Chronic pulmonary aspergillosis
| Chronic pulmonary aspergillosis | |
|---|---|
haemoptysis, fatigue, malaise, chest pain, sputum production, fever[1] | |
| Risk factors | Underlying respiratory disease,[2] genetic defects[3] |
| Diagnostic method | Via imaging (chest X-ray, high resolution CT scanning)[4] |
| Differential diagnosis | Lung cancer, tuberculosis, other fungal infections[5] |
| Treatment | Antifungal medications (oral or intravenous),[6][7] surgery,[6] glucocorticoids[8] |
| Prognosis | Approximately 20-40% mortality at 3 years; 50-80% at 7-10 years[9][10][11] |
Chronic pulmonary aspergillosis is a long-term fungal infection caused by members of the
Classification
Chronic pulmonary aspergillosis as a term encompasses a number of different presentations of varying severity. There is considerable overlap between disease forms which adds to confusion during diagnosis. The primary differentiation comes from radiological findings and serology.[8]
Aspergilloma
An aspergilloma is a fungus ball composed of Aspergillus hypha - the long filamentous strands which extend from the fungus to enable growth and reproduction.[13] They can arise within any bodily cavity, though in chronic pulmonary aspergillosis they form within pulmonary cavities that have been colonized by Aspergillus spp. If there is a single, stable cavity that provides minimal symptoms, the term 'simple aspergilloma' is commonly used to distinguish it from more severe forms of chronic pulmonary aspergillosis.[1]
Aspergillus nodule
Aspergillus can form single or multiple
Chronic cavitary pulmonary aspergillosis
When people without immunocompromise undergo formation of one or more pulmonary cavities, this is called chronic cavitary pulmonary aspergillosis.[8] Historically it was also known as "complex aspergilloma" in contrast to a "simple aspergilloma"; this is now considered inaccurate as many cases do not have a visible aspergilloma on imaging.[16] In contrast to aspergilloma and Aspergillus nodules, the vast majority of people with chronic cavitary pulmonary aspergillosis have positive tests for IgG antibodies.[17][18]
Chronic fibrosing pulmonary aspergillosis
When chronic cavitary pulmonary aspergillosis is left untreated, it can progress to a form of aspergillosis known as chronic fibrosing pulmonary aspergillosis).[8] As a result of the ongoing inflammation over an extended period of time, extensive fibrosis of the lung parenchyma occurs. This leads to a state known colloquially as "destroyed lung", and has features resembling treated pulmonary tuberculosis.[1][19]
Chronic necrotizing pulmonary aspergillosis
Also known as subacute invasive pulmonary aspergillosis, this form of chronic pulmonary aspergillosis leads to progressive features over the course of one to three months—usually in people with some degree of immunocompromise. It is more common in people who are elderly or dependent on alcohol, or with diseases such as diabetes, malnutrition, chronic obstructive pulmonary disease or HIV/AIDS.[8][6] In contrast to chronic cavitary pulmonary aspergillosis, for example, IgG antibodies for Aspergillus or an antigen called galactomannan may be found in the blood as well as in sputum samples.[6]
Signs and symptoms
People with chronic pulmonary aspergillosis typically present with a prolonged, several month
Complications
Chronic pulmonary aspergillosis can cause bleeding into the lung parenchyma which can range from mild to life-threatening. If left untreated, as the disease progresses the fungus can spread into the bloodstream causing a state known as fungemia. This widespread infection can distribute fungal spores to other parts of the body, and lead to areas of infarction, and cause haemorrhages.[21]
Causes
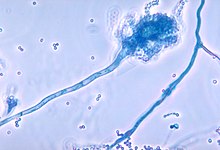
Aspergillosis is an infection caused by
The major risk factors for chronic pulmonary aspergillosis are previous cavity formation from other respiratory conditions. Examples include collapsed lungs which have formed bullae, chronic obstructive lung disease, lung cancer, and fibrocavitary sarcoidosis.[2][23] Another risk factor is immunosuppression; most commonly, this includes allogeneic stem cell transplantation, prolonged neutropaenia, immunosuppressive drug therapy, chronic granulomatous disease and haematological malignancies. Certain demographics are also at higher risk, including the elderly, male sex and those with a low body mass index.[24]
There appears to be increasing evidence for complex genetic factors increasing the risk of developing chronic pulmonary aspergillosis, such as defects to
Mechanism
The full underlying pathogenesis is not completely understood. Most people with chronic pulmonary aspergillosis have functional immune status, but usually have underlying structural damage to the lungs from an underlying process or disease. Most commonly, pre-existing pulmonary cavities from other diseases such as tuberculosis become colonised with Aspergillus conidia which have been inhaled—humans inhale between 1,000 and 10 billion spores per day, of which A. fumigatus is the most common.[27]
Aspergillomas themselves usually form in existing cavities but the cavities may form directly from chronic pulmonary aspergillosis.[8] People with pulmonary tuberculosis with a cavity larger than 2 cm appear to have a 20% increased risk of developing chronic pulmonary aspergillosis.[28]
It is postulated that conidia, once inhaled, are attacked by the host immune defences—specifically phagocytes and alveolar macrophage resident in the small airways. It is unknown whether these defences are sufficient to clear conidia or whether they are directly responsible for the inflammation leading to chronic pulmonary aspergillosis. Some Aspergillus have the ability to inhibit phagocyte nicotinamide adenine dinucleotide phosphate oxidase activation which is one of the core defence systems against filamentous fungi, which may increase susceptibility of the host to chronic pulmonary aspergillosis.[29]
Diagnosis

The diagnosis of chronic pulmonary aspergillosis is often initially considered when patients present with a history of unintentional weight loss and fatigue. Confirmation of this suspicion is normally achieved with a combination of radiological imaging and serological testing, with the goal of excluding other diagnoses like tuberculosis and finding evidence of fungus present. Whilst cavities seen on chest X-rays can raise suspicion, positive IgG testing for Aspergillus is required for confirmation.[8]
Sputum samples can be sent for culture, but where these return negative patients should undergo bronchoscopy and bronchoalveolar lavage for further culture samples.[6] Concurrent infections with non-tuberculous mycobacteria, or atypical infections such as MRSA or Pseudomonas aeruginosa are common and these can also form cavities.[8]
To confirm the presence of an aspergilloma, there needs to be radiological evidence of a round mass in the lungs with confirmatory evidence either from culture or IgG testing.
The fibrosing form—chronic fibrosing pulmonary aspergillosis—has similar criteria to chronic cavitary pulmonary aspergillosis but will be accompanied by significant fibrosis seen on either biopsy, tomosynthesis, or high resolution computed tomography.[8]
If chronic pulmonary aspergillosis has progressed to subacute invasive pulmonary aspergillosis, there must be a degree of immunosuppression. The microbiological criteria are similar to those of invasive aspergillosis but normally slower in progression, i.e. months rather than weeks.[6] Furthermore, there must be evidence of IgG or galactomannan in the blood and a confirmatory biopsy of affected tissue.[18][30]
Treatment
People with single aspergillomas generally do well with
For chronic cavitary pulmonary aspergillosis and chronic fibrosing pulmonary aspergillosis, lifelong use of antifungal medications is commonplace.
Prognosis
This section is empty. You can help by adding to it. (August 2019) |
References
- ^ PMID 12975754.
- ^ PMID 20595150.
- ^ PMID 18275280.
- S2CID 13065490.
- PMID 25778752.
- ^ PMID 26699723.
- PMID 27365388.
- ^ a b c d e f g h i j k l m n o p q Denning DW. "Clinical manifestations and diagnosis of chronic pulmonary aspergillosis". www.uptodate.com. UpToDate. Retrieved 18 August 2019.
- PMID 28179437.
- PMID 3622028.
- PMID 22349065.
- PMID 11890350.
- PMID 22121367.
- ^ PMID 27538521.
- PMID 23915502.
- PMID 24943102.
- PMID 4622826.
- ^ PMID 19068757.
- S2CID 45061168.
- PMID 31333999.
- S2CID 72764715.
- S2CID 15817761.
- S2CID 34312911.
- PMID 29190796.
- PMID 24274595.
- PMID 24712925.
- S2CID 3157271.
- PMID 10706494.
- PMID 18453606.
- ^ PMID 16110814.
- PMID 28703105.
- PMID 27806184.
- PMID 27365388.
For patients receiving triazole-based therapy for IA, prolonged azole prophylaxis, or other therapies for which drug interactions with azoles are anticipated, the committee recommends therapeutic drug monitoring (TDM) once the steady state has been reached. A moderate amount of data for itraconazole, voriconazole, and posaconazole suspension suggests this approach may be valuable in enhancing therapeutic efficacy, in evaluating therapeutic failures attributable to suboptimal drug exposures, and to minimize toxicities potentially attributable to the azoles (strong recommendation; moderate-quality evidence).
