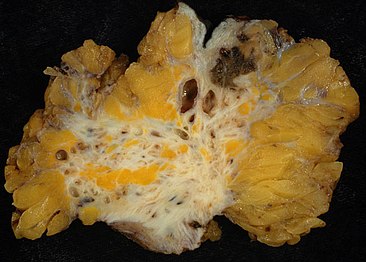
Endometriosis
| Endometriosis | |
|---|---|
intrauterine device with progestogen, surgery[2] | |
| Frequency | 10–15% of all women of reproductive age[4] |
| Deaths | ≈100 (0.0 to 0.1 per 100,000, 2015)[5][6] |
Endometriosis is a disease of the female reproductive system. It occurs in women and a limited number of
Diagnosis is usually based on symptoms and medical imaging;[2] but biopsy is the surest method of diagnosis.[2] Other causes of similar symptoms include pelvic inflammatory disease, irritable bowel syndrome, interstitial cystitis, and fibromyalgia.[1] Endometriosis is often misdiagnosed and many patients report being incorrectly told their symptoms are trivial or normal.[11] Patients with endometriosis see an average of seven physicians before receiving a correct diagnosis, with an average delay of 6.7 years between the onset of symptoms and surgically obtained biopsies, the gold standard for diagnosing the condition. This places endometriosis at the extreme end of diagnostic inefficiency.[12]
Nearly 11 million women are affected by endometriosis, globally.
The main cause of endometriosis is exposure to elevated levels of the female sex hormone estrogen, as well as estrogen receptor sensitivity.[15] Estrogen exposure worsens the inflammatory symptoms of endometriosis by stimulating an immune response.[16][17]
There is no cure for endometriosis, but a number of treatments may improve symptoms.
Signs and symptoms

Pain and infertility are common symptoms, although 20–25% of affected women are asymptomatic.[1] Presence of pain symptoms are associated with the type of endometrial lesions as 50% of women with typical lesions, 10% of women with cystic ovarian lesions, and 5% of women with deep endometriosis do not have pain.[18]
Pelvic pain
A major symptom of endometriosis is recurring pelvic pain. The pain can range from mild to severe cramping or stabbing pain that occurs on both sides of the pelvis, in the lower back and rectal area, and even down the legs. The amount of pain a person feels correlates weakly with the extent or stage (1 through 4) of endometriosis, with some individuals having little or no pain despite having extensive endometriosis or endometriosis with scarring, while others may have severe pain even though they have only a few small areas of endometriosis.[19] The most severe pain is typically associated with menstruation. Pain can also start a week before a menstrual period, during and even a week after a menstrual period, or it can be constant. The pain can be debilitating and result in emotional stress.[20] Symptoms of endometriosis-related pain may include:
- dysmenorrhea (64%)[21] – painful, sometimes disabling cramps during the menstrual period; pain may get worse over time (progressive pain), also lower back pains linked to the pelvis
- chronic pelvic pain– typically accompanied by lower back pain or abdominal pain
- dyspareunia – painful sexual intercourse
- dysuria – urinary urgency, frequency, and sometimes painful voiding[22]
- mittelschmerz – pain associated with ovulation[23]
- bodily movement pain – present during exercise, standing, or walking[22]
Compared with patients with superficial endometriosis, those with deep disease appear to be more likely to report shooting rectal pain and a sense of their insides being pulled down.[24] Individual pain areas and pain intensity appear to be unrelated to the surgical diagnosis, and the area of pain unrelated to the area of endometriosis.[24]
There are multiple causes of pain. Endometriosis lesions react to hormonal stimulation and may "bleed" at the time of menstruation. The blood accumulates locally if it is not cleared shortly by the immune, circulatory, and lymphatic system. This may further lead to swelling, which triggers inflammation with the activation of
Also, endometriotic lesions can develop their own nerve supply, thereby creating a direct and two-way interaction between lesions and the central nervous system, potentially producing a variety of individual differences in pain that can, in some cases, become independent of the disease itself.[19] Nerve fibres and blood vessels are thought to grow into endometriosis lesions by a process known as neuroangiogenesis.[26]
Infertility
About a third of women with infertility have endometriosis.[1] Among those with endometriosis, about 40% are infertile.[1] The pathogenesis of infertility is dependent on the stage of disease: in early stage disease, it is hypothesised that this is secondary to an inflammatory response that impairs various aspects of conception, whereas in later stage disease distorted pelvic anatomy and adhesions contribute to impaired fertilisation.[27]
Other
Other symptoms include diarrhea or
Rarely, endometriosis can cause endometrium-like tissue to be found in other parts of the body. Thoracic endometriosis occurs when endometrium-like tissue implants in the lungs or pleura. Manifestations of this include coughing up blood, a collapsed lung, or bleeding into the pleural space.[13][33] Endometriosis may also involve the nearby colon which in rare situations may progress to partial obstruction requiring emergency surgery.[34]
Stress may be a cause or a consequence of endometriosis.[35]
Complications
Physical health
Complications of endometriosis include internal scarring,
Ovarian endometriosis may complicate pregnancy by decidualization, abscess and/or rupture.[37]
A 20-year study of 12,000 women with endometriosis found that individuals under 40 who are diagnosed with endometriosis are three times more likely to have heart problems than their healthy peers.[40]
Results of a 30-year study of reproductive and pregnancy outcomes, involving 14,000+ women of child-bearing age, were presented at the 2015 European Society of Human Reproduction and Embryology (ESHRE) annual congress.[41] 39% of the study group had surgically confirmed non-graded endometriosis. The endometriosis subgroup had a 270% higher risk for ectopic pregnancy and a 76% higher risk for miscarriage compared to their peers. The miscarriage risk increased to 298% for women having deep endometriosis with >5 mm invasion (ASRM Stage II and higher).[42]
Women with endometriosis also have a significantly increased risk of experiencing ante- and postpartum hemorrhage[41] and an 170% increased risk of severe pre-eclampsia[43] during their pregnancies.
Endometriosis may increase about 1% or less chance of getting ovarian, breast and thyroid cancers in women compared with those without.[44]
It results in few deaths with unadjusted and age-standardized death rates of 0.1 and 0.0 per 100,000.[5]
Sciatic endometriosis also called catamenial or cyclical sciatica is a sciatica whose cause is endometriosis and whose incidence is unknown. Diagnosis is usually made by an MRI or CT-myelography.[45]
Endometriosis can also impact a woman's
Mental health
"Endometriosis is associated with an elevated risk of developing depression and anxiety disorders".[46] Studies suggest this is partially due to the pelvic pain experienced by endometriosis patients.
"It has been demonstrated that pelvic pain has significant negative effects on women's mental health and quality of life; in particular, women who suffer from pelvic pain report high levels of anxiety and depression, loss of working ability, limitations in social activities and a poor quality of life" [47]
Risk factors
Genetics
Endometriosis is a heritable condition influenced by both genetic and environmental factors,
Inheritance is significant, but not the sole risk factor for endometriosis. Studies attribute 50% of risk to genetics, the other 50% likely from environmental factors.[52] It has been proposed that endometriosis results from a series of multiple hits, i.e., multiple different mutations, within target genes, in a mechanism similar to the development of cancer.[48] In this case, the mutations may be either somatic or heritable.[48]
A 2019 genome-wide association study (GWAS) review enumerated 36 genes having mutations associated with endometriosis development.[53] Nine chromosome loci were robustly replicated:[54][55][56][57]
| Chromosome | Gene/cytoband | Gene Product | Function |
|---|---|---|---|
| 1 | WNT4/1p36.12 | Wingless-type MMTV integration site family member 4 | Vital for development of the female reproductive organs |
| 2 | GREB1/2p25.1 | Growth regulation by estrogen in breast cancer 1/Fibronectin 1 | Early response gene in the estrogen regulation pathway/Cell adhesion and migration processes |
| 2 | ETAA1/2p14 | (ETAA1 Activator Of ATR Kinase) is a Protein Coding gene. | Diseases associated with ETAA1 include Adult Lymphoma and Restless Legs Syndrome |
| 2 | IL1A/2q13 | Interleukin 1 alpha (IL-1α) is encoded by the IL1A gene. | Interleukin 1 alpha (IL-1α) is encoded by the IL1A gene. |
| 4 | KDR/4q12 | KDR is the human gene encoding kinase insert domain receptor also known as vascular endothelial growth factor receptor 2 (VEGFR-2) | Primary mediator of VEGF-induced endothelial proliferation, survival, migration, tubular morphogenesis and sprouting[58] |
| 6 | ID4/6p22.3 | Inhibitor of DNA binding 4 | Ovarian oncogene, biological function unknown |
| 7 | 7p15.2 | Transcription factors | Influence transcriptional regulation of uterine development |
| 9 | CDKN2BAS/9p21.3 | Cyclin-dependent kinase inhibitor 2B antisense RNA | Regulation of tumour suppressor genes |
| 12 | VEZT/12q22 | Vezatin, an adherens junction transmembrane protein | Tumor suppressor gene |
There are many findings of altered
Environmental toxins
Some factors associated with endometriosis include:
- prolonged exposure to naturally synthesized estrogen; for example, from late menopause[17] or early menarche[59][60]
- obstruction of menstrual outflow; for example, in Müllerian anomalies[17]
Potential toxins:
- Dioxins- Several studies have investigated the potential link between exposure to dioxins and endometriosis, but evidence is equivocal and potential mechanisms are poorly understood.[61] A 2004 review of studies of dioxin and endometriosis concluded that "the human data supporting the dioxin-endometriosis association are scanty and conflicting",[62] and a 2009 follow-up review also found that there was "insufficient evidence" in support of a link between dioxin exposure and developing endometriosis.[63]
- Endocrine-disrupting chemicals (EDCs)- A wider class of hormonally active agents, to which dioxin belongs, consists of both natural and manmade compounds, e.g., bisphenols, phthalates, pesticides (chlorpyrifos, hexachlorobenzene) and polychlorinated biphenyls (PCBs).[64] Dietary uptake represents a significant source of EDC exposure via consumption of food, water and beverages, but exposure can also occur through ingestion of EDC dust and inhalation of its gases or particles in the air.[64] Most EDCs are lipophilic, allowing them to bioaccumulate in adipose tissue (body fat) and increase in concentration.[65] Bisphenol A (BPA), bisphenol S (BPS), phthalates, pesticides and PCBs all have a suspected linkage to endometriosis,[64] though have not been definitively proven as being causative.[65]
Vaginal dysbiosis
A growing body of evidence has shown a correlation between an imbalance in the vaginal
Pathophysiology

While the exact cause of endometriosis remains unknown, many theories have been presented to better understand and explain its development. These concepts do not necessarily exclude each other. The pathophysiology of endometriosis is likely to be multifactorial and to involve an interplay between several factors.[48]
Formation
The main theories for the formation of the ectopic endometrium-like tissue include retrograde menstruation, Müllerianosis, coelomic metaplasia, vascular dissemination of stem cells, and surgical transplantation were postulated as early as 1870. Each is further described below.[13][68][69]
Retrograde menstruation theory
The theory of retrograde menstruation (also called the implantation theory or transplantation theory) is the most commonly accepted theory for the dissemination and transformation of ectopic endometrium into endometriosis. It suggests that during a woman's menstrual flow, some of the endometrial debris flow backward through the Fallopian tubes and into the peritoneal cavity, attaching itself to the peritoneal surface (the lining of the abdominal cavity) where it can proceed to invade the tissue as or transform into endometriosis. It is not clear at what stage the transformation of endometrium, or any cell of origin such as stem cells or coelomic cells (see those theories below), to endometriosis begins.[48][68][70]
Proofs in support of the theory are based on retrospective epidemiological studies that an association with endometrial implants attached to the peritoneal cavity, which would develop into endometrial lesions and retrograde menstruation; and the fact that animals like rodents and non-human primates whose endometrium is not shed during the estrous cycle don't develop naturally endometriosis contrary to animals that have a natural menstrual cycle like rhesus monkeys and baboons.[71]
Retrograde menstruation alone is not able to explain all instances of endometriosis, and additional factors such as genetics, immunology, stem cell migration, and coelomic metaplasia (see "Other theories" on this page) are needed to account for disseminated disease and why many individuals with retrograde menstruation are not diagnosed with endometriosis. In addition, endometriosis has shown up in people who have never experienced menstruation including cisgender men,[72] fetuses,[73] and prepubescent girls.[74][75] Further theoretical additions are needed to complement the retrograde menstruation theory to explain why cases of endometriosis show up in the brain[76] and lungs.[77]
Researchers are investigating the possibility that the immune system may not be able to cope with the cyclic onslaught of retrograde menstrual fluid. In this context there is interest in studying the relationship of endometriosis to autoimmune disease, allergic reactions, and the impact of toxic materials.[16][78] It is still unclear what, if any, causal relationship exists between toxic materials or autoimmune disease and endometriosis. There are immune system changes in people with endometriosis, such as an increase of macrophage-derived secretion products, but it is unknown if these are contributing to the disorder or are reactions from it.[79]
Endometriotic lesions differ in their biochemistry, hormonal response, immunology, inflammatory response when compared to endometrium.[13][80] This is likely because the cells that give rise to endometriosis are a side population of cells.[48] Similarly, there are changes in, for example, the mesothelium of the peritoneum in people with endometriosis, such as loss of tight junctions, but it is unknown if these are causes or effects of the disorder.[79]
In rare cases where
The theory of retrograde menstruation as a cause of endometriosis was first proposed by John A. Sampson.[68][81]
Other theories
- Stem cells: Endometriosis may arise from stem cells from bone marrow and potentially other sources. In particular, this theory explains endometriosis found in areas remote from the pelvis such as the brain or lungs.[69] Stem cells may be from local cells such as the peritoneum (see coelomic metaplasia below) or cells disseminated in the blood stream (see vascular dissemination below) such as those from the bone marrow.[68][69][82]
- Vascular dissemination: Vascular dissemination is a 1927 theory that has been revived with new studies of bone-marrow stem cells involved in pathogenesis.[69][82]
- Environment: Environmental toxins (e.g., dioxin, nickel) may cause endometriosis.[83][84] Toxins such as dioxins and dioxin-like compounds tend to bioaccumulate within the human body. Further research is needed but "it is plausible that inflammatory-like processes, caused by dioxin-like environmental chemicals, can alter normal endometrial and immune cell physiology allowing persistence and development of endometrial tissue within the peritoneal cavity, normally cleared by immune system cells".[85]
- Müllerianosis: A theory supported by foetal autopsy is that cells with the potential to become endometrial, which are laid down in tracts during embryonic development called the female reproductive (Müllerian) tract as it migrates downward at 8–10 weeks of embryonic life, could become dislocated from the migrating uterus and act like seeds or
- Coelomic metaplasia: peritoneal cells may undergo metaplasia (transformation) from one type of cell to the other, perhaps triggered by inflammation.[68][86]
- Vasculogenesis: Up to 37% of the microvascular endothelium of ectopic endometrial tissue originates from endothelial progenitor cells, which result in de novo formation of microvessels by the process of vasculogenesis rather than the conventional process of angiogenesis.[87][clarification needed]
- Neural growth: An increased expression of new nerve fibres is found in endometriosis but does not fully explain the formation of ectopic endometriotic tissue and is not definitely correlated with the amount of perceived pain.[88][clarification needed]
- Autoimmune: Graves disease is an autoimmune disease characterized by hyperthyroidism, goiter, ophthalmopathy, and dermopathy. People with endometriosis had higher rates of Graves disease. One of these potential links between Graves disease and endometriosis is autoimmunity.[89][90]
- high-grade lesions.[91]
Localization
Most often, endometriosis is found on the:
- ovaries
- fallopian tubes
- tissues that hold the uterus in place (ligaments)
- outer surface of the uterus[2]
Less common pelvic sites are:
Endometriosis may spread to the cervix and vagina or to sites of a surgical abdominal incision, known as "scar endometriosis."[92] Rectovaginal or bowel endometriosis affects approximately 5-12% of those with endometriosis, and can cause severe pain with bowel movements.[93][citation needed]
Deep infiltrating endometriosis (DIE) has been defined as the presence of endometrial glands and stroma infiltrating more than 5 mm in the subperitoneal tissue. The prevalence of DIE is estimated to be 1 to 2% in women of reproductive age. Deep endometriosis typically presents as a single nodule in the vesicouterine fold or in the lower 20 cm of the bowel. Deep endometriosis can be associated with severe pain. However, it can be present without severe levels of pain.[94]
Extrapelvic endometriosis
Rarely, endometriosis appears in extrapelvic parts of the body, such as the lungs, brain, and skin.[2][39][92] "Scar endometriosis" can occur in surgical abdominal incisions.[92] Risk factors for scar endometriosis include previous abdominal surgeries, such as a hysterotomy or cesarean section, or ectopic pregnancies, salpingostomy puerperal sterilization, laparoscopy, amniocentesis, appendectomy, episiotomy, vaginal hysterectomies, and hernia repair.[95][96][97]
Endometriosis may also present with skin lesions in cutaneous endometriosis.[92]
Less commonly lesions can be found on the diaphragm or lungs. Diaphragmatic endometriosis is rare, almost always on the right hemidiaphragm, and may inflict the cyclic pain of the right
Diagnosis
A health history and a physical examination can lead the health care practitioner to suspect endometriosis. There is a clear benefit for performing a
Definitive diagnosis is based on the morphology (form and structure) of the pelvic region, determined by observation (surgical or non-invasive imaging), classified into four different stages of endometriosis. The American Society of Reproductive Medicine's scale, revised in 1996, gives higher scores to deep, thick lesions or intrusions on the ovaries and dense, enveloping adhesions on the ovaries or fallopian tubes.[99] Additionally, histological studies, when performed, should show specific findings.
For many patients, there are significant delays in diagnosis. Studies show an average delay of 11.7 years in the United States. Patients in the UK have an average delay of 8 years and in Norway of 6.7 years.[100] A third of women had consulted their GP six or more times before being diagnosed.[100]
The most common sites of endometriosis are the ovaries, followed by the Douglas pouch, the posterior leaves of the broad ligaments, and the sacrouterine ligaments.[21]
As for deep infiltrating endometriosis,
Laparoscopy
Laparoscopy, a surgical procedure where a camera is used to look inside the abdominal cavity, is the only way to accurately diagnose the extent and severity of pelvic/abdominal endometriosis.[102] Laparoscopy is not an applicable test for extrapelvic sites such as umbilicus, hernia sacs, abdominal wall, lung, or kidneys.[102]
Reviews in 2019 and 2020 concluded that 1) with advances in imaging, endometriosis diagnosis should no longer be considered synonymous with immediate laparoscopy for diagnosis, and 2) endometriosis should be classified a syndrome that requires confirmation of visible lesions seen at laparoscopy in addition to characteristic symptoms.[103][104]
Laparoscopy permits lesion visualization unless the lesion is visible externally (e.g., an endometriotic nodule in the vagina) or is extra-abdominal.[102] If the growths (lesions) are not visible, a biopsy must be taken to determine the diagnosis.[105] Surgery for diagnoses also allows for surgical treatment of endometriosis at the same time.
During a laparoscopic procedure, lesions can appear dark blue, powder-burn black, red, white, yellow, brown or non-pigmented. Lesions vary in size.[106] Some within the pelvis walls may not be visible, as normal-appearing peritoneum of infertile women reveals endometriosis on biopsy in 6–13% of cases.[107] Early endometriosis typically occurs on the surfaces of organs in the pelvic and intra-abdominal areas.[106] Health care providers may call areas of endometriosis by different names, such as implants, lesions, or nodules. Larger lesions may be seen within the ovaries as endometriomas or "chocolate cysts", "chocolate" because they contain a thick brownish fluid, mostly old blood.[106]
Frequently during diagnostic laparoscopy, no lesions are found in individuals with chronic pelvic pain, a symptom common to other disorders including
Ultrasound
Vaginal ultrasound can be used to diagnosis endometriosis, or for localizing endometrioma before surgery.[109] This can be used to identify the spread of disease in individuals with well-established clinical suspicion of endometriosis.[109] Vaginal ultrasound is inexpensive, easily accessible, has no contraindications and requires no preparation.[109] By extending the ultrasound assessment into the posterior and anterior pelvic compartments a sonographer is able to evaluate structural mobility and look for deep infiltrating endometriotic nodules.[110] Better sonographic detection of deep infiltrating endometriosis could reduce the number of diagnostic laparoscopies, as well as guide disease management and enhance patient quality of life.[110]
Magnetic resonance imaging
MRI is another means of detecting lesions in a non-invasive manner.
Stages of disease
By surgical observation, endometriosis can be classified as stage I–IV by the 1996 scale of the
Stage I (Minimal)
- Findings restricted to only superficial lesions and possibly a few filmy adhesions.
Stage II (Mild)
- In addition, some deep lesions are present in the cul-de-sac.
Stage III (Moderate)
- As above, plus the presence of endometriomas on the ovary and more adhesions.
Stage IV (Severe)
- As above, plus large endometriomas, extensive adhesions. Implants and adhesions may be found beyond the uterus. Large ovarian cysts are common.
Markers
An area of research is the search for endometriosis markers.[113]
In 2010, essentially all proposed biomarkers for endometriosis were of unclear medical use, although some appear to be promising.
Another review in 2011 identified several putative biomarkers upon biopsy, including findings of small sensory nerve fibers or defectively expressed
A 2016 review of endometrial biomarkers for diagnosing endometriosis was unable to draw conclusions due to the low quality of the evidence.[116]
MicroRNAs have the potential to be used in diagnostic and therapeutic decisions.[117]
Histopathology
For a histopathological diagnosis, at least two of the following three criteria should be present:[118]
- Endometrial type stroma
- Endometrial epithelium with glands
- Evidence of chronic hemorrhage, mainly hemosiderin deposits
-
Endometriosis, abdominal wall
-
Micrograph showing endometriosis (right) and ovarian stroma (left)
-
stroma and hemosiderin-laden macrophages).
Pain quantification
The most common
Prevention
Limited evidence indicates that the use of combined oral contraceptives is associated with a reduced risk of endometriosis, as is regular exercise and the avoidance of alcohol and caffeine.[2] There is little known information on preventing endometriosis.[121]
Management
While there is no cure for endometriosis, there are two types of interventions; treatment of pain and treatment of
Pharmacotherapy for pain management can be initiated based on the presence of symptoms and examination and ultrasound findings that rule out other potential causes.[125]
In general, the diagnosis of endometriosis is confirmed during surgery, at which time removal can be performed. Further steps depend on circumstances: someone without infertility can manage symptoms with pain medication and hormonal medication that suppresses the natural cycle, while an infertile individual may be treated expectantly after surgery, with fertility medication, or with in vitro fertilisation (IVF).
A 2020 Cochrane systematic review found that for all types of endometriosis, "it is uncertain whether laparoscopic surgery improves overall pain compared to diagnostic laparoscopy".[126]
Surgery
Based on strong evidence, experts recommend that surgery be performed laparoscopically (through keyhole surgery) rather than open.
As for deep endometriosis, a segmental resection or shaving of nodules is effective but is associated with an increased rate of complications, of which about 4.6% are major.[133]
Historically, a hysterectomy (removal of the uterus) was thought to be a cure for endometriosis in individuals who do not wish to conceive. Removal of the uterus may be beneficial as part of the treatment, if the uterus itself is affected by adenomyosis. However, this should only be done in combination with removal of the endometriosis by excision. If endometriosis is not also removed at the time of hysterectomy, pain may persist.[105] A study of hysterectomy patients found those with endometriosis were not using less pain medication 3 years after the procedure.[134]
Presacral neurectomy may be performed where the nerves to the uterus are cut. However, this technique is not usually used due to the high incidence of associated complications including presacral hematoma and irreversible problems with urination and constipation.[105]
Recurrence
The underlying process that causes endometriosis may not cease after a surgical or medical intervention. A study has shown that dysmenorrhea recurs at a rate of 30 percent within a year following laparoscopic surgery. Resurgence of lesions tend to appear in the same location if the lesions were not completely removed during surgery. It has been shown that laser ablation resulted in higher and earlier recurrence rates when compared with endometrioma cystectomy; and recurrence after repetitive laparoscopy was similar to that after the first surgery. Endometriosis has a 10% recurrence rate after hysterectomy and bilateral salpingo-oophorectomy.[135]
Endometriosis recurrence following conservative surgery is estimated as 21.5% at 2 years and 40-50% at 5 years.[136]
Recurrence rate for DIE after surgery is less than 1%.[137]
Risks and safety of pelvic surgery
Risk of developing complications following surgery depend on the type of the lesion that has undergone surgery.[127] 55% to 100% of individuals develop adhesions following pelvic surgery,[138] which can result in infertility, chronic abdominal and pelvic pain, and difficult reoperative surgery. Trehan's temporary ovarian suspension, a technique in which the ovaries are suspended for a week after surgery, may be used to reduce the incidence of adhesions after endometriosis surgery.[139][140] Removal of cysts on the ovary without removing the ovary is a safe procedure.[127]
Hormonal medications
- Birth control pills reduce the menstrual pain and recurrence rate for endometrioma following conservative surgery for endometriosis.[141] A 2018 Cochrane systematic review found that there is insufficient evidence to make a judgement on the effectiveness of the combined oral contraceptive pill compared with placebo or other medical treatment for managing pain associated with endometriosis partly because of lack of included studies for data analysis (only two for COCP vs placebo).[142]
- voice changes.[144] There is tentative evidence based on cohort studies that dienogest and norethisterone acetate (NETA) may help patients with DIE in terms of pain.[145] There is tentative evidence based on a prospective study that vaginal danazol reduces pain in those affected by DIE.[145]
- GnRH antagonists such as elagolix and are thought to work by decreasing estrogen levels.[146] A 2010 Cochrane review found that GnRH modulators were more effective for pain relief in endometriosis than no treatment or placebo, but were not more effective than danazol or intrauterine progestogen, and had more side effects than danazol.[146] A 2018 Swedish systematic review found that GnRH modulators had similar pain-relieving effects to gestagen, but also decreased bone density.[109]
- Aromatase inhibitors are medications that block the formation of estrogen and have become of interest for researchers who are treating endometriosis.[147] Examples of aromatase inhibitors include anastrozole and letrozole. Evidence for aromatase inhibitors is confirmed by numerous controlled studies that show benefit in terms of pain control and quality of life when used in combination with gestagens or oral contraceptives with less side-effects when used in combination with oral contraceptives like norethisterone acetate.[148] Despite multiple benefits, there are lot of things to consider before using aromatase inhibitors for endometriosis, as it is common for them to induce functional cysts as an adverse effects. Moreover, dosages, treatment length, appropriate add-back therapies and mode of administration is still being investigated.[149]
- Progesterone receptor modulators like mifepristone and gestrinone have the potential (based on only one randomized controlled trial each) to be used as a treatment to manage pain caused by endometriosis.[150]
Other medicines
- Melatonin, there is tentative evidence for its use (at a dose of 10 mg) in reducing pain related to endometriosis.[151]
- Opioids: Morphine sulphate tablets and other opioid painkillers work by mimicking the action of naturally occurring pain-reducing chemicals called "endorphins". There are different long acting and short acting medications that can be used alone or in combination to provide appropriate pain control.
- Chinese herbal medicine was reported to have comparable benefits to gestrinone and danazol in patients who had had laparoscopic surgery, though the review notes that the two trials were small and of "poor methodological quality" and results should be "interpreted cautiously" as better quality research is needed.[152]
- Serrapeptase, a digestive enzyme found in the intestines of silkworms. Serrapeptase is widely used in Japan and Europe as an anti-inflammatory treatment.[153] More research is needed but serrapeptase may be used by endometriosis patients to reduce inflammation.[154]
- progestins, danazol and gonadotropin-releasing hormone agonists.[155] However, many of these agents are associated with undesirable side effects and more research is necessary. An ideal therapy would diminish inflammation and underlying symptoms without being contraceptive.[156][157]
- American Congress of Obstetricians and Gynecologists (ACOG) guidelines do not include immunomodulators, such as pentoxifylline, in standard treatment protocols.[159]
- NSAIDs are anti-inflammatory medications commonly used for endometriosis patients despite unproven efficacy and unintended adverse effects.[160]
- Neuromodulators like gabapentin did not prove to be superior to placebo in managing pain caused by endometriosis.[161]
The overall effectiveness of manual physical therapy to treat endometriosis has not yet been identified.[162]
Comparison of interventions
A 2021 meta-analysis found that GnRH analogues and combined hormonal contraceptives were the best treatment for reducing dyspareunia, menstrual and non menstrual pelvic pain.[163] A 2018 Swedish systematic review found a large number of studies but a general lack of scientific evidence for most treatments.[109] There was only one study of sufficient quality and relevance comparing the effect of surgery and non-surgery.[164] Cohort studies indicate that surgery is effective in decreasing pain.[164] Most complications occurred in cases of low intestinal anastomosis, while risk of fistula occurred in cases of combined abdominal or vaginal surgery, and urinary tract problems were common in intestinal surgery.[164] The evidence was found to be insufficient regarding surgical intervention.[164]
The advantages of physical therapy techniques are decreased cost, absence of major side-effects, it does not interfere with fertility, and near-universal increase of sexual function.[165] Disadvantages are that there are no large or long-term studies of its use for treating pain or infertility related to endometriosis.[165]
Treatment of infertility
Surgery is more effective than medicinal intervention for addressing infertility associated with endometriosis.
During fertility treatment, the ultralong pretreatment with GnRH-agonist has a higher chance of resulting in pregnancy for individuals with endometriosis, compared to the short pretreatment.[109]
Research
Preliminary research on mouse models showed that monoclonal antibodies, as well as inhibitors of MyD88 downstream signaling pathway, can reduce lesion volume. Thanks to that, clinical trials are being done on using a monoclonal antibody directed against IL-33 and using anakinra, an IL-1 receptor antagonist.[161]
Promising preclinical outcomes is pushing clinical trials into testing cannabinoid extracts, dichloroacetic acid and curcuma capsules.[161]
Epidemiology
Determining how many people have endometriosis is challenging because definitive diagnosis requires surgical visualization through laparoscopic surgery.[167] Criteria that are commonly used to establish a diagnosis include pelvic pain, infertility, surgical assessment, and in some cases, magnetic resonance imaging. An ultrasound can identify large clumps of tissue as potential endometriosis lesions and ovarian cysts but it is not effective for all patients, especially in cases with smaller, superficial lesions.[168]
Ethnic differences in endometriosis have been observed. The condition is more common in women of East Asian and Southeast Asian descent than in White women.[13] Risk factors include having a family history of the condition.[14]
One estimate is that 10.8 million people are affected globally as of 2015[update].[5] Other sources estimate 6 to 10% of the general female population[1] and 2 to 11% of asymptomatic women[13] are affected. In addition, 11% of women in a general population have undiagnosed endometriosis that can be seen on magnetic resonance imaging (MRI).[169][167] Endometriosis is most common in those in their thirties and forties; however, it can begin in girls as early as eight years old.[2][3] It results in few deaths with unadjusted and age-standardized death rates of 0.1 and 0.0 per 100,000.[5] Endometriosis was first determined to be a separate condition in the 1920s.[170] Before that time, endometriosis and adenomyosis were considered together.[170] It is unclear who first described the disease.
It chiefly affects adults from premenarche to postmenopause, regardless of race or ethnicity or whether or not they have had children and is estimated to affect over 190 million women in their reproductive years.[171] Incidences of endometriosis have occurred in postmenopausal individuals,[172] and in less common cases, individuals may have had endometriosis symptoms before they even reach menarche.[173][75]
The rate of recurrence of endometriosis is estimated to be 40-50% for adults over a 5-year period.[174] The rate of recurrence has been shown to increase with time from surgery and is not associated with the stage of the disease, initial site, surgical method used, or post-surgical treatment.[174]
History
Endometriosis was first discovered microscopically by
Hippocratic doctors believed that delaying childbearing could trigger diseases of the uterus, which caused endometriosis-like symptoms. Women with dysmenorrhea were encouraged to marry and have children at a young age.[176] The fact that Hippocratics were recommending changes in marriage practices due to an endometriosis-like illness implies that this disease was likely common, with rates higher than the 5-15% prevalence that is often cited today.[176] If indeed this disorder was so common historically, this may point away from modern theories that suggest links between endometriosis and dioxins, PCBs, and chemicals.[176]
The early treatment of endometriosis was
Society and culture
Public figures
A number of public figures have spoken about their experience with endometriosis, including:
- RuthAnne[183]
- Emma Barnett[184]
- Emma Bunton[185]
- Alexa Chung[186]
- Danielle Collins[187]
- Olivia Culpo[188]
- Lena Dunham[189]
- Abby Finkenauer[190]
- Bethenny Frankel[191]
- Whoopi Goldberg[192]
- Mel Greig[193]
- Halsey[194]
- Emma Hayes[195]
- Julianne Hough[196][197][198]
- Bridget Hustwaite[199]
- Bindi Irwin[200]
- Jaime King[201]
- Padma Lakshmi[202]
- Cyndi Lauper[203]
- Jillian Michaels[204]
- Monica[205]
- Marilyn Monroe[206]
- Tia Mowry[207]
- Sinéad O'Connor[208]
Economic burden
The economic burden of endometriosis is widespread and multifaceted.[224] Endometriosis is a chronic disease that has direct and indirect costs which include loss of work days, direct costs of treatment, symptom management, and treatment of other associated conditions such as depression or chronic pain.[224] One factor which seems to be associated with especially high costs is the delay between onset of symptoms and diagnosis.
Costs vary greatly between countries.[225] Two factors that contribute to the economic burden include healthcare costs and losses in productivity. A Swedish study of 400 endometriosis patients found "Absence from work was reported by 32% of the women, while 36% reported reduced time at work because of endometriosis".[226] An additional cross sectional study with Puerto Rican women, "found that endometriosis-related and coexisting symptoms disrupted all aspects of women's daily lives, including physical limitations that affected doing household chores and paid employment. The majority of women (85%) experienced a decrease in the quality of their work; 20% reported being unable to work because of pain, and over two-thirds of the sample continued to work despite their pain."[227]
Medical culture
There are a number of barriers that those affected face to receiving diagnosis and treatment for endometriosis. Some of these include outdated standards for laparoscopic evaluation, stigma about discussing menstruation and sex, lack of understanding of the disease, primary-care physicians' lack of knowledge, and assumptions about typical menstrual pain.[228] On average, those later diagnosed with endometriosis waited 2.3 years after the onset of symptoms before seeking treatment and nearly three quarters of women receive a misdiagnosis prior to endometriosis.[229] Self-help groups say practitioners delay making the diagnosis, often because they do not consider it a possibility. There is a typical delay of 7–12 years from symptom onset in affected individuals to professional diagnosis.[230] There is a general lack of knowledge about endometriosis among primary care physicians. Half of general health care providers surveyed in a 2013 study were unable to name three symptoms of endometriosis.[231] Health care providers are also likely to dismiss described symptoms as normal menstruation.[232] Younger patients may also feel uncomfortable discussing symptoms with a physician.[232]
Race and ethnicity
Race and ethnicity may play a role in how endometriosis affects one's life. Endometriosis is less thoroughly studied among Black people, and the research that has been done is outdated.[233] Black people with endometriosis may face barriers in receiving care due to racist misconceptions about how Black people feel pain.[234] Since pain is the primary symptom of endometriosis, this makes it increasingly possible for doctors to dismiss pain symptoms when their patient is Black.[234]
Cultural differences among ethnic groups also contribute to attitudes toward and treatment of endometriosis, especially in Hispanic or Latino communities. A study done in Puerto Rico in 2020 found that health care and interactions with friends and family related to discussing endometriosis were affected by stigma.[235] The most common finding was a referral to those expressing pain related to endometriosis as "changuería" or "changas", terms used in Puerto Rico to describe pointless whining and complaining, often directed at children.[235]
Stigma
The existing stigma surrounding women's health, specifically endometriosis, can lead to patients not seeking diagnoses, lower quality of healthcare, increased barriers to care and treatment, and negative reception from members of society.[236] Additionally, it is crucial to note that menstrual stigma significantly contributes to the broader issue of endometriosis stigma, creating an interconnected challenge that extends beyond reproductive health.[237][238] Widespread
See also
- Endometriosis Foundation of America
- Endometriosis Society of India
- MIT Center for Gynepathology Research
References
- ^ PMID 20574791.
- ^ a b c d e f g h i j k l m n o p q r s "Endometriosis". Office on Women's Health. 13 February 2017. Archived from the original on 13 May 2017. Retrieved 20 May 2017.
- ^ ISBN 978-0-19-964265-6. Archivedfrom the original on 10 September 2017.
- PMID 29276652.
- ^ PMID 27733282.
- PMID 27733281.
- ^ "Endometriosis: Overview". nichd.nih.gov. Archived from the original on 18 May 2017. Retrieved 20 May 2017.
- ^ "Endometriosis: Condition Information". nichd.nih.gov. Archived from the original on 30 April 2017. Retrieved 20 May 2017.
- ^ "Endometriosis Is More Than Just 'Painful Periods'". Yale Medicine. Retrieved 12 October 2023.
- S2CID 29998004.
- ^ PMID 23884896.
- PMID 21718982.
- ^ S2CID 214644045.
- ^ PMID 37676242. "Compared with Caucasian women, Asian women are more likely to be diagnosed with endometriosis (odds ratio (OR) 1.63, 95% CI 1.03–2.58) (14). Filipinos, Indians, Japanese, and Koreans are among the top Asian ethnicities who are more likely to have endometriosis than Caucasian women (17)."
- PMID 32316608.
These mechanisms might act in unison to cause endometriosis, but the main trophic factor in endometriosis is estrogen and estrogen exposure plays a crucial role in the development of the disease via estrogen receptors (ERs) [1].
- ^ PMID 3110710.
- ^ PMID 20573927.
- S2CID 237422801.
- ^ PMID 21106492.
- S2CID 19463907.
- ^ PMID 31699129..
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License - ^ a b c "What are the symptoms of endometriosis?". National Institutes of Health. Retrieved 4 October 2018.
- PMID 24610050.
- ^ PMID 19342028.
- ^ [page needed]Murray MT, Pizzorno J (2012). The Encyclopedia of Natural Medicine (3rd ed.). New York, NY: Simon and Schuster.
- PMID 21054165.
- ^ "Treatment of infertility in women with endometriosis". uptodate.com. Retrieved 18 December 2017.
- PMID 25400445.
- PMID 18833741.
- PMID 22361336.
- PMID 15894210.
- PMID 21925719.
- PMID 24331768.
- S2CID 52902719.
- S2CID 209896867.
- PMID 11402601.
- PMID 19356751.
- PMID 25337402.
- ^ PMID 32642009.
- S2CID 28699291.
- ^ a b Saraswat L (2015). "ESHRE2015: Endometriosis associated with a greater risk of complications in pregnancy". endometriosis.org. European Society of Human Reproduction and Embryology. Retrieved 14 February 2024.
- PMID 35570746.
- ^ PMID 28181672.
- PMID 33202017.
- S2CID 228834273.
- PMID 23078813.
- PMID 8463987.
- ^ PMID 21896560.
- PMID 15157639.
- ^ Kapoor D, Davila W (2005). Endometriosis, Archived 11 November 2007 at the Wayback Machine eMedicine.
- S2CID 208788714.
- PMID 31683028.
- PMID 30988702.
- PMID 24676469.
- ^ "MUC16 mucin 16, cell surface associated [Homo sapiens (human)] - Gene - NCBI". ncbi.nlm.nih.gov. Retrieved 13 November 2018.
- ^ "FN1 fibronectin 1 [Homo sapiens (human)] - Gene - NCBI". ncbi.nlm.nih.gov. Retrieved 13 November 2018.
- PMID 28537267.
- ^ "GeneCards®: The Human Gene Database". www.genecards.org. Weizmann Institute of Science. Retrieved 7 February 2024.
- PMID 20022587.[permanent dead link]
- PMID 22728052.
- S2CID 12813384.
- S2CID 29701466.
- PMID 19744969.
- ^ PMID 36982431.
- ^ PMID 33278007.
- ^ PMID 34073257.
- PMID 29692669.
- ^ PMID 9147102.
- ^ PMID 26375413.
- S2CID 29718095.
- PMID 32787880.
- PMID 445352.
- ^ PMID 19358700.
- PMID 19589710.
- ^ PMID 15749511.
- PMID 3559727.
- PMID 14493132.
- S2CID 35601442.
- ^ PMID 23720497.
- PMID 12372441.
- PMID 19969738.
- ^ .
- PMID 18394613.
- PMID 26439741.
- PMID 26125255.
- from the original on 6 June 2011. Retrieved 26 July 2011.
- PMID 21586449.
- PMID 24859987.
- PMID 26962803.
- S2CID 208788714.
- ^ PMID 29057034.
- ^ PMID 23762683.
- PMID 3574800.
- ^ S2CID 3759091.
- S2CID 7362461.
- PMID 160025.
- PMID 8356497.
- PMID 31618674.
- ^ PMID 9130884.
- ^ PMID 17550672.
- PMID 32855690.
- ^ PMID 26919512.
- S2CID 201838966.
- ^ "Reclassifying endometriosis as a syndrome would benefit patient care - The BMJ". 11 August 2020. Retrieved 17 August 2020.
- ^ PMID 23528916.
- ^ PMID 20436318.
- PMID 2351237.
- PMID 24630080.
- ^ a b c d e f "Endometriosis – Diagnosis, treatment and patient experiences". Swedish Agency for Health Technology Assessment and Assessment of Social Services (SBU). 4 May 2018. Retrieved 13 June 2018.
- ^ .
- ^ PMID 32706984.
- PMID 16936305.
- ^ PMID 20462942.
- ^ S2CID 22744182.
- PMID 21672902.
- PMID 27094925.
- PMID 32082539.
- ^ Aurelia Busca, Carlos Parra-Herran. "Ovary - nontumor - Nonneoplastic cysts / other - Endometriosis". Pathology Outlines. Topic Completed: 1 August 2017. Revised: 5 March 2020
- ^ McMaster-Fay R, Osborn R, Chandraratnam E. The Clinical Utility Of CD10 Immunohistochemical Staining In The Diagnosis Of Endometriosis (PDF). 10th World Congress of Endometriosis. Melbourne, Australia. Archived (PDF) from the original on 2 May 2013. Retrieved 18 July 2013.
- PMID 25180023.
- ^ "Endometriosis". www.who.int. Retrieved 24 November 2023.
- ^ "What are the treatments for endometriosis". Eunice Kennedy Shriver National Institute of Child Health and Human Development. Archived from the original on 3 August 2013. Retrieved 20 August 2013.
- PMID 20627430.
- ^ from the original on 29 October 2013.
- ^ "Update on pharmacologic treatment for endometriosis- related pain". Women's Healthcare. 7 June 2020. Retrieved 3 October 2021.
- PMID 33095458.
- ^ S2CID 13050344.
- ISBN 0-683-30379-1.
- ^ "Endometriosis and Infertility: Can Surgery Help?" (PDF). American Society for Reproductive Medicine. 2008. Archived (PDF) from the original on 11 October 2010. Retrieved 31 October 2010.
- ^ "UNC Center for Endometriosis". UNC Department of Obstetrics & Gynecology. Archived from the original on 14 July 2021. Retrieved 14 July 2021.
- PMID 28456617.
- ^ Andrea Muraskin (16 July 2023). "Endometriosis, a painful and often overlooked disease, gets attention in a new film". NPR.
- PMID 24435778.
- ^ Brunes, M, Altman, D, Pålsson, M, Söderberg, MW, Ek, M. Impact of hysterectomy on analgesic, psychoactive and neuroactive drug use in women with endometriosis: nationwide cohort study. BJOG 2021; 128: 846– 855. [1]
- PMID 24592083.
- PMID 19279046.
- PMID 29180308.
- S2CID 30816909.
- .
- PMID 11821616.
- S2CID 23340983.
- PMID 29786828.
- PMID 25406186.
- ^ "DANOCRINE : Brand of DANAZOL CAPSULES, USP" (PDF). Accessdata.fda.gov. Retrieved 3 March 2022.
- ^ PMID 33687160.
- ^ PMID 21154398.
- PMID 16647373.
- PMID 27095958.
- S2CID 225058751.
- PMID 28742263.
- S2CID 39113105.
- PMID 22592712.
- PMID 32104332.
- S2CID 89694879.
- ^ PMID 22718320.
- PMID 23485944.
- S2CID 10052884.
- S2CID 237294362.
- PMID 20567196.
- PMID 28114727.
- ^ S2CID 235226513.
- PMID 21589790.
- S2CID 219173190.
- ^ a b c d "Endometrios – diagnostik, behandling och bemötande". sbu.se (in Swedish). Statens beredning för medicinsk och social utvärdering (SBU); Swedish Agency for Health Technology Assessment and Assessment of Social Services. 4 May 2018. p. 121. Retrieved 13 June 2018.
- ^ from the original on 29 October 2013.
- PMID 33206374.
- ^ S2CID 51679656.
- ^ "Endometriosis Ultrasound: Procedure, Diagnosis, & Follow Up". Cleveland Clinic. Retrieved 7 March 2022.
- PMID 21719000.
- ^ ISBN 978-1-4443-9849-6.
- PMID 21693036.
- S2CID 25628258.
- PMID 14642954.
- ^ PMID 19279046.
- ISBN 978-0-85729-585-9.
- ^ PMID 23084567.
- PMID 17857917.
- ^ Barbieri RL (January 1992). "Hormonal therapy of endometriosis". Infertility and Reproductive Medicine Clinics of North America. 3 (1): 187–200.
The hormonal therapy of endometriosis continues to evolve. In the 1940s and 1950s, high-dose testosterone and diethylstilbestrol regimens were the only hormonal agents available in the treatment of endometriosis. These agents, although efficacious, were associated with intolerable side effects. The current armamentarium of hormonal agents-the GnRH analogues, danazol, and the synthetic progestins-is efficacious and has fewer side effects.
- ^ ISBN 978-1-4613-8265-2.
- ^ ISBN 978-1-4613-2157-6.
- ^ ISBN 978-0-8151-7479-0.
- S2CID 73455399.
- ^ Gallagher K (31 March 2021). "Irish songwriter Ruth Anne opens up on her debilitating fight with endometriosis". Irish Mirror. Retrieved 11 April 2023.
- TheGuardian.com. 22 October 2020.
- Her.ie. Retrieved 28 May 2021.
- ^ "Alexa Chung Reveals Her Battle With Endometriosis—And Taps Into an Empowering Online Community". Vogue. 18 July 2019. Retrieved 11 April 2023.
- ^ "Champions Corner: Collins unleashes the best tennis of her career after life-changing surgery". Women's Tennis Association. Retrieved 3 March 2022.
- ^ "Watch: Olivia Culpo Shares Emotional Details of Her Endometriosis Journey". Sports Illustrated.
- ^ "Lena Dunham Gives Health Update Following Battle with Endometriosis". People. Retrieved 11 April 2023.
- ^ "Congresswoman Abby Finkenauer Opens Up About Her Struggle With Endometriosis". Glamour. 5 March 2020. Retrieved 17 December 2021.
- ^ "EXCLUSIVE: Bethenny Frankel in Tears Over Recent Health Scare: 'I Really Tried to Hold It All Together'". Entertainment Tonight. 22 June 2016. Retrieved 11 April 2023.
- ^ "Blossom Ball 2009 – Whoopi Goldberg". Endometriosis Foundation of America. 27 November 2007. Retrieved 21 January 2021.
- ^ "Radio presenter Mel Greig's shocking photo shows reality of living with endometriosis". News.com.au. 28 March 2018. Retrieved 21 January 2021.
- ^ Iasimone, Ashley (7 January 2017). "Halsey undergoes surgery to treat endometriosis". Billboard. Retrieved 27 November 2018.
- ^ "Emma Hayes: Chelsea manager has emergency hysterectomy because of endometriosis". BBC Sport. BBC. 13 October 2022. Retrieved 28 December 2022.
- ^ Murray, Rheana (9 September 2017). "Julianne Hough opens up about endometriosis: 'I just thought it was normal'". Today. Retrieved 21 January 2021.
- ^ "Julianne Hough Won't Let Endometriosis Stop Her From Having a Family With Brooks Laich: "We've Discussed Options"". Endometriosis : Causes - Symptoms - Diagnosis - and Treatment. 23 April 2018. Retrieved 31 December 2023.
- ^ Olya G (24 March 2017). "Julianne Hough Opens Up About Her Struggle with Endometriosis". Peoplemag. Retrieved 31 December 2023.
- ^ Hustwaite, Bridget (14 August 2018). "Endometriosis: The pain sucks, but so does just getting a diagnosis". Hack on Triple J. Retrieved 21 January 2021.
- ^ Dye J (8 March 2023). "On International Women's Day, Bindi Irwin reveals 10-year struggle with endometriosis". Australian Broadcasting Corporation News. Retrieved 10 March 2023.
- ^ "Why Jaime King Decided It Was Time to Talk About Her Years-Long Fertility Struggle". E! Online. 24 April 2022. Retrieved 11 April 2023.
- ^ "Padma Lakshmi shares her struggle with endometriosis". Redbook. 17 October 2011. Archived from the original on 2 November 2020. Retrieved 9 March 2021 – via YouTube.
- ISSN 0362-4331. Retrieved 11 April 2023.
- ^ "No Kidding: Jillian Michaels is Not "Doing That" to Her Body". Bitch Media. 7 February 2011. Archived from the original on 11 April 2023. Retrieved 11 April 2023.
- ^ "Monica's Second Surgery For Her Endometriosis Was 'Very Hard' And She 'Ended Up Having Multiple Blood Transfusions'". MadameNoire. 9 June 2021. Retrieved 11 April 2023.
- ^ Wilson-Beevers H (28 September 2022). "Marilyn Monroe's battle with endometriosis is often ignored – but it's a vital part of her story". Cosmopolitan. Retrieved 11 April 2023.
- ^ Henderson W (14 June 2017). "Tia Mowry Releases a Cookbook for Women With Endometrosis". Endometriosis News. Retrieved 11 April 2023.
- ^ Devereux, Niamh (19 August 2015). "Sinead O'Connor tells of illness hell: "I'm in a bad way"". Retrieved 5 August 2023.
- ^ Vargas A. "12 celebrities who have opened up about having endometriosis". Insider. Retrieved 6 August 2021.
- ^ Scott, Ellen (12 June 2016). "Daisy Ridley opened up about her struggle with endometriosis". Cosmopolitan. Retrieved 29 June 2021.
- ^ Nast, Condé (11 November 2020). "Emma Roberts shares how her undiagnosed endometriosis affected her pregnancy journey". Self. Retrieved 15 July 2021.
- ^ endometriosis.org. "EFA2011: Susan Sarandon speaks up about endometriosis – Endometriosis.org". Retrieved 11 April 2023.
- ^ "Amy Schumer 'feeling good' after endometriosis surgery and liposuction". The Independent Tribune. 20 January 2022. Retrieved 11 April 2023.
- ^ "'General Hospital': Kirsten Storms opens up about return – The TV Guy – Orlando Sentinel". 25 December 2012. Archived from the original on 25 December 2012. Retrieved 18 October 2021.
- ^ Haller S. "Gabrielle Union says she probably can't get pregnant because of adenomyosis. What exactly is that?". USA Today. Retrieved 11 April 2023.
- ^ Writer S. "Another victim of the 'Dancing With The Stars' curse". The Columbus Dispatch. Retrieved 31 December 2023.
- ^ Richenthal M (30 October 2008). "Lacey Schwimmer is Also Sick". TV Fanatic. Retrieved 31 December 2023.
- ^ "Lena Dunham, Julianne Hough and More Who've Opened Up About Endometriosis Battles: "You Don't Have to Ignore Pain"". E! Online. 23 March 2017. Retrieved 31 December 2023.
- ^ Mazziotta, Julie (5 February 2021). "Chrissy Teigen says endometriosis surgery was 'a toughie' but better than 'the pain of endo'". People. Retrieved 15 July 2021.
- PerthNow. 16 March 2019. Retrieved 21 January 2021.
- ^ "Mae Whitman: 'Endometriosis Is Like Being Shot With a Cannonball in the Stomach'". Glamour. 21 May 2020. Retrieved 11 April 2023.
- ^ "Jessica Williams on the 'Debilitating' Symptom That Led to Her Endometriosis Diagnosis". Self. 12 April 2022. Retrieved 11 April 2023.
- ^ Dervish-O'Kane R (27 December 2022). "Leah Williamson, captain of the Lionesses, is our January cover star". Women's Health. Hearst UK. Retrieved 28 December 2022.
- ^ S2CID 20623034.
- S2CID 32839234.
- S2CID 214811610.
- PMID 28650252.
- S2CID 73480251.
- PMID 22990516.
- ISSN 1701-2163.
- PMID 22521982.
- ^ PMID 12660267.
- S2CID 6288739.
- ^ PMID 27044069.
- ^ S2CID 221862356.
- PMID 34360501.
- PMID 37654520.
- ^ Henry JE (27 May 2022). "Period Stigma and the Unacknowledged System of Oppression". Stanford | Digital Education. Retrieved 24 November 2023.
- PMID 34360501.
This article incorporates text in the public domain as a Swedish government "utterance" by URL§9
External links
- Endometriosis at Curlie
- Endometriosis fact sheet from the World Health Organization