Inflammatory bowel disease
| Inflammatory bowel diseases | |
|---|---|
celiac disease | |
| Frequency | 11.2 million worldwide (2015)[1] |
| Deaths | 47,400 worldwide (2015)[2] |
Inflammatory bowel disease (IBD) is a group of
Signs and symptoms
| Crohn's disease | Ulcerative colitis | |
|---|---|---|
| Defecation | Often porridge-like,[7] sometimes steatorrhea |
Often mucus-like and with blood[7] |
| Tenesmus | Less common[7] | More common[7] |
| Fever | Common[7] | Indicates severe disease[7] |
| Fistulae | Common[8] | Seldom |
| Weight loss | Often | More seldom |
In spite of Crohn's and UC being very different diseases, both may present with any of the following symptoms: abdominal pain,
| Crohn's disease | Ulcerative colitis | |
|---|---|---|
Terminal ileum involvement |
Commonly | Seldom |
| Colon involvement | Usually | Always |
| Rectum involvement | Seldom | Usually (95%)[15] |
| Involvement around the anus |
Common[16] | Seldom |
| Bile duct involvement | No increase in rate of primary sclerosing cholangitis | Higher rate[17] |
| Distribution of disease | Patchy areas of inflammation (skip lesions) | Continuous area of inflammation[15] |
| Endoscopy | Deep geographic and serpiginous (snake-like) ulcers
|
Continuous ulcer |
| Depth of inflammation | May be transmural, deep into tissues[16][5] | Shallow, mucosal |
| Stenosis | Common | Seldom |
| Granulomas on biopsy | May have non- | Non-peri- intestinal crypt granulomas not seen[20]
|
Causes
| Crohn's disease | Ulcerative colitis | |
|---|---|---|
| Cytokine response | Associated with Th17[21] |
Vaguely associated with Th2
|
IBD is a complex disease which arises as a result of the interaction of environmental and genetic factors leading to immunological responses and inflammation in the intestine.[4]
Diet
People living with IBD are very interested in diet, but little is known about the impact of diet on these patients. Recent reviews underlined the important role of nutritional counselling in IBD patients. Patients should be encouraged to adopt diets that are best supported by evidence and involve monitoring for the objective resolution of inflammation.[22][23]
A 2022 study found that diets with increased intake of fruits and vegetables, reduction of processed meats and refined carbohydrates, and preference of water for hydration were associated with lower risk of active symptoms with IBD, although increased intake of fruits and vegetables alone did not reduce risk of symptoms with Crohn's disease.[24]
Dietary patterns are associated with a risk for ulcerative colitis. In particular, subjects who were in the highest
A diet high in protein, particularly animal protein, and/or high in sugar may be associated with increased risk of IBD and relapses.[27][28]
Bile acids
Emerging evidence indicates that bile acids are important etiological agents in IBD pathogenesis.[29] IBD patients have a consistent pattern of an increased abundance of primary bile acids such as cholic acid and chenodeoxycholic acid (and their conjugated forms), and a decreased abundance of secondary bile acids such as lithocholic acid and deoxycholic acid.[29]
Microbiota
The human microbiota consists of 10–100 trillion microorganisms.[30] Several studies have confirmed that the microbiota composition is different in patients with IBD compared to healthy individuals.[31] Specifically, the difference is more pronounced in patients with Crohn's disease than in those with ulcerative colitis.[32] In IBD patients, there is a decrease or absence of beneficial bacteria such as Bifidobacterium longum, Eubacterium rectale, Faecalibacterium prausnitzii, and Roseburia intestinalis, while harmful species like Bacteroides fragilis, Ruminococcus torques, and Ruminococcus are more abundant.[33] The activation of reactive oxygen species and reactive nitrogen species leads to oxidative stress for both host cells and the gut microbiome. Consequently, in IBD, there is a microbial imbalance, known as dysbiosis, characterized by an increase in functional pathways involved in the microbial response to oxidative stress. This oxidative stress can promote the growth of certain species such as R. gnavus.[34] Another opportunistic bacterium called A. muciniphila contributes to IBD development and is more prevalent in individuals lacking NOD-like receptor 6 (NLRP6).[35] Both R. gnavus and A. muciniphila are bacterial species that are more abundant in IBD. Patients with IBD often exhibit stronger antibody and T-cell responses to microbial antigens.[36] The gut microbiome employs various approaches to interact with the host immune system. For instance, B. fragilis, which is symbiotic in humans, can transfer immune regulatory molecules to immune cells through the secretion of outer membrane vesicles. This mechanism plays a protective role in IBD by activating the non-classical autophagy pathway, dependent on Atg16L1 and NOD2 genes.[37] B. thetaiotaomicron induces the differentiation of T regulatory cells (Tregs) to modulate gut immunity, thus increasing the expression of Gata3 and FoxP3 genes.[38] The colonization of Clostridium spp. can enhance the aggregation of RORγT+ FOXP3 Treg cells, which inhibit the development of Th2 and Th17 cells. Ultimately, this colonization could decrease the response of colonic Th2 and Th17 cells.[39] Also F. prausnitzii atteracts atteract CD4 and CD8a (DP8α) regulatory T cells.[40] E. coli Nissle 1917 has the capability to inhibit the growth of Salmonella and other harmful bacteria. It prevents these pathogens from adhering to and invading intestinal epithelial cells, which significantly reduces the likelihood of inflammation in the gut and may also prevent the onset of IBD.[41]
Breach of intestinal barrier
Loss of integrity of the
Oxidative stress and DNA damage
Pereira et al.[45] reviewed evidence from numerous studies indicating that oxidative stress and DNA damage likely have a role in the pathophysiology of IBD. Oxidative DNA damage as measured by 8-OHdG levels was found to be significantly increased in patients with IBD compared to control patients, and in inflamed mucosa compared with non-inflamed mucosa.[45]
Genetics
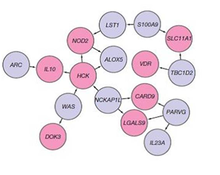
A genetic component to IBD has been recognized for over a century.[46] Research that has contributed to understanding of the genetics include studies of ethnic groups (e.g., Ashkenazi Jews, Irish), familial clustering, epidemiological studies, and twin studies. With the advent of molecular genetics, understanding of the genetic basis has expanded considerably, particularly in the past decade.[47] The first gene linked to IBD was NOD2 in 2001.
Genome-wide association studies have since added to understanding of the genomics and pathogenesis of the disease. More than 200
Diagnosis
The diagnosis is usually confirmed by biopsies on colonoscopy. Fecal calprotectin is useful as an initial investigation, which may suggest the possibility of IBD, as this test is sensitive but not specific for IBD.[53][54]
Classification
Inflammatory bowel diseases are
Differential diagnosis
Crohn's disease and ulcerative colitis are both common differential diagnoses for the other, and confidently diagnosing a patient with one of the two diseases may sometimes not be possible. No disease specific markers are currently known in the blood that would enable the reliable separation of patients with Crohn's disease and ulcerative colitis.
Liver function tests are often elevated in IBD, and are often mild and generally return spontaneously to normal levels.[67] The most relevant mechanisms of elevated liver functions tests in IBD are drug-induced hepatotoxicity and fatty liver.[67]
Treatment
Crohn's disease |
Ulcerative colitis
| |
|---|---|---|
| Mesalazine | Less useful[68] | More useful[68] |
| Antibiotics | Effective in long-term[69] | Generally not useful[70] |
| Surgery | Often returns following removal of affected part |
Usually cured by removal of colon |
Surgery
CD and UC are chronic inflammatory diseases, and are not medically curable.[71] However, Ulcerative Colitis can in most cases be cured by proctocolectomy, although this may not eliminate extra-intestinal symptoms. An ileostomy will collect feces in a bag. Alternatively, a pouch can be created from the small intestine; this serves as the rectum and prevents the need for a permanent ileostomy. Between one-quarter and one-half of patients with ileo-anal pouches do have to manage occasional or chronic pouchitis.[72]
Surgery cannot cure Crohn's disease but may be needed to treat complications such as abscesses, strictures or fistulae.[73] Severe cases may require surgery, such as bowel resection, strictureplasty or a temporary or permanent colostomy or ileostomy. In Crohn's disease, surgery involves removing the worst inflamed segments of the intestine and connecting the healthy regions, but unfortunately, it does not cure Crohn's or eliminate the disease. At some point after the first surgery, Crohn's disease can recur in the healthy parts of the intestine, usually at the resection site.[74] (For example, if a patient with Crohn's disease has an ileocecal anastomosis, in which the caecum and terminal ileum are removed and the ileum is joined to the ascending colon, their Crohn's will nearly always flare-up near the anastomosis or in the rest of the ascending colon).[75]
Medical therapies
Medical treatment of IBD is individualised to each patient.
Steroids, such as the glucocorticoid prednisone, are frequently used to control disease flares and were once acceptable as a maintenance drug. Biological therapy for inflammatory bowel disease, especially the TNF inhibitors, are used in people with more severe or resistant Crohn's disease and sometimes in ulcerative colitis.[77]
Treatment is usually started by administering drugs with high anti-inflammatory effects, such as prednisone. Once the inflammation is successfully controlled, another drug to keep the disease in remission, such as mesalazine in UC, is the main treatment. If further treatment is required, a combination of an immunosuppressive drug (such as azathioprine) with mesalazine (which may also have an anti-inflammatory effect) may be needed, depending on the patient. Controlled release budesonide is used for mild ileal Crohn's disease.[71]
Nutritional and dietetic therapies
Exclusive enteral nutrition is a first-line therapy in pediatric Crohn's disease with weaker data in adults.[78]: 331 [79] Evidence supporting exclusive enteral nutrition in ulcerative colitis is lacking.[78]: 333
Nutritional deficiencies play a prominent role in IBD. Malabsorption, diarrhea, and GI blood loss are common features of IBD. Deficiencies of B vitamins, fat-soluble vitamins, essential fatty acids, and key minerals such as magnesium, zinc, and selenium are extremely common and benefit from replacement therapy. Dietary interventions, including certain exclusion diets like the specific carbohydrate diet (SCD) can be beneficial for symptom management.[80] Dietary fiber interventions, such as psyillium supplementation (a mixture of soluble and insoluble fibers), may relieve symptoms as well as induce/maintain remission by altering the microbiome composition of the GI tract, thereby improving regulation of immune function, reducing inflammation, and helping to restore the intestinal mucosal lining.[81]
Gastrointestinal bleeding, occurring especially during ulcerative colitis relapse, can contribute to anaemia when chronic, and may be life-threatening when acute. To limit the possible risk of dietary intake disturbing hemostasis in acute gastrointestinal bleeding, temporary fasting is often considered necessary in hospital settings.[84] The effectiveness of this approach is unknown; a Cochrane review in 2016 found no published clinical trials including children.[85]
Low levels of vitamin D are associated with crohn's disease and ulcerative colitis and people with more severe cases of inflammatory bowl disease often have lower vitamin D levels. It is not clear if vitamin D deficiency causes inflammatory bowl disease or is a symptom of the disease.[86] There is some evidence that vitamin D supplementation therapy may be associated with improvements in scores for clinical inflammatory bowl disease activity and biochemical markers.[86] Vitamin D treatment may be associated with less inflammatory bowl disease reoccurrence of symptoms (relapse). It is not clear if this treatment improves the person's quality of life or what the clinical response to vitamin D treatment. The ideal treatment regime and dose of vitamin D therapy has not been well enough studied.[86]
Microbiome
There is preliminary evidence of an infectious contribution to IBD in some patients that may benefit from antibiotic therapy, such as with rifaximin.[87] The evidence for a benefit of rifaximin is mostly limited to Crohn's disease with less convincing evidence supporting use in ulcerative colitis.[88][89]
The use of oral probiotic supplements to modify the composition and behaviour of the microbiome has been considered as a possible therapy for both induction and maintenance of remission in people with Crohn's disease and ulcerative colitis. A Cochrane review in 2020 did not find clear evidence of improved remission likelihood, nor lower adverse events, in people with Crohn's disease, following probiotic treatment.[90]
For ulcerative colitis, there is low-certainty evidence that probiotic supplements may increase the probability of clinical remission.
Fecal microbiota transplant is a relatively new treatment option for IBD which has attracted attention since 2010.[93][94] Some preliminary studies have suggested benefits similar to those in Clostridioides difficile infection but a review of use in IBD shows that FMT is safe, but of variable efficacy. Systematic reviews showed that 33% of ulcerative colitis, and 50% of Crohn's disease patients reach clinical remission after fecal microbiota transplant.[95]
Alternative medicine
Complementary and alternative medicine approaches have been used in inflammatory bowel disorders.[96] Evidence from controlled studies of these therapies has been reviewed; risk of bias was quite heterogeneous. The best supportive evidence was found for herbal therapy, with Plantago ovata and curcumin in UC maintenance therapy, wormwood in CD, mind/body therapy and self-intervention in UC, and acupuncture in UC and CD.[97]
Novel approaches
Psychological interventions
Patients with IBD have a higher prevalence of depressive and anxiety disorders compared to the general population, women with IBD are more likely than men to develop affective disorders since up to 65% of them may have depression and anxiety disorder. [99][100] Currently, there is no evidence to recommend psychological treatment, such as
Treatment standards
Crohn's and Colitis Australia, the peak body for IBD in Australia, where prevalence is one of the highest in the world, reviewed the quality of care for patients admitted to Australian hospitals. They found that only one hospital met accepted standards for multidisciplinary care, but that care was improved with the availability of even minimal specialised services.[102]
Prognosis
| Crohn's disease |
Ulcerative colitis | ||
|---|---|---|---|
| Nutrient deficiency | Higher risk | ||
Colon cancer risk |
Slight | Considerable | |
| Prevalence of extraintestinal complications[103][104][105] | |||
Iritis/uveitis |
Females | 2.2% | 3.2% |
| Males | 1.3% | 0.9% | |
| Primary sclerosing cholangitis |
Females | 0.3% | 1% |
| Males | 0.4% | 3% | |
| Ankylosing spondylitis |
Females | 0.7% | 0.8% |
| Males | 2.7% | 1.5% | |
| Pyoderma gangrenosum |
Females | 1.2% | 0.8% |
| Males | 1.3% | 0.7% | |
| Erythema nodosum | Females | 1.9% | 2% |
| Males | 0.6% | 0.7% | |
While IBD can limit quality of life because of pain, vomiting, and diarrhea, it is rarely fatal on its own. Fatalities due to complications such as
Around one-third of individuals with IBD experience persistent gastrointestinal symptoms similar to
While patients of IBD do have an increased risk of colorectal cancer, this is usually caught much earlier than the general population in routine surveillance of the colon by colonoscopy, and therefore patients are much more likely to survive.[111]
New evidence suggests that patients with IBD may have an elevated risk of endothelial dysfunction and coronary artery disease.[112][113]
The goal of treatment is toward achieving remission, after which the patient is usually switched to a lighter drug with fewer potential side effects. Every so often, an acute resurgence of the original symptoms may appear; this is known as a "flare-up". Depending on the circumstances, it may go away on its own or require medication. The time between flare-ups may be anywhere from weeks to years, and varies wildly between patients – a few have never experienced a flare-up.[114]
Life with IBD can be challenging; however, many with the condition lead relatively normal lives. IBD carries a psychological burden due to stigmatization of being diagnosed, leading to high levels of anxiety, depression, and a general reduction in the quality of life.
Epidemiology
IBD resulted in a global total of 51,000 deaths in 2013 and 55,000 deaths in 1990.[117] The increased incidence of IBD since World War II has been correlated to the increase in meat consumption worldwide, supporting the claim that animal protein intake is associated with IBD.[118] However, there are many environmental risk factors that have been linked to the increased and decreased risk of IBD, such as smoking, air pollution and greenspace, urbanization and Westernization.[119] Inflammatory bowel diseases are increasing in Europe.[120] Incidence and prevalence of IBD has risen steadily for the last decades in Asia, which could be related changes in diet and other environmental factors.[121]
Around 0.8% of people in the UK have IBD.[122] Similarly, around 270,000 (0.7%) of people in Canada have IBD,[123] with that number expected to rise to 400,000 (1%) by 2030.[124]
Research
The following treatment strategies are not used routinely, but appear promising in some forms of IBD.
Initial reports[125] suggest that helminthic therapy may not only prevent but even control IBD: a drink with roughly 2,500 ova of the Trichuris suis helminth taken twice monthly decreased symptoms markedly in many patients. It is even speculated that an effective "immunization" procedure could be developed—by ingesting the cocktail at an early age.[126]
Prebiotics and probiotics are focusing increasing interest as treatments for IBD. Currently, there is evidence to support the use of certain probiotics in addition to standard treatments in people with ulcerative colitis but there is no sufficient data to recommend probiotics in people with Crohn's disease. Both single strain and multi-strain probiotics have been researched for mild to moderate cases of ulcerative colitis. The most clinically researched multi-strain probiotic with over 70 human trials is the De Simone Formulation.[127] Further research is required to identify specific probiotic strains or their combinations and prebiotic substances for therapies of intestinal inflammation.[128]
Currently, the probiotic strain, frequency, dose and duration of the probiotic therapy are not established.
In 2005
The team deliberately damaged the cells to cause inflammation of the gut lining and then added synthetically produced cannabinoids; the result was that gut started to heal: the broken cells were repaired and brought back closer together to mend the tears. It is believed that in a healthy gut, natural endogenous cannabinoids are released from endothelial cells when they are injured, which then bind to the CB1 receptors. The process appears to set off a wound-healing reaction, and when people use cannabis, the cannabinoids bind to these receptors in the same way.[131]
Previous studies have shown that CB1 receptors located on the nerve cells in the gut respond to cannabinoids by slowing gut
Activation of the
Alicaforsen is a first generation antisense oligodeoxynucleotide designed to bind specifically to the human
Cannabinoid CB2 receptor agonists are found to decrease the induction of ICAM-1 and VCAM-1 surface expression in human brain tissues and primary human brain endothelial cells (BMVEC) exposed to various pro-inflammatory mediators.[137]
In 2014, an alliance among the Broad Institute, Amgen and Massachusetts General Hospital formed with the intention to "collect and analyze patient DNA samples to identify and further validate genetic targets."[138]
In 2015, a meta-analysis on 938 IBD patients and 953 controls, IBD was significantly associated with having higher odds of vitamin D deficiency.[139]
Gram-positive bacteria present in the lumen could be associated with extending the time of relapse for ulcerative colitis.[128]
Bidirectional pathways between depression and IBD have been suggested [140] and psychological processes have been demonstrated to influence self-perceived physical and psychological health over time.[141] IBD-disease activity may impact quality of life and over time may significantly affect individual's mental well-being, which may be related to the increased risk to develop anxiety and/or depression.[140][142][143] On the other hand, psychological distress may also influence IBD activity.[144]
Higher rates of anxiety and depression are observed among those with IBD compared to healthy individuals, which correlated with disease severity.[142][144] Part of this phenotypic correlation is due to a shared genetic overlap between IBD and psychiatric comorbidities.[145] Moreover, anxiety and depression rates increase during active disease compared with inactive phases.[144]
In other species
IBD also occurs in dogs and is thought to arise from a combination of host genetics, intestinal microenvironment, environmental components and the immune system. There is an ongoing discussion, however, that the term "chronic enteropathy" might be better to use than "inflammatory bowel disease" in dogs because it differs from IBD in humans in how the dogs respond to treatment. For example, many dogs respond to only dietary changes compared to humans with IBD, who often need
See also
References
- PMID 27733282.
- PMID 27733281.
- OCLC 988941211.
- ^ S2CID 13544348.
- ^ S2CID 35264387.
- S2CID 4337332.
- ^ a b c d e f internetmedicin.se > Inflammatorisk tarmsjukdom, kronisk, IBD By Robert Löfberg. Retrieved Oct 2010 Translate.
- S2CID 31219115.)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - PMID 22882911.
- S2CID 25341683.
- S2CID 35344744.
- ^ Warner J (February 22, 2011). Martin LJ (ed.). "Inflammatory Bowel Disease Health Center". WebMD. Archived from the original on 20 October 2014. Retrieved 14 October 2014.
- PMID 24415866.
- from the original on 2022-11-29. Retrieved 2022-11-29.
- ^ S2CID 73473272.
- ^ S2CID 31219115.)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - S2CID 260320940.
- S2CID 36907992.
- S2CID 29476514.
- PMID 24942757.
- PMID 17570211.
- ^ Ananthakrishnan AN, Kaplan GG, Bernstein CN, Burke KE, Lochhead PJ, Sasson AN, Agrawal M, Tiong JHT, Steinberg J, Kruis W, Steinwurz F, Ahuja V, Ng SC, Rubin DT, Colombel JF, Gearry R; International Organization for Study of Inflammatory Bowel Diseases. Lifestyle, behaviour, and environmental modification for the management of patients with inflammatory bowel diseases: an International Organization for Study of Inflammatory Bowel Diseases consensus. Lancet Gastroenterol Hepatol. 2022 Apr 26:S2468-1253(22)00021-8.
- ^ Roncoroni L, Gori R, Elli L, Tontini GE, Doneda L, Norsa L, Cuomo M, Lombardo V, Scricciolo A, Caprioli F, Costantino A, Scaramella L, Vecchi M. Nutrition in Patients with Inflammatory Bowel Diseases: A Narrative Review. Nutrients. 2022 Feb 10;14(4):751.
- PMID 35092268.
- S2CID 3452004.
- S2CID 4119392.
- PMID 22055893.
- ^ Barron M (2021-01-11). "Sugar may trigger inflammatory bowel disease by breaking down gut mucus". Massive Science. Archived from the original on 2021-01-13. Retrieved 2021-01-15.
- ^ a b Thomas JP, Modos D, Rushbrook SM, Powell N, Korcsmaros T. The Emerging Role of Bile Acids in the Pathogenesis of Inflammatory Bowel Disease. Front Immunol. 2022 Feb 3;13:829525. doi: 10.3389/fimmu.2022.829525. PMID 35185922; PMCID: PMC8850271
- PMID 25522934.
- PMID 27065999.
- from the original on 2024-02-18. Retrieved 2024-02-18.
- PMID 30567928.
- PMID 29183332.
- PMID 28591587.
- from the original on 2024-02-18. Retrieved 2024-02-18.
- PMID 27230380.
- PMID 26218241.
- from the original on 2024-02-18. Retrieved 2024-02-18.
- from the original on 2024-02-18. Retrieved 2024-02-18.
- PMID 27350728.
- S2CID 205225483. Archived from the originalon 2019-10-29. Retrieved 2019-10-29.
- PMID 20803699.
- PMID 25593900.
- ^ S2CID 8068289.
- PMID 25331623.
- ^ PMID 26907531.
- PMID 27156530.
- PMID 23128233.
- PMID 27230380.
- PMID 33921348.
- ^ Staff (1 July 2020). "Celsius Therapeutics Teams With Oxford, Cleveland Clinic, LMU on Single-Cell IBD Research". genomeweb. New York City: Crain Communications. Archived from the original on 2 July 2020. Retrieved 1 July 2020.
- S2CID 30604736.
- from the original on 2022-05-07. Retrieved 2022-01-28.
- ^ "IBD Facts". Archived from the original on 2013-02-12. Retrieved 2013-02-13.
- PMID 25075198.
- PMID 23864791.
- PMID 24407107.
- ISSN 1478-1239.
- PMID 26632379.
- PMID 24696607.
- ^ "Crohn's & Colitis Foundation of America". Archived from the original on 2016-07-27. Retrieved 2004-10-18.
- PMID 27979414.
- ^ PMID 15563659.
- ^ "Inflammatory Bowel Disease" (PDF). World Gastroenterology Organization. August 2015. Archived (PDF) from the original on March 14, 2016. Retrieved Mar 13, 2016.
- PMID 24175291.
- ^ PMID 24966712.
- ^ ISBN 0-7817-7153-6.
- PMID 20067425.
- PMID 19444096.
- ^ S2CID 8269837.
- ^ "Pouchitis: Symptoms & Causes". Mayo Clinic. 21 December 2018. Archived from the original on 31 October 2013. Retrieved 28 October 2019.
- ^ Karimuddin A, Gilles G. "Surgery for Abdominal/Intestinal Crohn's Disease". Trusted Therapies. Archived from the original on 23 July 2016. Retrieved 19 May 2015.
- ^ "Inflammatory Bowel Disease". Mayo Clinic. Archived from the original on November 17, 2022. Retrieved November 18, 2022.
- PMID 20532706.
- PMID 22573191.
- S2CID 24401720.
- ^ (PDF) from the original on 2023-12-01. Retrieved 2024-02-19.
- from the original on 2024-02-19. Retrieved 2024-02-19.
- S2CID 267557.
- PMID 27314323.
- S2CID 27452694.
- PMID 23064018.
- S2CID 39937720.
- PMID 27197069.
- ^ PMID 37781953.
- S2CID 46928303.
- PMID 26202194.
- S2CID 26119818.
- PMID 32678465.
- ^ PMID 32128795.
- PMID 32128794.
- PMID 30214266.
- PMID 25223604.
- from the original on 2023-10-30. Retrieved 2023-10-15.
- S2CID 207205293.
- PMID 25518050.
- PMID 26230863.
- ^ Fracas E, Costantino A, Vecchi M, Buoli M. Depressive and Anxiety Disorders in Patients with Inflammatory Bowel Diseases: Are There Any Gender Differences? International Journal of Environmental Research and Public Health. 2023; 20(13):6255. https://doi.org/10.3390/ijerph20136255
- ^ Barberio B, Zamani M, Black CJ, Savarino EV, Ford AC. Prevalence of symptoms of anxiety and depression in patients with inflammatory bowel disease: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. 2021 May;6(5):359-370. doi: 10.1016/S2468-1253(21)00014-5
- ^ from the original on 2022-05-07. Retrieved 2022-01-11.
- (PDF) from the original on 2022-08-14. Retrieved 2022-07-01.
- PMID 957999.
- PMID 11316157.
- PMID 26614685.
- from the original on 2022-11-29. Retrieved 2022-11-29.
- PMID 32297974.
- S2CID 11007309.
- (PDF) from the original on 2023-12-06. Retrieved 2024-02-19.
- PMID 27799880.
- PMID 22523611.
- PMID 22840916.
- from the original on 2022-05-07. Retrieved 2013-09-14.
- ^ "Inflammatory bowel disease". nhs.uk. 2017-10-18. Archived from the original on 2022-11-29. Retrieved 2022-11-29.
- ^ Kemp K, Griffiths J, Lovell K. Understanding the health and social care needs ofpeople living with IBD: a meta-synthesis of the evidence. World J Gastroenterol2012;18:6240–9.
- PMID 25530442.
- S2CID 13160121.
- PMID 31294381.
- PMID 23395397.
- PMID 33527789.
- ^ British Society of Gastroenterology https://www.bsg.org.uk/covid-19-advice/bsg-advice-for-management-of-inflammatory-bowel-diseases-during-the-covid-19-pandemic/ Archived 2022-04-12 at the Wayback Machine
- ^ Crohn's and Colitis Canada 2018 Impact of IBD in Canada Report. https://crohnsandcolitis.ca/About-Us/Resources-Publications/Impact-of-IBD-Report/ Archived 2022-04-07 at the Wayback Machine
- PMID 30639677.
- S2CID 2605979.
- PMID 23178819.
- PMID 20517305.
- ^ PMID 25525379.
- ^ PMID 26900283.
- PMID 15930982.
- ^ PMID 16083701.
- PMID 29285108.
- ^ S2CID 34563008.
- PMID 7541009.
- S2CID 31495688.
- S2CID 11663330.
- PMID 22442067.
- Gen. Eng. Biotechnol. News(paper). Vol. 34, no. 4. p. 14.
- PMID 26348447.
- ^ PMID 28539843.
- S2CID 3375968.
- ^ PMID 33446900.
- PMID 31083476.
- ^ from the original on 2022-01-23. Retrieved 2022-01-11.
- PMID 35086532.
- S2CID 45207412.
- (PDF) from the original on 2024-01-18. Retrieved 2024-02-19.
- PMID 21486642.
External links
- Inflammatory bowel disease at Curlie
 Media related to Inflammatory bowel diseases at Wikimedia Commons
Media related to Inflammatory bowel diseases at Wikimedia Commons
