Milk allergy
| Milk allergy | |
|---|---|
| Causes | Type I hypersensitivity[2] |
| Risk factors | Childhood in developed countries where cow's milk infant formula is introduced to supplement or after breast feeding ends[3] |
| Diagnostic method | Medical history and standard allergy tests[4] |
| Prevention | Introduction to allergenic foods during infancy[5] |
| Treatment | Epinephrine[6] Antihistamines (mild)[7][8] |
| Prognosis | approximately 20% persist into adulthood[9] |
| Frequency | 2–3% in infants,[3] declining to 0.6% in adults[10] |
Milk allergy is an adverse
In the United States, 90% of
The condition may be managed by avoiding consumption of any dairy products or foods that contain dairy ingredients.
Milk allergy affects between 2% and 3% of babies and young children.
Signs and symptoms
Rapid and delayed response
Symptoms

IgE-mediated symptoms include: rash,
Non-lgE-mediated symptoms
For milk allergy, non-IgE-mediated responses are more common than are those that are IgE-mediated.
Mechanisms
Conditions caused by food allergies are classified into three groups according to the mechanism of the allergic response:[31]
- IgE-mediated (classic) – the most common type, manifesting as acute changes that occur shortly after eating, and may progress to anaphylaxis
- Non-IgE mediated – characterized by an immune response not involving IgE; may occur hours to days after eating, complicating the diagnosis
- IgE- and non-IgE-mediated – a hybrid of the above two types
In the early stages of acute allergic reaction,
After the chemical mediators of the acute response subside, late-phase responses can often occur because of the migration of other
Six major allergenic proteins from cow's milk have been identified: αs1-, αs2-, β-, and κ-casein from casein proteins and α-lactalbumin and β-lactoglobulin from whey proteins. There is some cross-reactivity with soy protein, particularly in non-IgE mediated allergy. Heat can reduce allergenic potential, so dairy ingredients in baked goods may be less likely to trigger a reaction than would milk or cheese.[2] For milk allergy, non-IgE-mediated responses are more common than are IgE-mediated. The former can manifest as atopic dermatitis and gastrointestinal symptoms, especially in infants and young children. Some will display both, so that a child could react to an oral food challenge with respiratory symptoms and hives (skin rash), followed a day or two later with a flareup of atopic dermatitis and gastrointestinal symptoms, including chronic diarrhea, blood in the stools, gastroesophageal reflux disease (GERD), constipation, chronic vomiting and colic.[2]
Diagnosis

Diagnosis of milk allergy is based on the person's history of allergic reactions,
Attempts have been made to identify SPT and IgE responses accurate enough to avoid the need for confirmation with an oral food challenge. A systematic review stated that in children younger than two years, cutoffs for specific IgE or SPT seem to be more homogeneous and may be proposed. For older children, the tests were less consistent. The review concluded: "None of the cut-offs proposed in the literature can be used to definitely confirm cow's milk allergy diagnosis, either to fresh pasteurized or to baked milk."[37]
Differential diagnosis
The symptoms of milk allergy can be confused with other disorders that present similar clinical features, such as
Lactose intolerance
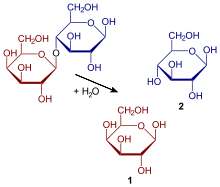
Milk allergy is distinct from lactose intolerance, which is a nonallergic
Prevention
Research regarding prevention seeks to determine the possibility of reducing the risk of developing an allergy before it manifests. Reviews have concluded that no strong evidence exists to recommend changes to the diets of pregnant or nursing women as a means of preventing the development of food allergy in their infants.[45][46][47] For mothers of infants considered at high risk of developing cow's milk allergy because of a family history, there is some evidence that the nursing mother avoiding allergens may reduce risk of the child developing eczema, but a Cochrane review concluded that more research is needed.[46]
There is some evidence that formula supplement given within the first 24 hours of a babies life in hospital increases the incidence of cow's milk allergy for mothers who then go on to exclusively breast feed.[48]
Guidelines from various government and international organizations recommend that for the lowest allergy risk, infants be exclusively breastfed for four to six months, but there does not appear to be any benefit beyond six months.[47][49] If a nursing mother decides to start feeding with an infant formula prior to four months, the recommendation is to use a formula containing cow's milk proteins.[50]
A different consideration occurs when a family history exists, either in parents or older siblings, of milk allergy. To avoid formula with intact cow's milk proteins, the product may be substituted with one containing extensively hydrolyzed milk proteins, with a non-dairy formula or with free amino acids. The
Treatment
The need for a dairy-free diet should be reevaluated every six months by testing milk-containing products low on the "milk ladder," such as fully cooked foods containing milk in which the milk proteins have been

Treatment for accidental ingestion of milk products by allergic individuals varies depending on the sensitivity of the person. An
Avoiding dairy
Most patients with milk allergy find it necessary to strictly avoid any item containing dairy ingredients[16] because the threshold dose capable of provoking an allergic reaction can be quite small, especially in infants. An estimated 5% react to less than 30 milligrams of dairy proteins, and 1% react to less than one milligram.[57] A more recent review calculated that the eliciting threshold dose for an allergic reaction in 1% of people (ED01) with confirmed cow's milk allergy is 0.1 mg of cow's milk protein.[58]
Beyond the obvious ingredients (anything with milk, cheese, cream, curd, butter, ghee or yogurt in the name), in countries where allergen labeling is mandatory, the ingredient list is expected to list all ingredients. Patients are advised to always carefully read food package labels, as sometimes even a familiar brand undergoes an ingredient change.[59] In the U.S., for all foods except meat, poultry, egg-processed products and most alcoholic beverages, if an ingredient is derived from one of the required-label allergens, the product's packaging must display the food name in parentheses or include a statement separate from, but adjacent to, the ingredients list that specifically names each allergen.[13][59][60][61] Dairy-sourced protein ingredients include casein, caseinates, whey and lactalbumin, among others.[59][62] The U.S. FDA has a recall process for foods that contain undeclared allergenic ingredients.[63] The University of Wisconsin maintains a list of foods that may contain dairy proteins but are not always obvious from the name or type of food.[62] This list contains the following examples:
- Bread, baked goods and desserts
- Caramel and nougat candies
- Cereals, crackers, food bars
- Chewing gum
- Chocolate (both milk chocolate and dark chocolate)
- "Cream of..." soups
- Creamy pasta sauces
- Creamy salad dressings
- Eggnog
- Flavored potato chips
- Hot dogs and lunch meat
- Instant mashed potatoes
- Margarine
- Medical food beverages
- Non-dairy creamer
- Sherbet
- Pudding and custard
There is a distinction between "Contains ___" and "May contain ___." The first is a deliberate addition to the ingredients of a food and is required. The second addresses unintentional possible introduction of ingredients occurring during transportation, storage or at the manufacturing site, and is voluntary; this is known as precautionary allergen labeling.[13][18][59]
Milk from other mammalian species such as goats and sheep should not be used as a substitute for cow's milk, as milk proteins from other mammals are often cross-reactive.[64] However, some people with cow's milk allergy can tolerate goat's or sheep's milk. Milk from camels, pigs, reindeer, horses and donkeys may also be tolerated in some cases.[53] Probiotic products have been tested, and some have been found to contain milk proteins that were not always indicated on the labels.[65][66]
Cross-reactivity with soy
Infants, either still 100% breastfeeding or on infant formula, and young children may be prone to a combined cow's milk and soy protein allergy, referred to as "milk soy protein intolerance" (MSPI). Some recommend that nursing mothers discontinue consumption of foods containing dairy or soy ingredients.[67] In opposition to this recommendation, a published scientific review stated that there was not yet sufficient evidence in the human trial literature to conclude that maternal dietary food avoidance during lactation would prevent or treat allergic symptoms in breastfed infants.[46]
A review presented information on milk allergy, soy allergy and cross-reactivity between the two. Milk allergy was described as occurring in 2.2% to 2.8% of infants and declining with age. Soy allergy was described as occurring in zero to 0.7% of young children. According to several studies cited in the review, between 10% and 14% of infants and young children with confirmed cow's milk allergy were determined to also be sensitized to soy and in some instances have a clinical reaction after consuming a soy-containing food. The research did not address whether the cause was two separate allergies or a cross-reaction resulting from a similarity in protein structure, as occurs for cow's milk and goat's milk.[53] Recommendations are that infants diagnosed as allergic to cow's milk infant formula should be switched to an extensively hydrolyzed protein formula rather than a soy whole-protein formula.[53][68]
Prognosis
Milk allergy typically presents in the first year of life. The majority of children outgrow milk allergy by the age of ten.[3][20] One large clinical trial reported resolutions of 19% by age 4 years, 42% by age 8 years, 64% by age 12 years, and 79% by 16 years.[9] Children are often better able to tolerate milk as an ingredient in baked goods relative to liquid milk. Childhood predictors for adult persistence are anaphylaxis, high milk-specific serum IgE, robust response to the skin prick test and absence of tolerance to milk-containing baked foods.[20] Resolution is more likely if baseline serum IgE is lower[9] or if IgE-mediated allergy is absent, leaving only cell-mediated, non-IgE allergy.[3] People with confirmed cow's milk allergy may also demonstrate an allergic response to beef, especially when cooked rare, because of the presence of bovine serum albumin.[69]
In U.S. government diet and health surveys conducted from 2007 to 2010, 6,189 children ages 2–17 were assessed. For those classified as allergic to cow's milk, mean weight, height and body-mass index were significantly lower than for their non-allergic peers. This was not true for children with other food allergies. Diet assessment showed a significant 23% reduction of calcium intake and near-significant trends for lower vitamin D and total calorie intake.[70]
Epidemiology
Incidence and prevalence are terms commonly used in describing disease epidemiology. Incidence is newly diagnosed cases, which can be expressed as new cases per year per million people. Prevalence is the number of cases alive, which may be expressed in terms of existing cases per million over a period of time.[71] The percentage of babies in developed countries with milk allergy is between 2% and 3%. This estimate is for antibody-based allergy; figures for allergy based on cellular immunity are unknown.[3] The percentage declines as children age. National survey data in the U.S. collected from 2005 to 2006 showed that from age six and older, the percentage with IgE-confirmed milk allergy was less than 0.4%.[22] For all age groups, a review conducted in Europe estimated that 0.6% had milk allergy.[10]
Regulation
Dairy allergy was one of the earliest food allergies to be recorded. An ancient Greek medical text attributed to the doctor Hippocrates (c. 460 – c. 370 BC) notes that some foods are harmful to certain individuals but not others, and "...cheese does not harm all men alike; some can eat their fill of it without the slightest hurt, nay, those it agrees with are wonderfully strengthened thereby. Others come off badly." The text attempts to explain the reaction to the cheese in terms of Hippocratic humorism, stating that some constitutions are naturally "hostile to cheese, and [are] roused and stirred to action under its influence."[72]
With the passage of mandatory labeling laws, food-allergy awareness has increased, with impacts on the quality of life for children, their parents and their immediate caregivers.[73][74][75][76] In the U.S., the Food Allergen Labeling and Consumer Protection Act of 2004 (FALCPA) mandates disclosure of allergen information on food packaging, and many restaurants have added allergen warnings to their menus. School systems maintain protocols regarding foods that cannot be brought into the school. Despite all of these precautions, people with serious allergies must maintain awareness that accidental exposure can occur in other peoples' homes, at school or in restaurants.[77]
Regulation of labeling

In response to the risk that certain foods pose to those with food allergies, some countries have responded by instituting labeling laws that require food products to clearly inform consumers if they contain major allergens or allergen byproducts among the ingredients intentionally added to foods. However, labeling laws do not mandate the declaration of the presence of trace amounts in the final product as a consequence of cross-contamination, except in Brazil.[12][13][15][18][59][60][61][19][excessive citations]
Ingredients intentionally added
In the US, FALCPA requires companies to disclose on the label whether a packaged food product contains a major food allergen added intentionally: cow's milk, peanuts, eggs, shellfish, fish, tree nuts, soy and wheat.
FALCPA applies to packaged foods regulated by the FDA, which does not include poultry, most meats, certain egg products, and most alcoholic beverages.[13] However, some meat, poultry, and egg processed products may contain allergenic ingredients, such as added milk proteins. These products are regulated by the Food Safety and Inspection Service (FSIS), which requires that any ingredient be declared in the labeling only by its common or usual name. Neither the identification of the source of a specific ingredient in a parenthetical statement nor the use of statements to alert for the presence of specific ingredients, like "Contains: milk", are mandatory according to FSIS.[60][61] FALCPA also does not apply to food prepared in restaurants.[12][78]
Trace amounts as a result of cross-contamination
The value of allergen labeling other than for intentional ingredients is controversial. This concerns labeling for ingredients present unintentionally as a consequence of cross-contact or cross-contamination at any point along the food chain (during raw material transportation, storage or handling, due to shared equipment for processing and packaging, etc.).[13][18] Experts in this field propose that if allergen labeling is to be useful to consumers, and healthcare professionals who advise and treat those consumers, ideally there should be agreement on which foods require labeling, threshold quantities below which labeling may be of no purpose, and validation of allergen detection methods to test and potentially recall foods that were deliberately or inadvertently contaminated.[79][80]
Labeling regulations have been modified to provide for mandatory labeling of ingredients plus voluntary labeling, termed precautionary allergen labeling (PAL), also known as "may contain" statements, for possible, inadvertent, trace amount, cross-contamination during production.[18][81] PAL labeling can be confusing to consumers, especially as there can be many variations on the wording of the warning.[81][82] As of 2014[update], PAL is regulated only in Switzerland, Japan, Argentina, and South Africa. Argentina decided to prohibit precautionary allergen labeling since 2010, and instead puts the onus on the manufacturer to control the manufacturing process and label only those allergenic ingredients known to be in the products. South Africa does not permit the use of PAL, except when manufacturers demonstrate the potential presence of allergen due to cross-contamination through a documented risk assessment despite adherence to Good Manufacturing Practice.[18] In Australia and New Zealand, there is a recommendation that PAL be replaced by guidance from VITAL 2.0 (Vital Incidental Trace Allergen Labelling). A review identified "the eliciting dose for an allergic reaction in 1% of the population" as 0.01 mg for cow's milk. This threshold reference dose (and similar results for egg, peanut and other proteins) will provide food manufacturers with guidance for developing precautionary labelling and give consumers a better idea of what might be accidentally in a food product beyond "may contain."[58][83] VITAL 2.0 was developed by the Allergen Bureau, a food industry-sponsored, non-government organization.[84] The EU has initiated a process to create labeling regulations for unintentional contamination but it is not expected to be published before 2024.[85]
Lack of compliance with labeling regulations is also a problem. As an example, the FDA documented failure to list milk as an ingredient in
In Brazil, since April 2016, the declaration of the possibility of cross-contamination is mandatory when the product does not intentionally add any allergenic food or its derivatives, but the Good Manufacturing Practices and allergen control measures adopted are not sufficient to prevent the presence of accidental trace amounts. Milk of all species of mammalians is included among these allergenic foods.[19]
Society and culture
Food fear has a significant impact on quality of life.[75][76] For children with allergies, their quality of life is also affected by the actions of their peers. An increased occurrence of bullying has been observed, which can include threats or deliberate acts of forcing allergic children to contact foods that they must avoid or intentional contamination of allergen-free food.[87]
Research
There is research – not specific to milk allergy – on the use of
See also
- Lactose intolerance
- List of allergens (food and non-food)
- Plant milk
References
- ^ a b c d MedlinePlus Encyclopedia: Food allergy
- ^ PMID 20205781.
- ^ PMID 25257836.
- ^ S2CID 21493978.
- PMID 31117223.
- ^ S2CID 11054771.
- ^ "Choosing Wisely: Don't rely on antihistamines as firstline treatment in severe allergic reactions". American Academy of Family Physicians. Archived from the original on 20 October 2021. Retrieved 28 August 2022.
- from the original on 2022-08-28. Retrieved 2022-09-08.
- ^ PMID 17935766.
- ^ S2CID 28692645.
- ^ "Asthma and Allergy Foundation of America". Archived from the original on 6 October 2012. Retrieved 23 December 2012.
- ^ a b c d e "Food Allergen Labeling and Consumer Protection Act of 2004 Questions and Answers". Food and Drug Administration. Archived from the original on 31 October 2017. Retrieved 29 September 2017.
- ^ a b c d e f g "Food Allergies: What You Need to Know". Food and Drug Administration. 18 December 2017. Archived from the original on 25 January 2018. Retrieved 12 January 2018.
- ^ PMID 25178179.
- ^ a b c "Food allergen labelling and information requirements under the EU Food Information for Consumers Regulation No. 1169/2011: Technical Guidance" (PDF). April 2015. Archived from the original (PDF) on 2015-09-10 – via Gov.uk.
- ^ S2CID 25204657.
- from the original on 2019-08-09. Retrieved 2019-07-06.
- ^ PMID 24791183.
- ^ a b c "Guia sobre Programa de Controle de Alergênicos". Agência Nacional de Vigilância Sanitária (in Brazilian Portuguese). 2016. Archived from the original on 29 April 2018. Retrieved 7 April 2018.
- ^ PMID 25459576.
- PMID 28698533.
- ^ PMID 20920770.
- ^ PMID 25345300.
- ^ S2CID 25333442.
- ^ S2CID 19972281.
- ^ PMID 24388012.
- PMID 28852472.
- ^ S2CID 207324496.
- ^ S2CID 6619743.
- ^ PMID 28167094.
- NHS Choices. 16 May 2016. Archivedfrom the original on 20 July 2017. Retrieved 31 January 2017.
A food allergy is when the body's immune system reacts unusually to specific foods
- ^ Food Reactions. Allergies Archived 2010-04-16 at the Wayback Machine. Foodreactions.org. Kent, England. 2005. Accessed 27 Apr 2010.
- ^ Mayo Clinic. Causes of Food Allergies. Archived 2010-02-27 at the Wayback Machine April 2010.
- ^ ISBN 978-0-8153-4101-7. Archivedfrom the original on 2009-06-28.
- ^ PMID 17011762.
- S2CID 40819814.
- PMID 29025431.
- ^ PMID 29270244.
- S2CID 6651513.
- S2CID 207328783.
- PMID 26393648.
- PMID 16951027.
- ^ a b c d e "Lactose Intolerance". NIDDK. June 2014. Archived from the original on 25 October 2016. Retrieved 25 October 2016.
- PMID 26978392.
- S2CID 23987626.
- ^ PMID 25404609.
- ^ from the original on 2020-10-29. Retrieved 2018-09-25.
- PMID 10452771.
- PMID 19685855.
- ^ PMID 27895813.
- ^ Labeling of Infant Formula: Guidance for Industry Archived 2017-05-02 at the Wayback Machine U.S. Food and Drug Administration (2016) Accessed 11 December 2017.
- PMID 26956579.
- ^ PMID 21453810.
- S2CID 204981786.
- ^ PMID 23152278.
- PMID 14567487.
- S2CID 41402604.
- ^ PMID 23987796.
- ^ a b c d e f "Have Food Allergies? Read the Label". Food and Drug Administration. 14 December 2017. Archived from the original on 12 November 2020. Retrieved 14 January 2018.
- ^ a b c "Food Ingredients of Public Health Concern" (PDF). United States Department of Agriculture. Food Safety and Inspection Service. 7 March 2017. Archived from the original (PDF) on 17 February 2018. Retrieved 16 February 2018.
- ^ a b c "Allergies and Food Safety". United States Department of Agriculture. Food Safety and Inspection Service. 1 December 2016. Archived from the original on 17 February 2018. Retrieved 16 February 2018.
- ^ University of Wisconsin Hospital and Clinics. Clinical Nutrition Services Department and the Department of Nursing. 2015. Archived(PDF) from the original on 15 January 2018. Retrieved 14 January 2018.
- ^ FDA (12 October 2014). "Finding Food Allergens Where They Shouldn't Be". Food and Drug Administration. Archived from the original on 23 April 2019. Retrieved 11 February 2018.
- PMID 25800671.
- S2CID 33691910.
- S2CID 41223984.
- ^ "Milk Soy Protein Intolerance (MSPI)". dhhs.ne.gov. 2017. Archived from the original on 14 January 2018. Retrieved 14 February 2018.
- PMID 18450914.
- PMID 10869903.
- PMID 25312758.
- ^ "What is Prevalence?" Archived 2020-12-26 at the Wayback Machine National Institute of Mental Health (Accessed 25 December 2020).
- ISBN 978-0-231-53919-7.
- PMID 25725570.
- PMID 25668890.
- ^ PMID 26120535.
- ^ S2CID 326837.
- PMID 18751571.
- PMID 24505841.
- S2CID 40395908.
- PMID 26022883.
- ^ S2CID 18362869.
- S2CID 21326926.
- PMID 24184597.
- ^ The VITAL Program Archived 2020-11-29 at the Wayback Machine Allergen Bureau, Australia and New Zealand.
- PMID 29202901.
- ^ "Consumer Updates – Dark Chocolate and Milk Allergies". FDA. 2017. Archived from the original on 14 December 2019. Retrieved 14 February 2018.
- S2CID 9719096.
- PMID 21277625.
- PMID 23009174.
- ^ http://acaai.org/allergies/allergy-treatment/allergy-immunotherapy/sublingual-immunotherapy-slit/ Archived 2021-01-25 at the Wayback Machine Sublingual Therapy (SLIT) American College of Allergy, Asthma and Immunology
- PMID 26810481.
- ^ PMID 26044853.
- ^ PMID 23543544.
- PMID 26198702.
- S2CID 206999857.
- PMID 26937896.

