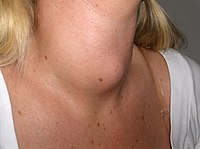
Goitre
| Goitre | |
|---|---|
| Other names | Goiter |
 | |
| Diffuse hyperplasia of the thyroid | |
| Specialty | Endocrinology |
A goitre, or goiter, is a swelling in the neck resulting from an enlarged thyroid gland.[1][2] A goitre can be associated with a thyroid that is not functioning properly.
Worldwide, over 90% of goitre cases are caused by iodine deficiency.[3] The term is from the Latin gutturia, meaning throat. Most goitres are not cancerous (benign), though they may be potentially harmful.
Signs and symptoms
A goitre can present as a palpable or visible enlargement of the
According to the WHO classification of goitre by palpation, the severity of goitre is currently graded as grade 0, grade 1, grade 2.[5]
-
Goitre Class II, WHO grade 2
-
Goitre Class III, WHO grade 2
Causes
Worldwide, the most common cause for goitre is
| Cause | Pathophysiology | Resultant thyroid activity | Growth pattern | Treatment | Incidence and prevalence | Prognosis |
|---|---|---|---|---|---|---|
| Iodine deficiency | Hyperplasia of thyroid to compensate for decreased efficacy | Can cause hypothyroidism | Diffuse | Iodine | Constitutes over 90% cases of goitre worldwide[3] | Increased size of thyroid may be permanent if untreated for around five years |
| Congenital hypothyroidism | Inborn errors of thyroid hormone synthesis | Hypothyroidism | ||||
| Goitrogen ingestion | ||||||
| Adverse drug reactions | ||||||
| Hashimoto's thyroiditis | Autoimmune disease in which the thyroid gland is gradually destroyed. Infiltration of lymphocytes. | Hypothyroidism | Diffuse and lobulated[8] |
Thyroid hormone replacement |
Prevalence: 1 to 1.5 in a 1000 | Remission with treatment |
| Pituitary disease | Hypersecretion of thyroid stimulating hormone, almost always by a pituitary adenoma[9] |
Diffuse | Pituitary surgery | Very rare[9] | ||
| Graves' disease—also called Basedow syndrome | Autoantibodies (TSHR-Ab) that activate the TSH -receptor (TSHR) |
Hyperthyroidism | Diffuse | Antithyroid agents, radioiodine, surgery | Will develop in about 0.5% of males and 3% of females | Remission with treatment, but still lower quality of life for 14 to 21 years after treatment, with lower mood and lower vitality, regardless of the choice of treatment[10] |
| Thyroiditis | Acute or chronic inflammation | Can be hyperthyroidism initially, but progress to hypothyroidism | ||||
| Thyroid cancer | Usually uninodular | Overall relative 5-year survival rate of 85% for females and 74% for males[11]
| ||||
| Benign thyroid neoplasms | Usually hyperthyroidism | Usually uninodular | Mostly harmless[12] | |||
Thyroid hormone insensitivity |
Secretional hyperthyroidism, Symptomatic hypothyroidism |
Diffuse |
- Sarcoidosis
- Amyloidosis
- Hydatidiform mole
- Cysts
- Acromegaly
- Pendred syndrome
Diagnosis

Goitre may be diagnosed via a
Types
A goitre may be classified either as nodular or diffuse. Nodular goitres are either of one nodule (uninodular) or of multiple nodules (multinodular).[14] Multinodular goiter (MNG) is the most common disorder of the thyroid gland.[15]
- Growth pattern
- Uninodular goitre: one thyroid nodule; can be either inactive, or active (toxic) – autonomously producing thyroid hormone.
- Multinodular goitre: multiple nodules;[16] can likewise be inactive or toxic, the latter is called toxic multinodular goitre and associated with hyperthyroidism. These nodules grow up at varying rates and secrete thyroid hormone autonomously, thereby suppressing TSH-dependent growth and function in the rest of gland. Inactive nodules in the same goitre can be malignant.[17] Thyroid cancer is identified in 13.7% of the patients operated for multinodular goitre.[18]
- Diffuse goitre: the whole thyroid appearing to be enlarged due to hyperplasia.
- Size
- Class I: the goitre in normal posture of the head cannot be seen; it is only found by palpation.
- Class II: the goitre is palpable and can be easily seen.
- Class III: the goitre is very large and is retrosternal (partially or totally lying below the sternum), pressure results in compression marks.
Treatment
Goitre is treated according to the cause. If the
Epidemiology

Goitre is more common among women, but this includes the many types of goitre caused by autoimmune problems, and not only those caused by simple lack of iodine.[21]
Iodine mainly accumulates in the sea and in the topsoil. Before iodine enrichment programs, goiters was common in areas with repeated flooding or glacial activities, which erodes the topsoil. It is endemic in populations where the intake of iodine is less than 10 µg per day.[22]
Examples of such regions include the alpine regions of Southern Europe (such as Switzerland), the Himalayans, the Great Lakes basin, etc. As reported in 1923, all the domestic animals have goiter in some of the glacial valleys of Southern Alaska. It was so severe in Pemberton Meadows that it was difficult to raise young animals there.[23]
History


Chinese physicians of the Tang dynasty (618–907) were the first to successfully treat patients with goitre by using the iodine-rich thyroid gland of animals such as sheep and pigs—in raw, pill, or powdered form.[24] This was outlined in Zhen Quan's (d. 643 AD) book, as well as several others.[24] One Chinese book, The Pharmacopoeia of the Heavenly Husbandman, asserted that iodine-rich sargassum was used to treat goitre patients by the 1st century BC, but this book was written much later.[24]
In the 12th century,
Paracelsus (1493–1541) was the first person to propose a relationship between goitre and minerals (particularly lead) in drinking water.[29] Iodine was later discovered by Bernard Courtois in 1811 from seaweed ash.[30]
Goitre was previously common in many areas that were deficient in iodine in the
Goitre had been prevalent in the alpine countries for a long time. Switzerland reduced the condition by introducing
Society and culture
In the 1920s wearing bottles of iodine around the neck was believed to prevent goitre.[35]
Notable cases
- Former U.S. President
Heraldry
The coat of arms and crest of Die Kröpfner, of
See also
- David Marine conducted substantial research on the treatment of goitre with iodine.
- Endemic goitre
- Struma ovarii—a kind of teratoma
- Thyroid hormone receptor
References
- ^ "Thyroid Nodules and Swellings". British Thyroid Foundation. 11 September 2019.
- ^ "Goitre - NHS Choices". NHS Choices. 19 October 2017.
- ^ ISBN 3-936072-27-2.)
{{cite book}}: CS1 maint: location missing publisher (link - ^ Porth CM, Gaspard KJ, Noble KA (2011). Essentials of pathophysiology: Concepts of altered health states (3rd ed.). Philadelphia, PA: Wolters Kluwer/Lippincott Williams & Wilkins.
- ^ "Goitre as a determinant of the prevalence and severity of iodine deficiency disorders in populations". World Health Organization. 2014.
- ISBN 978-1-4160-2973-1.
- ^ "Toxicological Profile For Cyanide" (PDF). Atsdr.cdc.gov. Archived (PDF) from the original on 28 July 2004. Retrieved 16 March 2017.
- PMID 21119426.
- ^ a b Thyrotropin (TSH)-secreting pituitary adenomas. By Roy E Weiss and Samuel Refetoff. Last literature review version 19.1: January 2011. This topic last updated: July 2, 2009
- PMID 16356093.
- ISBN 978-3-540-22309-2.
- S2CID 34137703.
- ^ "Goitre". nhs.uk. 19 October 2017. Retrieved 27 March 2019.
- ^ "Nodular Goiter - an overview | ScienceDirect Topics". www.sciencedirect.com. Retrieved 6 March 2022.
- PMID 25905424.
- S2CID 38834260.
- ^ "Toxic multinodular goitre - Symptoms, diagnosis and treatment | BMJ Best Practice". bestpractice.bmj.com.
- PMID 15481700.
- ^ "Goiter – Simple". The New York Times.
- ^ "Mortality and Burden of Disease Estimates for WHO Member States in 2002" (xls). World Health Organization. 2002.
- ^ 1
- ^ Goitre as a determinant of the prevalence and severity of iodine deficiency disorders in populations, World Health Organization - 2014
- PMID 18010882.
- ^ ISBN 0-671-62028-2.
- Who Named It?– the history and naming of the disease
- PMID 6355710.
- Who Named It?
- PMID 9771526.
- ^ "Paracelsus" Britannica
- S2CID 109845199.
- ^ "Iodine Deficiency".
- PMID 888801.
- ^ "In Raising the World's I.Q., the Secret's in the Salt", article by Donald G. McNeil, Jr., December 16, 2006, The New York Times
- ^ Wissen, Planet (16 March 2017). "Planet Wissen".
- ^ "ARCHIVED – Why take iodine?". Nrc-cnrc.gc.ca. 30 September 2011. Retrieved 1 November 2012.
- ISBN 978-0-06-008149-2.
- ^ Altman LK (14 September 1991). "A White House Puzzle: Immunity Ailments". The New York Times.
Doctors Say Bush Is in Good Health
- ^ Altman LK (28 May 1991). "The Doctor's World; A White House Puzzle: Immunity Ailments". The New York Times.
- ^ Fox-Davies AC (1904). The Art of Heraldry: An Encyclopædia of Armory. New York and London: Benjamin Blom, Inc. p. 413.