomen.[19] Hypertriglyceridemia and obesity are also concerns due to the large volume of glucose in the fluid, which can add 500-1200 calories to the diet per day.[20]
Method
Best practices for peritoneal dialysis state that before peritoneal dialysis should be implemented, the person's understanding of the process and support systems should be assessed, with education on how to care for the catheter and to address any gaps in understanding that may exist. The person should receive ongoing monitoring to ensure adequate dialysis, and be regularly assessed for complications. Finally, they should be educated on the importance of infection control and an appropriate medical regimen established with their cooperation.[21]
- Dialysis process
-
Hookup
-
Infusion
-
Diffusion (fresh)
-
Diffusion (waste)
-
Drainage

The abdomen is cleaned in preparation for surgery and a catheter is surgically inserted with one end in the abdomen and the other protruding from the skin.[22] Catheters can also be inserted without a general anaesthetic by a physician using a needle, known as a medical insertion. Both methods have similar safety profiles.[23][24] Before each infusion the catheter must be cleaned, and flow into and out of the abdomen tested. 2-3 liters of dialysis fluid is introduced into the abdomen over the next ten to fifteen minutes.[17] The total volume is referred to as a dwell[25] while the fluid itself is referred to as dialysate. The dwell can be as much as 3 liters, and medication can also be added to the fluid immediately before infusion.[17] The dwell remains in the abdomen and waste products diffuse across the peritoneum from the underlying blood vessels. After a variable period of time depending on the treatment (usually 4–6 hours[17] ), the fluid is removed and replaced with fresh fluid. This can occur automatically while the patient is sleeping (automated peritoneal dialysis, APD), or during the day by keeping two litres of fluid in the abdomen at all times, exchanging the fluids four to six times per day (continuous ambulatory peritoneal dialysis, CAPD).[25][26]
The fluid used typically contains
Though there are several different shapes and sizes of catheters that can be used, different insertion sites, number of cuffs in the catheter and immobilization, there is no evidence to show any advantages in terms of morbidity, mortality or number of infections, though the quality of information is not yet sufficient to allow for firm conclusions.[29]
A peritoneal equilibration test may be done to assess a person for peritoneal dialysis by determining the characteristics of the peritoneal membrane mass transport characteristics.
Improvised Dialysis
Peritoneal dialysis can be improvised in conditions such as combat surgery or disaster relief using surgical catheters and dialysate made from routinely available medical solutions to provide temporary renal replacement for people with no other options.[30]
Epidemiology
As of 2017, hemodialysis is the most widely available renal replacement modality found in 96% of countries whereas peritoneal dialysis (PD) is only available in 75% of countries.[10] In 2016, the proportion of people receiving peritoneal dialysis (PD) was estimated at 11% with wide differences between different countries and regions.[31] In Hong Kong and Mexico, PD is more common than the world average, with Mexico conducting most of its dialysis through PD, while Japan and Germany have rates lower than the world average.[32] Peritoneal dialysis first models, patients requiring renal replacement therapy are placed on PD first, and financial incentives for using PD are associated with increase uptake of PD in multiple countries.[31]
East and Southeast Asia
Hong Kong has the highest rate of PD use worldwide at 71.9% in 2014, while in Mainland China had 20% in 2014, 23% in Thailand during 2012, and 10-20% in Vietnam during 2011.[31] Hong Kong had a PD-first model since 1985, Thailand began a PD-first model since 2008 which increased their levels of PD from <10%.[31]
Americas
Prevalence in of PD use was 9.7% in USA during 2013 and 16.3% in Canada during 2013.[31] The lower PD rates in the USA are due to higher availability of large corporate owned hemodialysis centers. There have been recent increase in PD uptake in the USA due to changes to medicare reimbursement such as bundled payment for dialysis this incentivizes use of PD which is a less costly modality for dialysis.[31]
Overall, prevalence of PD use is 24.6% in Latin America during 2011.[31] Within Latin America, hemodialysis has a higher growth rate in use compared to PD between 1994 - 2010. In 2010, the most prevalent use of PD were in Mexico 55.9% and El Salvador 67.6%. Between 2000 - 2010, Colombia's PD rate dropped from 54% to 31.3%.[33]
History
Peritoneal dialysis was first carried out in the 1920s; however, long-term use did not come into medical practice until the 1960s.[34] The timeline was
- 1923 –
- 1946 – Howard Frank, Arnold Seligman, and Jacob Fine of Beth Israel Hospital in Boston report the first successful use of peritoneal dialysis in clinical practice,[35] in a 51-year-old man with acute renal failure caused by sulfathiazole poisoning.[36]
- 1959 – Paul Doolan and Richard Ruben of Naval Hospital Oakland first use peritoneal dialysis to treat end-stage renal disease, in a 33-year-old woman named Willie Mae Stewart. After 6 months of intermittent dialysis, she declines further treatment due to complications and dies in June 1960.[37]
- 1964–1965 – Henry Tenckhoff, G. Shilipetar and Fred Boen of the University of Washington report the first case of home peritoneal dialysis, with long-term success despite technical difficulties and a burdensome process.[37][38]
- 1968 – Henry Tenckhoff creates the Tenckhoff catheter, avoiding the need to replace the catheter in the abdomen at every treatment.[39]
Comparison to Hemodialysis
Compared to hemodialysis, PD allows greater patient mobility, produces fewer swings in symptoms due to its continuous nature, and
PD may also be used for patients with
Society and culture
Economics
The cost of dialysis treatment is related to how wealthy the country is.[7] In the United States peritoneal dialysis costs the government about $53,400 per person per year.[4]
References
- PMID 27009336.
- ISBN 978-1-58255-515-7. Archivedfrom the original on 2017-01-13.
- ^ ISBN 978-92-4-154765-9.
- ^ .
- hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- hdl:10665/345533. WHO/MHP/HPS/EML/2021.02.
- ^ ISBN 978-3-8055-9202-4. Archivedfrom the original on 2017-01-13.
- ^ OCLC 1076544294.
- PMID 24751170.
- ^ PMID 32733095.
- PMID 24771351.
- PMID 28390069.
- PMID 25117423.
- PMID 32069459. "Other studies suggest that a high peritoneal glucose load increases the risk of peritonitis, perhaps as the effect of impaired host defenses, vascular disease, and damage to the peritoneal membrane [9, 10, 11]."
- PMID 21248712.
- ^ S2CID 242938564.
- ^ ISBN 978-1-58255-532-4.
- S2CID 1050358.
- OCLC 1076544294.
- ISBN 978-0-7360-6565-8. Archivedfrom the original on 2013-06-18.
- ^ Wood M, et al. (CANNT Nursing Standards Working Group) (2008-08-01). "Nephrology Nursing Standards and Practice Recommendations" (PDF). Canadian Association of Nephrology Nurses and Technologists. Archived from the original (PDF) on 2010-03-31. Retrieved 2010-09-08.
- PMID 16769289.
- PMID 38106573.
- .
- ^ ISBN 978-0-7637-6591-0. Archivedfrom the original on 2013-06-18.
- ]
- S2CID 25034246.
- ISBN 978-0-7817-5253-4. Archivedfrom the original on 2013-06-18.
- PMID 31149735.
- S2CID 24251777.
- ^ S2CID 25054210.
- PMID 16204281.
- PMID 25349696.
- ^ ISBN 978-94-017-2560-6. Archivedfrom the original on 2017-01-13.
- ^ PMID 34569508.
- PMID 21016282.
- ^ ISBN 978-94-009-6768-7.
- PMID 14329068.
- PMID 27339663.
- PMID 23737482.
- from the original on 2009-10-08.