Ulcer (dermatology)
| Skin ulcer | |
|---|---|
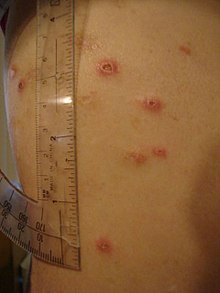 | |
| Erythema nodosum – Skin ulcers that occur in some patients with inflammatory bowel disease | |
| Specialty | Dermatology, surgery |
An ulcer is a sore on the
They can also be caused due to a lack of mobility, which causes prolonged pressure on the tissues. This stress in the blood circulation is transformed to a skin ulcer, commonly known as
forms.Signs and symptoms
Skin ulcers appear as open craters, often round, with layers of skin that have eroded. The skin around the ulcer may be red, swollen, and tender. Patients may feel pain on the skin around the ulcer, and fluid may ooze from the ulcer. In some cases, ulcers can
Ulcers develop in stages. In stage 1 the skin is red with soft underlying
Chronic ulcers may be painful. Most patients complain of constant pain at night and during the day. Chronic ulcer symptoms usually include increasing pain, friable granulation tissue, foul odour, and wound breakdown instead of healing.[2] Symptoms tend to worsen once the wound has become infected.
Although skin ulcers do not seem of great concern at a first glance, they are worrying conditions especially in people with
Ulcers may also appear on the cheeks, soft palate, the tongue, and on the inside of the lower lip. These ulcers usually last from 7 to 14 days and can be painful.[3]
Discharges
Different types of discharges from ulcer are:[4]
- Serous, usually seen in healing ulcer
- Purulent, seen in infected ulcer. Yellow creamy discharge is observed in staphylococcal infection; bloody opalescent discharge in streptococcal infection, while greenish discharge is seen in the case of Pseudomonas infection.
- Bloody (sanguineous), usually seen in malignant ulcers and in healing ulcers with healthy granulation tissue
- Seropurulent
- Serosanguinous
- Serous with sulphur granules, seen in actinomycosis
- Yellowish, as seen in tuberculous ulcer
Causes
The wounds from which ulcers arise can be caused by a wide variety of factors, but the main cause is impaired blood circulation. Especially, chronic wounds and ulcers are caused by poor circulation, either through cardiovascular issues or external pressure from a bed or a wheelchair.[2] A very common and dangerous type of skin ulcer is caused by what are called pressure-sensitive sores, more commonly called bed sores, which are frequent in people who are bedridden or who use wheelchairs for long periods.[citation needed]
Other causes producing skin ulcers include
Rare causes of skin ulcers include pyoderma gangraenosum, lesions caused by Crohn's disease or ulcerative colitis, granulomatosis with polyangiitis, morbus Behçet and infections that are usually seen in those who are immunocompromised, for example ecthyma gangraenosum. It is important to consider such causes if the skin ulcerations don't show improvement with antibiotic treatments and when other systemic symptoms are present. It is advised not to use surgical procedures on ulcerations caused by Behçet or pyoderma gangraenosum since those diseases usually exhibit pathergy.
Diagnosis
Grading
Wagner's grading of ulcer follows:[4]
| Grade | Description |
|---|---|
| 0 | Pre-ulcerative lesion or healed ulcer |
| 1 | Superficial ulcer |
| 2 | Ulcer deeper to subcutaneous tissue exposing soft tissue or bone |
| 3 | Abscess formation underneath, osteomyelitis |
| 4 | Gangrene of part of tissues, limb or foot |
| 5 | Gangrene of entire one area or foot |
Management
Investigations
Some of the investigations done for ulcer are:[4]: 19
- Study of discharging fluid: sensitivity
- Edge biopsy: Edge contains multiplying cells
- Radiographof affected area to look for periostitis or osteomyelitis
- Fine needle aspiration cytology(FNAC) of lymph node
- tuberculous ulcer
Treatment
Skin ulcers may take a very long time to heal. Treatment is typically to avoid the ulcer getting infected, remove any excess discharge, maintain a moist wound environment, control the edema, and ease pain caused by nerve and tissue damage.
Commonly, as a part of the treatment, patients are advised to change their lifestyle if possible and to change their diet. Improving the circulation is important in treating skin ulcers, and patients are consequently usually recommended to exercise, stop smoking, and lose weight.
In recent years, advances have been made in accelerating healing of
Leg ulcers can be prevented by using compression stockings to prevent blood pooling and back flow. It is likely that a person who has had a skin ulcer will have it again; use of compression stockings every day for at least five years after the skin ulcer has healed may help to prevent recurrence.
There is limited evidence that negative-pressure wound therapy may be effective in reducing the time to healing of leg ulcers.[7]
Specific types
- distaldigits
- Cortisol ulcer: caused by long term application of cortisol (steroid) topical creams to certain skin diseases.[8]
- complication of diabetes mellitus, and probably the major component of the diabetic foot.
- venous valves, usually of the legs
See also
- List of cutaneous conditions
- Skin disease
- Skin lesion
References
- ISBN 0-7216-0187-1.
- ^ a b "Wound Care & Skin Ulcers: Symptoms". Canadian Skin Patient Alliance. Archived from the original on 2010-06-19. Retrieved 2010-06-16.
- ^ "Ulcers Pictures and Descriptions". ulcerspictures.com. Retrieved 2010-06-16.
- ^ ISBN 9789350259443.
- ^ Goodman S (30 April 2013). "What Causes Skin Ulcers?". Embarrassing Issues. Retrieved 2010-06-16.
- ^ "Wound Care & Skin Ulcers: Treatments". Canadian Skin Patient Alliance. Archived from the original on 2010-01-27. Retrieved 2010-06-16.
- PMID 26171910.
- ISBN 9789350259443.
