Jaundice
| Jaundice | |
|---|---|
| Other names | Icterus rifampin[4] |
| Treatment | Based on the underlying cause[5] |
Jaundice, also known as icterus, is a yellowish or greenish pigmentation of the
Normal levels of bilirubin in
Causes of jaundice vary from relatively benign to potentially fatal.
Treatment of jaundice is typically determined by the underlying cause.
Signs and symptoms
The most common signs of jaundice in adults are a yellowish discoloration of the white area of the eye (sclera) and skin[13] with scleral icterus presence indicating a serum bilirubin of at least 3 mg/dl.[14] Other common signs include dark urine (bilirubinuria) and pale (acholia) fatty stool (steatorrhea).[15] Because bilirubin is a skin irritant, jaundice is commonly associated with severe itchiness.[16][17]
Eye conjunctiva has a particularly high affinity for bilirubin deposition due to high elastin content. Slight increases in serum bilirubin can, therefore, be detected early on by observing the yellowing of sclerae. Traditionally referred to as scleral icterus, this term is actually a misnomer, because bilirubin deposition technically occurs in the conjunctival membranes overlying the avascular sclera. Thus, the proper term for the yellowing of "white of the eyes" is conjunctival icterus.[18]
A much less common sign of jaundice specifically during childhood is yellowish or greenish teeth. In developing children, hyperbilirubinemia may cause a yellow or green discoloration of teeth due to bilirubin deposition during the process of tooth calcification.[19] While this may occur in children with hyperbilirubinemia, tooth discoloration due to hyperbilirubinemia is not observed in individuals with adult-onset liver disease. Disorders associated with a rise in serum levels of conjugated bilirubin during early development can also cause dental hypoplasia.[20]
Causes

Jaundice is a sign indicating the presence of an underlying diseases involving abnormal bilirubin metabolism, liver dysfunction, or biliary-tract obstruction. In general, jaundice is present when blood levels of bilirubin exceed 3 mg/dl.[14] Jaundice is classified into three categories, depending on which part of the physiological mechanism the pathology affects. The three categories are:
| Category | Definition |
|---|---|
| Prehepatic/hemolytic | The pathology occurs prior to the liver metabolism, due to either intrinsic causes to red blood cell rupture or extrinsic causes to red blood cell rupture. |
| Hepatic/hepatocellular | The pathology is due to damage of parenchymal liver cells. |
| Posthepatic/cholestatic | The pathology occurs after bilirubin conjugation in the liver, due to obstruction of the biliary tract and/or decreased bilirubin excretion.[citation needed] |
Prehepatic causes
Prehepatic jaundice is most commonly caused by a pathological increased rate of red blood cell (erythrocyte) hemolysis. The increased breakdown of erythrocytes → increased unconjugated serum bilirubin → increased deposition of unconjugated bilirubin into mucosal tissue.[21] These diseases may cause jaundice due to increased erythrocyte hemolysis:[22]
- Sickle-cell anemia[23]
- Spherocytosis[24]
- Thalassemia[25]
- Pyruvate kinase deficiency
- Glucose-6-phosphate dehydrogenase deficiency
- Microangiopathic hemolytic anemia
- Hemolytic–uremic syndrome
- Severe malaria (in endemic countries)
Hepatic causes
Hepatic jaundice is caused by abnormal liver metabolism of bilirubin.[26] The major causes of hepatic jaundice are significant damage to hepatocytes due to infectious, drug/medication-induced, autoimmune etiology, or less commonly, due to inheritable genetic diseases.[27] The following is a partial list of hepatic causes to jaundice:[28]
- Acute hepatitis
- Chronic hepatitis
- Hepatotoxicity
- Cirrhosis
- Drug-induced hepatitis
- Alcoholic liver disease
- Gilbert's syndrome (found in about 5% of the population, results in induced mild jaundice)
- Crigler–Najjar syndrome, type I
- Crigler–Najjar syndrome, type II
- Leptospirosis
Posthepatic causes (Obstructive jaundice)
Posthepatic jaundice (obstructive jaundice) is caused by a blockage of bile ducts that transport bile containing conjugated bilirubin out of the liver for excretion.[29] This is a list of conditions that can cause posthepatic jaundice:
- Choledocholithiasis (common bile duct gallstones). It is the most common cause of obstructive jaundice.
- Pancreatic cancer of the pancreatic head
- Biliary tract strictures
- Biliary atresia
- Primary biliary cholangitis
- Cholestasis of pregnancy
- Acute Pancreatitis
- Chronic Pancreatitis
- Pancreatic pseudocysts
- Mirizzi's syndrome
- Parasites ("liver flukes" of the Opisthorchiidae and Fasciolidae)[30]
Pathophysiology
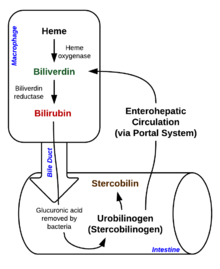
Jaundice is typically caused by an underlying pathological process that occurs at some point along the normal physiological pathway of heme metabolism. A deeper understanding of the anatomical flow of normal heme metabolism is essential to appreciate the importance of prehepatic, hepatic, and posthepatic categories. Thus, an anatomical approach to heme metabolism precedes a discussion of the pathophysiology of jaundice.[citation needed]
Normal heme metabolism
Prehepatic metabolism
When
Hepatic metabolism
Once unconjugated bilirubin arrives in the liver, liver enzyme
Posthepatic metabolism
Bilirubin enters the intestinal tract via bile. In the intestinal tract, bilirubin is converted into urobilinogen by symbiotic intestinal bacteria. Most urobilinogen is converted into stercobilinogen and further oxidized into stercobilin. Stercobilin is excreted via feces, giving stool its characteristic brown coloration.[32] A small portion of urobilinogen is reabsorbed back into the gastrointestinal cells. Most reabsorbed urobilinogen undergoes hepatobiliary recirculation. A smaller portion of reabsorbed urobilinogen is filtered into the kidneys. In the urine, urobilinogen is converted to urobilin, which gives urine its characteristic yellow color.[32]
Abnormalities in heme metabolism and excretion
One way to understand jaundice pathophysiology is to organize it into disorders that cause increased bilirubin production (abnormal heme metabolism) or decreased bilirubin excretion (abnormal heme excretion).[citation needed]
Prehepatic pathophysiology
Prehepatic jaundice results from a pathological increase in bilirubin production: an increased rate of erythrocyte hemolysis causes increased bilirubin production, leading to increased deposition of bilirubin in mucosal tissues and the appearance of a yellow hue.[citation needed]
Hepatic pathophysiology
Hepatic jaundice (hepatocellular jaundice) is due to significant disruption of liver function, leading to hepatic cell death and necrosis and impaired bilirubin transport across
The unconjugated bilirubin still enters the liver cells and becomes conjugated in the usual way. This conjugated bilirubin is then returned to the blood, probably by rupture of the congested bile canaliculi and direct emptying of the bile into the lymph exiting the liver. Thus, most of the bilirubin in the plasma becomes the conjugated type rather than the unconjugated type, and this conjugated bilirubin, which did not go to the intestine to become urobilinogen, gives the urine a dark color.[34][clarification needed]
Posthepatic pathophysiology
Posthepatic jaundice, also called obstructive jaundice, is due to the blockage of bile excretion from the biliary tract, which leads to increased conjugated bilirubin and bile salts there. In complete obstruction of the bile duct, conjugated bilirubin cannot access the intestinal tract, disrupting further bilirubin conversion to urobilinogen and, therefore, no stercobilin or urobilin is produced. In obstructive jaundice, excess conjugated bilirubin is filtered into the urine without urobilinogen. Conjugated bilirubin in urine (bilirubinuria) gives urine an abnormally dark brown color. Thus, the presence of pale stool (stercobilin absent from feces) and dark urine (conjugated bilirubin present in urine) suggests an obstructive cause of jaundice. Because these associated signs are also positive in many hepatic jaundice conditions, they cannot be a reliable clinical feature to distinguish obstructive versus hepatocellular jaundice causes.[35]
Diagnosis
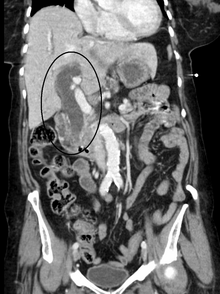
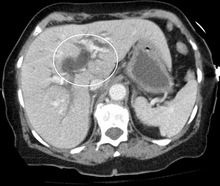
Most people presenting with jaundice have various predictable patterns of liver panel abnormalities, though significant variation does exist. The typical liver panel includes blood levels of enzymes found primarily from the liver, such as the
Laboratory tests
| Prehepatic jaundice | Hepatic jaundice | Posthepatic jaundice | |
|---|---|---|---|
| Total serum bilirubin | Normal / increased | Increased | Increased |
| Conjugated bilirubin | Normal | Increased | Increased |
| Unconjugated bilirubin | Normal / increased | Increased | Normal |
| Urobilinogen | Normal / increased | Decreased | Decreased / negative |
| Urine color | Normal[38] | Dark (urobilinogen, conjugated bilirubin) | Dark (conjugated bilirubin) |
| Stool color | Brown | Slightly pale | Pale, white |
| Alkaline phosphatase levels | Normal | Increased | Highly increased |
| Alanine transferase and aspartate transferase levels | Highly increased | Increased | |
| Conjugated bilirubin in urine | Not present | Present | Present |
Some bone and heart disorders can lead to an increase in ALP and the aminotransferases, so the first step in differentiating these from liver problems is to compare the levels of GGT, which are only elevated in liver-specific conditions. The second step is distinguishing from biliary (cholestatic) or liver causes of jaundice and altered laboratory results. ALP and GGT levels typically rise with one pattern while
Laboratory results for liver panels are frequently compared by the magnitude of their differences, not the pure number, as well as by their ratios. The AST:ALT ratio can be a good indicator of whether the disorder is alcoholic liver damage (above 10), some other form of liver damage (above 1), or hepatitis (less than 1). Bilirubin levels greater than 10 times normal could indicate neoplastic or intrahepatic cholestasis. Levels lower than this tend to indicate hepatocellular causes. AST levels greater than 15 times normal tend to indicate acute hepatocellular damage. Less than this tend to indicate obstructive causes. ALP levels greater than 5 times normal tend to indicate obstruction, while levels greater than 10 times normal can indicate drug (toxin) induced cholestatic hepatitis or
Laboratory findings depend on the cause of jaundice:
- Urine: conjugated bilirubin present, urobilinogen > 2 units but variable (except in children)
- Plasma proteinsshow characteristic changes.
- Plasma albumin level is low, but plasma globulins are raised due to an increased formation of antibodies.
Unconjugated bilirubin is hydrophobic, so cannot be excreted in urine. Thus, the finding of increased urobilinogen in the urine without the presence of bilirubin in the urine (due to its unconjugated state) suggests hemolytic jaundice as the underlying disease process.
Imaging
Medical imaging such as ultrasound, CT scan, and HIDA scan are useful for detecting bile-duct blockage.[40]
Differential diagnosis
- Yellow discoloration of the skin, especially on the palms and the soles, but not of the sclera or inside the mouth, is often due to carotenemia—a harmless condition.[41]
- Yellow discoloration of the skin can also rarely occur with hypercupremia, whether from Wilson's disease or from another metabolic derangement. Similarly, a golden-ish ring at the edges of the irises can occur (Kayser-Fleischer ring).
Treatment
Treatment of jaundice varies depending on the underlying cause.[5] If a bile duct blockage is present, surgery is typically required; otherwise, management is medical.[5][42][43][44]
Complications
Hyperbilirubinemia, more precisely hyperbilirubinemia due to the unconjugated fraction, may cause bilirubin to accumulate in the grey matter of the central nervous system, potentially causing irreversible neurological damage, leading to a condition known as kernicterus. Depending on the level of exposure, the effects range from unnoticeable to severe brain damage and even death. Newborns are especially vulnerable to hyperbilirubinemia-induced neurological damage, so must be carefully monitored for alterations in their serum bilirubin levels.[citation needed]
Individuals with parenchymal liver disease who have impaired hemostasis may develop bleeding problems.[45]
Epidemiology
Jaundice in adults is rare.[46][47][48] Under the five year DISCOVERY programme in the UK, annual incidence of jaundice was 0.74 per 1000 individuals over age 45, although this rate may be slightly inflated due to the main goal of the programme collecting and analyzing cancer data in the population.[49] Jaundice is commonly associated with severity of disease with an incidence of up to 40% of patients requiring intensive care in ICU experiencing jaundice.[48] The causes of jaundice in the intensive care setting is both due to jaundice as the primary reason for ICU stay or as a morbidity to an underlying disease (i.e. sepsis).[48]
In the developed world, the most common causes of jaundice are blockage of the bile duct or medication-induced. In the developing world, the most common cause of jaundice is infectious such as viral hepatitis, leptospirosis, schistosomiasis, or malaria.[4]
Risk factors
Risk factors associated with high serum bilirubin levels include male gender, white ethnicities, and active smoking.[50] Mean serum total bilirubin levels in adults were found to be higher in men (0.72 ± 0.004 mg/dl) than women (0.52 ± 0.003 mg/dl).[50] Higher bilirubin levels in adults are found also in non-Hispanic white population (0.63 ± 0.004 mg/dl) and Mexican American population (0.61 ± 0.005 mg/dl) while lower in non-Hispanic black population (0.55 ± 0.005 mg/dl).[50] Bilirubin levels are higher in active smokers.[50]
Special populations
Neonatal jaundice
Symptoms
Jaundice in infants presents with yellowed skin and icteral sclerae. Neonatal jaundice spreads in a cephalocaudal pattern, affecting the face and neck before spreading down to the trunk and lower extremities in more severe cases.[51] Other symptoms may include drowsiness, poor feeding, and in severe cases, unconjugated bilirubin can cross the blood-brain barrier and cause permanent neurological damage (kernicterus).
Causes
The most common cause of jaundice in infants is
- Formula jaundice[52]
- Hereditary spherocytosis
- Glucose-6-phosphate dehydrogenase deficiency
- Pyruvate kinase deficiency
- ABO/Rh blood type autoantibodies
- Alpha 1-antitrypsin deficiency
- Alagille syndrome (genetic defect resulting in hypoplastic intrahepatic bile ducts)
- Progressive familial intrahepatic cholestasis
- Pyknocytosis (due to vitamin deficiency)
- Cretinism(congenital hypothyroidism)
- Sepsis or other infectious causes
Pathophysiology
Transient neonatal jaundice is one of the most common conditions occurring in newborns (children under 28 days of age) with more than 80 per cent experienceing jaundice during their first week of life.[53] Jaundice in infants, as in adults, is characterized by increased bilirubin levels (infants: total serum bilirubin greater than 5 mg/dL).
Normal physiological neonatal jaundice is due to immaturity of liver enzymes involved in bilirubin metabolism, immature gut microbiota, and increased breakdown of fetal hemoglobin (HbF).
While most cases of newborn jaundice are not harmful, when bilirubin levels are very high, brain damage — kernicterus — may occur[55][8] leading to significant disability.[56] Kernicterus is associated with increased unconjugated bilirubin (bilirubin which is not carried by albumin). Newborns are especially vulnerable to this damage, due to increased permeability of the blood–brain barrier occurring with increased unconjugated bilirubin, simultaneous to the breakdown of fetal hemoglobin and the immaturity of gut flora. This condition has been rising in recent years. as babies spend less time in sunlight.[citation needed]
Treatment
Jaundice in newborns is usually transient and dissipates without medical intervention. In cases when serum bilirubin levels are greater than 4–21 mg/dl (68–360 μmol/L), infant may be treated with
Etymology
Jaundice comes from the French jaune, meaning 'yellow'; jaunisse meaning 'yellow disease'. The medical term is icterus, from the Greek word ikteros.
References
- ISBN 978-0-7817-6699-9.
- ^ PMID 25663760.
- ^ a b c d Jaundice. Archived from the original on 27 August 2016. Retrieved 13 August 2016.
{{cite book}}:|website=ignored (help) - ^ ISBN 978-0-19-856782-0. Archivedfrom the original on 8 September 2017.
- ^ ISBN 978-0-323-08430-7. Archivedfrom the original on 8 September 2017.
- ISBN 978-0-323-07585-5. Archivedfrom the original on 8 September 2017.
- ISBN 978-3-319-39746-7.
- ^ ISBN 978-0-323-35214-7.
- ^ PMID 25384650.
- ^ PMID 21872092.
- ^ Dr. Chase's Family Physician, Farrier, Bee-keeper, and Second Receipt Book,: Being an Entirely New and Complete Treatise ... Chase Publishing Company. 1873. p. 542. Archived from the original on 8 September 2017.
- ISBN 978-1-4377-0774-8.
- PMID 27904243.
- ^ ISBN 978-1-118-32138-6.
- ISBN 978-0-7817-7513-7. Archivedfrom the original on 8 September 2017.
- OCLC 62736861.
- PMID 25663760.
- ISBN 978-0-323-39276-1.
- ISBN 978-981-4371-07-0.
- PMID 20013583.
- PMID 31334972. Retrieved 23 April 2022.
- ^ "What causes jaundice in hemolytic anemia?". www.medscape.com. Retrieved 26 April 2022.
- ^ "What Is Sickle Cell Disease?". National Heart, Lung, and Blood Institute. 12 June 2015. Archived from the original on 6 March 2016. Retrieved 8 March 2016.
- ISBN 978-0-07-144035-6. Retrieved 15 November 2010.
- ^ "Thalassemia". The Lecturio Medical Concept Library. Retrieved 27 July 2021.
- PMID 29261920. Retrieved 23 April 2022.
- PMID 32965843. Retrieved 23 April 2022.
- ^ Tholey D (January 2023). "Jaundice". Merck Manual. Professional Version. Merck. Retrieved 12 April 2022.
- ^ "Bilirubin Metabolism – an overview | ScienceDirect Topics". www.sciencedirect.com. Retrieved 23 April 2022.
- ^ "CDC – Liver Flukes". www.cdc.gov. 18 April 2019. Retrieved 5 June 2020.
- ^ S2CID 11100275.
- ^ ISBN 978-1-351-07011-9.
- ISBN 978-81-312-1154-0.
- ISBN 978-1-4160-4574-8.
- PMID 11141153.
- ^ "Liver Function Tests". MedlinePlus. US National Library of Medicine. Retrieved 16 January 2021.
- PMID 14765767. Retrieved 22 September 2020.
- ISBN 978-0-19-967986-7. Archivedfrom the original on 8 September 2017.
- ^ Cadogen M (21 April 2019). "Bilirubin and Jaundice". Life in the Fast Lane. Retrieved 19 November 2019.
- ^ PMID 14765767.
- ^ Carotenemia at eMedicine
- PMID 24999215.
- ISBN 978-3-319-22272-1.
- PMID 27904244.
- ISBN 978-981-4371-07-0.
- ISBN 978-1-118-74252-5. Archivedfrom the original on 8 September 2017.
- PMID 18438808.
- ^ PMID 17116459.
- PMID 22247287.
- ^ S2CID 25854541.
- ISBN 978-0-323-39956-2.
- PMID 11230622.
- PMID 25384650.
- ISBN 978-0-19-922888-1.[page needed]
- ^ "Facts about Jaundice and Kernicterus". CDC. 23 February 2015. Archived from the original on 8 August 2016. Retrieved 13 August 2016.
- .
- PMID 36867730.
- ^ "Bili Lights for Jaundice: Effectiveness for Neonatal and Adults | Heliotherapy Research Institute". Retrieved 24 July 2022.
- PMID 24913724.
- ^ PMID 34228352.
- ^ O'Keefe L (May 2001). "Increased vigilance needed to prevent kernicterus in newborns". American Academy of Pediatrics. 18 (5): 231. Archived from the original on 27 September 2007.
- ^ a b "Definition of Icterus". MedicineNet.com. 2011. Archived from the original on 7 August 2012. Retrieved 3 February 2013.
- ^ Icterus | Define Icterus at Dictionary.com Archived 2010-12-31 at the Wayback Machine. Dictionary.reference.com. Retrieved on 2013-12-23.
- PMID 26061953.
Further reading
- Green J, Beyar R, Sideman S, Mordechovitz D, Better OS (1986). "The 'jaundiced heart': A possible explanation for postoperative shock in obstructive jaundice". Surgery. 100 (1): 14–20. PMID 3726756.
- Green J, Beyar R, Bomzon L, Finberg JP, Better OS (1984). "Jaundice, the Circulation and the Kidney". Nephron. 37 (3): 145–52. PMID 6738765.
- Fajers CM (2009). "Experimental Studies in Cholemic Nephrosis". Acta Pathologica et Microbiologica Scandinavica. 41 (1): 44–55. PMID 13443982.
