Keratoconus
| Keratoconus | |
|---|---|
| Other names | KC, KCN, conical cornea |
| Frequency | ~1 in 2,000 people[3] |
Keratoconus (KC) is a disorder of the
While the cause is unknown, it is believed to occur due to a combination of
Initially the condition can typically be corrected with
Keratoconus affects about 1 in 2,000 people.
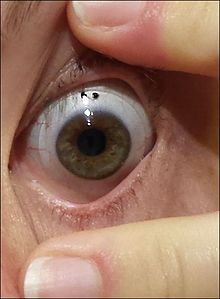
Signs and symptoms

"... a candle, when looked at, appears like a number of lights, confusedly running into one another" — Nottingham[12]
People with early keratoconus often notice a minor blurring or distortion of their vision, as well as an increased sensitivity to light, and visit their clinician seeking corrective lenses for reading or driving.

The classic symptom of keratoconus is the perception of multiple "ghost" images, known as
Genetics
Six genes have been found to be associated with the condition. These genes include
Patients with a parent, sibling, or child who has keratoconus have 15 to 67 times higher risk in developing corneal ectasia compared to patients with no affected relatives.[7][8]
Pathophysiology

Despite considerable research, the cause of keratoconus remains unclear.[18] Several sources suggest that keratoconus likely arises from a number of different factors: genetic, environmental or cellular, any of which may form the trigger for the onset of the disease.[19][20][21] Once initiated, the disease normally develops by progressive dissolution of Bowman's layer,[14] which lies between the corneal epithelium and stroma. As the two come into contact, cellular and structural changes in the cornea adversely affect its integrity and lead to the bulging and scarring characteristic of the disorder. Within any individual keratoconic cornea, regions of degenerative thinning coexisting with regions undergoing wound healing may be found. Scarring appears to be an aspect of the corneal degradation; however, a recent, large, multicenter study suggests abrasion by contact lenses may increase the likelihood of this finding by a factor over two.[22][23]
A number of studies have indicated keratoconic corneas show signs of increased activity by
A genetic predisposition to keratoconus has been observed,
Researches also have shed light on the role of hormones in the pathophysiology of keratoconus. Hormones such as androgen, prolactin, estrogen and progesterone have been shown to influence corneal biomechanics and tissue remodeling, potentially affecting the integrity of the cornea in individuals predisposed to keratoconus.[34] Moreover, fluctuations in hormonal levels during puberty and pregnancy have been associated with the onset or exacerbation of keratoconus in some cases.
Keratoconus has been associated with
Diagnosis


Prior to any
If keratoconus is suspected, the ophthalmologist or optometrist will search for other characteristic findings of the disease by means of
A handheld
Stages

Once keratoconus has been diagnosed, its degree may be classified by several metrics:[47]
- The steepness of greatest curvature from 'mild' (< 45 D), 'advanced' (up to 52 D) or 'severe' (> 52 D);
- The morphology of the cone: 'nipple' (small: 5 mm and near-central), 'oval' (larger, below-center and often sagging), or 'globus' (more than 75% of cornea affected);
- The corneal thickness from mild (> 506 μm) to advanced (< 446 μm).
Increasing use of corneal topography has led to a decline in use of these terms.[47]
| Stage | Characteristics[48][49] |
|---|---|
| Stage 1 |
|
| Stage 2 |
|
| Stage 3 |
|
| Stage 4 |
|
| Stage is determined if one of the characteristics applies. Corneal thickness is the thinnest measured spot of the cornea. | |
Treatment
Lenses

In early stages of keratoconus,
In people with keratoconus, rigid contact lenses improve vision by means of tear fluid filling the gap between the irregular corneal surface and the smooth regular inner surface of the lens, thereby creating the effect of a smoother cornea. Many specialized types of contact lenses have been developed for keratoconus, and affected people may seek out both doctors specialized in conditions of the cornea, and contact lens fitters who have experience managing people with keratoconus. The irregular cone presents a challenge[19] and the fitter will endeavor to produce a lens with the optimal contact, stability and steepness. Some trial-and-error fitting may prove necessary.[45]
Hybrid lenses
Traditionally, contact lenses for keratoconus have been the 'hard' or RGP variety, although manufacturers have also produced specialized 'soft' or
Scleral lenses
Scleral lenses are sometimes prescribed for cases of advanced or very irregular keratoconus; these lenses cover a greater proportion of the surface of the eye and hence can offer improved stability.
Piggybacking
Some people find good vision correction and comfort with a "piggyback" lens combination, in which RGP lenses are worn over soft lenses, both providing a degree of vision correction.[56] One form of piggyback lens makes use of a soft lens with a countersunk central area to accept the rigid lens. Fitting a piggyback lens combination requires experience on the part of the lens fitter, and tolerance on the part of the person with keratoconus.
Surgery
Corneal transplant
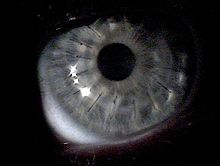

Between 11% and 27% of cases of keratoconus
The acute recovery period can take four to six weeks, and full postoperative vision stabilization often takes a year or more, but most transplants are very stable in the long term.
In the US, corneal transplants (also known as corneal grafts) for keratoconus are usually performed under sedation as
One way of reducing the risk of rejection is to use a technique called deep anterior lamellar keratoplasty (DALK). In a DALK graft, only the outermost epithelium and the main bulk of the cornea, the stroma, are replaced; the person's rearmost endothelium layer and the Descemet's membrane are left, giving some additional structural integrity to the postgraft cornea.[62] Furthermore, it is possible to transplant freeze-dried donor tissue. The freeze-drying process ensures this tissue is dead, so there is no chance of rejection.[62] Research from two trials in Iran provide low to moderate evidence that graft rejection is more likely to occur in penetrating keratoplasty than in DALK, though the likelihood for graft failure were similar with both procedures.[63]
Epikeratophakia
Rarely, a nonpenetrating keratoplasty known as an epikeratophakia (or epikeratoplasty) may be performed in cases of keratoconus. The corneal epithelium is removed and a lenticule of donor cornea is grafted on top of it.[19] The procedure requires a greater level of skill on the part of the surgeon, and is less frequently performed than a penetrating keratoplasty, as the outcome is generally less favorable. However, it may be seen as an option in a number of cases, particularly for young people.[64]
Corneal ring implants

A possible surgical alternative to corneal transplant is the insertion of intrastromal corneal ring segments. A small incision is made in the periphery of the cornea and two thin arcs of
Corneal intrastromal implantation surgery involving the implantation of a full ring is also available as a treatment option for keratoconus.[67] Evidence supports that the full-ring implant improves vision outcomes for at least a year.[68]
Cross-linking
Radial keratotomy
Radial keratotomy is a refractive surgery procedure where the surgeon makes a spoke-like pattern of incisions into the cornea to modify its shape. This early surgical option for myopia has been largely superseded by LASIK and other similar procedures. LASIK is absolutely contraindicated in keratoconus and other corneal thinning conditions as removal of corneal stromal tissue will further damage an already thin and weak cornea.[72] For similar reasons, radial keratotomy has also generally not been used for people with keratoconus.[73][74]
Prognosis

Patients with keratoconus typically present initially with mild
Corneal hydrops

In advanced cases, bulging of the cornea can result in a localized rupture of
Although disconcerting to the patient, the effect is normally temporary and after a period of six to eight weeks, the cornea usually returns to its former transparency. The recovery can be aided nonsurgically by bandaging with an osmotic saline solution. Although a hydrops usually causes increased scarring of the cornea, occasionally it will benefit a patient by creating a flatter cone, aiding the fitting of contact lenses.[76] Corneal transplantation is not usually indicated during corneal hydrops.
Epidemiology
The National Eye Institute reports keratoconus is the most common corneal dystrophy in the United States, affecting about one in 2,000 Americans,[77][78] but some reports place the figure as high as one in 500.[79] In the pediatric populations, ages three to 18, the prevalence of keratoconus was found to be as high as one in 334 children.[80] The inconsistency may be due to variations in diagnostic criteria,[14] with some cases of severe astigmatism interpreted as those of keratoconus, and vice versa.[45] A long-term study found a mean incidence rate of 2.0 new cases per 100,000 population per year.[78] Some studies have suggested a higher prevalence amongst females,[81] or that people of South Asian ethnicity are 4.4 times as likely to develop keratoconus as Caucasians, and are also more likely to be affected with the condition earlier.[82]
Keratoconus is normally bilateral[78] (affecting both eyes) although the distortion is usually asymmetric and is rarely completely identical in both corneas.[14] Unilateral cases tend to be uncommon, and may in fact be very rare if a very mild condition in the better eye is simply below the limit of clinical detection.[45] It is common for keratoconus to be diagnosed first in one eye and not until later in the other. As the condition then progresses in both eyes, the vision in the earlier-diagnosed eye will often remain poorer than that in its fellow.
History

The German
By 1869, when the pioneering Swiss ophthalmologist
Society and culture
According to the findings of the Collaborative Longitudinal Evaluation of Keratoconus (CLEK), people who have keratoconus could be expected to pay more than $25,000 over their lifetime post-diagnosis, with a standard deviation of $19,396.
Related disorders
Several other corneal ectatic disorders also cause thinning of the cornea:[45]
- Keratoglobus is a very rare condition that causes corneal thinning primarily at the margins, resulting in a spherical, slightly enlarged eye. It may be genetically related to keratoconus.[19]
- Pellucid marginal degeneration causes thinning of a narrow (1–2 mm) band of the cornea, usually along the inferior corneal margin. It causes irregular astigmatism that, in the early stages of the disease can be corrected by spectacles. Differential diagnosis may be made by slit-lamp examination.[30][93]
- Posterior keratoconus, a distinct disorder despite its similar name, is a rare abnormality, usually congenital, which causes a nonprogressive thinning of the inner surface of the cornea, while the curvature of the anterior surface remains normal. Usually only a single eye is affected.[19]
- Post-LASIK ectasia is a complication of LASIK eye surgery.
References
- ^ "Keratoconus". NORD (National Organization for Rare Disorders). Archived from the original on 19 February 2017.
- ^ "Keratoconus" (PDF). The University of Texas Health Science Center at San Antonio. Archived (PDF) from the original on 8 September 2017.
- ^ a b c d e f g h i j k l m n o p "Facts About the Cornea and Corneal Disease". NEI. May 2016. Archived from the original on 22 November 2016. Retrieved 5 November 2016.
- ^ a b "Cornea Research Foundation of America - Keratoconus". www.cornea.org.
- S2CID 204029105.
- ^ PMID 20537579.
- ^ PMID 27625877.
- ^ PMID 10951465.
- ^ a b "FDA approves first corneal cross-linking system for treatment". www.aoa.org. Retrieved 21 May 2019.
- ^ "Keratoconus - NORD".
- ^ "Keratoconus Origin". dictionary.com. Archived from the original on 8 January 2016. Retrieved 2 November 2015.
- ^ a b Nottingham J. Practical observations on conical cornea: and on the short sight, and other defects of vision connected with it. London: J. Churchill, 1854.
- ^ ISBN 978-0-323-02315-3.
- ^ a b c d e f g h i Epstein A (2000). "Keratoconus and related disorders" (PDF). North Shore Contact Lens. Archived from the original (PDF) on 8 February 2012. Retrieved 8 September 2007.
- PMID 17553566.
- PMID 19029032.
- ^ PMID 28676647.
- ^ a b c d e f g Caroline P, Andre M, Kinoshita B, Choo J. "Etiology, Diagnosis, and Management of Keratoconus: New Thoughts and New Understandings". Pacific University College of Optometry. Archived from the original on 7 January 2009. Retrieved 15 December 2008.
- ^ ISBN 978-0-8151-3654-5.
- ^ a b c Brown D. National Keratoconus Foundation: Research Overview. http://www.nkcf.org Archived 22 March 2004 at the Wayback Machine. Accessed 12 February 2006.
- ^ Warren, Catherine. What Causes Keratoconus? National Keratoconus Foundation. "What is Keratoconus Disease - Bulging Eye Disease Causes, Symptoms | NKCF". Archived from the original on 11 December 2013. Retrieved 30 March 2015. (14 March 2015)
- S2CID 220574540.
- ^ "The Collaborative Longitudinal Evaluation of Keratoconus (CLEK) Study Archive". Archived from the original on 30 June 2007.
- S2CID 22361390.
- S2CID 45104769.
- PMID 9008637.
- S2CID 25238570.
- S2CID 46643398.
- PMID 9856763. Archived from the originalon 3 October 2016. Retrieved 25 June 2016.
- ^ ISBN 978-0-7817-4206-1.
- ^ ISBN 978-1-57444-839-9.
- PMID 21996275.
- PMID 9493273.
- S2CID 249545241.
- ^ ISBN 978-1-4160-2973-1.
- PMID 18997547.
- PMID 14632614.
- PMID 10906086.
- S2CID 40534579.
- PMID 15734005.
- S2CID 8978974.
- S2CID 38203263.
- ISBN 978-0-7216-5209-2.
- ^ PMID 7767020.
- ^ PMID 6230745.
- PMID 2757091.
- ^ a b Gupta D. "Keratoconus: A clinical update" (PDF). Archived from the original (PDF) on 15 May 2006. Retrieved 26 March 2006.
- PMID 19431926.
- S2CID 72600086.
- ^ Vogt's striae in keratoconus, University of Iowa Health Care, Ophthalmology and Visual Sciences Archived 13 August 2016 at the Wayback Machine
- RNIB. Archivedfrom the original on 24 April 2014. Retrieved 20 January 2009.
- PMID 16303411.
- ^ "SoftPerm Hybrid Contact Lenses Discontinued". Archived from the original on 12 October 2010.
- ^ Davis Robert, Eiden Barry. Hybrid Contact Lens Management. Contact Lens Spectrum: "Contact Lens Spectrum". Archived from the original on 23 December 2010. Retrieved 12 October 2010..
- PMID 9395869.
- PMID 7490414.
- PMID 15905944.
- ^ S2CID 45054428.
- ]
- PMID 16488955.
- PMID 2381677.
- ^ a b Sugita J (1997). "Advances in Corneal Research: Selected Transactions of the World Congress on the Cornea". IV: 163–166.
{{cite journal}}: Cite journal requires|journal=(help) - PMID 25055058.
- PMID 11310764.
- ^ ISBN 978-0-323-01634-6.
- S2CID 23437970.
- ^ "Intracorneal ring: A good alternative to LASIK?". Ophthalmology Times, Europe. 1 October 2007. Retrieved 9 May 2020.[permanent dead link]
- S2CID 172136088.
- PMID 25803325.
- ^ "203324Orig2s000" (PDF). Retrieved 21 May 2019.
- ^ "The Save Sight Keratoconus Registry". Keratoconus Australia. Retrieved 9 June 2020.
- PMID 11709027.
- PMID 12648653.
- PMID 16303397.
- .
- ^ PMID 10703124.
- ^ US National Eye Institute, Facts About The Cornea and Corneal Disease Keratoconus Archived 31 October 2005 at the Wayback Machine. Accessed 12 February 2006.
- ^ PMID 3513592.
- ^ Weissman BA, Yeung KK. Keratoconus. eMedicine: Keratoconus Archived 12 January 2006 at the Wayback Machine. Accessed 24 December 2011.
- PMID 38345011.
- PMID 16083843.
- PMID 11040911.
- ^ Bowman W, On conical cornea and its treatment by operation. Ophthalmic Hosp Rep and J R Lond Ophthalmic Hosp. 1859;9:157.
- ^ Horner JF, Zur Behandlung des Keratoconus. Klinische Monatsblätter für Augenheilkunde. 1869.
- PMID 2677884.
- PMID 16693468.
- ^ Castroviejo, R.: International Abstract of Surgery, 65:5, December 1937.
- PMID 21310384.
- PMID 27163622.
- PMID 26315704.
- ^ Walker N. "Corneal cross-linking patients need Medicare rebate". Optometry Australia. Archived from the original on 12 November 2016. Retrieved 12 November 2016.
- ^ "Cost-Benefit Analysis of Corneal Transplant" (PDF). Restoresight.org. Archived from the original (PDF) on 5 March 2017. Retrieved 12 November 2016.
- PMID 21185225.
External links
- Keratoconus at Curlie
