Burn
| Burn | |
|---|---|
|
Fourth degree: Bone and tendon loss tetanus toxoid[2] | |
| Frequency | 67 million (2015)[7] |
| Deaths | 176,000 (2015)[8] |
A burn is an
Burns that affect only the superficial skin layers are known as superficial or first-degree burns.
Burns are generally preventable.
In 2015, fire and heat resulted in 67 million injuries.
History

Cave paintings from more than 3,500 years ago document burns and their management.[13] The earliest Egyptian records on treating burns describes dressings prepared with milk from mothers of baby boys,[15] and the 1500 BCE Edwin Smith Papyrus describes treatments using honey and the salve of resin.[13] Many other treatments have been used over the ages, including the use of tea leaves by the Chinese documented to 600 BCE, pig fat and vinegar by Hippocrates documented to 400 BCE, and wine and myrrh by Celsus documented to the 1st century CE.[13] French barber-surgeon Ambroise Paré was the first to describe different degrees of burns in the 1500s.[16] Guillaume Dupuytren expanded these degrees into six different severities in 1832.[13][17]
The first hospital to treat burns opened in 1843 in London, England, and the development of modern burn care began in the late 1800s and early 1900s.[13][16] During World War I, Henry D. Dakin and Alexis Carrel developed standards for the cleaning and disinfecting of burns and wounds using sodium hypochlorite solutions, which significantly reduced mortality.[13] In the 1940s, the importance of early excision and skin grafting was acknowledged, and around the same time, fluid resuscitation and formulas to guide it were developed.[13] In the 1970s, researchers demonstrated the significance of the hypermetabolic state that follows large burns.[13]
The "Evans formula", described in 1952, was the first burn resuscitation formula based on body weight and surface area (BSA) damaged. The first 24 hours of treatment entails 1ml/kg/% BSA of crystalloids plus 1 ml/kg/% BSA colloids plus 2000ml glucose in water, and in the next 24 hours, crystalloids at 0.5 ml/kg/% BSA, colloids at 0.5 ml/kg/% BSA, and the same amount of glucose in water.[18][19]
Signs and symptoms
The characteristics of a burn depend upon its depth. Superficial burns cause pain lasting two or three days, followed by peeling of the skin over the next few days.
| Type[2] | Layers involved | Appearance | Texture | Sensation | Healing Time | Prognosis and Complications | Example |
|---|---|---|---|---|---|---|---|
| Superficial (first-degree) | Epidermis[10] | Red without blisters[2] | Dry | Painful[2] | 5–10 days[2][25] | Heals well.[2] | 
|
| Superficial partial thickness (second-degree) | Extends into superficial (papillary) dermis[2] | Redness with clear blister.[2] Blanches with pressure.[2] | Moist[2] | Very painful[2] | 2–3 weeks[2][20] | Local infection (cellulitis) but no scarring typically[20] | |
| Deep partial thickness (second-degree) | Extends into deep (reticular) dermis[2] | Yellow or white. Less blanching. May be blistering.[2] | Fairly dry[20] | Pressure and discomfort[20] | 3–8 weeks[2] | Scarring, contractures (may require excision and skin grafting)[20] | 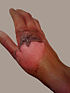
|
| Full thickness (third-degree) | Extends through entire dermis[2] | Stiff and white/brown.[2] No blanching.[20] | Leathery[2] | Painless[2] | Prolonged (months) and unfinished/incomplete[2] | Scarring, contractures, amputation (early excision recommended)[20] | 
|
| Fourth-degree | Extends through entire skin, and into underlying fat, muscle and bone[2] | Black; charred with eschar | Dry | Painless | Does not heal; Requires excision[2] | Amputation, significant functional impairment and, in some cases, death.[2] | 
|
Cause
Burns are caused by a variety of external sources classified as thermal (heat-related), chemical, electrical, and radiation.[26] In the United States, the most common causes of burns are: fire or flame (44%), scalds (33%), hot objects (9%), electricity (4%), and chemicals (3%).[27] Most (69%) burn injuries occur at home or at work (9%),[14] and most are accidental, with 2% due to assault by another, and 1–2% resulting from a suicide attempt.[24] These sources can cause inhalation injury to the airway and/or lungs, occurring in about 6%.[4]
Burn injuries occur more commonly among the poor.
Thermal
Graphs are unavailable due to technical issues. There is more info on Phabricator and on MediaWiki.org. |
In the United States, fire and hot liquids are the most common causes of burns.[4] Of house fires that result in death, smoking causes 25% and heating devices cause 22%.[5] Almost half of injuries are due to efforts to fight a fire.[5] Scalding is caused by hot liquids or gases and most commonly occurs from exposure to hot drinks, high temperature tap water in baths or showers, hot cooking oil, or steam.[30] Scald injuries are most common in children under the age of five[2] and, in the United States and Australia, this population makes up about two-thirds of all burns.[4] Contact with hot objects is the cause of about 20–30% of burns in children.[4] Generally, scalds are first- or second-degree burns, but third-degree burns may also result, especially with prolonged contact.[31] Fireworks are a common cause of burns during holiday seasons in many countries.[32] This is a particular risk for adolescent males.[33] In the United States, for non-fatal burn injuries to children, white males under the age of 6 comprise most cases.[34] Thermal burns from grabbing/touching and spilling/splashing were the most common type of burn and mechanism, while the bodily areas most impacted were hands and fingers followed by head/neck.[34]
Chemical
Chemical burns can be caused by over 25,000 substances,
Electrical
Electrical burns or injuries are classified as high voltage (greater than or equal to 1000
While electrical injuries primarily result in burns, they may also cause
Radiation
Non-accidental
In those hospitalized from scalds or fire burns, 3–10% are from assault.[44] Reasons include: child abuse, personal disputes, spousal abuse, elder abuse, and business disputes.[44] An immersion injury or immersion scald may indicate child abuse.[31] It is created when an extremity, or sometimes the buttocks are held under the surface of hot water.[31] It typically produces a sharp upper border and is often symmetrical,[31] known as "sock burns", "glove burns", or "zebra stripes" - where folds have prevented certain areas from burning.[45] Deliberate cigarette burns most often found on the face, or the back of the hands and feet.[45] Other high-risk signs of potential abuse include: circumferential burns, the absence of splash marks, a burn of uniform depth, and association with other signs of neglect or abuse.[46]
Pathophysiology

At temperatures greater than 44 °C (111 °F), proteins begin losing their three-dimensional shape and start breaking down.[49] This results in cell and tissue damage.[2] Many of the direct health effects of a burn are caused by failure of the skin to perform its normal functions, which include: protection from bacteria, skin sensation, body temperature regulation, and prevention of evaporation of the body's water. Disruption of these functions can lead to infection, loss of skin sensation, hypothermia, and hypovolemic shock via dehydration (i.e. water in the body evaporated away).[2] Disruption of cell membranes causes cells to lose potassium to the spaces outside the cell and to take up water and sodium.[2]
In large burns (over 30% of the total body surface area), there is a significant
Increased levels of
Diagnosis
Burns can be classified by depth, mechanism of injury, extent, and associated injuries. The most commonly used classification is based on the depth of injury. The depth of a burn is usually determined via examination, although a biopsy may also be used.[2] It may be difficult to accurately determine the depth of a burn on a single examination and repeated examinations over a few days may be necessary.[21] In those who have a headache or are dizzy and have a fire-related burn, carbon monoxide poisoning should be considered.[52] Cyanide poisoning should also be considered.[21]
Size

The size of a burn is measured as a percentage of total body surface area (TBSA) affected by partial thickness or full thickness burns.[2] First-degree burns that are only red in color and are not blistering are not included in this estimation.[2] Most burns (70%) involve less than 10% of the TBSA.[4]
There are a number of methods to determine the TBSA, including the Wallace rule of nines, Lund and Browder chart, and estimations based on a person's palm size.[10] The rule of nines is easy to remember but only accurate in people over 16 years of age.[10] More accurate estimates can be made using Lund and Browder charts, which take into account the different proportions of body parts in adults and children.[10] The size of a person's handprint (including the palm and fingers) is approximately 1% of their TBSA.[10]
Severity
| Minor | Moderate | Major |
|---|---|---|
| Adult <10% TBSA | Adult 10–20% TBSA | Adult >20% TBSA |
| Young or old < 5% TBSA | Young or old 5–10% TBSA | Young or old >10% TBSA |
| <2% full thickness burn | 2–5% full thickness burn | >5% full thickness burn |
| High voltage injury | High voltage burn | |
| Possible inhalation injury | Known inhalation injury | |
| Circumferential burn | Significant burn to face, joints, hands, or feet | |
| Other health problems | Associated injuries |
To determine the need for referral to a specialized burn unit, the American Burn Association devised a classification system. Under this system, burns can be classified as major, moderate, and minor. This is assessed based on a number of factors, including total body surface area affected, the involvement of specific anatomical zones, the age of the person, and associated injuries.[52] Minor burns can typically be managed at home, moderate burns are often managed in a hospital, and major burns are managed by a burn center.[52] Severe burn injury represents one of the most devastating forms of trauma.[53] Despite improvements in burn care, patients can be left to suffer for as many as three years post-injury.[54]
Prevention
Historically, about half of all burns were deemed preventable.[5] Burn prevention programs have significantly decreased rates of serious burns.[49] Preventive measures include: limiting hot water temperatures, smoke alarms, sprinkler systems, proper construction of buildings, and fire-resistant clothing.[5] Experts recommend setting water heaters below 48.8 °C (119.8 °F).[4] Other measures to prevent scalds include using a thermometer to measure bath water temperatures, and splash guards on stoves.[49] While the effect of the regulation of fireworks is unclear, there is tentative evidence of benefit[55] with recommendations including the limitation of the sale of fireworks to children.[4]
Management
Resuscitation begins with the assessment and stabilization of the person's airway, breathing and circulation.
Intravenous fluids
In those with poor
While
Wound care
Early cooling (within 30 minutes of the burn) reduces burn depth and pain, but care must be taken as over-cooling can result in hypothermia.[2][10] It should be performed with cool water 10–25 °C (50.0–77.0 °F) and not ice water as the latter can cause further injury.[10][49] Chemical burns may require extensive irrigation.[2] Cleaning with soap and water, removal of dead tissue, and application of dressings are important aspects of wound care. If intact blisters are present, it is not clear what should be done with them. Some tentative evidence supports leaving them intact. Second-degree burns should be re-evaluated after two days.[49]
In the management of first and second-degree burns, little quality evidence exists to determine which dressing type to use.[66] It is reasonable to manage first-degree burns without dressings.[49] While topical antibiotics are often recommended, there is little evidence to support their use.[67][68] Silver sulfadiazine (a type of antibiotic) is not recommended as it potentially prolongs healing time.[66][69] There is insufficient evidence to support the use of dressings containing silver[70] or negative-pressure wound therapy.[71] Silver sulfadiazine does not appear to differ from silver containing foam dressings with respect to healing.[72]
Medications
Burns can be very painful and a number of different options may be used for
Intravenous
Allogeneic cultured keratinocytes and dermal fibroblasts in murine collagen (Stratagraft) was approved for medical use in the United States in June 2021.[79]
Surgery
Wounds requiring surgical closure with skin grafts or flaps (typically anything more than a small full thickness burn) should be dealt with as early as possible.[80] Circumferential burns of the limbs or chest may need urgent surgical release of the skin, known as an escharotomy.[81] This is done to treat or prevent problems with distal circulation, or ventilation.[81] It is uncertain if it is useful for neck or digit burns.[81] Fasciotomies may be required for electrical burns.[81]
Skin grafts can involve temporary skin substitutes, derived from animal (human donor or pig) skin or synthesized. They are used to cover the wound as a dressing, preventing infection and fluid loss, but will eventually need to be removed. Alternatively, human skin can be treated to be left on permanently without rejection.[82]
There is no evidence that the use of copper sulphate to visualise phosphorus particles for removal can help with wound healing due to phosphorus burns. Meanwhile, absorption of copper sulphate into the blood circulation can be harmful.[83]
Alternative medicine
Honey has been used since ancient times to aid wound healing and may be beneficial in first- and second-degree burns.[84] There is moderate evidence that honey helps heal partial thickness burns.[85][86] The evidence for aloe vera is of poor quality.[87] While it might be beneficial in reducing pain,[25] and a review from 2007 found tentative evidence of improved healing times,[88] a subsequent review from 2012 did not find improved healing over silver sulfadiazine.[87] There were only three randomized controlled trials for the use of plants for burns, two for aloe vera and one for oatmeal.[89]
There is little evidence that vitamin E helps with keloids or scarring.[90] Butter is not recommended.[91] In low income countries, burns are treated up to one-third of the time with traditional medicine, which may include applications of eggs, mud, leaves or cow dung.[28] Surgical management is limited in some cases due to insufficient financial resources and availability.[28] There are a number of other methods that may be used in addition to medications to reduce procedural pain and anxiety including: virtual reality therapy, hypnosis, and behavioral approaches such as distraction techniques.[74]
Patient support
Burn patients require support and care – both physiological and psychological. Respiratory failure, sepsis, and multi-organ system failure are common in hospitalized burn patients. To prevent hypothermia and maintain normal body temperature, burn patients with over 20% of burn injuries should be kept in an environment with the temperature at or above 30 degree Celsius.
Metabolism in burn patients proceeds at a higher than normal speed due to the whole-body process and rapid fatty acid substrate cycles, which can be countered with an adequate supply of energy, nutrients, and antioxidants. Enteral feeding a day after resuscitation is required to reduce risk of infection, recovery time, non-infectious complications, hospital stay, long-term damage, and mortality. Controlling blood glucose levels can have an impact on liver function and survival.
Risk of thromboembolism is high and acute respiratory distress syndrome (ARDS) that does not resolve with maximal ventilator use is also a common complication. Scars are long-term after-effects of a burn injury. Psychological support is required to cope with the aftermath of a fire accident, while to prevent scars and long-term damage to the skin and other body structures consulting with burn specialists, preventing infections, consuming nutritious foods, early and aggressive rehabilitation, and using compressive clothing are recommended.
Prognosis
| TBSA | Mortality |
|---|---|
| 0–9% | 0.6% |
| 10–19% | 2.9% |
| 20–29% | 8.6% |
| 30–39% | 16% |
| 40–49% | 25% |
| 50–59% | 37% |
| 60–69% | 43% |
| 70–79% | 57% |
| 80–89% | 73% |
| 90–100% | 85% |
| Inhalation | 23% |
The prognosis is worse in those with larger burns, those who are older, and females.
Complications
A number of complications may occur, with
Anemia secondary to full thickness burns of greater than 10% TBSA is common.
Epidemiology

| no data < 50 50–100 100–150 150–200 200–250 250–300 | 300–350 350–400 400–450 450–500 500–600 > 600 |
In 2015 fire and heat resulted in 67 million injuries.
In the developed world, adult males have twice the mortality as females from burns. This is most probably due to their higher risk occupations and greater risk-taking activities. In many countries in the developing world, however, females have twice the risk of males. This is often related to accidents in the kitchen or domestic violence.[24] In children, deaths from burns occur at more than ten times the rate in the developing than the developed world.[24] Overall, in children it is one of the top fifteen leading causes of death.[5] From the 1980s to 2004, many countries have seen both a decrease in the rates of fatal burns and in burns generally.[24]
Developed countries
An estimated 500,000 burn injuries receive medical treatment yearly in the United States.[49] They resulted in about 3,300 deaths in 2008.[5] Most burns (70%) and deaths from burns occur in males.[2][14] The highest incidence of fire burns occurs in those 18–35 years old, while the highest incidence of scalds occurs in children less than five years old and adults over 65.[2] Electrical burns result in about 1,000 deaths per year.[102] Lightning results in the death of about 60 people a year.[23] In Europe, intentional burns occur most commonly in middle aged men.[44]
Developing countries
In India, about 700,000 to 800,000 people per year sustain significant burns, though very few are looked after in specialist burn units.[103] The highest rates occur in women 16–35 years of age.[103] Part of this high rate is related to unsafe kitchens and loose-fitting clothing typical to India.[103] It is estimated that one-third of all burns in India are due to clothing catching fire from open flames.[104] Intentional burns are also a common cause and occur at high rates in young women, secondary to domestic violence and self-harm.[24][44]
See also
References
- ^ "Burns - British Association of Plastic Reconstructive and Aesthetic Surgeons". BAPRAS.
- ^ ISBN 978-0-07-148480-0.
- ^ PMID 17606093.
- ^ ISBN 978-1-4377-2786-9.
- ^ ISBN 978-1-4377-2786-9.
- ^ a b c d e f g h i "Burns". World Health Organization. September 2016. Archived from the original on 21 July 2017. Retrieved 1 August 2017.
- ^ PMID 27733282.
- ^ PMID 27733281.
- ^ a b "Burns Fact sheet N°365". WHO. April 2014. Archived from the original on 10 November 2015. Retrieved 3 March 2016.
- ^ a b c d e f g h i j k l m n o p q Granger J (January 2009). "An Evidence-Based Approach to Pediatric Burns". Pediatric Emergency Medicine Practice. 6 (1). Archived from the original on 17 October 2013.
- ISBN 978-1-4557-2826-8. Archivedfrom the original on 21 December 2016.
- ^ PMID 26635210.
- ^ ]
- ^ a b c "Burn Incidence and Treatment in the United States: 2012 Fact Sheet". American Burn Association. 2012. Archived from the original on 21 February 2013. Retrieved 20 April 2013.
- PMID 23888738.
- ^ ISBN 978-1-4557-1055-3. Archivedfrom the original on 2 May 2016.
- ISBN 978-90-5487-572-7. Archivedfrom the original on 16 May 2016.
- PMID 5033490.
- PMID 30480960. Retrieved 31 October 2023.
- ^ ISBN 978-1-4377-2786-9.
- ^ ISBN 978-0-07-154769-7.
- ^ S2CID 3679902.
- ^ ISBN 978-0-323-05472-0.
- ^ PMID 21802856.
- ^ PMID 22230304.
- ISBN 978-0-7817-6521-3. Archivedfrom the original on 12 May 2016.
- ^ National Burn Repository Pg. i
- ^ PMID 16777340.
- ^ "Fire death rates". Our World in Data. Retrieved 17 November 2019.
- ISBN 978-0-19-922773-0. Archivedfrom the original on 25 April 2016.
- ^ PMID 18538478.
- ISBN 978-92-4-156357-4. Archivedfrom the original on 24 April 2016.
- ^ World Health Organization. "World report on child injury prevention" (PDF). Archived (PDF) from the original on 31 May 2013.
- ^ S2CID 207816299.
- PMID 22037150.
- ^ PMID 18605366.
- PMID 29244970.
- PMID 15777170.
- ISBN 978-1-59745-404-9. Archivedfrom the original on 20 May 2016.
- PMID 23393776.
- PMID 21357345.
- ^ ISBN 978-0-323-05472-0.
- ^ ISBN 978-0-683-08027-8. Archivedfrom the original on 5 May 2016.
- ^ PMID 22325849.
- ^ PMID 21738970.
- ^ ISBN 978-1-4377-2786-9.
- PMID 15091143.
- ISBN 978-92-4-156357-4. Archivedfrom the original on 17 June 2016.
- ^ ISBN 978-0-323-05472-0.
- ^ PMID 23121414.
- ISBN 978-1-60547-781-7. Archivedfrom the original on 1 May 2016.
- ^ ISBN 978-0-521-74776-9. Archivedfrom the original on 20 May 2016.
- ^ Barayan D, Vinaik R, Auger C, Knuth CM, Abdullahi A, Jeschke MG. Inhibition of Lipolysis With Acipimox Attenuates Postburn White Adipose Tissue Browning and Hepatic Fat Infiltration. Shock. 2020;53(2):137-145. doi:10.1097/SHK.0000000000001439, 10.1097/SHK.0000000000001439
- ^ Jeschke MG, Gauglitz GG, Kulp GA, Finnerty CC, Williams FN, Kraft R, Suman OE, Mlcak RP, Herndon DN: Long-term persistence of the pathophysi-ologic response to severe burn injury.PLoS One6:E21245, 2011.
- ISBN 978-3-7091-0348-7. Archivedfrom the original on 17 May 2016.
- ISBN 978-0-7817-7447-5. Archivedfrom the original on 20 May 2016.
- PMID 23582468.
- PMID 23397872.
- ^ S2CID 40561988.
- PMID 15242917.
- ISBN 978-3-7091-0348-7. Archivedfrom the original on 19 May 2016.
- S2CID 5525939.
- PMID 30073665.
- PMID 27613476.
- PMID 21367529.
- ^ PMID 23543513.
- ^ PMID 20156911.
- PMID 32725896.
- PMID 23740764.
- PMID 20238345.
- PMID 25500895.
- S2CID 121615225.
- PMID 22244605.
- ^ ISBN 978-1-4377-2786-9.
- PMID 25321859.
- ISBN 978-1-4377-2786-9.
- PMID 25222766.
- PMID 24093225.
- ^ "FDA Approves StrataGraft for the Treatment of Adults with Thermal Burns". U.S. Food and Drug Administration (FDA) (Press release). 15 June 2021. Retrieved 20 April 2023.
- ISBN 978-3-7091-0348-7. Archivedfrom the original on 10 May 2016.
- ^ PMID 19692906.
- ^ "General data about burns". Burn Centre Care. Archived from the original on 18 October 2018. Retrieved 24 June 2019.
- PMID 24896368.
- PMID 19648986.
- PMID 28700086.
- PMID 25742878.
- ^ PMID 22336851.[permanent dead link]
- PMID 17499928.
- S2CID 23859340.
- ^ PMID 19621835.
- ISBN 978-0-8160-7509-6. Archivedfrom the original on 18 May 2016.
- ^ "Medically Sound: Treating and Caring for Burn, Electricity, and Radiation Victims". Medically Sound. 26 September 2020. Retrieved 1 November 2020.
- ^ a b National Burn Repository, Pg. 10
- ISBN 978-0-7817-5386-9. Archivedfrom the original on 22 May 2016.
- ^ ISBN 978-1-60918-175-8. Archivedfrom the original on 30 April 2016.
- ^ "ACI Statewide Burn Injury Service. Physiotherapy and Occupational Therapy Clinical Practice Guidelines" (PDF). 5 March 2018. Archived from the original (PDF) on 19 April 2017. Retrieved 18 February 2023.
- PMID 24888226.
- S2CID 25937084.
- ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 11 November 2009. Retrieved 11 November 2009.
- PMID 25530442.)
{{cite journal}}:|author=has generic name (help)CS1 maint: numeric names: authors list (link - S2CID 1541253.
- PMID 16218900.
- ^ PMID 15321905.
- ISBN 978-81-7179-965-7. Archivedfrom the original on 27 April 2016.
General and cited references
- National Burn Repository 2012 Report (PDF). Dataset Version 8.0. Chicago: American Burn Association. 2012. Archived from the original (PDF) on 3 March 2016. Retrieved 20 April 2013.
External links
- WHO fact sheet on burns
- Parkland Formula
- "Burns". MedlinePlus. U.S. National Library of Medicine.

