Sweat gland
| Sweat gland | |
|---|---|
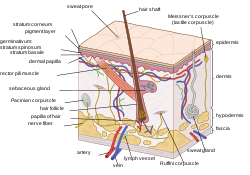 A cross-section of the human skin, with the sweat gland labeled at the bottom | |
| Details | |
| Precursor | Ectoderm[3] |
| System | Integumentary[3] |
| Nerve | Eccrine: cholinergic sympathetic nerves[4] Apocrine: adrenergic nerves[5] |
| Identifiers | |
| Latin | glandula sudorifera[1][2] |
| MeSH | D013545 |
| TA98 | A16.0.00.029 |
| TA2 | 7079 |
| FMA | 59152 |
| Anatomical terminology | |
Sweat glands, also known as sudoriferous or sudoriparous glands, from
- Eccrine sweat glands are distributed almost all over the human body, in varying densities, with the highest density in palms and soles, then on the head, but much less on the trunk and the extremities. Their water-based secretion represents a primary form of cooling in humans.[8]
- Apocrine sweat glands are mostly limited to the axillae (armpits) and perineal area in humans.[8] They are not significant for cooling in humans, but are the sole effective sweat glands in hoofed animals, such as the camels, donkeys, horses, and cattle.[9][10][11]
Structure

Generally, sweat glands consist of a secretory unit that produces sweat, and a duct that carries the sweat away. The secretory coil or base, is set deep in the lower
Each sweat gland receives several
| Eccrine Glands | Apocrine Glands | |
|---|---|---|
| Overall diameter of secretory coil | 500-700 µm
|
800 µm |
| Diameter of individual secretory tubule | 30-40 µm | 80-100 µm[18] |
| Composition of secretory epithelium | single layer, mixed clear cells & dark cells | single layer columnar cells[16] |
| Composition of ductal epithelium | two or more layers of cuboidal cells | double layer of cuboidal cells [19] |
| Duct opens to | skin surface | hair follicle, sometimes nearby skin surface |
Distribution

The number of active sweat glands varies greatly among different people, though comparisons between different areas (ex. axillae vs. groin) show the same directional changes (certain areas always have more active sweat glands while others always have fewer).[20] According to Henry Gray's estimates, the palm has around 370 sweat glands per cm2; the back of the hand has 200 per cm2; the forehead has 175 per cm2; the breast, abdomen, and forearm have 155 per cm2; and the back and legs have 60–80 per cm2.[2]
In the finger pads, sweat glands pores are somewhat irregularly spaced on the
Other animals
Non-primate mammals have eccrine sweat glands only on the palms and soles. Apocrine glands cover the rest of the body, though they are not as effective as humans' in temperature regulation (with the exception of horses').[8] Prosimians have a 1:20 ratio of follicles with apocrine glands versus follicles without.[21] They have eccrine glands between hairs over most of their body (while humans have them between the hairs on their scalp).[9]
The overall distribution of sweat glands varies among primates: the
Domestic animals[
Dogs and cats have apocrine glands that are specialized in both structure and function located at the eyelids (
History
The pores of eccrine sweat pores were first identified by the Italian physiologist Marcello Malpighi. Sweat glands themselves were first discovered by the Czech physiologist, Johannes Purkinjé in 1833. The differing densities of sweat glands in different body regions was first investigation in 1844 by the German anatomist Karl Krause. Sweat glands were first separated into kinds by the French histologist Louis-Antoine Ranvier, who separated them in 1887 regarding their type of secretion into holocrine glands (sebaceous glands) and the merocrine glands (sweat glands), the latter were then in 1917 divided into apocrine and eccrine sweat glands. In 1987, apoeccrine glands were identified.[25]
Types
Eccrine
Eccrine sweat glands are everywhere except the lips, ear canal, prepuce, glans penis, labia minora, and clitoris. They are ten times smaller than apocrine sweat glands, do not extend as deeply into the dermis, and excrete directly onto the surface of the skin.[8][5][26][4] The proportion of eccrine glands decreases with age.[27]
The clear secretion produced by eccrine sweat glands is termed
The total volume of sweat produced depends on the number of functional glands and the size of the surface opening. The degree of secretory activity is regulated by neural and hormonal mechanisms (men sweat more than women). When all of the eccrine sweat glands are working at maximum capacity, the rate of perspiration for a human being may exceed three liters per hour,[28] and dangerous losses of fluids and electrolytes can occur.
Eccrine glands have three primary functions:
- Thermoregulation: sweat (through evaporation and evaporative heat loss) can lead to cooling of the surface of the skin and a reduction of body temperature.[29]
- Excretion: eccrine sweat gland secretion can also provide a significant excretory route for water and electrolytes.[30]
- Protection: eccrine sweat gland secretion aids in preserving the skin's acid mantle, which helps protect the skin from colonization from bacteria and other pathogenic organisms.[31]
Apocrine
Apocrine sweat glands are found in the armpit, areola (around the nipples), perineum (between the anus and genitals), in the ear, and the eyelids. The secretory portion is larger than that of eccrine glands (making them larger overall). Rather than opening directly onto the surface of the skin, apocrine glands secrete sweat into the pilary canal of the hair follicle. [8]
Before puberty, the apocrine sweat glands are inactive;[32] hormonal changes in puberty cause the glands to increase in size and begin functioning.[33] The substance secreted is thicker than eccrine sweat and provides nutrients for bacteria on the skin: the bacteria's decomposition of sweat is what creates the acrid odor.[34] Apocrine sweat glands are most active in times of stress and sexual excitement.[35]
In mammals (including humans), apocrine sweat contains pheromone-like compounds to attract other organisms within their species. Study of human sweat has revealed differences between men and women in apocrine secretions and bacteria.[36]
Apoeccrine
Some human sweat glands cannot be classified as either apocrine or eccrine, having characteristics of both; such glands are termed apoeccrine.[37] They are larger than eccrine glands, but smaller than apocrine glands.[38] Their secretory portion has a narrow portion similar to secretory coils in eccrine glands as well as a wide section reminiscent of apocrine glands.[39]
Apocrine, found in the armpits and perianal region, have ducts opening onto the skin surface.[40] They are presumed to have developed in puberty from the eccrine glands,[41] and can comprise up to 50% of all axillary glands. Apoeccrine glands secrete more sweat than both eccrine and apocrine glands, thus playing a large role in axillary sweating.[42] Apoeccrine glands are sensitive to cholinergic activity, though they can also be activated via adrenergic stimulation.[37] Like eccrine glands, they continuously secrete a thin, watery sweat.[42]
Others
Specialized sweat glands, including the
Sweat
Sweat glands are used to regulate temperature and remove waste by secreting water,
Mechanism

Both apocrine and eccrine sweat glands use
Secretion of sweat occurs when the
Normally, only a certain number of sweat glands are actively producing sweat. When stimuli call for more sweating, more sweat glands are activated, with each then producing more sweat.[54][55]
Stimuli
Thermal
Both eccrine and apocrine sweat glands participate in thermoregulatory sweating,
Emotional
Emotional sweating is stimulated by stress, anxiety, fear, and pain; it is independent of ambient temperature. Acetylcholine acts on the eccrine glands and adrenaline acts on both eccrine and apocrine glands to produce sweat.[37] Emotional sweating can occur anywhere, though it is most evident on the palms, soles of the feet, and axillary regions.[29] Sweating on the palms and soles is thought to have evolved as a fleeing reaction in mammals: it increases friction and prevents slipping when running or climbing in stressful situations.[56]
Gustatory
Gustatory sweating refers to thermal sweating induced by the ingestion of food. The increase in metabolism caused by ingestion raises body temperature, leading to thermal sweating. Hot and spicy foods also lead to mild gustatory sweating in the face, scalp and neck:
Antiperspirant
Unlike
On apocrine glands, antiperspirants also contain
Pathology
Some diseases of the sweat glands include:
- Fox-Fordyce disease
- The apocrine sweat glands become inflamed, causing a persistent, itchy rash, usually in the axillae and pubic areas.[62]
- Frey's Syndrome
- If the auriculotemporal nerve is damaged (most often as a result of a Parotidectomy), excess sweat can be produced in the rear of the cheek area (just below the ear) in response to stimuli that cause salivation.[63]
- Heatstroke
- When the eccrine glands become exhausted and unable to secrete sweat. Heatstroke can lead to fatal hyperpyrexia (extreme rise in body temperature).[60]
- Hidradenitis suppurativa
- Occurs when the skin and sweat glands become inflamed with swollen lumps. These are typically painful and break open, releasing fluid or pus. The most commonly affected areas are the underarms, under the breasts, and the groin.
- Hyperhidrosis
- (also known as polyhidrosis or sudorrhea) is a pathological, excessive sweating that can be either generalized or localized (focal hyperhidrosis); focal hyperhidrosis occurs most often on the palms, soles, face, scalp and axillae. Hyperhidrosis is usually brought on by emotional or thermal stress,[64] but it can also occur or with little to no stimulus.[60] Local (or asymmetrical) hyperhidrosis is said to be caused by problems in the sympathetic nervous system: either lesions[64] or nerve inflammation.[65] Hyperhidrosis can also be caused by trench foot or encephalitis.[65]
- Milaria rubra
- Also called prickly heat. Milaria rubra is the rupture of sweat glands and migration of sweat to other tissues. In hot environments, the skin's horny layer can expand due to sweat retention, blocking the ducts of eccrine sweat glands. The glands, still stimulated by high temperatures, continues to secrete. Sweat builds up in the duct, causing enough pressure to rupture the duct where it meets the epidermis. Sweat also escapes the duct to adjacent tissues (a process called milaria).[60][66] Hypohydrosis then follows milaria (postmiliarial hypohydrosis).[67]
- Osmidrosis
- Often called bromhidrosis, especially in combination with hyperhidrosis. Osmohidrosis is excessive odor from apocrine sweat glands (which are overactive in the axillae).[64] Osmidrosis is thought to be caused by changes in the apocrine gland structure rather than changes in the bacteria that acts on sweat.[53]
Tumors
Sweat gland tumors include:[68][69]
- Acrospiroma
- Aggressive digital papillary adenocarcinoma
- Apocrine gland carcinoma
- Ceruminoma
- Cutaneous myoepithelioma
- Cylindroma
- Eccrine carcinoma
- Hidradenoma papilliferum
- Hidrocystoma
- Microcystic adnexal carcinoma
- Mucinous carcinoma
- Papillary eccrine adenoma
- Poroma
- Porocarcinoma
- Syringadenoma papilliferum
- Syringofibroadenoma
- Syringoma
Adenolipomas are
As signs in other illnesses
Many diseases cause sweat gland dysfunction:
- Acromegaly, a result of excess growth hormone, causes the size of sweat glands increase, which leads to thicker skin.[71]
- aquaporin 5 in the sweat glands.[72]
- Cystic fibrosis can be diagnosed by a sweat test, as the disease causes the sweat glands ducts to reabsorb less chloride, leading to higher concentrations of chloride in the secreted sweat.[73]
- Ectodermal dysplasia can present a lack of sweat glands.[74]
- Fabry disease, characterized by excess globotriaosylceramide (GL3), causes a decrease in sweat gland function due to GL3 deposits in the eccrine glands.[75]
- GM1 gangliosidoses, characterized by abnormal lipid storage, leads to vacuolization in eccrine sweat gland cells.[76]
- Hunter syndrome can include metachromin granules and mucin in the cytoplasm of the eccrine sweat gland cells.[77]
- thyroid hormone lead to decreased secretions from sweat glands; the result is dry, coarse skin.[78]
- mitochondria in eccrine sweat glands.[79]
- polyglucosan deposits. These "Lafora bodies" appear in the ducts of sweat glands, as well as the myoepithelial cells of apocrine glands.[80]
- lymphoid infiltrate around eccrine sweat glands.[81]
- Metachromatic leukodystrophy, a lysosomal storage disease, leads to the accumulation of lipopigments and lysosomal residual bodies in the epithelial cells of sweat glands.[82]
- Neuronal ceroid lipofuscinosis causes abnormal deposits of lipopigment in sweat gland epithelial cells (among other places).[83]
- Neutral lipid storage disease includes abnormal lipid deposits in cells, including those of the sweat gland.[84]
- lipid storage disease, includes abnormal lipid storage in sweat glands.[85]
- Schindler disease causes cytoplasmic vacuoles that appear to be empty or contain filamentous material to manifest in eccrine sweat gland cells.[86]
- Small fiber peripheral neuropathy can damage the nerves that control the sweat glands. The sweat gland nerve fiber density test can diagnose this condition.[87]
See also
Gallery
 |
 |
Notes
- ^ TA A16.0.00.029
- ^ a b c d e Gray, Henry (1918). "The Organs of the Senses and the Common Integument". Anatomy of the Human Body (20th ed.). Philadelphia: Lea & Febiger.
- ^ a b Neas, John F. "Development of the Integumentary System". In Martini, Frederic H.; Timmons, Michael J.; Tallitsch, Bob (eds.). Embryology Atlas (4th ed.). Benjamin Cumings. Archived from the original on 2012-08-08.
- ^ a b Krstic 2004, p. 464.
- ^ a b c Krstic 2004, p. 466.
- ^ "sudoriferous". The New Oxford American Dictionary (2nd ed.).
- ^ a b "sweat gland". Miller-Keane Encyclopedia & Dictionary of Medicine, Nursing, and Allied Health (7th ed.). Saunders. 2003. Retrieved 18 December 2012.
- ^ a b c d e f Kurosumi, Shibasaki & Ito 1984, p. 255.
- ^ a b Folk & Semken 1991, p. 181.
- PMID 5428889.
- ^ Sørensen & Prasad 1973, p. 173.
- ISBN 9781893357259. Archived from the originalon 2011-04-21.
- ^ Caceci, Thomas. "Integument I: Skin". VM8054 Veterinary Histology Laboratory Exercises. Virginia–Maryland Regional College of Veterinary Medicine. Archived from the original on 6 January 2013. Retrieved 19 December 2012.
- ^ Kurosumi, Shibasaki & Ito 1984, p. 256.
- ^ Eroschenko 2008, pp. 222, 226, 228.
- ^ ISBN 978-0723435716.)
{{cite book}}: CS1 maint: multiple names: authors list (link - PMID 7525893.
- ^ Wilke et al. 2007, pp. 173, 175.
- ^ a b Eroschenko 2008, p. 228.
- ^ a b Randall 2012.
- ^ Folk & Semken 1991, p. 182.
- ^ Folk & Semken 1991, p. 183.
- ^ Merck Sharp; Dohme Corp. "Cutaneous Apocrine Gland Tumors". The Merck Veterinary Manual.
- ISBN 9780721686073.
- PMID 23849497.
- ISBN 9780521200486.
- ^ Wilke et al. 2007, pp. 175–176.
- ISBN 9780072439403.
- ^ a b c Wilke et al. 2007, p. 170.
- ^ a b Romich 2009, p. 203.
- OL 5915977M.
- ^ "apocrine sweat gland". Mosby's Medical Dictionary (8th ed.). Elsevier. 2009, cited in "apocrine sweat gland". The Free Dictionary. Farlex. Retrieved 6 June 2013.
- ISBN 978-3-642-97933-0.
- ^ Dorland's Medical Dictionary for Health Consumers. Saunders. 2007,
{{cite encyclopedia}}: Missing or empty|title=(help) cited in "apocrine sweat gland". The Free Dictionary. Farlex. Retrieved 6 June 2013. - ^ The American Heritage Medical Dictionary. Houghton Mifflin Company. 2007,
{{cite encyclopedia}}: Missing or empty|title=(help) cited in "apocrine sweat gland". The Free Dictionary. Farlex. Retrieved 6 June 2013. - ^ Currie, Ariel; Coshnear, Hank; Quinn, Mila; Sand, Logan. "Human Pheromones". Macalaster College. Archived from the original on 12 May 2013. Retrieved 6 June 2013.
- ^ a b c d e Wilke et al. 2007, p. 171.
- ISBN 9781597452472.
- ISBN 978-3-8055-7306-1.
- ISBN 978-3805573061.
- ^ a b Wilke et al. 2007, p. 175.
- ^ a b Wilke et al. 2007, p. 176.
- ^ ISBN 9781402737886.
- ^ Romich 2009, p. 206.
- ISBN 9781402072574.
- ^ Eroschenko 2008, p. 215.
- ISBN 978-1416024439.
- ^ Slegers 1964, p. 271.
- ^ ISBN 9781849960267.
- ^ "Apocrine Sweat Glands". Histology@Yale. Archived from the original on 7 August 2020. Retrieved 23 March 2019.
- ^ Slegers 1964, p. 265.
- ^ Slegers 1964, p. 272.
- ^ a b Tsai 2006, p. 497.
- ^ Shibasaki, Wilson & Crandall 2006, p. 1694.
- PMID 16695370.
- ^ a b Folk & Semken 1991, p. 180.
- ^ Shibasaki, Wilson & Crandall 2006, p. 1693.
- ^ Kasture et al. 2008, p. 15.15.
- ^ Kasture et al. 2008, p. 15.14.
- ^ a b c d "skin disease". Britannica Online Encyclopedia. Encyclopædia Britannica, Inc. Retrieved 18 December 2012.
- ^ a b Kasture et al. 2008, p. 15.16.
- ^ "disease". Dorland's Medical Dictionary for Health Consumers. Saunders. 2007. Retrieved 3 January 2013.
- PMID 16822997.
- ^ a b c Tsai 2006, p. 496.
- ^ a b "hyperhidrosis". Britannica Online Encyclopedia. Encyclopædia Britannica, Inc. Retrieved 18 December 2012.
- ^ James, Berger & Elston 2011, p. 19.
- ^ James, Berger & Elston 2011, p. 20.
- ^ James, Berger & Elston 2011.
- S2CID 235714739.
- ^ James, Berger & Elston 2011, p. 612.
- ^ Rubin & Strayer 2011, p. 1043.
- ^ James, Berger & Elston 2011, p. 210.
- ISBN 9780781770309.
- ^ "Ectodermal dysplasia". MedlinePlus Medical Encyclopedia. U.S. National Library of Medicine. Retrieved 2 January 2013.
- ISBN 9789048190331.
- S2CID 43884684.
- ^ James, Berger & Elston 2011, p. 534.
- ^ Rubin & Strayer 2011, p. 1048.
- ISBN 9789061938071.
- PMID 1469407.
- ^ James, Berger & Elston 2011, p. 223–224.
- PMID 2486156.
- S2CID 22200975.
- ^ James, Berger & Elston 2011, p. 555.
- S2CID 28257992.
- ISBN 9783211993903.
- ^ "Sweat Gland Nerve Fiber Density". Therapath. Archived from the original on 2013-12-08. Retrieved 2013-08-05.
References
- Eroschenko, Victor P. (2008). "Integumentary System". DiFiore's Atlas of Histology with Functional Correlations. Lippincott Williams & Wilkins. pp. 212–234. ISBN 9780781770576.
- Folk, G. Edgar Jr.; Semken, A. Jr. (1 September 1991). "The evolution of sweat glands". International Journal of Biometeorology. 35 (3): 180–186. S2CID 28234765.
- Kasture, P. V.; Gokhal, S. B.; Parakh, S. R.; Paradkar, A. R. (7 September 2008). Pharmaceutics-II: Second Year Diploma in Pharmacy (10 ed.). Nirali Prakashan. pp. 15.14–15.16. ISBN 9788185790220.
- Kurosumi, Kazumasa; Shibasaki, Susumu; Ito, Toshiho (1984). "Cytology of the Secretion in Mammalian Sweat Glands". In Bourne, Geoffrey H.; Danielli, James F. (eds.). Protein Diffusion in Cell Membranes: Some Biological Implications. Orlando, Florida: Academic Press. pp. 253–330. ISBN 9780123644879.
- James, William D.; Berger, Timothy G.; Elston, Dirk M. (2011). Andrews' Diseases of the Skin: Clinical Dermatology (11th ed.). London: Elsevier. ISBN 9781437703146.
- Krstic, Radivoj V. (18 March 2004). Human Microscopic Anatomy: An Atlas for Students of Medicine and Biology. Springer. pp. 464, 466–469. ISBN 9783540536666.
- Rubin, Raphael; Strayer, David Sheldon (29 March 2011). Rubin's Pathology: Clinicopathologic Foundations of Medicine. Lippincott Williams & Wilkins. pp. 1043, 1048. ISBN 9781605479682.
- Shibasaki, Manabu; Wilson, Thad E.; Crandall, Craig G. (2006). "Neural control and mechanisms of eccrine sweating during heat stress and exercise". Journal of Applied Physiology. 100 (5): 1692–1701. PMID 16614366.
- Sørensen, Vibeke W.; Prasad, Gaya (1973). "On the fine structure of horse sweat glands". Zeitschrift für Anatomie und Entwicklungsgeschichte. 139 (2): 173–183. S2CID 9847627.
- Slegers, J. F. G. (1964). "The mechanism of sweat-secretion". Pflügers Archiv für die gesamte Physiologie des Menschen und der Tiere. 279 (3): 265–273. S2CID 9644549.
- Tsai, Ren-Yu (1 January 2006). "Treatment of Excessive Axillary Sweat Syndrome (Hyperhidrosis, Osmidrosis, Bromhidrosis) with Liposuction". In Shiffman, Melvin A.; Di Giuseppe, Alberto (eds.). Liposuction: Non-Cosmetic Applications. Germany: Springer. pp. 496–497. ISBN 9783540280439.
- Wilke, K.; Martin, A.; Terstegen, L.; Biel, S. S. (June 2007). "A short history of sweat gland biology". International Journal of Cosmetic Science. 29 (3): 169–179. PMID 18489347.
