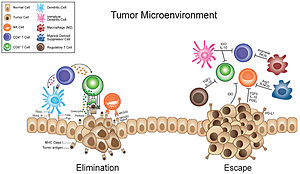
Tumor microenvironment

The tumor microenvironment is a complex ecosystem surrounding a tumor, composed of cancer cells, stromal tissue (including blood vessels, immune cells, fibroblasts and signaling molecules) and the extracellular matrix.[2][3][4][5] Mutual interaction between cancer cells and the different components of the tumor microenvironment support its growth and invasion in healthy tissues which correlates with tumor resistance to current treatments and poor prognosis. The tumor microenvironment is in constant change because of the tumor's ability to influence the microenvironment by releasing extracellular signals, promoting tumor angiogenesis and inducing peripheral immune tolerance, while the immune cells in the microenvironment can affect the growth and evolution of cancerous cells.[2][6][7][8][9]
History
The concept of the tumor microenvironment (TME) dates back to 1863 when Rudolf Virchow established a connection between inflammation and cancer. However, it wasn't until 1889 that Stephen Paget's "seed and soil" theory introduced the important role of TME in cancer metastasis, highlighting the intricate relationship between tumors and their surrounding microenvironment. The theory indicated that cancer cells have tendencies when spreading. Paget proposed that the metastases of a particular type of cancer ("the seed") often metastasizes to certain sites ("the soil") based on the similarity of the original and secondary tumor sites. In other words, just as seeds need fertile soil to grow, cancer cells require a supportive microenvironment to metastasize.[10][11]
In 1928, James Ewing challenged Paget's theory with his own perspective on cancer metastasis. Ewing proposed that the ability of cancer cells to metastasize was primarily influenced by mechanical mechanisms such as anatomical and hemodynamic factors of the vascular connection, with tumor cells more likely to be trapped in the first connected organ.[10][12] This viewpoint suggested that certain properties or mutations within cancer cells might dictate their metastatic potential, independent of the surrounding tissue environment.[10] Isaiah Fidler formulated a complementary hypothesis in the 1970s, where he proposed that while the mechanical aspects of blood flow is important, metastatic colonization specifically targets certain organs, known as organotropism.[13]
In the late 1970s, attention shifted towards understanding the role of lymphocytes within the tumor microenvironment. Reports emerged detailing the presence and activities of tumor-infiltrating T and B lymphocytes, as well as natural killer (NK) cells. Researchers observed that tumor-infiltrating T cells had both anti-tumor cytotoxicity and immune-suppressive properties. However, their cytotoxic activity was found to be lower compared to lymphocytes from distant sites, likely due to the overall immunosuppressive state in tumor-bearing individuals.[14]
Vasculature
A tumor's vasculature is important to its growth, as blood vessels deliver oxygen, nutrients, and growth factors to the tumor.[15] Tumors smaller than 1–2 mm in diameter are delivered oxygen and nutrients through passive diffusion. In larger tumors the center becomes too far away from the existing blood supply, leading the tumor microenvironment to become hypoxic and acidic.[16] Angiogenesis is upregulated to feed the cancer cells and is linked to tumor malignancy.[17]
Endothelial cells and angiogenesis
In hypoxic environments the tissue sends out signals called hypoxia inducible factors (HIFs) that can stimulate nearby endothelial cells to secrete factors such as vascular endothelial growth factor (VEGF). VEGF activates the endothelial cells, which begins the process of angiogenesis, where new blood vessels emerge from pre-existing vasculature.[18] The blood vessel formed in the tumor environment often doesn't mature properly, and as a result the vasculature formed in the tumor microenvironment differs from that of normal tissue. The blood vessels formed are often "leaky" and tortuous, with a compromised blood flow.[19][16] As tumors cannot grow large without proper vasculature, sustained angiogenesis is therefore considered one of the hallmarks of cancer.[20]
In later stages of tumor progression endothelial cells can differentiate into carcinoma associated fibroblasts, which furthers metastasis.[16]
Enhanced permeability and retention effect
The enhanced permeability and retention effect is the observation that the vasculature of tumors tend to accumulate macromolecules in the blood stream to a greater extent than in normal tissue. This is due to the "leaky" nature of the vasculature around tumors, and a lacking
Hypoxia

While angiogenesis can reduce the hypoxia in the tumor microenvironment, the partial pressure of oxygen is below 5 mmHg in over 50% of locally advanced solid tumors, compared to venous blood which has a partial pressure of oxygen at 40-60 mmHg.[18][5] A hypoxic environment leads to genetic instability by downregulating genes involved in DNA repair mechanisms such as nucleotide excision repair and mismatch repair pathways.[23] This genetic instability leads to a high number of mutated cells, and is associated with cancer progression.[5] Periods of mild and acute hypoxia and reoxygenation can lead cancer cells to adapt and grow into more aggressive phenotypes.[18]
Hypoxia causes the upregulation of hypoxia induced factors (HIFs), which are transcription factors that decides how cells respond to a lack of oxygen.[16] HIFs induces the transcription of thousands of genes, some of which induces angiogenesis or furthers metastasis, leading, for instance, to increased cell migration and matrix remodeling.[24][4] An increased HIF expression can lead tumor cells to shift their metabolism from aerobic to anaerobic, where they obtain energy through glycolysis.[25] Cells with an elevated glucose metabolism produce lactate, which decreases the pH in the microenvironment from a neutral and healthy 7.35-7.45 to an acidic 6.3-7.0. This phenomenon is described as the "Warburg effect".[25][26] HIFs also regulate immune cells, and an increased expression can lead to the inactivation of anti-tumor functions. This furthers the survival of tumor cells and hinders anti-tumor treatment.[25]
Stromal cells
Cancer is a complex disease involving both tumor cells and surrounding stromal cells. In cancer biology, the stroma is defined as the nonmalignant cells found in the supportive tissue surrounding tumors. These cells include fibroblasts, immune cells, endothelial cells, and various other cell types.[27]
Stromal cells within the tumor microenvironment represent an important cellular component in cancer development, influencing tumor metabolism, growth, metastasis, immune evasion, and resistance to chemotherapy. These cells can originate from neighboring non-cancerous stromal cells or undergo transdifferentiation from tumor cells. Stromal cells contribute to tumor initiation, progression and drug resistance, and the stroma is known to evolve as the tumor develops. Understanding the interactions between cancer cells and stromal cells is essential for developing effective cancer treatments.[27][28] Alterations in the stroma, including the activation of fibroblasts into carcinoma-associated fibroblasts (CAFs) and remodeling of the extracellular matrix (ECM), are recognized as important in cancer progression and potential targets for therapy and diagnosis.[29]
Carcinoma associated fibroblasts

Carcinoma associated fibroblasts (CAFs) are a heterogenous group of activated fibroblasts central to the reactive stroma within the tumor microenvironment. The precise definition of CAFs remains challenging due to variations in cellular origins and expression markers. However, evidence suggests CAFs originate from activated resident fibroblasts, bone marrow-derived mesenchymal stem cells (MSCs), cancer cells undergoing epithelial-mesenchymal transition (ETM), or endothelial cells trough endothelial to mesenchymal transition (EndMT).[31][32][11]
CAFs are one of the most common components of the tumor stroma and are particularly found in the interstitial spaces of breast, prostate, and pancreatic cancer.
CAFs play a dual role in
Targeting CAF has emerged as a promising strategy for improving cancer treatment, but the research faces several challenges. These include gaps in our understanding of CAF origins and their diverse functions, some of which may be helpful in combating tumors.[11][33][28]
Extracellular matrix remodeling

The extracellular matrix (ECM) is a tree-dimensional network of proteins and proteoglycans in the microenvironment and is present in all tissue. The ECM is a highly dynamic structure and is essential for tissue development, repair, support, and homeostasis.[36][37] In healthy skin, the EMC is composed of various molecules such as collagens, glycoproteins, and glycosaminoglycans that regulate functions and mechanical properties. However, in tumors, the ECM plays an important role in shaping the tumor microenvironment and influences cancer progression, metastasis, and therapeutic response. This process is called extracellular matrix remodeling and is characterized by changes in protein content and enzymatic activity which influences signal transduction and cell-matrix alterations.[38] ECM remodeling involves dynamic alterations in ECM composition, organization, and biomechanical properties. ECM remodeling is induced by factors such as hypoxia, acidosis, inflammatory cells, or proteases secreted by tumor or stromal cells.[39]
Cellular mechanisms
Cells interact with and bind to the ECM through
In addition to integrins, other cell receptors like
Impact on cancer progression
While ECM remodeling is tightly regulated under normal physiological conditions, it also modulates many of the tumor cell behaviors associated with cancer progression. This includes evasion of apoptosis, sustained angiogenesis, limitless replication potential, and tissue invasion.[43][44] In cancer, changes in the ECM dynamics lead to changes in composition, density, and mechanical properties, affecting tumor aggressiveness and response to therapy. Research suggests that both pro- and anti-tumorigenic effects occurs during ECM remodeling. In early tumor formation, stromal cells produce excess ECM proteins, causing the tissue around the tumor to stiffen. Some of the contributing factors to tumor stiffness is increased type 1 collagen and acid deposition.[43][45] Additionally, the restructured ECM and its degradation fragments (matrikines) impacts signaling pathways via cell-surface receptor interactions, leading to dysregulated stromal cell behavior and the emergence of an oncogenic microenvironment.[46]
Immune cells
Tumor-associated immune cells can be tumor-antagonizing or tumor-promoting, meaning that they can suppress or promote tumor growth.[47] Because of the effects of hypoxia, the anti-tumor abilities of many tumor-antagonizing immune cells, such as cytotoxic T cells and natural killer cells, become inhibited. Tumor-promoting immune cells such as regulatory T cells and myeloid derived suppressor cells will, on the other hand, become upregulated.[25]



Myeloid-derived suppressor cells and tumor-associated macrophages
Tumor-associated macrophages are a central component in the strong link between chronic inflammation and cancer, and are recruited to the tumor as a response to cancer-associated inflammation.[50] Their sluggish NF-κB activation allows for the smoldering inflammation seen in cancer.[51] Unlike normal macrophages, tumor-associated macrophages lack cytotoxic activity.[52] Monocyte derived macrophages are divided into inflammatory M1-polarized macrophages and anti-inflammatory M2-polarized macrophages. M1-polarized macrophages phagocytize tumor cells and are considered tumor-antagonizing.[16] M2-polarized macrophages are, on the other hand, tumor-promoting, because they promote tumor progression by suppressing immunosurveillance,[47] aiding angiogenesis by secreting vascular endothelial growth factor (VEGF)[5] and remodeling the extracellular matrix.[47] The tumor microenvironment promotes the M2-polarized macrophages, and an increased amount of tumor-associated macrophages is associated with worse prognosis.[16][53][54]
Tumor-associated macrophages are associated with using exosomes to deliver invasion-potentiating microRNA into cancerous cells, specifically breast cancer cells.[49][55]
Neutrophils
Experiments in mice have mainly shown that tumor-associated neutrophils exhibit tumor-promoting functions,[62][63][64][65] but a smaller number of studies show that neutrophils can also inhibit tumor growth.[66][67] Tumor associated neutrophils can be divided into N1- and N2-polarized neutrophils.[47] N1-polarized neutrophils accumulate in the tumor in its early stages and support with tumor cell death. In later stages N2-polarized neutrophils promotes angiogenesis by secreting vascular endothelial growth factor (VEGF).[16]
Tumor infiltrating lymphocytes
Tumor infiltrating lymphocytes are lymphocytes, including T cells, B cells and natural killer cells, that penetrate the tumor and has the ability to recognize and kill cancer cells.[68] A high concentration is generally positively correlated with good prognosis (802).[69] This type of immune cells can also block metastasis, as natural killer cells are most efficient at killing cancer cells outside of the tumor microenvironment.[16] Tumor infiltrating lymphocytes has been used in therapeutic treatments, where lab amplificated immune cells are transferred to cancer patients to help their immune system fight the cancer.[69] This treatment has seen success in solid tumors such as melanoma.[70]
Tumor infiltrating lymphocytes can become tumor-promoting due to the immunosuppressive mechanisms of the tumor microenvironment.[69] Cancer cells induce apoptosis of activated T cells by secreting exosomes containing death ligands such as FasL and TRAIL, and via the same method, turn off the normal cytotoxic response of natural killer cells.[71][72]
T cells
There are several types of T cells that are important to tumorigenesis, including cytotoxic T cells (CD8+), T helper 1 (Th-1) cells and regulatory T cells (Tregs).[16] CD8+ cells are tumor-antagonizing cells that recognize tumor antigens and targets cancer cells for destruction. In addition, CD8+ cells slow tumor progression and suppress angiogenesis by releasing interferon-gamma (IFN-γ).[16] Th-1 cells supports the activation and proliferation of CD8+ cells by secreting IFN-γ and interleukin-2 (IL-2), and by cross-presenting tumor antigens.[47] Tregs are, as opposed to CD8+, tumor promoting. They secrete tumor growth factors, and indirectly support cancer survival by interacting with endothelial cells and carcinoma associated fibroblasts.[16] Tregs also have immunosuppressive mechanisms that can make CD8+ cells less effective.[47]
T cells reach tumor sites via the vascular system, where the tumor microenvironment appears to preferentially recruit other immune cells over T cells. One such discriminating mechanism is the release of cell-type specific
T cells must replicate after arriving at the tumor site to effectively kill the cancer cells, survive hostile elements and migrate through the stroma to the cancer cells. This is affected by the tumor microenvironment. The draining lymph nodes are the likely location for cancer specific T cell replication, although this also occurs within the tumor.[3]
Research
Models
Several in vitro and in vivo models have been developed that seek to replicate the TME in a controlled environment. Tumor immortalised cell lines and primary cell cultures have been long used in order to study various tumors. They are quick to set up and inexpensive, but simplistic and prone to genetic drift.[73] 3D tumor models have been developed as a more spatially representative model of the TME. Spheroid cultures, scaffolds and organoids are generally derived from stem cells or ex vivo and are much better at recreating the tumour architecture than 2D cell cultures.[74]
Drug development
Advancements in remodeling
Therapies
Antibodies
Targeting immunoregulatory membrane receptors succeeded in some patients with
Kinase inhibitors
Mutated
Chimeric antigen receptor cell therapy
See also
- Tumor-associated endothelial cells
References
- PMID 31450598.
- ^ PMID 24310355.
- ^ PMID 25838376.
- ^ PMID 26938687.
- ^ PMID 21963199.
- PMID 26854213.
- S2CID 232432582.
- S2CID 244452599.
- PMID 37615187.
- ^ S2CID 53010974.
- ^ PMID 23114846.
- PMID 29197379.
- PMID 34685596.
- S2CID 13777357.
- PMID 34147821.
- ^ PMID 32810447.
- PMID 32993787.
- ^ PMID 34350796.
- PMID 34613483.
- PMID 36917953.
- ISBN 978-0-323-52725-5, retrieved 2024-02-19
- ^ PMID 20797419.
- PMID 33796526.
- PMID 35642641.
- ^ PMID 36212414.
- PMID 32570870.
- ^ PMID 26222075.
- ^ PMID 37666813.
- PMID 34298680.
- PMID 33763348.
- ^ PMID 36010899.
- PMID 37394578.
- ^ PMID 33712707.
- ^ PMID 37463917.
- PMID 31980749.
- PMID 25415508.
- PMID 35558554.
- PMID 35892357.
- PMID 32351878.
- ^ S2CID 202571768.
- PMID 16919434.
- PMID 31063753.
- ^ PMID 37092398.
- PMID 30678058.
- PMID 30091653.
- PMID 35008401.
- ^ S2CID 208063582.
- S2CID 4429118.
- ^ PMID 23099347.
- PMID 15766659.
- S2CID 5884781.
- PMID 20371344.
- S2CID 26116121.
- S2CID 24840259.
- PMID 21939504.
- S2CID 4393159.
- PMID 26193342.
- S2CID 21924175.
- S2CID 926930.
- PMID 25865224.
- PMID 24591638.
- PMID 25822788.
- PMID 29191879.
- PMID 25624500.
- PMID 26649828.
- PMID 25985180.
- PMID 21907922.
- ^ "tumor-infiltrating lymphocyte". www.cancer.gov. 2011-02-02. Retrieved 2024-02-19.
- ^ PMID 35165861.
- PMID 21954698.
- PMID 17409393.
- PMID 15885603.
- S2CID 20557369.
- PMID 34572836.
- S2CID 252676223.
- PMID 35701781.
- .
- PMID 22827162.
- PMID 23323560.
- PMID 3555767.
- PMID 32335505.
- PMID 32680511.
- PMID 31643906, retrieved 2024-02-20
- PMID 29455663.
- S2CID 237943611.
- PMID 35434273.
- PMID 30725979, retrieved 2024-02-20
- PMID 29103912.
- PMID 33098993.
