Radiation burn
| Radiation burn | |
|---|---|
| Other names | Radiodermatitis |
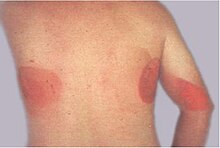 | |
| Ionizing radiation burn: large red patches of skin on the back and arm from multiple prolonged fluoroscopy procedures | |
| Specialty | Dermatology |
A radiation burn is a damage to the
The most common type of radiation
Radiation burns can also occur with high power
Types
Radiation dermatitis (also known as radiodermatitis) is a
There are three specific types of radiodermatitis: acute radiodermatitis, chronic radiodermatitis, and eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy.[3]: 39–40 Radiation therapy can also cause radiation cancer.[3]: 40
With interventional fluoroscopy, because of the high skin doses that can be generated in the course of the intervention, some procedures have resulted in early (less than two months after exposure) and/or late (two months or more after exposure) skin reactions, including necrosis in some cases.[5]: 773
Radiation dermatitis, in the form of intense erythema and vesiculation of the skin, may be observed in radiation ports.[3]: 131
As many as 95% of patients treated with radiation therapy for cancer will experience a skin reaction. Some reactions are immediate, while others may be later (e.g., months after treatment).[6]
Acute
Acute radiodermatitis occurs when an "erythema dose" of ionizing radiation is given to the skin, after which visible erythema appears up to 24 hours after.[3]: 39 Radiation dermatitis generally manifests within a few weeks after the start of radiotherapy.[4]: 143 Acute radiodermatitis, while presenting as red patches, may sometimes also present with desquamation or blistering.[7] Erythema may occur at a dose of 2 Gy radiation or greater.[8]
Chronic

Chronic radiodermatitis occurs with chronic exposure to "sub-erythema" doses of ionizing radiation over a prolonged period, producing varying degrees of damage to the skin and its underlying parts after a variable latent period of several months to several decades.
Other
Eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy is a skin condition that occurs most often in women receiving cobalt radiotherapy for internal cancer.[3]: 39–40
Radiation-induced erythema multiforme may occur when phenytoin is given prophylactically to neurosurgical patients who are receiving whole-brain therapy and systemic steroids.[3]: 130
Delayed effects
Radiation acne is a cutaneous condition characterized by comedo-like papules occurring at sites of previous exposure to therapeutic ionizing radiation, skin lesions that begin to appear as the acute phase of radiation dermatitis begins to resolve.[10]: 501
Radiation recall reactions occur months to years after radiation treatment, a reaction that follows recent administration of a chemotherapeutic agent and occurs with the prior radiation port, characterized by features of radiation dermatitis.[3][11] Restated, radiation recall dermatitis is an inflammatory skin reaction that occurs in a previously irradiated body part following drug administration.[12] There does not appear to be a minimum dose, nor an established radiotherapy dose relationship.[12]
Alpha burns
"Alpha burns" are caused by alpha particles, which can cause extensive tissue damage if inhaled.[13] Due to the keratin in the epidermal layer of the skin, external alpha burns are limited to only mild reddening of the outermost layer of skin.[14]
Beta burns
"Beta burns"—caused by beta particles—are shallow surface burns, usually of skin and less often of lungs or gastrointestinal tract, caused by beta particles, typically from hot particles or dissolved radionuclides that came to direct contact with or close proximity to the body. They can appear similar to sunburn. Unlike gamma rays, beta emissions are stopped much more effectively by materials and therefore deposit all their energy in only a shallow layer of tissue, causing more intense but more localized damage. On cellular level, the changes in skin are similar to radiodermatitis.
The dose is influenced by relatively low penetration of beta emissions through materials. The
The
Careful washing of exposed body surface, removing the radioactive particles, may provide significant dose reduction. Exchanging or at least brushing off clothes also provides a degree of protection.
If the exposure to beta radiation is intense, the beta burns may first manifest in 24–48 hours by itching and/or burning sensation that last for one or two days, sometimes accompanied by
- In first degree beta burns the damage is largely limited to epidermis. Dry or wet desquamation occurs; dry scabs are formed, then heal rapidly, leaving a depigmented area surrounded with irregular area of increased pigmentation. The skin pigmentation returns to normal within several weeks.
- Second degree beta burns lead to formation of blisters.
- Third and fourth degree beta burns result in deeper, wet ulcerated lesions, which heal with routine medical care after covering themselves with dry scab. In case of heavy tissue damage, ulcerated necrotic dermatitis may occur. Pigmentation may return to normal within several months after wound healing.[15]
Lost hair begins regrowing in nine weeks and is completely restored in about half a year.[19]
The acute dose-dependent effects of beta radiation on skin are as follows:[20]
| 0–6 Gy | no acute effect |
| 6–20 Gy | moderate early erythema |
| 20–40 Gy | early erythema in 24 hours, skin breakdown in 2 weeks
|
| 40–100 Gy | severe erythema in less than 24 hours |
| 100–150 Gy | severe erythema in less than 4 hours, skin breakdown in 1–2 weeks |
| 150–1000 Gy | blistering immediate or up to 1 day |
According to other source:[21]
| 2–6 Gy | transient erythema 2–24 h |
| 3–5 Gy | dry desquamation in 3–6 weeks |
| 3–4 Gy | temporary epilation in 3 weeks |
| 10–15 Gy | erythema 18–20 days |
| 15–20 Gy | moist desquamation |
| 25 Gy | ulceration with slow healing |
| 30–50 Gy | blistering, necrosis in 3 weeks |
| 100 Gy | blistering, necrosis in 1–3 weeks |
As shown, the dose thresholds for symptoms vary by source and even individually. In practice, determining the exact dose tends to be difficult.
Similar effects apply to animals, with fur acting as additional factor for both increased particle retention and partial skin shielding. Unshorn thickly wooled sheep are well protected; while the epilation threshold for sheared sheep is between 23 and 47 Gy (2500–5000
Energy vs penetration depth
t½ )
(year |
Yield (%) |
keV )
|
βγ
| |
|---|---|---|---|---|
155Eu
|
4.76 | 0.0803 | 252 | βγ |
| 85Kr | 10.76 | 0.2180 | 687 | βγ |
113mCd
|
14.1 | 0.0008 | 316 | β |
| 90Sr | 28.9 | 4.505 | 2826 | β |
| 137Cs | 30.23 | 6.337 | 1176 | βγ |
121mSn
|
43.9 | 0.00005 | 390 | βγ |
151Sm
|
88.8 | 0.5314 | 77 | β |
The effects depend on both the intensity and the energy of the radiation. Low-energy beta (sulfur-35, 170 keV) produces shallow ulcers with little damage to dermis, while
The electron energies from
The energy-depth-dose profile is a curve starting with a surface dose, ascending to the maximum dose in a certain depth dm (usually normalized as 100% dose), then descends slowly through depths of 90% dose (d90) and 80% dose (d80), then falls off linearly and relatively sharply though depth of 50% dose (d50). The extrapolation of this linear part of the curve to zero defines the maximum electron range, Rp. In practice, there is a long tail of weaker but deep dose, called "bremsstrahlung tail", attributable to bremsstrahlung. The penetration depth depends also on beam shape, narrower beam tend to have less penetration. In water, broad electron beams, as is the case in homogeneous surface contamination of skin, have d80 about E/3 cm and Rp about E/2 cm, where E is the beta particle energy in MeV.[24]
The penetration depth of lower-energy beta in water (and soft tissues) is about 2 mm/MeV. For a 2.3 MeV beta the maximum depth in water is 11 mm, for 1.1 MeV it is 4.6 mm. The depth where maximum of the energy is deposited is significantly lower.[25]
The energy and penetration depth of several isotopes is as follows:[26]
| isotope | half-life | specific activity (TBq/g) |
avg. (keV) |
max. (keV) |
in air (mm) |
in tissue (mm) |
comment |
|---|---|---|---|---|---|---|---|
| tritium | 12.3 years | 357 | 5.7 | 18.6 | 6 | 0.006 | no beta passes the dead layer of skin; however, tritium and its compounds may diffuse through skin |
| carbon-14 | 5730 years | 0.165 | 49 | 156 | 240 | 0.28 | about 1% of beta passes through the dead layer of skin |
sulfur-35
|
87.44 days | 1580 | 48.8 | 167.47 | 260 | 0.32 | |
phosphorus-33
|
25.3 days | 5780 | 76.4 | 248.5 | 500 | 0.6 | |
| phosphorus-32 | 14.29 days | 10600 | 695 | 1710 | 6100 | 7.6 | risk of Bremsstrahlung if improperly shielded |
For a wide beam, the depth-energy relation for dose ranges is as follows, for energies in
| MeV | surface dose % |
max. depth |
90% | 80% | 50% | 10% | Rp |
|---|---|---|---|---|---|---|---|
| 5 | 74% | 9 | 12 | 14 | 17 | 22 | 23 |
| 7 | 76% | 16 | 20 | 22 | 27 | 33 | 34 |
| 10 | 82% | 24 | 31 | 34 | 39 | 48 | 49 |
| 13 | 88% | 32 | 40 | 43 | 51 | 61 | 64 |
| 16 | 93% | 34 | 51 | 56 | 65 | 80 | 80 |
| 19 | 94% | 26–36 | 59 | 67 | 78 | 95 | 95 |
| 22 | 96% | 26–36 | 65 | 76 | 93 | 113 | 114 |
| 25 | 96% | 26–36 | 65 | 80 | 101 | 124 | 124 |
Causes
Radiation burns are caused by exposure to high levels of radiation. Levels high enough to cause burn are generally lethal if received as a whole-body dose, whereas they may be treatable if received as a shallow or local dose.
Medical imaging
Fluoroscopy may cause burns if performed repeatedly or for too long.[10]
Similarly, X-ray
A study of radiation-induced skin injuries[27][28] has been performed by the Food and Drug Administration (FDA) based on results from 1994,[29] followed by an advisory to minimize further fluoroscopy-induced injuries.[30] The problem of radiation injuries due to fluoroscopy has been further investigated in review articles in 2000,[31] 2001,[32][33] 2009[34] and 2010.[35][36][37]
Radioactive fallout
Beta burns are frequently the result of exposure to
After the
The fallout produced by the
During the Zebra test of the
The Upshot–Knothole Harry test at the Frenchman Flat site released a large amount of fallout. A significant number of sheep died after grazing on contaminated areas. The AEC however had a policy to compensate farmers only for animals showing external beta burns, so many claims were denied. Other tests on the Nevada Test Site also caused fallout and corresponding beta burns to sheep, horses and cattle.[43] During the Operation Upshot–Knothole, sheep as far as 50 miles (80 km) from the test site developed beta burns to their backs and nostrils.[42]
During underground nuclear testing in Nevada, several workers developed burns and skin ulcers, in part attributed to exposure to tritium.[44]
Nuclear accidents
Beta burns were a serious medical issue for some victims of the
The burns may manifest at different times at different body areas. The Chernobyl liquidators' burns first appeared on wrists, face, neck and feet, followed by chest and back, then by knees, hips and buttocks.[45]
Industrial radiography sources are a common source of beta burns in workers.
Radiation therapy sources can cause beta burns during exposure of the patients. The sources can be also lost and mishandled, as in the Goiânia accident, during which several people had external beta burns and more serious gamma burns, and several died. Numerous accidents also occur during radiotherapy due to equipment failures, operator errors, or wrong dosage.
Electron beam sources and particle accelerators can be also sources of beta burns.[46] The burns may be fairly deep and require skin grafts, tissue resection or even amputation of fingers or limbs.[47]
Treatment
Radiation burns should be covered by a clean, dry dressing as soon as possible to prevent infection. Wet dressings are not recommended.[48] The presence of combined injury (exposure to radiation plus trauma or radiation burn) increases the likelihood of generalized sepsis.[49] This requires administration of systemic antimicrobial therapy.[50]
See also
- Effective radiated power
- Radiation poisoning
- Radiation protection
- Therac-25
References
- ^ ARRL: RF Exposure Regulations News Archived 2008-05-17 at the Wayback Machine
- ^ ARRL: RF Radiation and Electromagnetic Field Safety
- ^ ISBN 978-0-7216-2921-6.
- ^ PMID 17785763.
- PMID 10580952.
- PMID 12024597.
- ^ ISBN 978-0-323-01198-3.
- S2CID 70923586.
- PMID 10026359.
- ^ ISBN 978-1-4160-2999-1.
- ^ Hird AE, Wilson J, Symons S, Sinclair E, Davis M, Chow E. Radiation recall dermatitis: case report and review of the literature. Current Oncology. 2008 February; 15(1):53-62.
- ^ S2CID 10211887.
- PMID 21321665.
- ^ "Multi-side Approach to the Realities of the Chernobyl NPP Accident" (PDF). Kyoto University, Research Reactor Institute. Retrieved May 16, 2019.
- ^ ISBN 978-0-8493-7004-5.
- ISBN 978-1-4398-0906-8.
- ^ ISBN 978-0-412-53710-3.
- ISBN 978-0-683-04481-2.
- ISBN 978-81-7648-312-4.
- ^ a b United States. Dept. of the Army (1990). Nuclear handbook for medical service personnel. p. 18.
- ^ Medical decision making and care of casualties from delayed effects of a nuclear detonation[permanent dead link], Fred A. Mettler Jr., New Mexico Federal Regional Medical Center
- ISBN 9780309018692.
- ISBN 978-0-7503-0860-1.
- ^ ISBN 978-0-7817-4221-4.
- ^ α, β, γ Penetration and Shielding. Fas.harvard.edu.
- ^ Isotope Safety Data Sheets
- ^ Shope, T. B. (1995). "Radiation-induced Skin Injuries from Fluoroscopy". FDA / Center for Devices and Radiological Health.
- PMID 8888398.
- PMID 8136601.
- ^ "FDA Public Health Advisory: Avoidance of Serious X-Ray-Induced Skin Injuries to Patients During Fluoroscopically-Guided Procedures". FDA / Center for Devices and Radiological Health. September 30, 1994.
- S2CID 70923586.
- PMID 11709468.
- PMID 11418390.
- PMID 19933677.
- PMID 20339253.
- PMID 20093507.
- PMID 20959547.
- ^ a b National Research Council (U.S.). Committee on Fire Research, United States. Office of Civil Defense (1969). Mass burns: proceedings of a workshop, 13–14 March 1968. National Academies. p. 248.
- ISBN 978-0-520-05852-1.
beta burns.
- ISBN 978-0-8263-0768-2.
- ISBN 978-1-56072-556-5.
- ^ ISBN 978-0-520-08323-3.
- ISBN 978-0-87417-370-3.
- ^ ISBN 978-0-8493-6159-3.
- ISBN 978-0-521-81472-0.
- PMID 7396251.
- PMID 5318671.
- ^ Of The Army, United States. Dept (1982). Nuclear handbook for medical service personnel.
- PMID 21233728.
- PMID 15080238.
