Fish allergy
| Fish allergy | |
|---|---|
 | |
| Raw salmon steaks | |
| Frequency | Fish allergy frequency estimated at ~1.5% (self-reported, developed world)[1][2][3] |
Fish allergy is an
Unlike early childhood allergic reactions to milk and eggs, which often lessen as the children age,[6] fish allergy tends to first appear in school-age children and persist in adulthood.[7] Strong predictors for adult-persistence are anaphylaxis, high fish-specific serum immunoglobulin E (IgE) and robust response to the skin prick test. It is unclear if the early introduction of fish to the diet of babies aged 4–6 months decreases the risk of later development of fish allergy. Adult onset of fish allergy is common in workers in the fish catching and processing industry.[8][9]
Signs and symptoms

Food allergies in general usually have an onset of symptoms in the range of minutes to hours for an IgE-mediated response, which may include anaphylaxis.[10] Symptoms may include rash, hives, itching of mouth, lips, tongue, throat, eyes, skin, or other areas, swelling of lips, tongue, eyelids, or the whole face, difficulty swallowing, runny or congested nose, hoarse voice, wheezing, shortness of breath, diarrhea, abdominal pain, lightheadedness, fainting, nausea, or vomiting.[11] Non-IgE-mediated responses occur hours to days after consuming the allergenic food, and are not as severe as IgE-mediated symptoms. Symptoms of allergies vary from person to person and incident to incident.[11]
Potentially life-threatening, the anaphylactic onset of an allergic reaction is characterized by respiratory distress, as indicated by wheezing, breathing difficulty, and
Causes
Eating fish
The cause is typically the eating of fish or foods that contain fish. Once an allergic reaction has occurred it usually remains a lifelong sensitivity.[7] Briefly, the immune system overreacts to proteins found in fish, primarily to parvalbumin,[14] but sometimes to other proteins, such as fish collagen. The allergic reaction to shellfish and crustaceans such as lobster and shrimp is to a different protein, tropomyosin, so there is no cross-reactivity between fish and shellfish allergy.[14][15][16]
Cross-contact
Cross-contact, also referred to as cross-contamination, occurs when foods are being processed in factories or at food markets, or are being prepared for cooking in restaurants and home kitchens. The allergenic proteins are transferred from one food to another.[17]
Fish parasite

The food-borne parasite
Occupational exposure
An industry review conducted in 1990 estimated that 28.5 million people worldwide were engaged in some aspect of the seafood industry: fishing, aquaculture, processing and industrial cooking. Men predominate in fishing, women in processing facilities.
Exercise as contributing factor
Exercise can be a contributing factor to an allergic food response. There is a condition called food-dependent, exercise-induced anaphylaxis. For people with this condition, exercise alone is not sufficient, nor consumption of a food to which they are mildly allergic sufficient, but when the food in question is consumed within a few hours before high intensity exercise, the result can be anaphylaxis. Fish are specifically mentioned as a causative food.[22][23][24] One theory is that exercise is stimulating the release of mediators such as histamine from IgE-activated mast cells.[24] Two of the reviews postulate that exercise is not essential for the development of symptoms, but rather that it is one of several augmentation factors, citing evidence that the culprit food in combination with alcohol or aspirin will result in a respiratory anaphylactic reaction.[22][24]
Mechanisms
Allergic response
Conditions caused by food allergies are classified into three groups according to the mechanism of the allergic response:[25]
- IgE-mediated (classic) – the most common type, manifesting acute changes that occur shortly after eating, and may progress to anaphylaxis
- Non-IgE mediated – characterized by an immune response not involving immunoglobulin E; may occur hours to days after eating, complicating diagnosis
- IgE and non-IgE-mediated – a hybrid of the above two types
The
After the chemical mediators of the acute response subside, late-phase responses can often occur due to the migration of other
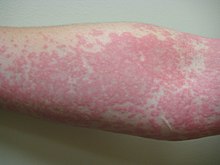
In addition to IgE-mediated responses, fish allergy can manifest as atopic dermatitis, especially in infants and young children.[33] Some will display both, so that a child could react to an oral food challenge with allergic symptoms, followed a day or two later with a flare up of atopic dermatitis and/or gastrointestinal symptoms, including allergic eosinophilic esophagitis.[34]
Fish allergenic proteins
The protein
Non-allergic intolerance


Scombroid food poisoning, also referred to as scrombroid, is a reaction from consuming fish that mimics an allergic reaction.[7][42][43][44] It is caused by high concentrations of histamine, synthesized by bacteria in spoiled fish. Histamine is the main natural chemical responsible for true allergic reactions, hence the confusion with fish allergy. Scombroid symptoms onset is typically 10–30 minutes after consumption, and may include flushed skin, headache, itchiness, blurred vision, abdominal cramps and diarrhea.[42] Fish commonly implicated include tuna, mackerel, sardine, anchovy, herring, bluefish, amberjack and marlin. These fish naturally have high levels of the amino acid histidine, which is converted to histamine when bacterial growth occurs during improper storage. Subsequent cooking, smoking, canning or freezing does not eliminate the histamine.[7][42][43][44]
Diagnosis
Diagnosis of fish allergy is based on the person's history of allergic reactions,
Prevention
When fish is introduced to a baby's diet, it is thought to affect risk of developing allergy, but there are contradictory recommendations. Reviews of allergens in general stated that introducing solid foods at 4–6 months may result in the lowest subsequent allergy risk.[45] Reviews specific to when fish is introduced to the diet state that fish consumption during the first year of life reduce the subsequent risks of eczema and allergic rhinitis,[45][46] but maternal consumption during pregnancy had no such effect.[46]
Treatment

Treatment for accidental ingestion of fish products by allergic individuals varies depending on the sensitivity of the person. An
Prognosis
Unlike milk and egg allergies,[6][50] fish allergy usually persists into adulthood.[2][7]
Epidemiology
Incidence and prevalence are terms commonly used in describing disease epidemiology. Incidence is newly diagnosed cases, which can be expressed as new cases per year per million people. Prevalence is the number of cases alive, expressible as existing cases per million people during a period of time.[51] Reviews cite self-reported fish allergy in range of 0 to 2.5% in the general population.[1][2][3] Self-reported allergy prevalence is always higher than food-challenge confirmed allergy, which two reviews put at 0.1% and 0.3%, respectively.[1][39]
Regulation
Whether food allergy prevalence is increasing or not, food allergy awareness has definitely increased, with impacts on the quality of life for children, their parents and their immediate caregivers.
Regulation of labeling

In response to the risk that certain foods pose to those with food allergies, some countries have responded by instituting labeling laws that require food products to clearly inform consumers if their products contain major allergens or byproducts of major allergens among the ingredients intentionally added to foods. Nevertheless, there are no labeling laws to mandatory declare the presence of trace amounts in the final product as a consequence of cross-contamination.[56][59][60][61][62]
Ingredients intentionally added
FALCPA requires companies to disclose on the label whether a packaged food product contains any of these eight major food allergens, added intentionally: cow's milk, peanuts, eggs, shellfish, fish, tree nuts, soy and wheat.[56] This list originated in 1999 from the World Health Organisation Codex Alimentarius Commission.[63] To meet FALCPA labeling requirements, if an ingredient is derived from one of the required-label allergens, then it must either have its "food sourced name" in parentheses, for example "Casein (milk)," or as an alternative, there must be a statement separate but adjacent to the ingredients list: "Contains milk" (and any other of the allergens with mandatory labeling).[56][60]
See also
- List of allergens (food and non-food)
References
- ^ S2CID 28692645.
- ^ S2CID 26248686.
- ^ PMID 17628647.
- ^ National Report of the Expert Panel on Food Allergy Research, NIH-NIAID 2003 "June 30 2003.pdf" (PDF). Archived from the original (PDF) on 2006-10-04. Retrieved 2006-08-07.
- ^ "Food Allergy Facts" Archived 2012-10-06 at the Wayback Machine Asthma and Allergy Foundation of America
- ^ PMID 25178179.
- ^ S2CID 1154235.
- ^ S2CID 1276304.
- ^ PMID 11511741.
- ^ S2CID 11054771.
- ^ a b c MedlinePlus Encyclopedia: Food allergy
- PMID 28780941.
- ^ PMID 24388012.
- ^ PMID 30323632.
- ^ S2CID 46921072.
- ^ PMID 26022875.
- ^ "Avoiding Cross-Contact". FARE: Food Allergy Research & Education. Retrieved 5 December 2020.
- ^ PMID 31338296.
- PMID 32191412.)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - S2CID 1185184.
- PMID 18400801.
- ^ PMID 28283153.
- PMID 27822074.
- ^ PMID 24133612.
- NHS Choices. 16 May 2016. Retrieved 31 January 2017.
A food allergy is when the body's immune system reacts unusually to specific foods
- ISBN 978-0-7817-5317-3.
- S2CID 205691620.
- S2CID 10621652.
- PMID 25778347.
- ^ ISBN 978-0-8153-4101-7. Archivedfrom the original on 2009-06-28.
- PMID 17011762.
- S2CID 40819814.
- PMID 24229818.
- S2CID 5421783.
- S2CID 29615377.
- ^ S2CID 22539836.
- PMID 25451973.
- S2CID 22118352.
- ^ PMID 30741635.
- PMID 32389794.
- PMID 27114499.
- ^ a b c "Food Poisoning from Marine Toxins - Chapter 2 - 2018 Yellow Book". Centers for Disease Control and Prevention (CDC). 2017. Retrieved 15 July 2020.
- ^ S2CID 21610715.
- ^ S2CID 34835091.
- ^ PMID 31117223.
- ^ S2CID 22656321.
- PMID 14567487.
- S2CID 11054771.
- PMID 29676439.
- PMID 25459576.
- ^ "What is Prevalence?" National Institute of Mental Health (Accessed 25 December 2020).
- PMID 25725570.
- PMID 25668890.
- PMID 26120535.
- S2CID 326837.
- ^ a b c d "Food Allergen Labeling and Consumer Protection Act of 2004". FDA. 2 August 2004. Retrieved 7 March 2022.
- ^ Culinary Institute of America Allergen-free oasis comes to the CIA (2017)
- PMID 18751571.
- ^ "Food allergen labelling and information requirements under the EU Food Information for Consumers Regulation No. 1169/2011: Technical Guidance" Archived 2017-07-07 at the Wayback Machine (April 2015).
- ^ a b FDA (14 December 2017). "Have Food Allergies? Read the Label". Food and Drug Administration. Retrieved 14 January 2018.
- ^ "Food Ingredients of Public Health Concern" (PDF). United States Department of Agriculture. Food Safety and Inspection Service. 7 March 2017. Retrieved 16 February 2018.
- ^ "Allergies and Food Safety". United States Department of Agriculture. Food Safety and Inspection Service. 1 December 2016. Retrieved 16 February 2018.
- PMID 24791183.
