Liver tumor
This article includes a improve this article by introducing more precise citations. (September 2009) ) |
| Liver tumor | |
|---|---|
| Other names | Hepatic tumors |
| Specialty | Oncology, Gastroenterology, Hepatology |
| Diagnostic method | medical imaging, liver biopsy |
| Treatment | varies based on type |
Liver tumors (also known as hepatic tumors) are abnormal growth of liver cells on or in the
Classification

Liver tumors can be broadly classified as
Benign
There are several types of benign liver tumors. They are caused by either abnormal growth of
: 693–704Hemangiomas
Liver hemangiomas do not usually cause symptoms.[2][5] They are usually small, with sizes up to 10 centimeters.[5] Their size tends to remain stable overtime.[5] However, if the hemangioma is large it can cause abdominal pain, a sense of fullness in right upper abdominal area, heart problems, and coagulation dysfunction.[2][5] Cavernous hemangiomas are diagnosed with medical imaging (do not usually need biopsy to confirm diagnosis).[2]
Given their benign course and often asymptomatic nature, cavernous hemangiomas are typically diagnosed
Focal nodular hyperplasia
Focal nodular hyperplasia (FNH) is the second most common benign tumor of the liver.[2] FNH is found in 0.2%–0.3% of adults worldwide.[2] FNH is more common in females (10:1 female to male ratio) except in Japan and China, in which there is a more equal prevalence of cases between females and males.[2] FNH is associated with women of childbearing years and has been associated with women taking hormonal oral contraceptives.[2] This tumor is the result of a congenital arteriovenous malformation hepatocyte response. This process is one in which all normal constituents of the liver are present, but the pattern by which they are presented is abnormal.[citation needed]
These tumors usually do not have any symptoms. If large, they may present with abdominal pain.
Given the benign nature of FNH and the fact that they rarely progress in size or undergo malignant transformation, FNH tumors are usually managed with clinical monitoring.
Hepatic adenoma
Hepatocellular adenomas are most often
Because hepatocellular adenomas are so rare, there are no clear guidelines for the best course of treatment.
Women of childbearing age with hepatic adenomas were previously recommended to avoid becoming pregnant altogether; however, currently a more individualized approach is recommended that takes into account the size of the adenoma and whether surgical resection is possible prior to becoming pregnant.[9][7] Currently, there is a clinical trial called the Pregnancy and Liver Adenoma Management (PALM) study that is investigating management of hepatic adenomas during pregnancy; however, the results of this trial have not been published as of February 2021.[10]
Liver Cell Adenomatosis
Liver cell adenomatosis (also called hepatic adenomatosis) is a related but distinct diagnosis from hepatocellular adenoma.[11][7] On medical imaging and histopathological biopsy results they are the same as hepatic adenomas.[7] Liver cell adenomatosis differs from hepatic adenomas by its definition of more than 10 hepatic adenomas that are in both liver lobes in a person who does not have a glycogen storage disease and is not taking exogenous hormones.[7] Liver cell adenomatosis is not associated with steroid use (e.g. their size does not change when taking or not taking oral contraceptives containing estrogen or anabolic steroids), which is another distinction from hepatic adenomas.[11] Liver cell adenomatosis is associated with liver dysfunction and higher rates of bleeding than hepatic adenomas alone.[7] Available evidence suggests that bleeding occurs in approximately 63% of patients with liver cell adenomatosis.[11] Liver cell adenomatosis is also associated with becoming hepatocellular carcinoma.[11] Like hepatic adenomas, they are diagnosed with imaging and biopsies as needed. Treatment of liver cell adenomatosis is difficult due to the multiple, widespread lesions. Liver imaging should be reviewed to see if it is possible to surgically remove the tumors.[7] Liver transplantation is a treatment option for some patients.[7]
Simple Liver Cysts
Liver cysts are common. They are fluid-filled contained structures within the liver. Simple liver cysts are seen most commonly in women and kids.
Pseudotumors:
Pseudotumors differ from liver tumors in that they are not a proliferation of abnormal cells but are "local variations" of tissue type.
Cancerous


- Most cases are renal cancer, prostate cancer, etc.
- The most frequent, malignant, primary liver cancer is hepatocellular carcinoma.[13]
- Other forms of primary forms of liver cancer include cholangiocarcinoma, mixed tumors, sarcoma, and hepatoblastoma.
Diagnosis
Upon discovery of a liver tumor, the main issue in the workup is to determine whether the tumor is benign or malignant. Many imaging modalities are used to aid in the diagnosis of malignant liver tumors. These include
Ultrasound
Ultrasonography of liver tumors involves two stages: detection and characterization.[citation needed] Tumor detection is based on the performance of the method and should include morphometric information (three axes dimensions, volume) and topographic information (number, location specifying liver segment and lobe/lobes). The specification of these data is important for staging liver tumors and prognosis.[citation needed] Tumor characterization is a complex process based on a sum of criteria leading towards tumor nature definition. Often, other diagnostic procedures, especially interventional ones are no longer necessary. Tumor characterization using the ultrasound method will be based on the following elements: consistency (solid, liquid, mixed), echogenicity, structure appearance (homogeneous or heterogeneous), delineation from adjacent liver parenchyma (capsular, imprecise), elasticity, posterior acoustic enhancement effect, the relation with neighboring organs or structures (displacement, invasion), vasculature (presence and characteristics on Doppler ultrasonography and contrast-enhanced ultrasound (CEUS).[citation needed]
Computed tomography
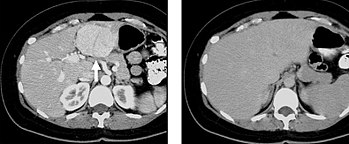
When evaluating hepatic masses by
References
- ^ "Liver Tumors". Johns Hopkins Medicine. Retrieved 4 July 2021.
- ^ OL 29371356M – via Google Books.
- ^ "Benign Liver Tumors". The Lecturio Medical Concept Library. Retrieved 4 July 2021.
- OL 28261767M.
- ^ PMID 26361504.
- S2CID 31253509.
- ^ PMID 26557953.
- PMID 20887318.
- PMID 23320183.
- PMID 22748109.
- ^ PMID 26011213.
- ^ Prevention, CDC-Centers for Disease Control and (2019-07-16). "CDC - Echinococcosis - Biology". www.cdc.gov. Retrieved 2021-02-15.
- PMID 31439937.
- PMID 23396291.
- PMID 24649215.
