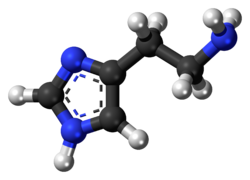
Histamine
 | |
 | |
| Names | |
|---|---|
| IUPAC name
2-(1H-Imidazol-4-yl)ethanamine
| |
| Identifiers | |
3D model (
JSmol ) |
|
| ChEBI | |
| ChEMBL | |
| ChemSpider | |
| DrugBank | |
ECHA InfoCard
|
100.000.092 |
IUPHAR/BPS |
|
| KEGG | |
| MeSH | Histamine |
PubChem CID
|
|
| UNII | |
CompTox Dashboard (EPA)
|
|
| |
SMILES
| |
| Properties | |
| C5H9N3 | |
| Molar mass | 111.148 g·mol−1 |
| Melting point | 83.5 °C (182.3 °F; 356.6 K) |
| Boiling point | 209.5 °C (409.1 °F; 482.6 K) |
| Easily soluble in cold water, hot water[1] | |
| Solubility in other solvents | Easily soluble in methanol. Very slightly soluble in diethyl ether.[1] Easily soluble in ethanol. |
| log P | −0.7[2] |
| Acidity (pKa) | Imidazole: 6.04 Terminal NH2: 9.75[2] |
| Pharmacology | |
| L03AX14 (WHO) V04CG03 (WHO) (phosphate) | |
Except where otherwise noted, data are given for materials in their standard state (at 25 °C [77 °F], 100 kPa).
| |
Histamine is an organic
Properties
Histamine base, obtained as a mineral oil

Histamine has two
Synthesis and metabolism
Histamine is derived from the

Once formed, histamine is either stored or rapidly inactivated by its primary
Bacteria also are capable of producing histamine using
Storage and release

Most histamine in the body is generated in granules in
The most important pathophysiologic mechanism of mast cell and basophil histamine release is
Histamine release occurs when allergens bind to mast-cell-bound IgE antibodies. Reduction of IgE overproduction may lower the likelihood of allergens finding sufficient free IgE to trigger a mast-cell-release of histamine.
Degradation
Histamine is released by mast cells as an immune response and is later degraded primarily by two enzymes:
DAO is typically expressed in epithelial cells at the tip of the villus of the small intestine mucosa.[14] Reduced DAO activity is associated with gastrointestinal disorders and widespread food intolerances. This is due to an increase in histamine absorption through enterocytes, which increases histamine concentration in the bloodstream.[15] One study found that migraine patients with gluten sensitivity were positively correlated with having lower DAO serum levels.[16] Low DAO activity can have more severe consequences as mutations in the ABP1 alleles of the AOC1 gene have been associated with ulcerative colitis.[17] Heterozygous or homozygous recessive genotypes at the rs2052129, rs2268999, rs10156191 and rs1049742 alleles increased the risk for reduced DAO activity.[18] People with genotypes for reduced DAO activity can avoid foods high in histamine, such as alcohol, fermented foods, and aged foods, to attenuate any allergic reactions. Additionally, they should be aware whether any probiotics they are taking contain any histamine-producing strains and consult with their doctor to receive proper support [citation needed].
HNMT is expressed in the central nervous system, where deficiencies have been shown to lead to aggressive behavior and abnormal sleep-wake cycles in mice.[19] Since brain histamine as a neurotransmitter regulates a number of neurophysiological functions, emphasis has been placed on the development of drugs to target histamine regulation. Yoshikawa et al. explores how the C314T, A939G, G179A, and T632C polymorphisms all impact HNMT enzymatic activity and the pathogenesis of various neurological disorders.[15] These mutations can have either a positive or negative impact. Some patients with ADHD have been shown to exhibit exacerbated symptoms in response to food additives and preservatives, due in part to histamine release. In a double-blind placebo-controlled crossover trial, children with ADHD who responded with aggravated symptoms after consuming a challenge beverage were more likely to have HNMT polymorphisms at T939C and Thr105Ile.[20] Histamine's role in neuroinflammation and cognition has made it a target of study for many neurological disorders, including autism spectrum disorder (ASD). De novo deletions in the HNMT gene have also been associated with ASD.[13]
Mast cells serve an important immunological role by defending the body from antigens and maintaining homeostasis in the gut microbiome. They act as an alarm to trigger inflammatory responses by the immune system. Their presence in the digestive system enables them to serve as an early barrier to pathogens entering the body. People who suffer from widespread sensitivities and allergic reactions may have mast cell activation syndrome (MCAS), in which excessive amounts of histamine are released from mast cells, and cannot be properly degraded. The abnormal release of histamine can be caused by either dysfunctional internal signals from defective mast cells or by the development of clonal mast cell populations through mutations occurring in the tyrosine kinase Kit.[21] In such cases, the body may not be able to produce sufficient degradative enzymes to properly eliminate the excess histamine. Since MCAS is symptomatically characterized as such a broad disorder, it is difficult to diagnose and can be mislabeled as a variety of diseases, including irritable bowel syndrome and fibromyalgia.[21]
Histamine is often explored as a potential cause for diseases related to hyper-responsiveness of the immune system. In patients with asthma, abnormal histamine receptor activation in the lungs is associated with bronchospasm, airway obstruction, and production of excess mucus. Mutations in histamine degradation are more common in patients with a combination of asthma and allergen hypersensitivity than in those with just asthma. The HNMT-464 TT and HNMT-1639 TT polymorphisms are significantly more common among children with allergic asthma, the latter of which is overrepresented in African-American children.[22]
Mechanism of action
In humans, histamine exerts its effects primarily by binding to
G-protein coupled receptor |
Location | Function | Sources |
|---|---|---|---|
| Histamine H1 receptor |
• CNS: Expressed on the dendrites of the output neurons of the histaminergic tuberomammillary nucleus, which projects to the dorsal raphe, locus coeruleus, and additional structures. mast cells , sensory nerves
|
• CNS: , involved in cognition• Periphery: Causes urticaria .
|
[23][24][25][26][27] |
| Histamine H2 receptor |
• CNS: Dorsal striatum (caudate nucleus and putamen), cerebral cortex (external layers), hippocampal formation, dentate nucleus of the cerebellum • Periphery: Located on |
• CNS: Not established (note: most known H2 receptor ligands are unable to cross the blood–brain barrier in sufficient concentrations to allow for neuropsychological and behavioral testing) |
[23][24][28][27] |
| Histamine H3 receptor | Located in the central nervous system and to a lesser extent peripheral nervous system tissue | Autoreceptor and heteroreceptor functions: decreased neurotransmitter release of histamine, acetylcholine, norepinephrine, serotonin. Modulates nociception, gastric acid secretion, and food intake. | [23] |
| Histamine H4 receptor | Located primarily on colon .
|
Plays a role in mast cell chemotaxis, itch perception, cytokine production and secretion, and visceral hypersensitivity. Other putative functions (e.g., inflammation, allergy, cognition, etc.) have not been fully characterized. | [23] |
| Ligand-gated ion channel | Location | Function | Sources |
| Histamine-gated chloride channel | Putatively: CNS (hypothalamus, thalamus) and intestinal epithelium | Brain: Produces fast secretory diarrhea )
|
[23][24] |
Roles in the body
Although histamine is small compared to other biological molecules (containing only 17 atoms), it plays an important role in the body. It is known to be involved in 23 different physiological functions. Histamine is known to be involved in many physiological functions because of its chemical properties that allow it to be versatile in binding. It is Coulombic (able to carry a charge), conformational, and flexible. This allows it to interact and bind more easily.[29]
Vasodilation and fall in blood pressure
It has been known for more than one hundred years that an intravenous injection of histamine causes a fall in the blood pressure.[30] The underlying mechanism concerns both vascular hyperpermeability and vasodilation. Histamine binding to endothelial cells causes them to contract, thus increasing vascular leak. It also stimulates synthesis and release of various vascular smooth muscle cell relaxants, such as nitric oxide, endothelium-derived hyperpolarizing factors and other compounds, resulting in blood vessel dilation.[31] These two mechanisms play a key role in the pathophysiology of anaphylaxis.
Effects on nasal mucous membrane
Increased vascular permeability causes fluid to escape from capillaries into the tissues, which leads to the classic symptoms of an allergic reaction: a runny nose and watery eyes. Allergens can bind to
- sneezing due to histamine-associated sensory neural stimulation
- hyper-secretion from glandular tissue
- nasal congestion due to vascular engorgement associated with vasodilation and increased capillary permeability
Sleep-wake regulation
Histamine is a
First-generation
Gastric acid release
Enterochromaffin-like cells in the stomach release histamine, stimulating parietal cells via H2 receptors. This triggers carbon dioxide and water uptake from the blood, converted to carbonic acid by carbonic anhydrase. The acid dissociates into hydrogen and bicarbonate ions within the parietal cell. Bicarbonate returns to the bloodstream, while hydrogen ions are pumped into the stomach lumen. Histamine release ceases as stomach pH decreases.[medical citation needed] Antagonist molecules, such as ranitidine or famotidine, block the H2 receptor and prevent histamine from binding, causing decreased hydrogen ion secretion.[medical citation needed]
Protective effects
While histamine has stimulatory effects upon neurons, it also has suppressive ones that protect against the susceptibility to convulsion, drug sensitization, denervation supersensitivity, ischemic lesions and stress.[36] It has also been suggested that histamine controls the mechanisms by which memories and learning are forgotten.[37]
Erection and sexual function
sexual dysfunction in females. . (October 2023) |
Schizophrenia
Metabolites of histamine are increased in the cerebrospinal fluid of people with schizophrenia, while the efficiency of H1 receptor binding sites is decreased. Many atypical antipsychotic medications have the effect of increasing histamine production, because histamine levels seem to be imbalanced in people with that disorder.[40]
Multiple sclerosis
Histamine therapy for treatment of multiple sclerosis is currently being studied. The different H receptors have been known to have different effects on the treatment of this disease. The H1 and H4 receptors, in one study, have been shown to be counterproductive in the treatment of MS. The H1 and H4 receptors are thought to increase permeability in the blood-brain barrier, thus increasing infiltration of unwanted cells in the central nervous system. This can cause inflammation, and MS symptom worsening. The H2 and H3 receptors are thought to be helpful when treating MS patients. Histamine has been shown to help with T-cell differentiation. This is important because in MS, the body's immune system attacks its own myelin sheaths on nerve cells (which causes loss of signaling function and eventual nerve degeneration). By helping T cells to differentiate, the T cells will be less likely to attack the body's own cells, and instead, attack invaders.[41]
Disorders
As an integral part of the immune system, histamine may be involved in
Histamine intolerance is a presumed set of adverse reactions (such as flush, itching, rhinitis, etc.) to ingested histamine in food. The mainstream theory accepts that there may exist adverse reactions to ingested histamine, but does not recognize histamine intolerance as a separate condition that can be diagnosed.[44]
The role of histamine in health and disease is an area of ongoing research. For example, histamine is researched in its potential link with migraine episodes, when there is a noted elevation in the plasma concentrations of both histamine and calcitonin gene-related peptide (CGRP). These two substances are potent vasodilators, and have been demonstrated to mutually stimulate each other's release within the trigeminovascular system, a mechanism that could potentially instigate the onset of migraines. In patients with a deficiency in histamine degradation due to variants in the AOC1 gene that encodes diamine oxidase enzyme, a diet high in histamine has been observed to trigger migraines, that suggests a potential functional relationship between exogenous histamine and CGRP, which could be instrumental in understanding the genesis of diet-induced migraines, so that the role of histamine, particularly in relation to CGRP, is a promising area of research for elucidating the mechanisms underlying migraine development and aggravation, especially relevant in the context of dietary triggers and genetic predispositions related to histamine metabolism.[45]
Measurement
Histamine, a biogenic amine, involves many physiological functions, including the immune response, gastric acid secretion, and neuromodulation. However, its rapid metabolism makes it challenging to measure histamine levels directly in plasma.[46]
As a solution for the rapid metabolism of histamine, the measurement of histamine and its metabolites, particularly the 1,4-methyl-imidazolacetic acid, in a 24-hour urine sample, provides an efficient alternative to histamine measurement because the values of these metabolites remain elevated for a much longer period than the histamine itself.[47]
Commercial laboratories provide a
The urine test involves collecting all urine produced in a 24-hour period, which is then analyzed for the presence of 1,4-methyl-imidazolacetic acid. This comprehensive approach ensures a more accurate reflection of histamine metabolism over an extended period; as such, the 1,4-methyl-imidazolacetic acid urine test offered by commercial labs is currently the most reliable method to determine the rate of histamine metabolism, which may be helpful for the health care practitioners to assess individual’s health status,[51][52] such as to diagnose interstitial cystitis.[53]
History
The properties of histamine, then called β-imidazolylethylamine, were first described in 1910 by the British scientists
, yielding "tissue amine"."H substance" or "substance H" are occasionally used in medical literature for histamine or a hypothetical histamine-like diffusible substance released in allergic reactions of skin and in the responses of tissue to inflammation.
See also
- Anaphylaxis
- Diamine oxidase
- Histamine N-methyltransferase
- Hay fever (allergic rhinitis)
- Histamine intolerance
- Histamine receptor antagonist
- Scombroid food poisoning
- Photic sneeze reflex
References
- ^ a b Histamine Material Safety Data Sheet (Technical report). sciencelab.com. 2013-05-21. Archived from the original on 2012-03-24.
- ^ PMID 21332182.
- ISBN 0-8053-4989-8.
- PMID 27563055.
- PMID 27028114.
- (PDF) from the original on 2019-03-30. Retrieved 2024-02-20.
- ISBN 0-17-625987-2.
- ^ "Histamine". webbook.nist.gov. Archived from the original on 2018-04-27. Retrieved 2015-01-04.
- ^ "Histamine dihydrochloride H7250". Sigma-Aldrich. Archived from the original on 2015-08-09.
- ISBN 9287152810. Archived from the original(PDF) on 2015-01-04. Retrieved 2015-01-04.
- PMID 5452432.
- PMID 17892274. Archived from the original(PDF) on 19 July 2011.
- ^ PMID 28485729.
- PMID 2110876.
- ^ PMID 30744146.
- S2CID 216303896.
- PMID 16489678.
- S2CID 205405463.[permanent dead link]
- PMID 30224900.
- PMID 20551163.
- ^ PMID 22957768.
- PMID 25909280.
- ^ PMID 26084539.
- ^ PMID 26194403.
- PMID 22586376.
- PMID 30846750.
- ^ S2CID 210119438.
- ^ Maguire JJ, Davenport AP (29 November 2016). "H2 receptor". IUPHAR/BPS Guide to Pharmacology. International Union of Basic and Clinical Pharmacology. Archived from the original on 21 March 2017. Retrieved 20 March 2017.
- ISBN 380557715X.
- PMID 16993030.
- ISBN 978-0-323-47978-3.
- ^
Monroe EW, Daly AF, Shalhoub RF (February 1997). "Appraisal of the validity of histamine-induced wheal and flare to predict the clinical efficacy of antihistamines". The Journal of Allergy and Clinical Immunology. 99 (2): S798-806. PMID 9042073.
- ISBN 978-0-12-374947-5.
- S2CID 10170830.
- PMID 17021184.
- PMID 16890992.
- S2CID 205879131.
- ^ S2CID 23148946.
- PMID 7850330.
- PMID 15334189.
Many atypical antipsychotics also increased histamine turnovers.
- S2CID 7852375.
- PMID 19309354.
- PMID 11377686.
- license.
- PMID 38447930.
- from the original on 18 August 2024. Retrieved 18 August 2024.
- from the original on 18 August 2024. Retrieved 18 August 2024.
- PMID 32928382.
- ^ "2-(1-methyl-1H-imidazol-4-yl)acetic acid". PubChem. U.S. National Library of Medicine. Archived from the original on 18 August 2024. Retrieved 2024-08-18.
- PMID 28321587.
- from the original on 18 August 2024. Retrieved 18 August 2024.
- from the original on 18 August 2024. Retrieved 18 August 2024.
- PMID 8015069.
- PMID 16993030.[permanent dead link]
