Sunburn
| Sunburn | |
|---|---|
 | |
| A sunburned neck | |
| Specialty | Dermatology |
| Complications | Skin cancer |
| Risk factors | Working outdoors, skin unprotected by clothes or sunscreen, skin type, age |
| Prevention | Use of sunscreen, sun protective clothing |
| Treatment | Avoiding further exposure to the sun. Cool, frequent baths or showers for pain relief. Anti-inflammatory medications such as ibuprofen or aspirin can also help with pain. Drinking water to stay hydrated. |
Sunburn is a form of
Sun protective measures like sunscreen and sun protective clothing are widely accepted to prevent sunburn and some types of skin cancer.[4] Special populations, including children, are especially susceptible to sunburn and protective measures should be used to prevent damage.[5]
Signs and symptoms
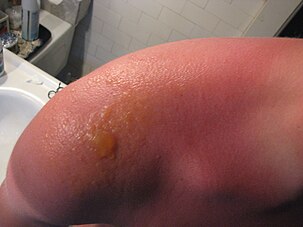
Typically, there is initial redness, followed by varying degrees of pain, the severity of which is proportional to the duration and intensity of sun exposure.[citation needed]
Other symptoms can include
Variations
Minor sunburns typically cause nothing more than slight redness and tenderness to the affected areas. In more serious cases, blistering can occur. Extreme sunburns can be painful to the point of debilitation and may require hospital care.[7]
Duration
Sunburn can occur in less than 15 minutes in response to sun exposure and in seconds when exposed to non-shielded welding arcs or other sources of intense ultraviolet light. Nevertheless, the inflicted harm is often not immediately obvious.[citation needed]
After sun exposure, the skin may turn red in as little as 30 minutes, but sunburn usually takes 2 to 6 hours. Pain is usually strongest 6 to 48 hours after exposure. The burn continues to develop for 1 to 3 days, occasionally followed by peeling skin after 3 to 8 days. Some peeling and itching may continue for several weeks.[citation needed]
Skin cancer
Ultraviolet radiation causes sunburns and increases the risk of three types of skin cancer: melanoma, basal-cell carcinoma and squamous-cell carcinoma.[1][2][8] Of greatest concern is that the melanoma risk increases dose-dependently proportional to the number of a person's lifetime cumulative episodes of sunburn.[9] An estimated 1/3 of melanomas in the United States and Australia could be prevented with regular sunscreen use.[10]
Causes
Sunburn is caused by
Melanin readily absorbs UV wavelength light, acting as a photoprotectant. By preventing UV photons from disrupting chemical bonds, melanin inhibits both the direct alteration of DNA, as well as the generation of free radicals, to prevent them from indirectly damaging DNA. However, human melanocytes contain over 2,000 genomic sites that are highly sensitive to UV, and such sites can be up to 170-fold more sensitive to UV induction of cyclobutane pyrimidine dimers than the average site[11] These sensitive sites often occur at biologically significant locations near genes.
Sunburn causes an inflammation process that includes the production of prostanoids and bradykinin. These chemical compounds increase sensitivity to heat by reducing the threshold of heat receptor (TRPV1) activation from 109 °F (43 °C) to 85 °F (29 °C).[12] The pain may be caused by the overproduction of a protein called CXCL5, which activates nerve fibers.[13]
Skin type determines the ease of sunburn. People with lighter skin tones and limited capacity to develop a tan after UV radiation exposure have a greater risk of sunburn. Fitzpatrick's Skin phototypes classification describes the normal variations of skin responses to UV radiation. Persons with type I skin have the greatest capacity to sunburn, and type VI have the least capacity to burn. However, all skin types can develop sunburn.[14]
Fitzpatrick's skin phototypes:
- Type 0: Albino
- Type I: Pale white skin, burns easily, does not tan
- Type II: White skin, burns easily, tans with difficulty
- Type III: White skin, may burn, but tans easily
- Type IV: Light brown/olive skin, hardly burns, tans easily
- Type V: Brown skin, usually does not burn, tans easily
- Type VI: Black skin, very unlikely to burn, becomes darker with UV radiation exposure[15]
Age also affects how skin reacts to the sun. Children younger than six and adults older than sixty are more sensitive to sunlight.[16]
Certain genetic conditions, for example, xeroderma pigmentosum, increase a person's susceptibility to sunburn and subsequent skin cancers. These conditions involve defects in DNA repair mechanisms which decrease the ability to repair DNA damaged by UV radiation.[17]
Medications
The risk of sunburn can be increased by
UV intensity
The
- The time of day. In most locations, the sun's rays are strongest between approximately 10 am and 4 pm daylight saving time.[19]
- Cloud cover. Clouds partially block UV, but even on an overcast day, a significant percentage of the sun's damaging UV radiation can pass through clouds.[20][21]
- Proximity to reflective surfaces, such as water, sand, concrete, snow, and ice. All of these reflect the sun's rays and can cause sunburns.
- The season of the year. The Sun's position in late spring and early summer can cause a more-severe sunburn.
- Altitude. At a higher altitude, it is easier to become burnt, because there is less of the Earth's atmosphere to block the sunlight. UV exposure increases about 4% for every 1000 ft (305 m) gain in elevation.
- Proximity to the equator (latitude). Between the polar and tropical regions, the closer to the equator, the more direct sunlight passes through the atmosphere over a year. For example, the southern United States gets fifty percent more sunlight than the northern United States.

Because of variations in the intensity of UV radiation passing through the atmosphere, the risk of sunburn increases with proximity to the
The skin and eyes are most sensitive to damage by UV at 265–275 nm wavelength, which is in the lower UVC band that is rarely encountered except from artificial sources like welding arcs. Longer wavelengths of UV radiation cause most sunburn because those wavelengths are more prevalent in ground-level sunlight.[citation needed]
Ozone depletion
In recent decades, the incidence and severity of sunburn have increased worldwide, partly because of chemical damage to the atmosphere's ozone layer. Between the 1970s and the 2000s, average stratospheric ozone decreased by approximately 4%, contributing an approximate 4% increase to the average UV intensity at the Earth's surface. Ozone depletion and the seasonal "ozone hole" have led to much larger changes in some locations, especially in the southern hemisphere.[22]
Tanning
Sunburns associated with indoor tanning can be severe.[25]
The World Health Organization, American Academy of Dermatology, and the Skin Cancer Foundation have recommended avoiding artificial UV sources such as tanning beds. Suntans are not recommended as a form of sun protection.[26][27][28]
Diagnosis

Differential diagnosis
The differential diagnosis of sunburn includes other skin pathology induced by UV radiation, including photoallergic reactions, phototoxic reactions to topical or systemic medications, and other dermatologic disorders that are aggravated by exposure to sunlight. Considerations for diagnosis include duration and intensity of UV exposure, topical or systemic medication use, history of dermatologic disease, and nutritional status.
- Phototoxic reactions: Non-immunological response to sunlight interacting with certain drugs and chemicals in the skin which resembles an exaggerated sunburn. Common medications that may cause a phototoxic reaction include
- Photoallergic reactions: Uncommon immunological response to sunlight interacting with certain drugs and chemicals in the skin. When in an excited state by UVR, these drugs and chemicals form free radicals that react to form functional antigens and induce a Type IV hypersensitivity reaction. These drugs include 6-methylcoumarin, aminobenzoic acid and esters, chlorpromazine, promethazine, diclofenac, sulfonamides, and sulfonylureas. Unlike phototoxic reactions which resemble exaggerated sunburns, photoallergic reactions can cause intense itching and can lead to thickening of the skin.[29]
- Phytophotodermatitis: UV radiation induces skin inflammation after contact with certain plants (including limes, celery, and meadow grass). Causes pain, redness, and blistering of the skin in the distribution of plant exposure.[14]
- Polymorphic light eruption: Recurrent abnormal reactions to UVR present in various ways, including pink-to-red bumps, blisters, plaques and urticaria.[14]
- Solar urticaria: A rare allergic reaction to the sun that occurs within minutes of exposure and fades within hours.[14]
- Other skin diseases exacerbated by sunlight: Several dermatologic conditions can increase in severity with exposure to UVR. These include systemic lupus erythematosus (SLE), dermatomyositis, acne, atopic dermatitis, and rosacea.[14]
Additionally, since sunburn is a type of
Prevention

The most effective way to prevent sunburn is to reduce the amount of UV radiation reaching the skin. The World Health Organization, American Academy of Dermatology, and Skin Cancer Foundation recommend the following measures to prevent excessive UV exposure and skin cancer:[33][34][35]
- Limiting sun exposure between the hours of 10 am and 4 pm, when UV rays are the strongest
- Seeking shade when UV rays are most intense
- Wearing sun-protective clothing, including a wide-brim hat, sunglasses, and tightly woven, loose-fitting clothing
- Using sunscreen
- Avoiding tanning beds and artificial UV exposure
UV intensity
The strength of sunlight is published in many locations as a
Sunscreen
Commercial preparations that block UV light are known as
Sunscreen is effective and thus recommended for preventing
Recommendations
Research has shown that the best sunscreen protection is achieved by application 15 to 30 minutes before exposure, followed by one reapplication 15 to 30 minutes after exposure begins. Further reapplication is necessary after activities such as swimming, sweating, and rubbing.[41] Recommendations are product dependent varying from 80 minutes in water to hours based on the indications and protection shown on the label. The American Academy of Dermatology recommends the following criteria in selecting a sunscreen:[42]
- Broad spectrum: protects against both UVA and UVB rays
- SPF 30 or higher
- Water resistant: sunscreens are classified as water resistant based on time, either 40 minutes, 80 minutes, or not water resistant
Eyes
The eyes are also sensitive to sun exposure at about the same UV wavelengths as skin;
The tender skin of the eyelids can also become sunburned and can be especially irritating.[citation needed]
Lips
The
Feet
The skin of the feet is often tender and protected, so sudden prolonged exposure to UV radiation can be particularly painful and damaging to the top of the foot. Protective measures include sunscreen, socks, or swimwear that covers the foot.
Diet
Dietary factors influence susceptibility to sunburn, recovery from sunburn, and risk of secondary complications. Several dietary
Protecting children
Babies and children are particularly susceptible to UV damage which increases their risk of both melanoma and non-melanoma skin cancers later in life. Children should not sunburn at any age, and protective measures can reduce their future risk of skin cancer.[50]
- Infants 0–6 months: Children under 6mo generally have skin too sensitive for sunscreen and protective measures should focus on avoiding excessive UV exposure by using window mesh covers, wide-brim hats, loose clothing that covers the skin, and reducing UV exposure between the hours of 10am and 4pm.
- Infants 6–12 months: Sunscreen can safely be used on infants this age. It is recommended to apply a broad-spectrum, water-resistant SPF 30+ sunscreen to exposed areas and avoid excessive UV exposure by using wide-brim hats and protective clothing.
- Toddlers and Preschool-aged children: Apply a broad-spectrum, water-resistant SPF 30+ sunscreen to exposed areas, use wide-brim hats and sunglasses, avoid peak UV intensity hours of 10 am - 4 pm and seek shade. Sun-protective clothing with an SPF rating can also provide additional protection.
Artificial UV exposure
The WHO recommends that artificial UV exposure, including tanning beds, should be avoided as no safe dose has been established.[51] Special protective clothing (for example, welding helmets/shields) should be worn when exposed to any artificial source of occupational UV. Such sources can produce UVC, an extremely carcinogenic wavelength of UV, which ordinarily is not present in normal sunlight, having been filtered out by the atmosphere.[citation needed]
Treatment
The primary measure of treatment is avoiding further exposure to the sun. The best treatment for most sunburns is time; most sunburns heal completely within a few weeks.
The American Academy of Dermatology recommends the following for the treatment of sunburn:[52]
- For pain relief, take cool baths or showers frequently.
- Use soothing moisturizers that contain aloe veraor soy.
- can help with pain.
- Keep hydrated and drink extra water.
- Do not pop blisterson a sunburn; let them heal on their own instead.
- Protect sunburned skin (see: Sun protective clothing and Sunscreen) with loose clothing when going outside to prevent further damage while not irritating the sunburn.
A home treatment that may help the discomfort is using cool and wet cloths on the sunburned areas.
See also
- Sun tanning
- Freckles
- Skin cancer
- Snow blindness
- Chapped lips
References
- ^ a b World Health Organization, International Agency for Research on Cancer "Do sunscreens prevent skin cancer" Archived 26 November 2006 at the Wayback Machine Press release No. 132, 5 June 2000
- ^ a b World Health Organization, International Agency for Research on Cancer "Solar and ultraviolet radiation" Archived 29 July 2013 at the Wayback Machine IARC Monographs on the Evaluation of Carcinogenic Risks to Humans, Volume 55, November 1997
- ^ a b Sunburn at eMedicine
- S2CID 205188894.
- PMID 22271688.
- ^ "How to treat sunburn | American Academy of Dermatology". www.aad.org. Archived from the original on 20 March 2018. Retrieved 29 March 2018.
- S2CID 8254557.
- ^ "Facts About Sunburn and Skin Cancer" Archived 2 June 2013 at the Wayback Machine, Skin Cancer Foundation
- PMID 18652979.
- from the original on 7 August 2020. Retrieved 13 December 2019.
- PMID 31723047.
- ^ Linden DJ (2015). Touch: The Science of Hand, Heart and Mind. Viking. Archived from the original on 15 October 2021. Retrieved 1 March 2015.
- PMID 21734176.
- ^ OCLC 813301093.
- ^ Wolff, K, ed. (2017). "PHOTOSENSITIVITY, PHOTO-INDUCED DISORDERS, AND DISORDERS BY IONIZING RADIATION". Fitzpatrick's Color Atlas and Synopsis of Clinical Dermatology (8th ed.). New York, NY: McGraw Hill. Archived from the original on 21 March 2018. Retrieved 20 March 2018.
- ^ a b "Sunburn – Topic Overview". Healthwise. 15 November 2013. Archived from the original on 30 September 2017. Retrieved 29 November 2014.
- from the original on 17 April 2021. Retrieved 23 March 2018.
- ^ "Avoiding Sun-Related Skin Damage". Fact-Sheets.com. 2004. Retrieved 3 January 2015.
- ^ "Tanning – Ultraviolet (UV) Radiation". Health Center for Devices and Radiological. United States Food and Drug Administration. Archived from the original on 23 May 2017. Retrieved 19 May 2017.
- ^ "Global Solar UV Index: A Practical Guide" (PDF). World Health Organization. 2002. Archived (PDF) from the original on 27 November 2014. Retrieved 2 January 2015.
Up to 80% of solar UV radiation can penetrate light cloud cover.
- EPA. 2012. Archivedfrom the original on 16 February 2015. Retrieved 2 January 2015.
Clear skies allow virtually 100% of UV to pass through, scattered clouds transmit 89%, broken clouds transmit 73%, and overcast skies transmit 31%.
- ^ "Twenty Questions and Answers About the Ozone Layer" (PDF). Scientific Assessment of Ozone Depletion: 2010. World Meteorological Organization. 2011. Archived (PDF) from the original on 1 April 2014. Retrieved 13 March 2015.
- ^ "Suntan". Healthwise. 27 March 2005. Retrieved 26 August 2006.
- ^ "The Surgeon General's Call to Action to Prevent Skin Cancer" (PDF). U.S. Department of Health and Human Services. 2014. p. 20. Archived (PDF) from the original on 26 November 2014. Retrieved 17 August 2016.
A UVB-induced tan provides minimal sun protection, equivalent to an SPF of about 3.
- PMID 25506731.
- ^ "Prevention - SkinCancer.org". skincancer.org. Archived from the original on 30 March 2018. Retrieved 30 March 2018.
- ^ "Dangers of indoor tanning | American Academy of Dermatology". www.aad.org. Archived from the original on 30 March 2018. Retrieved 30 March 2018.
- ^ "WHO | Artificial tanning devices: public health interventions to manage sunbeds". WHO. Archived from the original on 29 June 2017. Retrieved 30 March 2018.
- ^ OCLC 893557976.
- ^ "What Are the Types and Degrees of Burns?". Archived from the original on 7 June 2019. Retrieved 7 June 2019.
- ^ "Sunburn – Health Encyclopedia – University of Rochester Medical Center". Archived from the original on 8 June 2019. Retrieved 7 June 2019.
- ^ "Acute Radiation Syndrome | CDC". 23 October 2020. Archived from the original on 8 June 2019. Retrieved 7 June 2019.
- ^ a b "Sun protection". World Health Organization. Archived from the original on 22 March 2018. Retrieved 28 March 2018.
- ^ "Prevention Guidelines - SkinCancer.org". skincancer.org. Archived from the original on 29 March 2018. Retrieved 28 March 2018.
- ^ "Prevent skin cancer | American Academy of Dermatology". www.aad.org. Archived from the original on 14 May 2018. Retrieved 28 March 2018.
- S2CID 22599824.
- PMID 22123420.
- PMID 21392107.
- S2CID 40870536.
- S2CID 12276606.
- PMID 11712033.
- ^ "How to select a sunscreen | American Academy of Dermatology". www.aad.org. Archived from the original on 29 March 2018. Retrieved 28 March 2018.
- PMID 16395131.
- PMID 16714259.
- S2CID 40041207.
- PMID 9448204.
- S2CID 86776862.
- S2CID 22417600.
- PMID 23467449.
- ^ "Children - SkinCancer.org". skincancer.org. 13 September 2016. Archived from the original on 29 March 2018. Retrieved 28 March 2018.
- ^ "WHO | Artificial tanning devices: public health interventions to manage sunbeds". WHO. Archived from the original on 29 June 2017. Retrieved 28 March 2018.
- ^ "How to treat sunburn | American Academy of Dermatology". www.aad.org. Archived from the original on 20 March 2018. Retrieved 28 March 2018.
- ^ "Sunburn – Home Treatment". Healthwise. 15 November 2013. Archived from the original on 12 July 2012. Retrieved 29 November 2014.
- ^ ISBN 978-1-4443-0064-2. Archivedfrom the original on 14 January 2023. Retrieved 20 September 2020.
- ^ a b c d "How to treat sunburn". American Academy of Dermatology. Archived from the original on 20 March 2018. Retrieved 26 June 2016.
- ISBN 978-0-7817-6058-4. Archivedfrom the original on 14 January 2023. Retrieved 20 September 2020.
- PMID 17499928.
- PMID 29495390.
- PMID 19218914.
External links
- Sunburn at Curlie
