Pulmonary contusion
| Pulmonary contusion or Lung contusion | |
|---|---|
| Other names | Lung contusion |
 | |
| A CT scan showing a pulmonary contusion (red arrow) accompanied by a rib fracture (purple arrow) | |
| Specialty | Emergency medicine |
A pulmonary contusion, also known as lung contusion, is a
A pulmonary contusion is usually caused directly by blunt trauma but can also result from explosion injuries or a shock wave associated with penetrating trauma. With the use of explosives during World Wars I and II, pulmonary contusion resulting from blasts gained recognition. In the 1960s its occurrence in civilians began to receive wider recognition, in which cases it is usually caused by traffic accidents. The use of seat belts and airbags reduces the risk to vehicle occupants.
Diagnosis is made by studying the cause of the injury,
The severity ranges from mild to severe: small contusions may have little or no impact on health, yet pulmonary contusion is the most common type of potentially lethal chest trauma. It occurs in 30–75% of severe chest injuries. The risk of death following a pulmonary contusion is between 14 and 40%. Pulmonary contusion is usually accompanied by other injuries. Although associated injuries are often the cause of death, pulmonary contusion is thought to cause death directly in a quarter to half of cases. Children are at especially high risk for the injury because the relative flexibility of their bones prevents the chest wall from absorbing force from an impact, causing it to be transmitted instead to the lung. Pulmonary contusion is associated with complications including pneumonia and acute respiratory distress syndrome, and it can cause long-term respiratory disability.
Classification

Pulmonary contusion and laceration are injuries to the lung tissue.
Signs and symptoms
Presentation may be subtle; people with mild contusion may have no symptoms at all.
Signs and symptoms take time to develop, and as many as half of cases are asymptomatic at the initial presentation.[5] The more severe the injury, the more quickly symptoms become apparent. In severe cases, symptoms may occur as quickly as three or four hours after the trauma.[11] Hypoxemia (low oxygen concentration in the arterial blood) typically becomes progressively worse over 24–48 hours after injury.[14] In general, pulmonary contusion tends to worsen slowly over a few days,[4] but it may also cause rapid deterioration or death if untreated.[6]
Causes
Pulmonary contusion is the most common injury found in blunt chest trauma,[15] occurring in 25–35% of cases.[16] It is usually caused by the rapid deceleration that results when the moving chest strikes a fixed object.[12] About 70% of cases result from motor vehicle collisions,[17] most often when the chest strikes the inside of the car.[6] Falls,[17] assaults,[18] and sports injuries are other causes.[19] Pulmonary contusion can also be caused by explosions; the organs most vulnerable to blast injuries are those that contain gas, such as the lungs.[20] Blast lung is severe pulmonary contusion, bleeding, or edema with damage to alveoli and blood vessels, or a combination of these.[21] This is the primary cause of death among people who initially survive an explosion.[22] Unlike other mechanisms of injury in which pulmonary contusion is often found alongside other injuries, explosions can cause pulmonary contusion without damage to the chest wall.[15]
In addition to
Mechanism
The physical processes behind pulmonary contusion are poorly understood. However, it is known that lung tissue can be crushed when the chest wall bends inward on impact.[26] Three other possible mechanisms have been suggested: the inertial effect, the spalling effect, and the implosion effect.
- In the inertial effect, the lighter alveolar tissue is hilar structures, an effect similar to diffuse axonal injury in head injury.[5] It results from the fact that different tissues have different densities, and therefore different rates of acceleration or deceleration.[10]
- In the spalling effect, lung tissue bursts or is sheared where a shock wave meets the lung tissue, at interfaces between gas and liquid.[20] The alveolar walls form such a gas-liquid interface with the air in the alveoli.[5][27] The spalling effect occurs in areas with large differences in density; particles of the denser tissue are spalled (thrown) into the less dense particles.[28]
- The implosion effect occurs when a pressure wave passes through a tissue containing bubbles of gas: the bubbles first implode, then rebound and expand beyond their original volume.[29] The air bubbles cause many tiny explosions, resulting in tissue damage;[29] the overexpansion of gas bubbles stretches and tears alveoli.[30][31] This effect is thought to occur microscopically when the pressure in the airways increases sharply.[26]
Contusion usually occurs on the lung directly under the site of impact, but, as with traumatic brain injury, a contrecoup contusion may occur at the site opposite the impact as well.[24] A blow to the front of the chest may cause contusion on the back of the lungs because a shock wave travels through the chest and hits the curved back of the chest wall; this reflects the energy onto the back of the lungs, concentrating it. (A similar mechanism may occur at the front of the lungs when the back is struck.)[31]
The amount of energy transferred to the lung is determined in a large part by the compliance (flexibility) of the chest wall.[24] Children's chests are more flexible because their ribs are more elastic and there is less ossification of their intercostal cartilage.[13] Therefore, their chest walls bend, absorbing less of the force and transmitting more of it to the underlying organs.[13][32] An adult's more bony chest wall absorbs more of the force itself rather than transmitting it.[32] Thus children commonly get pulmonary contusions without fractures overlying them, while elderly people are more likely to develop fractures than contusions.[14][24] One study found that pulmonary contusions were accompanied by fractures 62% of the time in children and 80% of the time in adults.[31]
Pathophysiology

Pulmonary contusion results in bleeding and fluid leakage into lung tissue, which can become stiffened and lose its normal elasticity. The water content of the lung increases over the first 72 hours after injury, potentially leading to frank pulmonary edema in more serious cases.[20] As a result of these and other pathological processes, pulmonary contusion progresses over time and can cause hypoxia (insufficient oxygen).
Bleeding and edema
In contusions, torn
Consolidation and collapse
Pulmonary contusion can cause parts of the lung to
Ventilation/perfusion mismatch
Normally, the
Diagnosis
To diagnose pulmonary contusion, health professionals use clues from a physical examination, information about the event that caused the injury, and radiography.[17] Laboratory findings may also be used; for example, arterial blood gasses may show insufficient oxygen and excessive carbon dioxide even in someone receiving supplemental oxygen.[35] However, blood gas levels may show no abnormality early in the course of pulmonary contusion.[23]
X-ray
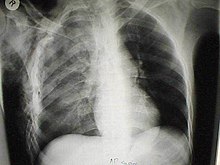
Although chest radiography is an important part of the diagnosis, it is often not sensitive enough to detect the condition early after the injury.[35] In a third of cases, pulmonary contusion is not visible on the first chest radiograph performed.[7] It takes an average of six hours for the characteristic white regions to show up on a chest X-ray, and the contusion may not become apparent for 48 hours.[7][27][43] When a pulmonary contusion is apparent in an X-ray, it suggests that the trauma to the chest was severe and that a CT scan might reveal other injuries that were missed with X-ray.[2]
Computed tomography

Ultrasound

Pulmonary
Prevention
Prevention of pulmonary contusion is similar to that of other chest trauma. Airbags in combination with seat belts can protect vehicle occupants by preventing the chest from striking the interior of the vehicle during a collision, and by distributing forces involved in the crash more evenly across the body.[6] However, in rare cases, an airbag causes pulmonary contusion in a person who is not properly positioned when it deploys.[50] Child restraints such as carseats protect children in vehicle collisions from pulmonary contusion.[51] Equipment exists for use in some sports to prevent chest and lung injury; for example, in softball the catcher is equipped with a chest protector.[52] Athletes who do not wear such equipment, such as basketball players, can be trained to protect their chests from impacts.[52] Protective garments can also prevent pulmonary contusion in explosions.[53] Although traditional body armor made from rigid plates or other heavy materials protects from projectiles generated by a blast, it does not protect against pulmonary contusion, because it does not prevent the blast's shock wave from being transferred to the lung.[53] Special body armor has been designed for military personnel at high risk for blast injuries; these garments can prevent a shock wave from being propagated across the chest wall to the lung, and thus protect wearers from blast lung injuries.[53] These garments alternate layers of materials with high and low acoustic impedance (the product of a material's density and a wave's velocity through it) in order to "decouple" the blast wave, preventing its propagation into the tissues.[53]
Treatment
No treatment is known to speed the healing of a pulmonary contusion; the main care is supportive.
Ventilation
People with signs of inadequate
Pulmonary contusion or its complications such as acute respiratory distress syndrome may cause lungs to lose
Fluid therapy
The administration of
Supportive care
Retaining secretions in the airways can worsen hypoxia
Prognosis

Pulmonary contusion usually resolves itself
Complications

Pulmonary contusion can result in respiratory failure—about half of such cases occur within a few hours of the initial trauma.[43] Other severe complications, including infections and acute respiratory distress syndrome (ARDS) occur in up to half of cases.[31] Elderly people and those who have heart, lung, or kidney disease prior to the injury are more likely to stay longer in hospital and have complications from the injury. Complications occur in 55% of people with heart or lung disease and 13% of those without.[37] Of people with pulmonary contusion alone, 17% develop ARDS, while 78% of people with at least two additional injuries develop the condition.[6] A larger contusion is associated with an increased risk. In one study, 82% of people with 20% or more of the lung volume affected developed ARDS, while only 22% of people with less than 20% did so.[7]
Associated injuries

A large amount of force is required to cause pulmonary contusion; a person injured with such force is likely to have other types of injuries as well.[23] In fact, pulmonary contusion can be used to gauge the severity of trauma.[25] Up to three quarters of cases are accompanied by other chest injuries,[39] the most common of these being hemothorax and pneumothorax.[37] Flail chest is usually associated with significant pulmonary contusion,[15] and the contusion, rather than the chest wall injury, is often the main cause of respiratory failure in people with these injuries.[69] Other indications of thoracic trauma may be associated, including fracture of the sternum and bruising of the chest wall.[63] Over half of fractures of the scapula are associated with pulmonary contusion.[27] The contusion is frequently found underlying fracture sites.[35] When accompanied by a fracture, it is usually concentrated into a specific location—the contusion is more diffuse when there is no fracture.[31][43] Pulmonary lacerations may result from the same blunt or penetrating forces that cause contusion.[6] Lacerations can result in pulmonary hematomas; these are reported to develop in 4–11% of pulmonary contusions.[6]
Epidemiology
Pulmonary contusion is found in 30–75% of severe cases of chest injury, making it the most common serious injury to occur in association with
Pulmonary contusion is the most common cause of death among vehicle occupants involved in accidents,[72] and it is thought to contribute significantly in about a quarter of deaths resulting from vehicle collisions.[25] As vehicle use has increased, so has the number of auto accidents, and with it the number of chest injuries.[39] However an increase in the number of airbags installed in modern cars may be decreasing the incidence of pulmonary contusion.[6] Use of child restraint systems has brought the approximate incidence of pulmonary contusion in children in vehicle accidents from 22% to 10%.[51]
Differences in the bodies of children and adults lead to different manifestations of pulmonary contusion and associated injuries; for example, children have less body mass, so the same force is more likely to lead to trauma in multiple body systems.[31] Since their chest walls are more flexible, children are more vulnerable to pulmonary contusion than adults are,[23] and thus suffer from the injury more commonly.[30] Pulmonary contusion has been found in 53% of children with chest injuries requiring hospitalization.[73] Children in forceful impacts suffer twice as many pulmonary contusions as adults with similar injury mechanisms, yet have proportionately fewer rib fractures.[13] The rates of certain types of injury mechanisms differ between children and adults; for example, children are more often hit by cars as pedestrians.[31] Some differences in children's physiology might be advantageous (for example they are less likely to have other medical conditions), and thus they have been predicted to have a better outcome.[74] However, despite these differences, children with pulmonary contusion have similar mortality rates to adults.[31]
History

In 1761, the Italian anatomist Giovanni Battista Morgagni was first to describe a lung injury that was not accompanied by injury to the chest wall overlying it.[20] Nonetheless, it was the French military surgeon Guillaume Dupuytren who is thought to have coined the term pulmonary contusion in the 19th century.[71] It still was not until the early 20th century that pulmonary contusion and its clinical significance began to receive wide recognition.[70] With the use of explosives during World War I came many casualties with no external signs of chest injury but with significant bleeding in the lungs.[70] Studies of World War I injuries by D.R. Hooker showed that pulmonary contusion was an important part of the concussive injury that results from explosions.[70]
Pulmonary contusion received further attention during World War II, when the bombings of Britain caused blast injuries and associated respiratory problems in both soldiers and civilians.[20] Also during this time, studies with animals placed at varying distances from a blast showed that protective gear could prevent lung injuries.[65] These findings suggested that an impact to the outside of the chest wall was responsible for the internal lesions.[65] In 1945, studies identified a phenomenon termed "wet lung", in which the lungs accumulated fluid and were simultaneously less able to remove it.[20][75] They attributed the respiratory failure often seen in blunt chest trauma in part to excessive fluid resuscitation, and the question of whether and how much to administer fluids has remained controversial ever since.[20]
During the Vietnam War, combat again provided the opportunity for study of pulmonary contusion; research during this conflict played an important role in the development of the modern understanding of its treatment.
References
- ^ ISBN 978-0-7817-6314-1.
- ^ S2CID 22311233.
- ISBN 0-397-51732-7.
- ^ ISBN 0-07-137069-2.
- ^ PMID 16849051.
- ^ a b c d e f g h i j k l m n o
Miller DL, Mansour KA (2007). "Blunt traumatic lung injuries". Thoracic Surgery Clinics. 17 (1): 57–61. PMID 17650697.
- ^ PMID 14979330.
- ISBN 1-4051-0461-9.
- ISBN 0-7295-3743-9.
- ^ a b c
Boyd AD (1989). "Lung injuries". In Hood RM, Boyd AD, Culliford AT (eds.). Thoracic Trauma. Philadelphia: Saunders. pp. 153–155. ISBN 0-7216-2353-0.
- ^ S2CID 1919039.
- ^ PMID 15732422.
- ^ a b c d e f g
Tovar JA (2008). "The lung and pediatric trauma". Seminars in Pediatric Surgery. 17 (1): 53–59. PMID 18158142.
- ^ ISBN 978-0-7817-6275-5.
- ^ PMID 23114493.
- ^ a b c
Moloney JT, Fowler SJ, Chang W (February 2008). "Anesthetic management of thoracic trauma". Current Opinion in Anesthesiology. 21 (1): 41–46. S2CID 39075971.
- ^ a b c d e f g h i j
Ullman EA, Donley LP, Brady WJ (2003). "Pulmonary trauma emergency department evaluation and management". Emergency Medicine Clinics of North America. 21 (2): 291–313. PMID 12793615.
- ^
Haley K, Schenkel K (2003). "Thoracic trauma". In Thomas DO, Bernardo LM, Herman B (eds.). Core curriculum for pediatric emergency nursing. Sudbury, Mass: Jones and Bartlett Publishers. pp. 446. ISBN 0-7637-0176-9.
- ^
France R (2003). "The chest and abdomen". Introduction to Sports Medicine and Athletic Training. Thomson Delmar Learning. pp. 506–507. ISBN 1-4018-1199-X.
- ^ PMID 9191684.
- ^
Sasser SM, Sattin RW, Hunt RC, Krohmer J (2006). "Blast lung injury". Prehospital Emergency Care. 10 (2): 165–72. S2CID 2912045.
- ^
Born CT (2005). "Blast trauma: The fourth weapon of mass destruction" (PDF). Scandinavian Journal of Surgery. 94 (4): 279–285. S2CID 44680290. Archived from the original(PDF) on 25 February 2009.
- ^ a b c d e f
Lucid WA, Taylor TB (2002). "Thoracic trauma". In Strange GR (ed.). Pediatric Emergency Medicine: A Comprehensive Study Guide. New York: McGraw-Hill, Medical Publishing Division. pp. 92–100. ISBN 0-07-136979-1.
- ^ ISBN 1-4020-7215-5.
- ^ a b c d e
Stern EJ, White C (1999). Chest Radiology Companion. Hagerstown, MD: Lippincott Williams & Wilkins. p. 80. ISBN 0-397-51732-7.
- ^ .
- ^ a b c d e f g h i j k
Allen GS, Coates NE (November 1996). "Pulmonary contusion: A collective review". The American Surgeon. 62 (11): 895–900. PMID 8895709.
- ^ Maxson TR (2002). "Management of pediatric trauma: Blast victims in a mass casualty incident". Clinical Pediatric Emergency Medicine. 3 (4): 256–261. .
- ^ a b
Bridges EJ (September 2006). "Blast injuries: From triage to critical care". Critical Care Nursing Clinics of North America. 18 (3): 333–348. PMID 16962455.
- ^ a b c
Matthay RA, George RB, Light RJ, Matthay MA, eds. (2005). "Thoracic trauma, surgery, and perioperative management". Chest Medicine: Essentials of Pulmonary and Critical Care Medicine. Hagerstown, MD: Lippincott Williams & Wilkins. p. 578. ISBN 0-7817-5273-6.
- ^ a b c d e f g h i j k l m
Allen GS, Cox CS (December 1998). "Pulmonary contusion in children: Diagnosis and management". Southern Medical Journal. 91 (12): 1099–1106. S2CID 28583201.
- ^ a b c
Sartorelli KH, Vane DW (May 2004). "The diagnosis and management of children with blunt injury of the chest". Seminars in Pediatric Surgery. 13 (2): 98–105. PMID 15362279.
- ^ ISBN 0-7817-5074-1.
- ISBN 0-7817-5561-1.
- ^ PMID 11759554.
- ISBN 0-443-05841-5.
- ^ a b c d e f g
Klein Y, Cohn SM, Proctor KG (February 2002). "Lung contusion: Pathophysiology and management". Current Opinion in Anesthesiology. 15 (1): 65–68. S2CID 34262617.
- ^ a b c d e f
Bastos R, Calhoon JH, Baisden CE (2008). "Flail chest and pulmonary contusion". Seminars in Thoracic and Cardiovascular Surgery. 20 (1): 39–45. PMID 18420125.
- ^ a b c d e f g h i j k l m
Sutyak JP, Wohltmann CD, Larson J (2007). "Pulmonary contusions and critical care management in thoracic trauma". Thoracic Surgical Clinics. 17 (1): 11–23. PMID 17650693.
- ^ a b c
Prentice D, Ahrens T (August 1994). "Pulmonary complications of trauma". Critical Care Nursing Quarterly. 17 (2): 24–33. S2CID 29662985.
- ^ a b c d e f g
Kishen R, Lomas G (2003). "Thoracic trauma". In Gwinnutt CL, Driscoll P (eds.). Trauma Resuscitation: The Team Approach. Informa Healthcare. pp. 55–64. ISBN 1-85996-009-X.
- ^
Fish RM (2003). "Diagnosis and treatment of blast injury". In Fish RM, Geddes LA, Babbs CF (eds.). Medical and Bioengineering Aspects of Electrical Injuries. Tucson, AZ: Lawyers & Judges Publishing. p. 55. ISBN 1-930056-08-7.
- ^ PMID 18420127.
- ISBN 3-540-43557-3.
- ^
Keel M, Meier C (December 2007). "Chest injuries — what is new?". Current Opinion in Critical Care. 13 (6): 674–679. S2CID 19317500.
- ^
Miller LA (March 2006). "Chest wall, lung, and pleural space trauma". Radiologic Clinics of North America. 44 (2): 213–224, viii. PMID 16500204.
- ISBN 0-7817-3889-X.
- PMID 9372688.
- PMID 16899855. Archived from the originalon 3 May 2007.
- PMID 18072996.
- ^ a b
Cullen ML (March 2001). "Pulmonary and respiratory complications of pediatric trauma". Respiratory Care Clinics of North America. 7 (1): 59–77. PMID 11584805.
- ^ ISBN 978-0-7637-4949-1.
- ^ PMID 8606389.
- ^
Ridley SC (1998). "Surgery for adults". In Pryor JA, Webber BR (eds.). Physiotherapy for Respiratory and Cardiac Problems. Edinburgh: Churchill Livingstone. pp. 316. ISBN 0-443-05841-5.
- ^
Ruddy RM (March 2005). "Trauma and the paediatric lung". Paediatric Respiratory Reviews. 6 (1): 61–67. PMID 15698818.
- ^ a b
Pettiford BL, Luketich JD, Landreneau RJ (February 2007). "The management of flail chest". Thoracic Surgery Clinics. 17 (1): 25–33. PMID 17650694.
- ^
Dueck R (December 2006). "Alveolar recruitment versus hyperinflation: A balancing act". Current Opinion in Anesthesiology. 19 (6): 650–654. S2CID 41312348.
- ^
Anantham D, Jagadesan R, Tiew PE (2005). "Clinical review: Independent lung ventilation in critical care". Critical Care. 9 (6): 594–600. PMID 16356244.
- ^
Smith M, Ball V (1998). "Thoracic trauma". Cardiovascular/respiratory physiotherapy. St. Louis: Mosby. p. 221. ISBN 0-7234-2595-7.
- ^
Danne PD, Hunter M, MacKillop AD (2003). "Airway control". In Moore EE, Feliciano DV, Mattox KL (eds.). Trauma. Fifth Edition. McGraw-Hill Professional. p. 183. ISBN 0-07-137069-2.
- PMID 8650276.
- ^ ISBN 0-07-137069-2.
- ^ ISBN 0-7817-5003-2.
- PMID 17767714.
- ^ PMID 8810987.
- ISBN 978-0-7817-7138-2.
- ISBN 978-0-7817-7138-2.
- PMID 18394149.
- ^
Hemmila MR, Wahl WL (2005). "Management of the injured patient". In Doherty GM (ed.). Current Surgical Diagnosis and Treatment. McGraw-Hill Medical. p. 214. ISBN 0-07-142315-X.
- ^ a b c d e EAST practice management workgroup for pulmonary contusion — flail chest: Simon B, Ebert J, Bokhari F, Capella J, Emhoff T, Hayward T; et al. (2006). "Practice management guide for Pulmonary contusion — flail chest" (PDF). The Eastern Association for the Surgery of Trauma. Archived from the original (PDF) on 25 February 2009. Retrieved 18 June 2008.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ a b
Karmy-Jones R, Jurkovich GJ (March 2004). "Blunt chest trauma". Current Problems in Surgery. 41 (3): 211–380. PMID 15097979.
- ISBN 0-340-69189-1.
- PMID 2589889.
- ^
Allen GS, Cox CS, Moore FA, Duke JH, Andrassy RJ (September 1997). "Pulmonary contusion: are children different?". Journal of the American College of Surgeons. 185 (3): 229–33. PMID 9291398.
- PMID 21008101.
External links
- Chest Trauma - pulmonary contusion, trauma.org
