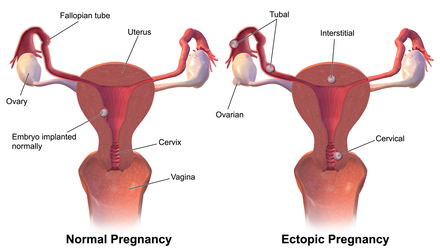
Ectopic pregnancy
| Ectopic pregnancy | |
|---|---|
| Other names | EP, eccyesis, extrauterine pregnancy, EUP, tubal pregnancy (when in fallopian tube) |
| Treatment | methotrexate, surgery[2] |
| Prognosis | Mortality 0.2% (developed world), 2% (developing world)[4] |
| Frequency | ~1.5% of pregnancies (developed world)[5] |
Ectopic pregnancy is a complication of pregnancy in which the embryo attaches outside the uterus.[5] Signs and symptoms classically include abdominal pain and vaginal bleeding, but fewer than 50 percent of affected women have both of these symptoms.[1] The pain may be described as sharp, dull, or crampy.[1] Pain may also spread to the shoulder if bleeding into the abdomen has occurred.[1] Severe bleeding may result in a fast heart rate, fainting, or shock.[5][1] With very rare exceptions, the fetus is unable to survive.[6]
Overall, ectopic pregnancies annually affect less than 2% of pregnancies worldwide.[5] Risk factors for ectopic pregnancy include
Prevention is by decreasing risk factors such as chlamydia infections through screening and treatment.
The rate of ectopic pregnancy is about 11 to 20 per 1,000 live births in developed countries, though it may be as high as 4% among those using assisted reproductive technology.[5] It is the most common cause of death among women during the first trimester at approximately 6-13% of the total.[2] In the developed world outcomes have improved while in the developing world they often remain poor.[7] The risk of death among those in the developed world is between 0.1 and 0.3 percent while in the developing world it is between one and three percent.[4] The first known description of an ectopic pregnancy is by Al-Zahrawi in the 11th century.[7] The word "ectopic" means "out of place".[8]
Signs and symptoms
Up to 10% of those with ectopic pregnancy have no symptoms, and one-third have no
Signs and symptoms of ectopic pregnancy include increased hCG, vaginal bleeding (in varying amounts), sudden lower abdominal pain,
Rupture of an ectopic pregnancy can lead to symptoms such as
Complications
The most common complication is rupture with internal bleeding which may lead to hypovolemic shock. Damage to the fallopian tubes can lead to difficulty becoming pregnant in the future. The woman's other fallopian tube may function sufficiently for pregnancy. After the removal of one damaged fallopian tube, pregnancy remains possible in the future. If both are removed, in-vitro fertilization remains an option for women hoping to become pregnant.[10][11][12]
Causes
There are a number of risk factors for ectopic pregnancies. However, in as many as one-third[13] to one-half[14] no risk factors can be identified. Risk factors include: pelvic inflammatory disease, infertility, use of an intrauterine device (IUD), previous exposure to diethylstilbestrol (DES), tubal surgery, intrauterine surgery (e.g. D&C), smoking, previous ectopic pregnancy, endometriosis, and tubal ligation.[15][16] A previous induced abortion does not appear to increase the risk.[17] The IUD does not increase the risk of ectopic pregnancy, but with an IUD if pregnancy occurs it is more likely to be ectopic than intrauterine.[18] The risk of ectopic pregnancy after chlamydia infection is low.[19] The exact mechanism through which chlamydia increases the risk of ectopic pregnancy is uncertain, though some research suggests that the infection can affect the structure of fallopian tubes.[20]
| Relative risk factors | |
|---|---|
| High | Tubal sterilization, IUD, prior ectopic, PID (pelvic inflammatory disease), endometriosis, SIN (salpingitis isthmica nodosa) |
| Moderate | Smoking, having more than 1 partner, infertility, chlamydia |
| Low | Douching, age greater than 35, age less than 18, GIFT (gamete intrafallopian transfer) |
Tube damage

Tubal pregnancy is when the egg is implanted in the fallopian tubes. Hair-like cilia located on the internal surface of the fallopian tubes carry the fertilized egg to the uterus. Fallopian cilia are sometimes seen in reduced numbers subsequent to an ectopic pregnancy, leading to a hypothesis that cilia damage in the fallopian tubes is likely to lead to an ectopic pregnancy.[23] Women who smoke have a higher chance of an ectopic pregnancy in the fallopian tubes. Smoking leads to risk factors of damaging and destroying cilia.[23] As cilia degenerate, the amount of time it takes for the fertilized egg to reach the uterus will increase. The fertilized egg, if it does not reach the uterus in time, will hatch from the non-adhesive zona pellucida and implant itself inside the fallopian tube, thus causing the ectopic pregnancy.
Women with pelvic inflammatory disease (PID) have a high occurrence of ectopic pregnancy.
Tubal ligation can predispose to ectopic pregnancy. Reversal of tubal sterilization (tubal reversal) carries a risk for ectopic pregnancy. This is higher if more destructive methods of tubal ligation (tubal cautery, partial removal of the tubes) have been used than less destructive methods (tubal clipping). A history of a tubal pregnancy increases the risk of future occurrences to about 10%.[25] This risk is not reduced by removing the affected tube, even if the other tube appears normal. The best method for diagnosing this is to do an early ultrasound.
Endometriosis
Endometriosis is a disease in which cells similar to those of the endometrium, the tissue covering the inside of the uterus, grow outside the uterus. An embryo attaching to such lesions leads to an ectopic pregnancy. Results of a 30 year study of reproductive and pregnancy outcomes, involving 14,000+ women of child-bearing age, were presented at the 2015 European Society of Human Reproduction and Embryology (ESHRE) annual congress.[22] 39% of the study group had surgically confirmed endometriosis. Compared to their peers, the endometriosis subgroup had a 76% higher risk for miscarriage and a 270% higher risk for ectopic pregnancy. The higher endometriosis risks were attributed to increased pelvic inflammation and structural and functional changes in the uterus' lining.
Other
Although some investigations have shown that patients may be at higher risk for ectopic pregnancy with advancing age, it is believed that age is a variable which could act as a surrogate for other risk factors. Vaginal douching is thought by some to increase ectopic pregnancies.
Diagnosis
An ectopic pregnancy should be considered as the cause of abdominal pain or vaginal bleeding in everyone who has a positive pregnancy test.[1] The primary goal of diagnostic procedures in possible ectopic pregnancy is to triage according to risk rather than establishing pregnancy location.[5]
Transvaginal ultrasonography
An ultrasound showing a gestational sac with fetal heart in the fallopian tube has a very high specificity of ectopic pregnancy. It involves a long, thin transducer, covered with the conducting gel and a plastic/latex sheath and inserted into the vagina.[33] Transvaginal ultrasonography has a sensitivity of at least 90% for ectopic pregnancy.[5] The diagnostic ultrasonographic finding in ectopic pregnancy is an adnexal mass that moves separately from the ovary. In around 60% of cases, it is an inhomogeneous or a noncystic adnexal mass sometimes known as the "blob sign". It is generally spherical, but a more tubular appearance may be seen in case of hematosalpinx. This sign has been estimated to have a sensitivity of 84% and specificity of 99% in diagnosing ectopic pregnancy.[5] In the study estimating these values, the blob sign had a positive predictive value of 96% and a negative predictive value of 95%.[5] The visualization of an empty extrauterine gestational sac is sometimes known as the "bagel sign", and is present in around 20% of cases.[5] In another 20% of cases, there is visualization of a gestational sac containing a yolk sac or an embryo.[5] Ectopic pregnancies where there is visualization of cardiac activity are sometimes termed "viable ectopic".[5]
-
Transvaginal ultrasonographyof an ectopic pregnancy, showing the field of view in the following image
-
A "blob sign", which consists of the ectopic pregnancy. The ovary is distinguished from it by having follicles, whereof one is visible in the field. This patient had anintrauterine device (IUD) with progestogen, whose cross-section is visible in the field, leaving an ultrasound shadow distally to it.
-
Ultrasound image showing an ectopic pregnancy where a gestational sac and fetus has been formed

The combination of a positive pregnancy test and the presence of what appears to be a normal intrauterine pregnancy does not exclude an ectopic pregnancy, since there may be either a heterotopic pregnancy or a "pseudosac", which is a collection of within the endometrial cavity that may be seen in up to 20% of women.[5]
A small amount of
Currently, Doppler ultrasonography is not considered to significantly contribute to the diagnosis of ectopic pregnancy.[5]
A common misdiagnosis is of a normal intrauterine pregnancy is where the pregnancy is implanted laterally in an arcuate uterus, potentially being misdiagnosed as an interstitial pregnancy.[5]
Ultrasonography and β-hCG
Where no intrauterine pregnancy (IUP) is seen on ultrasound, measuring β-human chorionic gonadotropin (β-hCG) levels may aid in the diagnosis. The rationale is that a low β-hCG level may indicate that the pregnancy is intrauterine but yet too small to be visible on ultrasonography. While some physicians consider that the threshold where an intrauterine pregnancy should be visible on transvaginal ultrasound is around 1500 mIU/mL of β-hCG, a review in the JAMA Rational Clinical Examination Series showed that there is no single threshold for the β-human chorionic gonadotropin that confirms an ectopic pregnancy. Instead, the best test in a pregnant woman is a high resolution transvaginal ultrasound.[1] The presence of an adnexal mass in the absence of an intrauterine pregnancy on transvaginal sonography increases the likelihood of an ectopic pregnancy 100-fold (LR+ 111). When there are no adnexal abnormalities on transvaginal sonography, the likelihood of an ectopic pregnancy decreases (LR- 0.12). An empty uterus with levels higher than 1500 mIU/mL may be evidence of an ectopic pregnancy, but may also be consistent with an intrauterine pregnancy which is simply too small to be seen on ultrasound. If the diagnosis is uncertain, it may be necessary to wait a few days and repeat the blood work. This can be done by measuring the β-hCG level approximately 48 hours later and repeating the ultrasound. The serum hCG ratios and logistic regression models appear to be better than absolute single serum hCG level.[35] If the β-hCG falls on repeat examination, this strongly suggests a spontaneous abortion or rupture. The fall in serum hCG over 48 hours may be measured as the hCG ratio, which is calculated as:[5]
An hCG ratio of 0.87, that is, a decrease in hCG of 13% over 48 hours, has a sensitivity of 93% and specificity of 97% for predicting a failing pregnancy of unknown location (PUL).[5] The majority of cases of ectopic pregnancy will have serial serum hCG levels that increase more slowly than would be expected with an IUP (that is, a suboptimal rise), or decrease more slowly than would be expected with a failing PUL. However, up to 20% of cases of ectopic pregnancy have serum hCG doubling times similar to that of an IUP, and around 10% of EP cases have hCG patterns similar to a failing PUL.[5]
Other methods
Direct examination
A laparoscopy or laparotomy can also be performed to visually confirm an ectopic pregnancy. This is generally reserved for women presenting with signs of an acute abdomen and hypovolemic shock.[5] Often if a tubal abortion or tubal rupture has occurred, it is difficult to find the pregnancy tissue. A laparoscopy in very early ectopic pregnancy rarely shows a normal-looking fallopian tube.
Culdocentesis
Culdocentesis, in which fluid is retrieved from the space separating the vagina and rectum, is a less commonly performed test that may be used to look for internal bleeding. In this test, a needle is inserted into the space at the very top of the vagina, behind the uterus and in front of the rectum. Any blood or fluid found may have been derived from a ruptured ectopic pregnancy.[citation needed]
Progesterone levels
Mathematical models
There are various mathematical models, such as logistic regression models and Bayesian networks, for the prediction of PUL outcome based on multiple parameters.[5] Mathematical models also aim to identify PULs that are low risk, that is, failing PULs and IUPs.[5]
Dilation and curettage
Dilation and curettage (D&C) is sometimes used to diagnose pregnancy location with the aim of differentiating between an EP and a non-viable IUP in situations where a viable IUP can be ruled out. Specific indications for this procedure include either of the following:[5]
- No visible IUP on transvaginal ultrasonography with a serum hCG of more than 2000 mIU/mL.
- An abnormal rise in hCG level. A rise of 35% over 48 hours is proposed as the minimal rise consistent with a viable intrauterine pregnancy.
- An abnormal fall in hCG level, such as defined as one of less than 20% in two days.
Classification
Tubal pregnancy
The vast majority of ectopic pregnancies implant in the fallopian tube. Pregnancies can grow in the fimbrial end (5% of all ectopic pregnancies), the ampullary section (80%), the isthmus (12%), and the cornual and interstitial part of the tube (2%).[25] Mortality of a tubal pregnancy at the isthmus or within the uterus (interstitial pregnancy) is higher as there is increased vascularity that may result more likely in sudden major internal bleeding. A review published in 2010 supports the hypothesis that tubal ectopic pregnancy is caused by a combination of retention of the embryo within the fallopian tube due to impaired embryo-tubal transport and alterations in the tubal environment allowing early implantation to occur.[36]
Nontubal ectopic pregnancy
Two percent of ectopic pregnancies occur in the ovary, cervix, or are intra-abdominal. Transvaginal ultrasound examination is usually able to detect a cervical pregnancy. An ovarian pregnancy is differentiated from a tubal pregnancy by the Spiegelberg criteria.[37]
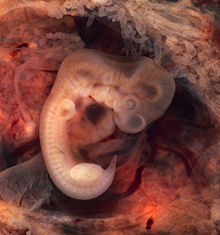
While a fetus of ectopic pregnancy is typically not viable, very rarely, a live baby has been delivered from an abdominal pregnancy. In such a situation the placenta sits on the intra-abdominal organs or the peritoneum and has found sufficient blood supply. This is generally bowel or mesentery, but other sites, such as the renal (kidney), liver or hepatic (liver) artery or even aorta have been described. Support to near viability has occasionally been described, but even in Third World countries, the diagnosis is most commonly made at 16 to 20 weeks' gestation. Such a fetus would have to be delivered by laparotomy. Maternal morbidity and mortality from extrauterine pregnancy are high as attempts to remove the placenta from the organs to which it is attached usually lead to uncontrollable bleeding from the attachment site. If the organ to which the placenta is attached is removable, such as a section of bowel, then the placenta should be removed together with that organ. This is such a rare occurrence that true data is unavailable and reliance must be made on anecdotal reports.[38][39][40] However, the vast majority of abdominal pregnancies require intervention well before fetal viability because of the risk of bleeding.
With the increase in Cesarean sections performed worldwide,[41][42] Cesarean section ectopic pregnancies (CSP) are rare, but becoming more common. The incidence of CSP is not well known, however there have been estimates based on different populations of 1:1800–1:2216.[43][44] CSP are characterized by abnormal implantation into the scar from a previous cesarean section,[45] and allowed to continue can cause serious complications such as uterine rupture and hemorrhage.[44] Patients with CSP generally present without symptoms, however symptoms can include vaginal bleeding that may or may not be associated with pain.[46][47] The diagnosis of CSP is made by ultrasound and four characteristics are noted: (1) Empty uterine cavity with bright hyperechoic endometrial stripe (2) Empty cervical canal (3) Intrauterine mass in the anterior part of the uterine isthmus, and (4) Absence of the anterior uterine muscle layer, and/or absence or thinning between the bladder and gestational sac, measuring less than 5 mm.[45][48][49] Given the rarity of the diagnosis, treatment options tend to be described in case reports and series, ranging from medical with methotrexate or KCl[50] to surgical with dilation and curettage,[51] uterine wedge resection,[citation needed] or hysterectomy.[47] A double-balloon catheter technique has also been described,[52] allowing for uterine preservation. Recurrence risk for CSP is unknown, and early ultrasound in the next pregnancy is recommended.[45]
Heterotopic pregnancy
In rare cases of ectopic pregnancy, there may be two fertilized eggs, one outside the uterus and the other inside. This is called a heterotopic pregnancy.[1] Often the intrauterine pregnancy is discovered later than the ectopic, mainly because of the painful emergency nature of ectopic pregnancies. Since ectopic pregnancies are normally discovered and removed very early in the pregnancy, an ultrasound may not find the additional pregnancy inside the uterus. When hCG levels continue to rise after the removal of the ectopic pregnancy, there is the chance that a pregnancy inside the uterus is still viable. This is normally discovered through an ultrasound.
Although rare, heterotopic pregnancies are becoming more common, likely due to increased use of IVF. The survival rate of the uterine fetus of a heterotopic pregnancy is around 70%.[53]
Rudimentary horn pregnancy
A
Persistent ectopic pregnancy
A persistent ectopic pregnancy refers to the continuation of trophoblastic growth after a surgical intervention to remove an ectopic pregnancy. After a conservative procedure that attempts to preserve the affected fallopian tube such as a
Pregnancy of unknown location
Pregnancy of unknown location (PUL) is the term used for a pregnancy where there is a positive pregnancy test but no pregnancy has been visualized using transvaginal ultrasonography.[5] Specialized early pregnancy departments have estimated that between 8% and 10% of women attending for an ultrasound assessment in early pregnancy will be classified as having a PUL.[5] The true nature of the pregnancy can be an ongoing viable intrauterine pregnancy, a failed pregnancy, an ectopic pregnancy or rarely a persisting PUL.[5]
Because of frequent ambiguity on ultrasonography examinations, the following classification is proposed:[5]
| Condition | Criteria |
|---|---|
| Definite ectopic pregnancy | Extrauterine gestational sac with yolk sac or embryo (with or without cardiac activity). |
| Pregnancy of unknown location – probable ectopic pregnancy | Inhomogeneous adnexal mass or extrauterine sac-like structure. |
| "True" pregnancy of unknown location | No signs of intrauterine nor extrauterine pregnancy on transvaginal ultrasonography. |
| Pregnancy of unknown location – probable intrauterine pregnancy | Intrauterine gestational sac-like structure. |
| Definite intrauterine pregnancy | Intrauterine gestational sac with yolk sac or embryo (with or without cardiac activity). |
In women with a pregnancy of unknown location, between 6% and 20% have an ectopic pregnancy.[5] In cases of pregnancy of unknown location and a history of heavy bleeding, it has been estimated that approximately 6% have an underlying ectopic pregnancy.[5] Between 30% and 47% of women with pregnancy of unknown location are ultimately diagnosed with an ongoing intrauterine pregnancy, whereof the majority (50–70%) will be found to have failing pregnancies where the location is never confirmed.[5]
Persisting PUL is where the hCG level does not spontaneously decline and no intrauterine or ectopic pregnancy is identified on follow-up transvaginal ultrasonography.
Differential diagnosis
Other conditions that cause similar symptoms include: miscarriage, ovarian torsion, and acute appendicitis, ruptured ovarian cyst, kidney stone, and pelvic inflammatory disease, among others.[1]
Treatment
Expectant management
Most women with a PUL are followed up with serum hCG measurements and repeat TVS examinations until a final diagnosis is confirmed.[5] Low-risk cases of PUL that appear to be failing pregnancies may be followed up with a urinary pregnancy test after two weeks and get subsequent telephone advice.[5] Low-risk cases of PUL that are likely intrauterine pregnancies may have another TVS in two weeks to access viability.[5] High-risk cases of PUL require further assessment, either with a TVS within 48 h or additional hCG measurement.[5]
Medical
Early treatment of an ectopic pregnancy with methotrexate is a viable alternative to surgical treatment[56] which was developed in the 1980s.[57] If administered early in the pregnancy, methotrexate terminates the growth of the developing embryo; the developing embryo may then be either resorbed by the woman's body or pass with a menstrual period. Contraindications include liver, kidney, or blood disease, as well as an ectopic embryonic mass > 3.5 cm.
Also, it may lead to the inadvertent termination of an undetected intrauterine pregnancy, or severe abnormality in any surviving pregnancy.[5] Therefore, it is recommended that methotrexate should only be administered when hCG has been serially monitored with a rise less than 35% over 48 hours, which practically excludes a viable intrauterine pregnancy.[5]
For nontubal ectopic pregnancy, evidence from randomised clinical trials in women with CSP is uncertain regarding treatment success, complications and side effects of methotrexate compared with surgery (uterine arterial embolization or uterine arterial chemoembolization).[58]
The United States uses a multi dose protocol of methotrexate (MTX) which involves four doses of intramuscular along with an intramuscular injection of folinic acid to protect cells from the effects of the drugs and to reduce side effects. In France, the single dose protocol is followed, but a single dose has a greater chance of failure.[59]
Surgery
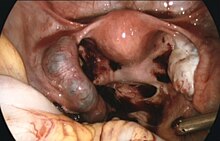

If bleeding has already occurred, surgical intervention may be necessary. However, whether to pursue surgical intervention is an often difficult decision in a stable patient with minimal evidence of blood clot on ultrasound.[citation needed]
Surgeons use laparoscopy or laparotomy to gain access to the pelvis and can either incise the affected fallopian tube and remove only the pregnancy (salpingostomy) or remove the affected tube with the pregnancy (salpingectomy). The first successful surgery for an ectopic pregnancy was performed by Robert Lawson Tait in 1883.[60] It is estimated that an acceptable rate of PULs that eventually undergo surgery is between 0.5 and 11%.[5] People that undergo salpingectomy and salpingostomy have a similar recurrent ectopic pregnancy rate of 5% and 8% respectively. Additionally, their intrauterine pregnancy rates are also similar, 56% and 61%.[61]
Autotransfusion of a woman's own blood as drained during surgery may be useful in those who have a lot of bleeding into their abdomen.[62]
Published reports that a re-implanted embryo survived to birth were debunked as false.[63]
Prognosis
When ectopic pregnancies are treated, the prognosis for the mother is very good in Western countries; maternal death is rare, but all fetuses die or are aborted. For instance, in the UK, between 2003 and 2005 there were 32,100 ectopic pregnancies resulting in 10 maternal deaths (meaning that 1 in 3,210 women with an ectopic pregnancy died).[64] In 2006–2008 the UK Confidential Enquiry into Maternal Deaths found that ectopic pregnancy is the cause of 6 maternal deaths (0.26/100,000 pregnancies).[18]
In the developing world, however, especially in Africa, the death rate is very high, and ectopic pregnancies are a major cause of death among women of childbearing age.
In women having had an ectopic pregnancy, the risk of another one in the next pregnancy is around 10%.[65]
Future fertility
Fertility following ectopic pregnancy depends upon several factors, the most important of which is a prior history of infertility.[66] The treatment choice does not play a major role; a randomized study in 2013 concluded that the rates of intrauterine pregnancy two years after treatment of ectopic pregnancy are approximately 64% with radical surgery, 67% with medication, and 70% with conservative surgery.[67] In comparison, the cumulative pregnancy rate of women under 40 years of age in the general population over two years is over 90%.[68]
Methotrexate does not affect future fertility treatments. The number of oocytes that were retrieved before and after treatment with methotrexate does not change.[69]
In case of ovarian ectopic pregnancy, the risk of subsequent ectopic pregnancy or infertility is low.[70]
There is no evidence that massage improves fertility after ectopic pregnancy.[71]
Epidemiology
The rate of ectopic pregnancy is about 1% and 2% of that of live births in developed countries, though it is as high as 4% in pregnancies involving assisted reproductive technology.
Between 5% and 42% of women seen for ultrasound assessment with a positive pregnancy test have a pregnancy of unknown location, that is a positive pregnancy test but no pregnancy visualized at transvaginal ultrasonography.[5] Between 6% and 20% of pregnancy of unknown location are subsequently diagnosed with actual ectopic pregnancy.[5]
Society and culture
Salpingectomy as a treatment for ectopic pregnancy is one of the common cases when the principle of double effect can be used to justify accelerating the death of the embryo by doctors and patients opposed to outright abortions.[73]
In the Catholic Church, there are moral debates on certain treatments. A significant number of Catholic moralists consider use of methotrexate and the salpingostomy procedure to be not "morally permissible" because they destroy the embryo; however, situations are considered differently in which the mother's health is endangered, and the whole fallopian tube with the developing embryo inside is removed.[74][75]
Organisations exist that provide information and support to help those who experience ectopic pregnancy. Studies show that people can experience post-traumatic stress, depression, and anxiety for which they would need specialist therapies.[76] Partners can also experience post-traumatic stress.[77]
Live birth
There have been cases where ectopic pregnancy lasted many months and ended in a live baby delivered by laparotomy.
In July 1999, Lori Dalton gave birth by caesarean section in Ogden, Utah, United States, to a healthy baby girl, Saige, who had developed outside of the uterus. Previous ultrasounds had not discovered the problem. "[Dalton]'s delivery was slated as a routine Caesarean birth at Ogden Regional Medical Center in Utah. When Dr. Naisbitt performed Lori's Caesarean, he was astonished to find Saige within the amniotic membrane outside the womb ... ."[78] "But what makes this case so rare is that not only did mother and baby survive—they're both in perfect health. The father, John Dalton took home video inside the delivery room. Saige came out doing extremely well because even though she had been implanted outside the womb, a rich blood supply from a uterine fibroid along the outer uterus wall had nourished her with a rich source of blood."[79]
In September 1999 an English woman, Jane Ingram (age 32) gave birth to triplets: Olivia, Mary and Ronan, with an extrauterine fetus (Ronan) below the womb and
On May 29, 2008, an Australian woman, Meera Thangarajah (age 34), who had an ectopic pregnancy in the ovary, gave birth to a healthy full term 6 pound 3 ounce (2.8 kg) baby girl, Durga, via Caesarean section. She had no problems or complications during the 38‑week pregnancy.[81][82]
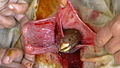
Animals
Ectopic gestation exists in
-
Leg of fetal lamb appearing out of the uterus during caesarean section
-
External view of fetal sac, necrotic distal part
-
Internal view of fetal sac, before resection of distal necrotic part
-
Internal view of fetal sac. The necrotic distal part is to the left.
-
External side of fetal sac, proximal end, with ovary and uterine horn
-
Resected distal part of fetal sac, with attached placenta
See also
References
- ^ S2CID 205049738.
- ^ S2CID 26727563.
- PMID 31168219.
- ^ a b Mignini L (26 September 2007). "Interventions for tubal ectopic pregnancy". who.int. The WHO Reproductive Health Library. Archived from the original on 2 April 2015. Retrieved 12 March 2015.
- ^ PMID 24101604.
- S2CID 35923100.
- ^ S2CID 22538462.
- ISBN 9780877799108. Archivedfrom the original on 2017-09-10.
- S2CID 333306.
- ^ "Ectopic pregnancy". Archived from the original on 28 August 2021. Retrieved 4 December 2018.
- ISBN 978-0-323-03506-4.
- PMID 10706160.
- S2CID 26445888.
- PMID 18232175.
- ^ "BestBets: Risk Factors for Ectopic Pregnancy". Archived from the original on 2008-12-19.
- S2CID 42807796.
- ISBN 9781444358476. Archivedfrom the original on 2017-09-10.
- ^ PMID 26571203.
- S2CID 30584041.
- PMID 21727242.
- PMID 22510618.
- ^ a b Saraswat, Lucky (2015). "ESHRE2015: Endometriosis associated with a greater risk of complications in pregnancy". endometriosis.org. European Society of Human Reproduction and Embryology. Retrieved 14 February 2024.
- ^ PMID 16565155.
- PMID 10924442.
- ^ ISBN 978-0-683-30379-7.
- ^ PMID 6281085.
- PMID 3583040.
- PMID 4038744.
- PMID 10438408.
- ^ from the original on 2015-04-02.
- PMID 19482272.
- S2CID 25547683.
- ^ "Pelvic Ultrasound". www.hopkinsmedicine.org. 8 August 2021. Retrieved 2022-04-26.
- ^ "UOTW#61 - Ultrasound of the Week". Ultrasound of the Week. 14 October 2015. Archived from the original on 9 May 2017.
- PMID 22956411.
- PMID 20071358.
- Who Named It?
- ^ "'Special' baby grew outside womb". BBC News. 2005-08-30. Archived from the original on 2007-02-12. Retrieved 2006-07-14.
- ^ "Bowel baby born safely". BBC News. 2005-03-09. Archived from the original on 2007-02-11. Retrieved 2006-11-10.
- S2CID 35923100.
- ^ "Rates of Cesarean Delivery -- United States, 1993". www.cdc.gov. Retrieved 2020-08-11.
- PMID 26849801.
- S2CID 27272542.
- ^ S2CID 36067188.
- ^ a b c Luis Izquierdo, M. D.; Mariam Savabi, M. D. (16 August 2019). "How to diagnose and treat cesarean scar pregnancy". Contemporary Ob/Gyn Journal. Vol 64 No 08. 64 (8). Retrieved 2020-08-11.
- S2CID 39198754.
- ^ S2CID 34003037.
- )
- S2CID 28083933.
- PMID 9022622.
- PMID 26345396.
- S2CID 51966025.
- PMID 10438980.
- S2CID 5616550.
- PMID 9050473.
- PMID 17591007.
- ^ "History, Diagnosis and Management of Ectopic Pregnancy" Archived 2015-10-05 at the Wayback Machine
- PMID 32609376.
- PMID 27572300.
- ^ "eMedicine - Surgical Management of Ectopic Pregnancy: Article Excerpt by R Daniel Braun". Archived from the original on 2007-10-13. Retrieved 2007-09-17.
- PMID 29059454.
- S2CID 24721754.
- PMID 16672756.
- ^ "Ectopic Pregnancy". Archived from the original on 2015-10-14. Retrieved 2015-10-22.
- ISBN 9781841848181.
- ISBN 978-0-8247-0844-3.
- PMID 23482340.
- NICE clinical guidelineCG156 – Issued: February 2013
- PMID 25056087.
- PMID 25709640.
- PMID 29593844.
- .
- ^ Delgado G. "Pro-Life Open Forum, Apr 10, 2013 (49min40s)". Catholic answers. Archived from the original on 2 April 2015. Retrieved 2 September 2014.
- ^ Pacholczyk T. "When Pregnancy Goes Awry". Making Sense Out of Bioethics (blog). National Catholic Bioethics Center. Archived from the original on 2011-11-23.
- ^ Anderson, MA et al. Ectopic Pregnancy and Catholic Morality Archived 2016-04-18 at the Wayback Machine. National Catholic Bioethics Quarterly, Spring 2011
- ^ "Post-traumatic stress, anxiety and depression following miscarriage and ectopic pregnancy: a multicenter, prospective, cohort study". Farren J, Jalmbrant M, Falconieri N, et al. Am J Obstet Gynecol 2020;222:367.e1-22.
- ^ "Post-traumatic stress experienced by partners following miscarriage". 9 October 2020.
- ^ "Registry Reports" (PDF). Volume XVI, Number 5. Ogden, Utah: ARDMS The Ultrasound Choice. October 1999. Archived from the original (PDF) on 2010-12-23. Retrieved 2011-06-22.
- ^ "Miracle baby". Ogden, Utah: Utah News from KSL-TV. 1999-08-05. Archived from the original on 2011-09-30. Retrieved 2011-06-22.
- ^ "Doctors hail 'miracle' baby". BBC News. 2009-09-10. Archived from the original on 2008-09-19.
- ^ "Baby Born After Rare Ovarian Pregnancy". Associated Press. 2008-05-30. Archived from the original on June 3, 2008. Retrieved 2008-05-30.
- ^ Cavanagh R (2008-05-30). "Miracle baby may be a world first". Archived from the original on 2008-05-30. Retrieved 2008-05-30.