Medullary cystic kidney disease
| Medullary cystic kidney disease | |
|---|---|
 | |
| Medullary cystic kidney disease has an autosomal dominant pattern of inheritance | |
| Specialty | Medical genetics |
| Symptoms | Polydipsia[1] |
| Types | MCKD1 and MCKD2[2][3] |
| Diagnostic method | Kidney biopsy, Kidney ultrasound, CBC[4] |
| Medication | Currently no cure, Drink plenty of fluids, Salt supplement[4] |
Medullary cystic kidney disease (MCKD) is an
Signs and symptoms
In terms of the signs/symptoms of medullary cystic kidney disease, the disease is not easy to diagnose and is uncommon. In this condition, loss of kidney function occurs slowly over time, however the following signs/symptoms could be observed in an affected individual:[1]
- Polydipsia
- Enuresis
- Weakness
- Lack of appetite
- Pruritus
- Bone pain
- Pallor
- Nausea
Some individuals with this disease develop gout,[8] which is a condition in which patients develop severe pain and swelling in the big toe or another joint such as the knee. If untreated, it becomes chronic and affects the joints most of the time, instead of intermittently.[9]
Cause
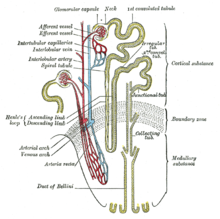
Normal individuals have two copies of the
MKD1/Mucin-1 kidney disease

Mucin-1 kidney disease (MKD) is due to a
This mutation alters the genetic sequence in the MUC1 gene, resulting in a new, mutated protein, furthermore, The disease is extremely rare and its prevalence is unknown. This disease is
Earlier on the condition was called medullary cystic kidney disease type 1. It was named this because some people with the disease had cysts (small holes) in the middle (medulla) of their kidneys. It has since then been found that these cysts are uncommon and are not found in the majority of the patients with MUC1 mutations. For this reason, this name has been abandoned, scientists (part of the Kidney Dialysis Initiatives and Global Outcomes group) specializing in this disease came together formally and created an official name for this and similar conditions.[6]
This condition was designated as Autosomal Dominant Tubulointerstitial Kidney Disease (ADTKD). In
MKD2/Uromodulin kidney disease
Medullary cystic kidney disease type 2 is due to mutations in a
In MKD2 inheritance, just as MKD1, autosomal dominant indicates that 50% of children of an affected person will inherit the disease. "Tubulointerstitial" is used because the problems that occur in this disease happen in the compartment of the kidney known as the tubulointerstitium, a shorter name of the disease is used by most individuals - uromodulin kidney disease (UKD).[15]
Diagnosis

The diagnosis of medullary cystic kidney disease can be done via a physical exam.[4] Further tests/exams are as follows:[1]
- A routine blood test called the serum creatinine can be done. Creatinine is a breakdown product from the muscle, as kidney function declines, the amount of blood creatinine goes up. Thus, most affected individuals have no symptoms of MCKD, but find that they have the condition due to an elevation in the blood creatinine level.[16]
- Affected individuals also have an elevation in the blood uric acid level. In MCKD, the kidney has difficulty getting rid of uric acid. One can find out that the uric acid level in the blood is high when a blood test is done. Gout is caused by high uric acid levels, and thus patients often have gout.[17]
- A kidney
- Definitive testing and diagnosis of MCKD can be made by analyzing the UMOD gene for mutations, this can be done by a blood test.[20]
Treatment
In terms of treatment/management for medullary cystic kidney disease, at present there are no specific therapies for this disease, and there are no specific diets known to slow progression of the disease. However, management for the symptoms can be dealt with as follows: erythropoietin is used to treat anemia, and growth hormone is used when growth becomes an issue. Additionally, a kidney transplant may be needed at some point. Finally, foods that contain potassium and phosphate must be reduced.[1]
Research
Scientists from the Broad Institute, Cambridge, Massachusetts identified the genetic cause of UKD as mutations in the MUC1 gene.[12]
See also
References
- ^ a b c d e f "Medullary Cystic Disease Treatment & Management: Medical Care, Surgical Care, Consultations". eMedicine. MedScape. Retrieved 15 June 2016.
- ^ a b "OMIM Entry - # 174000 - MEDULLARY CYSTIC KIDNEY DISEASE 1; MCKD1". omim.org. Retrieved 2 January 2018.
- ^ a b "OMIM Entry - # 603860 - MEDULLARY CYSTIC KIDNEY DISEASE 2; MCKD2". omim.org. Retrieved 2 January 2018.
- ^ a b c "Medullary cystic kidney disease: MedlinePlus Medical Encyclopedia". www.nlm.nih.gov. Retrieved 2016-06-03.
- ISBN 978-1-4557-4836-5.
Because the development of medullary cysts is neither an early nor a typical feature of the disease, many now consider the term medullary cystic kidney disease to be a misnomer and have proposed the term autosomal dominant tubulointerstitial kidney disease (ADTKD) to refer to a group of diseases caused by at least four genes: MUC1 encoding the mucoprotein mucin-1 (MUC-1) (chromosomal location 1q22); UMOD encoding uromodulin, also known as Tamm-Horsfall protein (chromosome 16p12.3); HNF1B encoding hepatocyte nuclear factor-1β (chromosome 17q12); and REN encoding renin (chromosome 1q32.1).
- ^ PMID 25738250. – via ScienceDirect(Subscription may be required or content may be available in libraries.)
- ^ Kmoch, Stanislav; Živná, Martina; Bleyer, Anthony (1993). "Autosomal Dominant Tubulointerstitial Kidney Disease, REN-Related". Autosomal Dominant Tubulointerstitial Kidney Disease, REN-Related (ADTKD-REN). University of Washington, Seattle. Retrieved June 11, 2016.
{{cite book}}:|website=ignored (help) - ^ PMID 12787393.
- ^ "Gout: MedlinePlus". www.nlm.nih.gov. Retrieved 2016-06-15.
- ^ a b Reference, Genetics Home. "medullary cystic kidney disease type 1". Genetics Home Reference. Retrieved 2016-06-15.
- ^ a b Reference, Genetics Home. "uromodulin-associated kidney disease". Genetics Home Reference. Retrieved 2016-06-15.
- ^ PMID 23396133.
- PMID 23946964.update 2013
- PMID 12471200.
- PMID 20301530.update 2013
- ^ "Creatinine blood test: MedlinePlus Medical Encyclopedia". www.nlm.nih.gov. Retrieved 2016-06-15.
- ^ "Uric acid - blood : MedlinePlus Medical Encyclopedia". www.nlm.nih.gov. Retrieved 2016-06-15.
- ^ "Kidney Biopsy". www.niddk.nih.gov. Retrieved 2016-06-15.
- ^ "Abdominal ultrasound: MedlinePlus Medical Encyclopedia". www.nlm.nih.gov. Retrieved 2016-06-15.
- ^ Reference, Genetics Home. "UMOD". Genetics Home Reference. Retrieved 2016-06-15.
Further reading
- Hateboer, Nick (2001). "Confirmation of a gene locus for medullary cystic kidney disease (MCKD2) on chromosome 16p12". Kidney International. 60 (4): 1233–1239. PMID 11576337.
- PMID 10966501. Retrieved 15 June 2016.
