Caesarean section
| Caesarean section | |
|---|---|
 A team of five performing a caesarean section[1] | |
| Other names | C-section, caesarean section, caesarean delivery |
| Specialty | Obstetrics, gynaecology, surgery, neonatology, pediatrics, family medicine |
| ICD-10-PCS | 10D00Z0 |
| ICD-9-CM | 74 |
| MeSH | D002585 |
| MedlinePlus | 002911 |
Caesarean section, also known as C-section or caesarean delivery, is the
A C-section typically takes 45 minutes to an hour.
C-sections result in a small overall increase in poor outcomes in low-risk pregnancies.
In 2012, about 23 million C-sections were done globally.
Uses
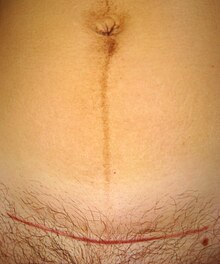
Caesarean section (C-section) is recommended when vaginal delivery might pose a risk to the mother or baby. C-sections are also carried out for personal and social reasons on maternal request in some countries.
Medical uses
Complications of labor and factors increasing the risk associated with vaginal delivery include:
- Abnormal presentation (breech or transverse positions)
- Prolonged labor or a failure to progress (obstructed labour, also known as dystocia)
- Fetal distress
- Cord prolapse
- Uterine rupture or an elevated risk thereof
- Uncontrolled hypertension, pre-eclampsia,[16] or eclampsia in the mother
- Tachycardia in the mother or baby after amniotic rupture (the waters breaking)
- placenta accreta)
- Failed labor induction
- Failed instrumental delivery (by ventouse(Sometimes, a trial of forceps/ventouse delivery is attempted, and if unsuccessful, the baby will need to be delivered by caesarean section.)
- Large baby weighing > 4,000 grams (macrosomia)
- Umbilical cord abnormalities (velamentous insertion)
Other complications of pregnancy, pre-existing conditions, and concomitant disease, include:
- Previous (high risk) fetus
- HIV infection of the mother with a high viral load (HIV with a low maternal viral load is not necessarily an indication for caesarean section)
- An outbreak of genital herpes in the third trimester[17] (which can cause infection in the baby if born vaginally)
- Previous classical (longitudinal) caesarean section
- Previous uterine rupture
- Prior problems with the healing of the perineum (from previous childbirth or Crohn's disease)
- Bicornuate uterus
- Rare cases of posthumous birth after the death of the mother
Other
- Decreasing experience of accoucheurs with the management of breech presentation. Although obstetricians and midwives are extensively trained in proper procedures for breech presentation deliveries using simulation mannequins, there is decreasing experience with actual vaginal breech delivery, which may increase the risk.[18]
Prevention
The prevalence of caesarean section is generally agreed to be higher than needed in many countries, and physicians are encouraged to actively lower the rate, as a caesarean rate higher than 10–15% is not associated with reductions in maternal or infant mortality rates,[4] although some evidence support that a higher rate of 19% may result in better outcomes.[8]
Some of these efforts are: emphasizing a long
Risks
Adverse outcomes in low-risk pregnancies occur in 8.6% of vaginal deliveries and 9.2% of caesarean section deliveries.[3]
Mother
In those who are low risk, the risk of death for caesarean sections is 13 per 100,000 vs. for vaginal birth 3.5 per 100,000 in the developed world.[3] The United Kingdom National Health Service gives the risk of death for the mother as three times that of a vaginal birth.[21]
In Canada, the difference in serious morbidity or mortality for the mother (e.g. cardiac arrest, wound hematoma, or hysterectomy) was 1.8 additional cases per 100.[22] The difference in in-hospital maternal death was not significant.[22]
A caesarean section is associated with risks of postoperative
Wound infections occur after caesarean sections at a rate of 3–15%.[25] The presence of chorioamnionitis and obesity predisposes the woman to develop a surgical site infection.[25]
Women who had caesarean sections are more likely to have problems with later pregnancies, and women who want larger families should not seek an elective caesarean unless medical indications to do so exist. The risk of
Mothers can experience an increased incidence of
Subsequent pregnancies
Women who have had a caesarean for any reason are somewhat less likely to become pregnant again as compared to women who have previously delivered only vaginally.[28]
Women who had just one previous caesarean section are more likely to have problems with their second birth.[3] Delivery after previous caesarean section is by either of two main options:[29]
- Vaginal birth after caesarean section (VBAC)
- Elective repeat caesarean section (ERCS)
Both have higher risks than a vaginal birth with no previous caesarean section. A vaginal birth after caesarean section (VBAC) confers a higher risk of
Adhesions
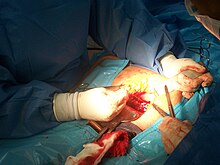
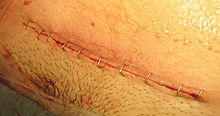
There are several steps that can be taken during abdominal or pelvic surgery to minimize postoperative complications, such as the formation of
- Handling all tissue with absolute care
- Using powder-free surgical gloves
- Controlling bleeding
- Choosing sutures and implants carefully
- Keeping tissue moist
- Preventing infection with antibiotics given intravenously to the mother before skin incision
Despite these proactive measures, adhesion formation is a recognized complication of any abdominal or pelvic surgery. To prevent adhesions from forming after caesarean section, adhesion barrier can be placed during surgery to minimize the risk of adhesions between the uterus and ovaries, the small bowel, and almost any tissue in the abdomen or pelvis. This is not current UK practice, as there is no compelling evidence to support the benefit of this intervention.
Adhesions can cause long-term problems, such as:
- Infertility, which may end when adhesions distort the tissues of the ovaries and tubes, impeding the normal passage of the egg (ovum) from the ovary to the uterus. One in five infertility cases may be adhesion related (stoval)
- Chronic pelvic pain, which may result when adhesions are present in the pelvis. Almost 50% of chronic pelvic pain cases are estimated to be adhesion related (stoval)
- Small bowel obstruction: the disruption of normal bowel flow, which can result when adhesions twist or pull the small bowel.
The risk of adhesion formation is one reason why vaginal delivery is usually considered safer than elective caesarean section where there is no medical indication for section for either maternal or fetal reasons.
Child
Non-medically indicated (elective) childbirth before 39 weeks gestation "carry significant risks for the baby with no known benefit to the mother." Newborn mortality at 37 weeks may be up to 3 times the number at 40 weeks, and is elevated compared to 38 weeks gestation. These early term births were associated with more death during infancy, compared to those occurring at 39 to 41 weeks (full term).[34] Researchers in one study and another review found many benefits to going full term, but no adverse effects in the health of the mothers or babies.[34][35]
The
For otherwise healthy twin pregnancies where both twins are head down a trial of vaginal delivery is recommended at between 37 and 38 weeks.[36][37] Vaginal delivery, in this case, does not worsen the outcome for either infant as compared with caesarean section.[37] There is some controversy on the best method of delivery where the first twin is head first and the second is not, but most obstetricians will recommend normal delivery unless there are other reasons to avoid vaginal birth.[37] When the first twin is not head down, a caesarean section is often recommended.[37] Regardless of whether the twins are delivered by section or vaginally, the medical literature recommends delivery of dichorionic twins at 38 weeks, and monochorionic twins (identical twins sharing a placenta) by 37 weeks due to the increased risk of stillbirth in monochorionic twins who remain in utero after 37 weeks.[38][39] The consensus is that late preterm delivery of monochorionic twins is justified because the risk of stillbirth for post-37-week delivery is significantly higher than the risks posed by delivering monochorionic twins near term (i.e., 36–37 weeks).[40] The consensus concerning monoamniotic twins (identical twins sharing an amniotic sac), the highest risk type of twins, is that they should be delivered by caesarean section at or shortly after 32 weeks, since the risks of intrauterine death of one or both twins is higher after this gestation than the risk of complications of prematurity.[41][42][43]
In a research study widely publicized, singleton children born earlier than 39 weeks may have developmental problems, including slower learning in reading and math.[44]
Other risks include:
- Wet lung (Transient Tachypnea of the Newborn): Failure to pass through the birth canal does not expose the baby to cortisol and epinephrine which typically would reverse the potassium/sodium pumps in the baby's lung. This causes fluid to remain in the lung.[45]
- Potential for early delivery and complications: Preterm delivery may be inadvertently carried out if the due-date calculation is inaccurate. One study found an increased complication risk if a repeat elective caesarean section is performed even a few days before the recommended 39 weeks.[46]
- Higher infant mortality risk: In caesarean sections performed with no indicated medical risk (singleton at full term in a head-down position with no other obstetric or medical complications), the risk of death in the first 28 days of life has been cited as 1.77 per 1,000 live births among women who had caesarean sections, compared to 0.62 per 1,000 for women who delivered vaginally.[47]
Birth by caesarean section also seems to be associated with worse health outcomes later in life, including overweight or obesity, problems in the immune system, and poor digestive system.[48][49] However, caesarean deliveries are found to not affect a newborn's risk of developing food allergy.[50] This finding contradicts a previous study that claims babies born via caesarean section have lower levels of Bacteroides that is linked to peanut allergy in infants.[51]
Classification
Caesarean sections have been classified in various ways by different perspectives.[52] One way to discuss all classification systems is to group them by their focus either on the urgency of the procedure (most common), characteristics of the mother, or as a group based on other, less commonly discussed factors.[52]
By urgency
Conventionally, caesarean sections are classified as being either an
A planned caesarean (or elective/scheduled caesarean), arranged ahead of time, is most commonly arranged for medical indications which have developed before or during the pregnancy, and ideally after 39 weeks of gestation. In the UK, this is classified as a 'grade 4' section (delivery timed to suit the mother or hospital staff) or as a 'grade 3' section (no maternal or fetal compromise but early delivery needed). Emergency caesarean sections are performed in pregnancies in which a vaginal delivery was planned initially, but an indication for caesarean delivery has since developed. In the UK they are further classified as grade 2 (delivery required within 90 minutes of the decision but no immediate threat to the life of the woman or the fetus) or grade 1 (delivery required within 30 minutes of the decision: immediate threat to the life of the mother or the baby or both.)[54]
Elective caesarean sections may be performed on the basis of an obstetrical or medical indication, or because of a medically non-indicated
By characteristics of the mother
Caesarean delivery on maternal request
Caesarean delivery on maternal request (CDMR) is a medically unnecessary caesarean section, where the conduct of a
After previous caesarean
Mothers who have previously had a caesarean section are more likely to have a caesarean section for future pregnancies than mothers who have never had a caesarean section. There is discussion about the circumstances under which women should have a vaginal birth after a previous caesarean.
Vaginal birth after caesarean (VBAC) is the practice of
Twins
For otherwise healthy twin pregnancies where both twins are head down a trial of vaginal delivery is recommended at between 37 and 38 weeks.[36][37] Vaginal delivery in this case does not worsen the outcome for either infant as compared with caesarean section.[37] There is controversy on the best method of delivery where the first twin is head first and the second is not.[37] When the first twin is not head down at the point of labor starting, a caesarean section should be recommended.[37] Although the second twin typically has a higher frequency of problems, it is not known if a planned caesarean section affects this.[36] It is estimated that 75% of twin pregnancies in the United States were delivered by caesarean section in 2008.[68]
Breech birth
A breech birth is the birth of a baby from a breech presentation, in which the baby exits the pelvis with the buttocks or feet first as opposed to the normal head-first presentation. In breech presentation, fetal heart sounds are heard just above the umbilicus.
Babies are usually born head first. If the baby is in another position the birth may be complicated. In a 'breech presentation', the unborn baby is bottom-down instead of head-down. Babies born bottom-first are more likely to be harmed during a normal (vaginal) birth than those born head-first. For instance, the baby might not get enough oxygen during the birth. Having a planned caesarean may reduce these problems. A review looking at planned caesarean section for singleton breech presentation with planned vaginal birth, concludes that in the short term, births with a planned caesarean were safer for babies than vaginal births. Fewer babies died or were seriously hurt when they were born by caesarean. There was tentative evidence that children who were born by caesarean had more health problems at age two. Caesareans caused some short-term problems for mothers such as more abdominal pain. They also had some benefits, such as less urinary incontinence and less perineal pain.[69]
The bottom-down position presents some hazards to the baby during the process of birth, and the mode of delivery (vaginal versus caesarean) is controversial in the fields of obstetrics and midwifery.
Though vaginal birth is possible for the breech baby, certain fetal and maternal factors influence the safety of vaginal breech birth. The majority of breech babies born in the United States and the UK are delivered by caesarean section as studies have shown increased risks of morbidity and mortality for vaginal breech delivery, and most obstetricians counsel against planned vaginal breech birth for this reason. As a result of reduced numbers of actual vaginal breech deliveries, obstetricians and midwives are at risk of de-skilling in this important skill. All those involved in delivery of obstetric and midwifery care in the UK undergo mandatory training in conducting breech deliveries in the simulation environment (using dummy pelvises and mannequins to allow practice of this important skill) and this training is carried out regularly to keep skills up to date.
Resuscitative hysterotomy
A resuscitative hysterotomy, also known as a peri-mortem caesarean delivery, is an emergency caesarean delivery carried out where maternal cardiac arrest has occurred, to assist in resuscitation of the mother by removing the aortocaval compression generated by the gravid uterus. Unlike other forms of caesarean section, the welfare of the fetus is a secondary priority only, and the procedure may be performed even prior to the limit of fetal viability if it is judged to be of benefit to the mother.
Other ways, including the surgery technique
There are several types of caesarean section (CS). An important distinction lies in the type of incision (longitudinal or transverse) made on the uterus, apart from the incision on the skin: the vast majority of skin incisions are a transverse suprapubic approach known as a Pfannenstiel incision but there is no way of knowing from the skin scar which way the uterine incision was conducted.
- The classical caesarean section involves a longitudinal midline incision on the uterus which allows a larger space to deliver the baby. It is performed at very early gestations where the lower segment of the uterus is unformed as it is safer in this situation for the baby: but it is rarely performed other than at these early gestations, as the operation is more prone to complications than a low transverse uterine incision. Any woman who has had a classical section will be recommended to have an elective repeat section in subsequent pregnancies as the vertical incision is much more likely to rupture in labor than the transverse incision.
- The bladder. It results in less blood lossand has fewer early and late complications for the mother, as well as allowing her to consider a vaginal birth in the next pregnancy.
- A caesarean hysterectomy consists of a caesarean section followed by the removal of the uterus. This may be done in cases of intractable bleeding or when the placenta cannot be separated from the uterus.
The EXIT procedure is a specialized surgical delivery procedure used to deliver babies who have airway compression.
The Misgav Ladach method is a modified caesarean section which has been used nearly all over the world since the 1990s. It was described by Michael Stark, the president of the New European Surgical Academy, at the time he was the director of Misgav Ladach, a general hospital in Jerusalem. The method was presented during a FIGO conference in Montréal in 1994[70] and then distributed by the University of Uppsala, Sweden, in more than 100 countries. This method is based on minimalistic principles. He examined all steps in caesarean sections in use, analyzed them for their necessity and, if found necessary, for their optimal way of performance. For the abdominal incision he used the modified Joel Cohen incision and compared the longitudinal abdominal structures to strings on musical instruments. As blood vessels and muscles have lateral sway, it is possible to stretch rather than cut them. The peritoneum is opened by repeat stretching, no abdominal swabs are used, the uterus is closed in one layer with a big needle to reduce the amount of foreign body as much as possible, the peritoneal layers remain unsutured and the abdomen is closed with two layers only. Women undergoing this operation recover quickly and can look after the newborns soon after surgery. There are many publications showing the advantages over traditional caesarean section methods. There is also an increased risk of abruptio placentae and uterine rupture in subsequent pregnancies for women who underwent this method in prior deliveries.[71][72]
Since 2015, the World Health Organization has endorsed the Robson classification as a holistic means of comparing childbirth rates between different settings, with a view to allowing more accurate comparison of caesarean section rates.[73]
Technique
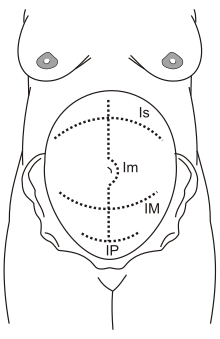
Is: supra-umbilical incision
Im: median incision
IM: Maylard incision
IP: Pfannenstiel incision
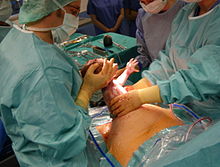
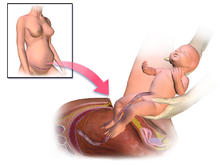
Antibiotic prophylaxis is used before an incision.[74] The uterus is incised, and this incision is extended with blunt pressure along a cephalad-caudad axis.[74] The infant is delivered, and the placenta is then removed.[74] The surgeon then makes a decision about uterine exteriorization.[74] Single-layer uterine closure is used when the mother does not want a future pregnancy.[74] When subcutaneous tissue is 2 cm thick or more, surgical suture is used.[74] Discouraged practices include manual cervical dilation, any subcutaneous drain,[75] or supplemental oxygen therapy with intent to prevent infection.[74]
Caesarean section can be performed with
Anesthesia
Both
Regional anaesthesia is used in 95% of deliveries, with spinal and combined spinal and epidural anaesthesia being the most commonly used regional techniques in scheduled caesarean section.
General anesthesia may be necessary because of specific risks to mother or child. Patients with heavy, uncontrolled bleeding may not tolerate the hemodynamic effects of regional anesthesia. General anesthesia is also preferred in very urgent cases, such as severe fetal distress, when there is no time to perform a regional anesthesia.
Prevention of complications
Postpartum infection is one of the main causes of maternal death and may account for 10% of maternal deaths globally.
Women who have caesareans can recognize the signs of fever that indicate the possibility of wound infection.
Some doctors believe that during a caesarean section, mechanical cervical dilation with a finger or forceps will prevent the obstruction of blood and lochia drainage, and thereby benefit the mother by reducing the risk of death. The evidence as of 2018[update] neither supported nor refuted this practice for reducing postoperative morbidity, pending further large studies.[91]
Skin-to-skin contact
The
It is known that during the hours of labor before a vaginal birth a woman's body begins to produce oxytocin which aids in the bonding process, and it is thought that SSC can trigger its production as well. Indeed, women have reported that they felt that SSC had helped them to feel close to and bond with their infant. A review of literature also found that immediate or early SSC increased the likelihood of successful breastfeeding and that newborns were found to cry less and relax quicker when they had SSC with their father as well.[93]
Recovery
It is common for women who undergo caesarean section to have reduced or absent bowel movements for hours to days. During this time, women may experience abdominal cramps, nausea and vomiting. This usually resolves without treatment.
There may be a somewhat higher incidence of postnatal depression in the first weeks after childbirth for women who have caesarean sections, but this difference does not persist.[36] Some women who have had caesarean sections, especially emergency caesareans, experience post-traumatic stress disorder.[36]
Those who undergoes caesarean section has 18.3% chance of chronic surgical pain at three months and 6.8% chance of surgical pain at 12 months.[99]
In recent meta-analyses, caesarean section has been associated to a lower risk of urinary incontinence and pelvic organ prolapse compared to vaginal delivery.[100][101] Women who have vaginal births, after a previous caesarean, are more than twice as likely to subsequently have pelvic floor surgery as those who have another caesarean.[102][103]
Frequency
Global rates of caesarean section are increasing.[25] It doubled from 2003 to 2018 to reach 21%, and is increasing annually by 4%. The trend towards increasing rates is particularly strong in middle and high income countries.[104]: 101 In southern Africa, the cesarean rate is less than 5%; while the rate is almost 60% in some parts of Latin America.[105] The Canadian rate was 26% in 2005–2006.[106] Australia has a high caesarean section rate, at 31% in 2007.[107] At one time a rate of 10% to 15% was thought to be ideal;[4] a rate of 19% may result in better outcomes.[8] The World Health Organization officially withdrew its previous recommendation of a 15% C-section rate in June 2010. Their official statement read, "There is no empirical evidence for an optimum percentage. What matters most is that all women who need caesarean sections receive them."[108]
More than 50 nations have rates greater than 27%. Another 45 countries have rates less than 7.5%.[8] There are efforts to both improve access to and reduce the use of C-section.[8] Globally, 1% of all caesarean deliveries are carried out without medical need. Overall, the caesarean section rate was 25.7% for 2004–2008.[109][110]
There is no significant difference in caesarean rates when comparing midwife continuity care to conventional fragmented care.[111] More emergency caesareans—about 66%—are performed during the day rather than the night.[112]
The rate has risen to 46% in
Europe
Across Europe, there are differences between countries: in Italy the caesarean section rate is 40%, while in the Nordic countries it is 14%.[116] In the United Kingdom, in 2008, the rate was 24%.[117] In Ireland the rate was 26.1% in 2009.[118]
In Italy, the incidence of caesarean sections is particularly high, although it varies from region to region.[119] In Campania, 60% of 2008 births reportedly occurred via caesarean sections.[120] In the Rome region, the mean incidence is around 44%, but can reach as high as 85% in some private clinics.[121][122]
United States
In the United States, cesarean deliveries began rising in the 1960s and started becoming routine in the 1960s and 1970s.[104]: 101
In the United States the rate of C-section is around 33%, varying from 23% to 40% depending on the state.[3] One of three women who gave birth in the US delivered by caesarean in 2011. In 2012, close to 23 million C-sections were carried out globally.[8]
With nearly 1.3 million stays, caesarean section was one of the most common procedures performed in U.S. hospitals in 2011. It was the second-most common procedure performed for people ages 18 to 44 years old.[123] Caesarean rates in the U.S. have risen considerably since 1996.[124] The rate has increased in the United States, to 33% of all births in 2012, up from 21% in 1996.[3] In 2010, the caesarean delivery rate was 32.8% of all births (a slight decrease from 2009's high of 32.9% of all births).[125] A study found that in 2011, women covered by private insurance were 11% more likely to have a caesarean section delivery than those covered by Medicaid.[126] The increase in use has not resulted in improved outcomes, resulting in the position that C-sections may be done too frequently.[3] It is believed that the high rate of induced deliveries has also led to the high rate of c-sections because they are twice as likely to lead to one.[127]
Hospitals and doctors make more money from C-section births than vaginal deliveries. Economists have calculated that hospitals may make a few thousand dollars more and doctors a few hundred. It has been found that for-profit hospitals do more c-sections than non-profit hospitals.[127] One study looked at the rate of c-sections done for women who were themselves doctors. It found that there was a 10 percent decrease to the rate of c-sections vs the general population. But if the hospital paid their doctors a flat salary removing the incentive to do the surgical procedures, which take more time, the rate of c-sections done on women who were themselves physicians exceeded that of the procedure done on non-medically knowledgeable mothers, suggesting that some women who actually needed c-sections were not getting them.[128]
Concerned over the rising number of cesarean deliveries and hospital costs, in 2009 Minnesota introduced a blended payment rate for either vaginal or cesarean uncomplicated births (i.e., a similar payment regardless of delivery mode). As a result, the prepolicy cesarean rate of 22.8% dropped 3.24 percentage points. The cost of childbirth hospitalizations in Minnesota dropped by $425.80 at the time the policy was initiated and continued to drop by $95.04 per quarter with no significant effects on maternal morbidity.[129]
The rise of cesarean births in the United States has coincided with counter-movements emphasizing natural childbirth with a lesser degree of medical intervention.[104]: 101–102
China
The rate of cesarean sections began to sharply increase in China in the 1990s.[104]: 101 This increase was driven by the expansion of China's modern hospital infrastructure, and occurred first in urban areas.[104]: 101 The rise in cesarean deliveries has also resulted in social critique of the medical establishment over the medical necessity of performing cesarean sections.[104]: 101–102
History
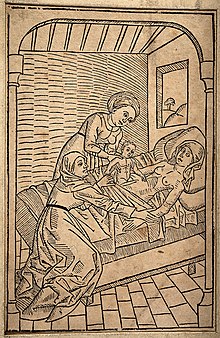
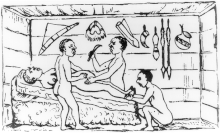
Historically, caesarean sections performed upon a live woman usually resulted in the death of the mother.[130] It was considered an extreme measure, performed only when the mother was already dead or considered to be beyond help. By way of comparison, see the resuscitative hysterotomy or perimortem caesarean section.
According to the ancient Chinese
The
An early account of caesarean section in Iran (Persia) is mentioned in the book of
In the Irish mythological text the Ulster Cycle, the character Furbaide Ferbend is said to have been born by posthumous caesarean section, after his mother was murdered by his evil aunt Medb.
The
The Spanish saint Raymond Nonnatus (1204–1240) received his surname—from the Latin non-natus ('not born')—because he was born by caesarean section. His mother died while giving birth to him.[140]
There is some indirect evidence that the first caesarean section that was survived by both the mother and child was performed in Prague in 1337.[141][142] The mother was Beatrice of Bourbon, the second wife of the King of Bohemia John of Luxembourg. Beatrice gave birth to the king's son Wenceslaus I, later the duke of Luxembourg, Brabant, and Limburg, and who became the half brother of the later King of Bohemia and Holy Roman Emperor, Charles IV.
In an account from the 1580s, Jakob Nufer, a veterinarian in Siegershausen, Switzerland, is supposed to have performed the operation on his wife after a prolonged labour, with her surviving. His wife allegedly bore five more children, including twins, and the baby delivered by caesarean section purportedly lived to the age of 77.[143][144][145]
For most of the time since the 16th century, the procedure had a high mortality rate. In Great Britain and Ireland, the mortality rate in 1865 was 85%. Key steps in reducing mortality were:
- Introduction of the transverse incision technique to minimize bleeding by Ferdinand Adolf Kehrer in 1881 is thought to be first modern CS performed.
- The introduction of uterine Max Sängerin 1882
- Modification by Hermann Johannes Pfannenstiel in 1900, see Pfannenstiel incision
- Extraperitoneal CS and then moving to low transverse incision (Krönig, 1912)[clarification needed]
- Adherence to principles of asepsis
- Anesthesia advances
- Blood transfusion
- Antibiotics
Indigenous people in the
The first successful caesarean section to be performed in the United States took place in Rockingham County, Virginia in 1794. The procedure was performed by Dr. Jesse Bennett on his wife Elizabeth.[150]
Caesarius of Terracina

The patron saint of caesarean section is Caesarius, a young deacon martyred at Terracina, who has replaced and Christianized the pagan figure of Caesar.[151] The martyr (Saint Cesareo in Italian) is invoked for the success of this surgical procedure, because it was considered the new "Christian Caesar" – as opposed to the "pagan Caesar" – in the Middle Ages it began to be invoked by pregnant women to wish a physiological birth, for the success of the expulsion of the baby from the uterus and, therefore, for their salvation and that of the unborn. The practice continues, in fact the martyr Caesarius is invoked by the future mothers who, due to health problems or that of the baby, must give birth to their child by caesarean section.[152]
Etymology
The Roman Lex Regia (royal law), later the Lex Caesarea (imperial law), of Numa Pompilius (715–673 BC),[153] required the child of a mother who had died during childbirth to be cut from her womb.[154] There was a cultural taboo that mothers should not be buried pregnant,[155] that may have reflected a way of saving some fetuses. Roman practice required a living mother to be in her tenth month of pregnancy before resorting to the procedure, reflecting the knowledge that she could not survive the delivery.[156]
Speculations that the Roman dictator Julius Caesar was born by the method now known as C-section are false.[157] Although caesarean sections were performed in Roman times, no classical source records a mother surviving such a delivery, while Caesar's mother lived for years after his birth.[154][158] As late as the 12th century, scholar and physician Maimonides expresses doubt over the possibility of a woman's surviving this procedure and again becoming pregnant.[159] The term has also been explained as deriving from the verb caedere, 'to cut', with children delivered this way referred to as caesones. Pliny the Elder refers to a certain Julius Caesar (an ancestor of the famous Roman statesman) as ab utero caeso, 'cut from the womb' giving this as an explanation for the cognomen Caesar which was then carried by his descendants.[154] Nonetheless, the false etymology has been widely repeated until recently. For example, the first (1888) and second (1989) editions of the Oxford English Dictionary say that caesarean birth "was done in the case of Julius Cæsar".[160] More recent dictionaries are more diffident: the online edition of the OED (2021) mentions "the traditional belief that Julius Cæsar was delivered this way",[161] and Merriam-Webster's Collegiate Dictionary (2003) says "from the legendary association of such a delivery with the Roman cognomen Caesar".[162]
The word Caesar, meaning either Julius Caesar or an emperor in general, is also borrowed or calqued in the name of the procedure in many other languages in Europe and beyond.[163]
Finally, the Roman praenomen (given name) Caeso was said to be given to children who were born via C-section. While this was probably just folk etymology made popular by Pliny the Elder, it was well known by the time the term came into common use.[164]
Spelling
The term caesarean is spelled in various accepted ways, as discussed at Wiktionary. The Medical Subject Headings (MeSH) of the United States National Library of Medicine (NLM) uses cesarean section,[165] while some other American medical works, e.g. Saunders Comprehensive Veterinary Dictionary, use caesarean,[166] as do most British works. The online versions of the US-published Merriam-Webster Dictionary[167] and American Heritage Dictionary[166] list cesarean first and other spellings as "variants".
Society and culture
Presence of father
In many hospitals, the mother's partner is encouraged to attend the surgery to support her and share the experience.[168] While traditionally there has been an opaque surgical drape obstructing the parents' view, some patients and doctors are opting for a "gentle C-section" using a clear drape, allowing the parents to watch the delivery and see their infant immediately.[169]
Special cases
In
In rare cases, caesarean sections can be used to remove a dead
The mother may perform a caesarean section on herself; there have been successful cases, such as Inés Ramírez Pérez of Mexico who, on 5 March 2000, took this action. She survived, as did her son, Orlando Ruiz Ramírez.[174][175][176]
In 2024, a female western lowland gorilla had a successful cesarean section after zoo veterinarians diagnosed her with pre-eclampsia. The premature gorilla infant survived, as a result of similar methods used with human infants.[177]
References
- .
- ^ a b c d e f g h i j k l "Pregnancy Labor and Birth". Office on Women's Health, U.S. Department of Health and Human Services. 1 February 2017. Archived from the original on 28 July 2017. Retrieved 15 July 2017.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ a b c d e f g h i j k l "Safe Prevention of the Primary Cesarean Delivery". American Congress of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine. March 2014. Retrieved 23 January 2022.
- ^ a b c d "WHO Statement on Caesarean Section Rates" (PDF). 2015. Archived (PDF) from the original on 1 May 2015. Retrieved 6 May 2015.
- ISBN 978-1-4496-1948-0. Archivedfrom the original on 11 September 2017.
- American Congress of Obstetricians and Gynecologists, archivedfrom the original on 1 September 2013, retrieved 1 August 2013
- S2CID 2638969.
- ^ PMID 26624825.
- ^ "Births: Provisional Data for 2017" (PDF). CDC. May 2018. Archived (PDF) from the original on 17 May 2018. Retrieved 18 May 2018.
- ^ ISBN 978-0-8018-8133-6.
- ^ ISSN 0144-3615.
- ^ "Cesarean Section - A Brief History preface". www.nlm.nih.gov. Retrieved 14 March 2024.
- ^ ISSN 2091-2749.
- PMID 1788548.
- ^ "The Truth About Julius Caesar and "Caesarean" Sections". 25 October 2013.
- JSTOR 2135690.
- ^ "Management of Genital Herpes in Pregnancy". ACOG. May 2020. Archived from the original on 16 January 2021. Retrieved 3 May 2020.
- S2CID 27545840.
- PMID 24631706.
- PMID 33818996.
- ^ "Caesarean Section". NHS Direct. Archived from the original on 1 February 2009. Retrieved 26 July 2006.
- ^ PMID 17296957.
- ^ a b Pain M (2000). "Medical Interventions: Caesarean Sections as a Case Study". Economic and Political Weekly. 35 (31): 2755–61.
- ^ "Why are Caesareans Done?". Gynaecworld. Archived from the original on 3 December 2008. Retrieved 26 July 2006.
- ^ PMID 28077411.
- S2CID 257455.
- ^ S2CID 22137961.
- PMID 23644593.
- ^ "UpToDate". www.uptodate.com. Retrieved 10 February 2024.
- ^ "Birth After Previous Caesarean Birth, Green-top Guideline No. 45" (PDF). Royal College of Obstetricians and Gynaecologists. February 2007. Archived from the original (PDF) on 7 December 2014.
- ^ a b c "Vaginal Birth after Cesarean (VBAC)". American Pregnancy Association. Archived from the original on 21 June 2012. Retrieved 16 June 2012.
- ^ a b "Vaginal birth after C-section (VBAC) guide". Mayo Clinic. Archived from the original on 12 March 2010.
- ^ PMID 20664418.
- ^ a b c "Elimination of Non-medically Indicated (Elective) Deliveries Before 39 Weeks Gestational Age" (PDF). Archived from the original (PDF) on 20 November 2012. Retrieved 13 July 2012.
- PMID 21606738.
- ^ from the original on 2 January 2016.
- ^ PMID 23062593.
- PMID 22713501.
- S2CID 20983040.
- S2CID 5152813.
- S2CID 26098748.
- S2CID 40347063.
- S2CID 37447326.
- ^ "Academic Achievement Varies With Gestational Age Among Children Born at Term". Archived from the original on 4 September 2015. Retrieved 12 July 2012.
- PMID 30726039. Retrieved 22 June 2022.
- ^ "Study: Early Repeat C-Sections Puts Babies At Risk". NPR.org. 8 January 2009. Archived from the original on 31 January 2016. Retrieved 26 July 2011.
- ^ "High infant mortality rate seen with elective c-section". Reuters Health—September 2006. Medicineonline.com. 14 September 2006. Archived from the original on 18 July 2011. Retrieved 26 July 2011.
- PMID 30349009.
- ^ C. Yuan et al. (2016), "Association Between Cesarean Birth and Risk of Obesity in Offspring in Childhood, Adolescence, and Early Adulthood", JAMA Pediatrics.
- S2CID 248903112.
- ^ "Why C-Section Babies May Be at Higher Risk for a Food Allergy". Consumer Health News | HealthDay. 30 April 2021. Retrieved 25 May 2022.
- ^ PMID 21283801.
- ^ PMID 10928020.
- ^ Miheso J, Burns S. "Care of women undergoing emergency caesarean section" (PDF). NHS Choices. Archived from the original (PDF) on 8 March 2018. Retrieved 7 March 2018.
- ^ PMID 23635708.
- PMID 18755018.
- PMID 23002336.
- PMID 23706093.
- PMID 17054264.
- PMID 16267757.
- PMID 16738168. Archived from the original(PDF) on 18 January 2017. Retrieved 30 December 2008.
- PMID 22419296.
- ^ "Elective Surgery and Patient Choice – ACOG". Archived from the original on 25 September 2015. Retrieved 4 October 2015.
- S2CID 32050828.
- ^ a b "Caesarean section | Guidance and guidelines | NICE". www.nice.org.uk. 23 November 2011. Retrieved 5 January 2019.
- ^ WebMD Editorial Contributors. Johnson TC (ed.). "Vaginal Birth After Cesarean (VBAC) – Overview". WebMD. Archived from the original on 30 December 2009.
- ^ "NCHS Data Brief: Recent Trends in Cesarean Delivery in the United States Products". Centers for Disease Control and Prevention. March 2010. Archived from the original on 17 May 2012. Retrieved 16 June 2012.
- PMID 22015878.
- PMID 26196961.
- ^ Stark M. Technique of cesarean section: Misgav Ladach method. In: Popkin DR, Peddle LJ (eds): Women's Health Today. Perspectives on current research and clinical practice. Proceedings of the XIV World Congress of Gynaecology and Obstetrics, Montreal. Parthenon Publishing group, New York, 81–5
- S2CID 5847957.
- S2CID 809690.
- S2CID 40829330.
- ^ PMID 23467047.
- PMID 24338262.
- S2CID 72559269.
- PMID 25048608.
- PMID 25110856.
- S2CID 25845500.
- ^ PMID 23076903.
- S2CID 21467445.
- PMID 29926477.
- PMID 16129992.
- PMID 28797894.
- PMID 23972750.
- PMID 24138769.
- PMID 24797575.
- ^ PMID 25350672.
- PMID 25479008.
- PMID 32580252.
- PMID 30096215.
- PMID 32619039.
- ^ PMID 24720501.
- PMID 27747876.
- PMID 30940757.
- S2CID 221466152.
- ^ "C-section recovery: What to expect". Mayo Clinic.
- PMID 11489150.
- PMID 27756207.
- PMID 29360829.
- S2CID 208064082.
- PMID 36413515.
- S2CID 267222803.
- ^ ISBN 978-0-295-74738-5.
- ^ "Stemming the global caesarean section epidemic". The Lancet. 13 October 2018. Retrieved 14 November 2018.
- ^ "C-section rate in Canada continues upward trend". Canada.com. 26 July 2007. Archived from the original on 14 May 2014.
- ^ "To push or not to push? It's a woman's right to decide". The Sydney Morning Herald. 2 January 2011. Archived from the original on 30 August 2011.
- ^ "Should there be a limit on Caesareans?". BBC News. 30 June 2010. Archived from the original on 20 July 2010.
- ^ "WHO | Global survey on maternal and perinatal health". Archived from the original on 10 November 2016. Retrieved 15 July 2017.
- PMID 21067593.
- PMID 18843605.
- PMID 12929294.
- ^ "C-section rates around globe at 'epidemic' levels". AP / NBC News. 12 January 2010. Archived from the original on 16 March 2013. Retrieved 21 February 2010.
- ^ "More evidence for a link between Caesarean sections and obesity". The Economist. 11 October 2017.
- S2CID 43551235.
- ^ "Women can choose Caesarean birth". BBC News. 23 November 2011. Archived from the original on 19 August 2012.
- ^ "Focus on: caesarean section—NHS Institute for Innovation and Improvement". Institute.nhs.uk. 8 October 2009. Archived from the original on 28 December 2011. Retrieved 26 May 2012.
- ^ "Caesarean Section Rates Royal College of Physicians of Ireland". Rcpi.ie. Archived from the original on 2 May 2012.
- ^ "La clinica dei record: 9 neonati su 10 nati con il parto cesareo". Corriere della Sera. 14 January 2009. Archived from the original on 24 July 2009. Retrieved 5 February 2009.
- ^ "Sagliocco denuncia boom di parti cesarei in Campania". Pupia.tv. 31 January 2009. Archived from the original on 18 April 2013. Retrieved 5 February 2009.
- ^ "Tassi di taglio cesareo per istituto ordinati (rango) per valore del tasso 2008. Anno 2008 - III trimestre 2009 (dati provvisori)" [Cesarean section rates by institution sorted (rank) by rate value 2008. Year 2008 - 3rd quarter 2009 (provisional data)] (PDF) (in Italian). Archived from the original (PDF) on 22 July 2011. Retrieved 12 August 2009.
- ^ "Cesarei, alla Mater Dei il record". Tgcom.mediaset.it. 14 January 2009. Retrieved 5 February 2009.
- ^ Pfuntner A., Wier L.M., Stocks C. Most Frequent Procedures Performed in U.S. Hospitals, 2011. HCUP Statistical Brief #165. October 2013. Agency for Healthcare Research and Quality, Rockville, MD. "Most Frequent Procedures Performed in U.S. Hospitals, 2011 – Statistical Brief #165". Archived from the original on 24 October 2013. Retrieved 22 October 2013..
- ^ "Births: Preliminary Data for 2007" (PDF). National Center for Health Statistics. Archived (PDF) from the original on 21 August 2013. Retrieved 23 November 2006.
- ^ "National Vital Statistics Reports" (PDF). Archived (PDF) from the original on 20 July 2017. Retrieved 9 September 2017.
- ^ Moore JE, Witt WP, Elixhauser A (April 2014). "Complicating Conditions Associate With Childbirth, by Delivery Method and Payer, 2011". HCUP Statistical Brief #173. Rockville, MD: Agency for Healthcare Research and Quality. Archived from the original on 14 July 2014. Retrieved 6 June 2014.
- ^ a b Hensley S (13 September 2010). "C-Sections And The Profit Motive In California". NPR. Retrieved 25 November 2022.
- ^ Vedantam S (30 August 2013). "Money May Be Motivating Doctors To Do More C-Sections". NPR. Retrieved 25 November 2022.
- S2CID 49305610.
- ISBN 0-465-03029-7.
- ^ Qian S. "楚世家 (House of Chu)". Records of the Grand Historian (in Chinese). Archived from the original on 10 March 2012. Retrieved 3 December 2011.
- S2CID 26690619.
- ^ S2CID 26690619.
- ^ Shahbazi AS. "RUDABA". Encyclopedia Iranica. Retrieved 19 July 2009.[permanent dead link]
- PMID 13777540.
- ^ Wikipedia Rostam
- PMID 16562221.
- ISBN 978-0-19-875856-3, retrieved 19 August 2023
- ^ "The Truth About Julius Caesar and "Caesarean" Sections". Today I Found Out. 25 October 2013. Retrieved 9 October 2020.
- ^ "St. Raymond Nonnatus". Catholic Online. Archived from the original on 19 July 2006. Retrieved 26 July 2006.
- PMID 27882755.
- ISSN 0362-4331. Retrieved 29 December 2019.
- ^ United States Congress House Committee on Appropriations (1970). Hearings, Reports and Prints of the House Committee on Appropriations. U.S. Government Printing Office.
- ISBN 0-7190-2925-2.
- ^ Sewell JE (1993), "Cesarean Section: A Brief History" (PDF), A Brochure to Accompany an Exhibition on the History of Cesarean Section at the National Library of Medicine, National Library on Medicine], archived from the original (PDF) on 5 November 2004
- ^ "Cesarean Section – A Brief History: Part 2". U.S. National Institutes of Health. 25 June 2009. Archived from the original on 21 December 2010. Retrieved 27 November 2010.
- ISBN 0-8248-1487-8.
- PMID 10212095.
- ^ Pain S (6 March 2008). "The 'male' military surgeon who wasn't". NewScientist.com. Archived from the original on 14 March 2008. Retrieved 16 March 2008.
- ^ "Woman's Ills". Time. 18 June 1951. Archived from the original on 13 April 2009. Retrieved 1 April 2009.
- ^ Caesarius Diaconus, testi e illustrazioni di Giovanni Guida, [s.l.: s.n.], 2015
- ^ Pasero Roberta, Cesareo di Terracina, un santo poco conosciuto: è il protettore del parto cesareo, in "DiPiù", anno XIV, n° 48, 3 dicembre 2018.
- ISBN 978-1-85070-321-1. Retrieved 7 December 2012.
- ^ a b c Van Dongen PW (August 2009). "Caesarean section–etymology and early history". South African Journal of Obstetrics and Gynaecology. 15 (2): 62–66. Archived from the original on 15 May 2013.
- ^ "As there was a cultural taboo against burying an undelivered woman in Roman and German societies, according to Lex Caesarea". U Högberg, E Iregren, CH Siven, "Maternal deaths in medieval Sweden: an osteological and life table analysis", Journal of Biosocial Science, 1987, 19: 495–503 Cambridge University Press
- ^ "Ancient Gynecology: Caesarean Section". Claude Moore Sciences Health Library. University of Virginia Health System. Archived from the original on 3 April 2013.
- ^ Bad Medicine: Misconceptions and Misuses Revealed, by Christopher Wanjek, p. 5 (John Wiley & Sons, 2003)
- ^ "could not survive the trauma of a Caesarean" Oxford Classical Dictionary, Third Edition, "Childbirth"
- ^ Commentary to Mishnah Bekhorot 8:2
- ^ "s.v. Cæsarean, 2". Oxford English Dictionary (2nd ed.). 1989. Archived from the original on 12 July 2020.
- ^ "most recently modified version published online March 2021" "s.v. Cæsarean, 2". Oxford English Dictionary.
- ISBN 978-0-87779-809-5
- ^ For a summary, of an article about the relevant historical and linguistic questions, see "Kaiserschnitt - Cäsars Geburtsgeschichte war ein historisches Missverständnis (W3)". Archived from the original on 6 January 2007.
- ISBN 978-0-8014-9974-6. "Appendix: Creative Etymology: Caesarean Section from Pliny to Rousset" (pp. 143-153) presents a history of the legend of caesarean births in Western culture.
- ^ "Cesarean Section".
- ^ a b "Caesarean".
- ^ "Definition of CESAREAN". 20 July 2023.
- PMID 26328461.
- ^ "'Gentle C-sections': Bringing a traditional birth experience to the OR | Your Pregnancy Matters | UT Southwestern Medical Center". utswmed.org. Retrieved 13 July 2023.
- ^ See Chok Yaakov 470:2; Kaf ha-Chayim 470:3; "Weekly-Halacha, Pesach 5758 - Torah.org". Archived from the original on 18 August 2010. Retrieved 28 July 2010.
- ^ "Pidyon HaBen — Definition of Pidyon HaBen (Redemption of the Firstborn)". Judaism.about.com. 19 October 2012. Archived from the original on 19 October 2011. Retrieved 15 August 2011.
- ^ "Kohanim forever from the sources, who is a cohen, the blessing of the Cohanim,. Mitvah of the cohen, Halacha, Temple service groups, pidyon—redemption of the firstborn". Cohen-levi.org. Archived from the original on 18 August 2011. Retrieved 15 August 2011.
- ^ Casey FE, Spandorfer SD (25 January 2022). Rivlin ME (ed.). "Elective Abortion". Medscape. Archived from the original on 14 December 2004. Retrieved 18 March 2016.
- ^ "True grit: the mum who delivered her own baby". The Sydney Morning Herald. 1 June 2004. Archived from the original on 18 July 2010. Retrieved 4 November 2010.
- S2CID 38220990.
- S2CID 10641064.
- ^ Yousef N (17 February 2024). "Texas zoo delivers baby gorilla via caesarean section". BBC News. Retrieved 18 February 2024.
